CDC Data Show U.S. Life Expectancy Continues to Decline
Suicides, Drug Overdose Deaths Named as Key Contributors
December 10, 2018, 04:02 pm Michael Devitt – A century ago, the average life expectancy in the United States was just 39 years. Admittedly, that figure is something of an outlier, given the deadly influenza pandemic that raged that year, killing an estimated 50 million people or more around the globe, including some 675,000 Americans. The years immediately before and after the so-called Spanish flu wreaked havoc worldwide saw life expectancies of 51 and 55 years, respectively.
Although that may sound like good news, it all depends on one's perspective. Three data briefs published by the CDC late last month show that for the second time in three years, the average life expectancy in the United States has actually gone down, with two highly avoidable causes responsible for much of the drop, according to a top CDC official.
"The latest CDC data show that the U.S. life expectancy has declined over the past few years," said CDC Director Robert Redfield, M.D., in a Nov. 29 statement. "Tragically, this troubling trend is largely driven by deaths from drug overdose and suicide.
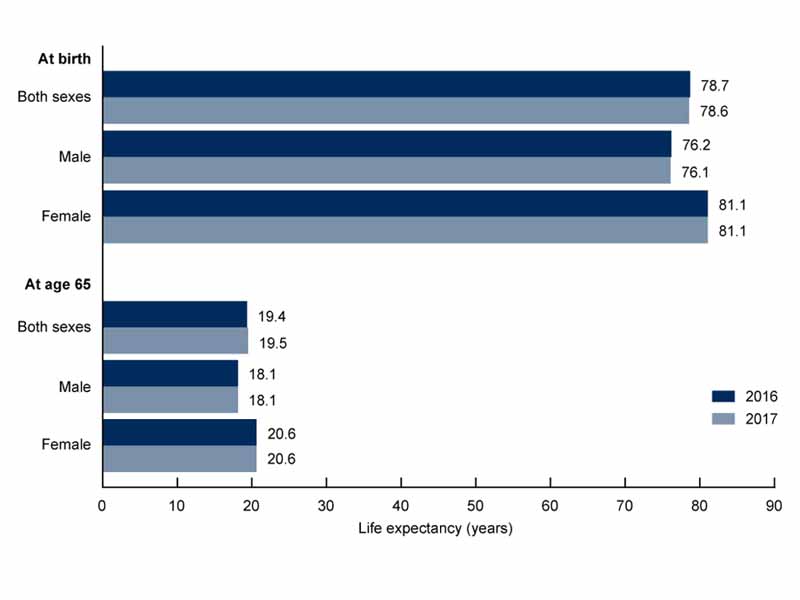
SOURCE: National Center for Health Statistics, National Vital Statistics System, Mortality.
"Life expectancy gives us a snapshot of the nation's overall health, and these sobering statistics are a wake-up call that we are losing too many Americans, too early and too often, to conditions that are preventable."
One family physician expert who spoke with AAFP News couldn't agree more.
"It is shocking that the United States, with its vast resources, continues to see increases in preventable deaths," said Jennifer Frost, M.D., medical director for the Academy's Health of the Public and Science Division. "We need to make better use of our resources and work to improve the lives of all Americans."
Data Briefs Address Mortality, Drug Overdose, Suicide Rates
The first of those CDC briefs updated a report the agency published in September and provided a snapshot of longevity rates in the United States throughout 2017. Data from the brief and that earlier report showed that average life expectancy decreased from 78.9 years in 2014 to 78.7 years in 2015, remained unchanged between 2015 and 2016, and then decreased again between 2016 and 2017 to the current 78.6 years.
More than 2.8 million deaths occurred in the United States in 2017, an increase of about 70,000 from the previous year. Death rates rose significantly in three age groups during that period (i.e., in those 25-34, 35-44, and 85 and older) and dropped in 45- to 54-year-olds, yielding an overall age-adjusted increase of 0.4 percent. That percentage represents a rise from 728.8 deaths per 100,000 standard population to 731.9 per 100,000.
The 10 leading causes of death remained the same from 2016 to 2017: heart disease, cancer, unintentional injuries, chronic lower respiratory diseases, stroke, Alzheimer's disease, diabetes, influenza and pneumonia, kidney disease, and suicide. Age-adjusted death rates increased significantly for seven of the 10 causes, led by influenza and pneumonia (5.9 percent), unintentional injuries (4.2 percent) and suicide (3.7 percent). Death rates for cancer actually decreased by 2.1 percent, while heart disease and kidney disease rates did not change significantly.
The second CDC brief used information from the National Vital Statistics System (NVSS) to analyze drug overdose deaths in the United States from 1999 to 2017. It reported a total of 70,237 such deaths in 2017, which yielded an age-adjusted rate that was 9.6 percent higher in 2017 than in 2016.
Drug overdose death rates increased across all age groups, with the highest rate occurring in adults ages 35-44 (39 per 100,000) and the lowest in adults 65 and older (6.9 per 100,000).
A sharp increase in drug overdose deaths involving synthetic opioids other than methadone was seen between 2016 and 2017, with the age-adjusted rate involving drugs such as fentanyl, fentanyl analogs and tramadol shooting up 45 percent during that period. For other opioids, drug overdose death rates remained unchanged: Drug overdose death rates for methadone (1.0 per 100,000), natural and semisynthetic opioids (4.4 per 100,000) and heroin (4.9 per 100,000) were the same in 2017 as in 2016.
In both males and females, suicide rates in the 10-14, 15-24, 25-44, 45-64 and 65-74 age groups were significantly higher in 2017 than in 1999, but they were significantly lower in those 75 and older. In women, 2017 suicide rates were highest among those 45-64 (9.7 per 100,000), while in men, suicide rates were highest among those 75 and older (39.7 per 100,000).
Age-adjusted suicide rates varied considerably based on a person's environment. In 2017, the age adjusted rate for the most rural counties was 1.8 times the rate for the most urban counties. The overall age-adjusted suicide rate for the most rural counties was 53 percent higher in 2017 than in 1999.
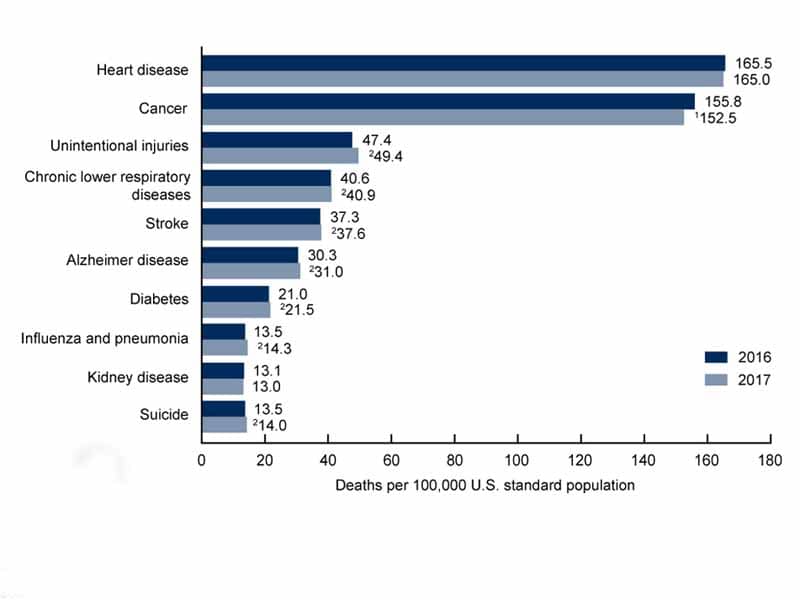
SOURCE: National Center for Health Statistics, National Vital Statistics System, Mortality.
What Family Physicians Can Do
Americans have enjoyed an unprecedented run at living longer, healthier lives for much of the 20th century. Clean air and water, improved sanitation and refrigeration systems, public education, vaccines and life-saving drugs, and management of chronic diseases all have added years to the average American's lifespan and virtually guaranteed that a child born in the United States would be expected to live longer than his or her parents.
Now, slowly, those gains are being eaten away.
Fortunately, some steps are being taken to address causes of excess mortality at the federal level. In October, for example, President Donald Trump signed the Substance Use-Disorder Prevention that Promotes Opioid Recovery and Treatment for Patients and Communities Act, a bipartisan bill that, among other things, expands access to treatment for opioid use disorder and authorizes funding for comprehensive opioid recovery centers and other programs.
The AAFP supported this legislation in letters to both House and Senate leaders.
And just last month, the Academy joined dozens of other organizations in urging Congress to pass the Preventing Maternal Deaths Act, which seeks to stem the growing crisis of mothers dying from pregnancy-related complications at a rate that surpasses that of any other developed nation.
But although the AAFP and other groups are looking at such problems from a national perspective, there are plenty of ways family physicians can help patients at the individual level.
"The causes of drug addiction and suicide are complex, but there are some things that can help prevent them that family physicians do every day," Frost told AAFP News.
With regard to drug addiction, Frost recommended that family physicians limit the number of opioids they prescribe to patients with acute pain and work to increase their awareness of the risk factors for and warning signs of addiction.
Regarding suicide, she recommended that FPs screen all adolescents and adults, including pregnant women, for depression. If a patient has a positive screen, the family physician should confirm the diagnosis and ensure the patient receives appropriate treatment.
Frost also noted that the percentage of deaths from influenza and pneumonia rose more than any other leading cause of death from 2016 to 2017. "It was the cause of death that increased the most, and it is something that family physicians can directly impact," she said, and encouraged FPs to ensure that all patients receive the recommended vaccinations against these diseases.
Related AAFP News Coverage
Authors See Crucial Role for Primary Care in Opioid Epidemic
(7/10/2018)
Suicide Rates Spike Across United States, Says CDC
Family Physicians Can Help Combat the Trend
(6/12/2018)
Nearly One in 12 U.S. Adults Reports Having Depression
Women Twice as Likely as Men to Be Depressed
(2/19/2018)
Additional Resources
CDC: Influenza (Flu): Preventive Steps
CDC: Pneumonia: Management and Prevention Guidelines
