What is insulin lispro, and how can it help control my blood sugar levels?
Insulin lispro (brand name: Humalog) is the newest type of insulin on the market. It's a fast-acting insulin that starts working sooner than other insulins. It also reaches peak activity faster and goes away sooner. Insulin lispro helps keep your blood sugar levels from going too high after you eat. Studies show that insulin lispro may do this better than regular insulin. In fact, insulin lispro may replace regular insulin for many patients with diabetes mellitus.
The medicines your doctor has prescribed are very important in keeping your diabetes under control. To keep your blood sugar level steady, your doctor will probably prescribe either a longer-acting insulin or another drug for you to take each day in addition to the insulin lispro.
When and how do I take insulin lispro?
Insulin lispro should be injected under the skin within 15 minutes before you eat. Your doctor will tell you how much insulin lispro to inject. Remember, you must eat 15 minutes after you take this insulin shot.
Insulin lispro is a little easier to take than regular insulin. If you've been using regular insulin, you've had to inject the insulin and then wait 30 to 45 minutes before eating. Many people find it hard to time regular insulin injections and mealtimes. Sometimes they end up eating too early or too late. Then they don't get the best blood sugar control. Since insulin lispro is taken so close to meals, it may help you get the best possible blood sugar control.
Can I mix insulin lispro with other insulins?
It's best that you mix insulin lispro only with Humulin U or Humulin N, which are brand names for certain longer-acting insulins. Insulin lispro should always be drawn into the syringe first. This will keep the longer-acting insulin from getting into the insulin lispro bottle. After mixing insulin lispro in the same syringe with Humulin U or Humulin N, you must inject the mixture under your skin within 15 minutes. Remember to eat soon after the injection.
How do I prepare the correct dose?
To prepare a dose of insulin lispro, follow these steps:
- Wash your hands.
- Take the plastic cover off the new insulin bottle and wipe the top of the bottle with a cotton swab that you have dipped in alcohol. It's best to allow the insulin to be at room temperature before you inject it.
- Pull back the plunger of the syringe. This way, you can draw air into the syringe equal to the dose of insulin lispro that you are taking. Then put the syringe needle through the rubber top of the insulin bottle. Inject air into the bottle by pushing the syringe plunger forward. Then turn the bottle upside down.
- Make sure that the tip of the needle is in the insulin. Pull back on the syringe plunger to draw the correct dose of insulin into the syringe (PICTURE 1). The dose of insulin is measured in units. PICTURE 1.Pull back on the plunger to draw the insulin into the syringe.ILLUSTRATIONS BY KATHRYN BORN
- Make sure there are no air bubbles in the syringe before you take the needle out of the insulin bottle. Air bubbles can cut down the amount of insulin that you get in your injection. If air bubbles are present, hold the syringe and the bottle straight up in one hand, tap the syringe with your other hand and let the air bubbles float to the top. Push on the plunger of the syringe to move the air bubbles back into the insulin bottle. Then withdraw the correct insulin dose by pulling back on the plunger.
Where do I inject the insulin lispro?
Insulin lispro is injected just under the skin. Your doctor or office staff will show you how and where to give an insulin injection. First, clean your skin with cotton dipped in alcohol (PICTURE 2, top). Most people are able to grab a fold of skin and inject insulin at a 90-degree angle (PICTURE 3). If you're thin, you may need to pinch the skin and inject the insulin at a 45-degree angle (PICTURE 4). When the needle is in your skin, you don't need to draw back on the syringe plunger to check for blood.
PICTURE 2.
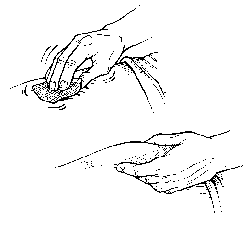
Clean the injection area using cotton and alcohol (top). Pinch an area of skin (bottom).
PICTURE 3.
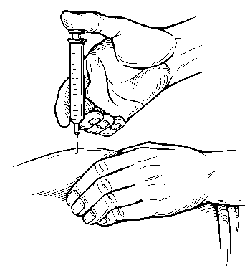
Inject the insulin with the needle at an angle of about 90 degrees.
PICTURE 4.
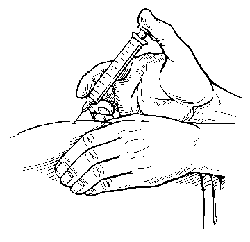
Thin people may find it easier to inject at an angle of 45 degrees.
The usual places to inject insulin are the upper arm, the front and side parts of the thighs and the abdomen (tummy area). Don't inject insulin closer than two inches to your navel (belly button).
To keep your skin from thickening, try not to inject the insulin in the same place over and over. Instead, change injection places. But if you usually inject insulin into your arm, just inject in different spots on your arm rather than switch to the thigh or abdomen. This works better because insulin is absorbed at different rates from your arm, your thigh and your abdomen.
What do I do if I have an “insulin reaction”?
Hypoglycemia is the name for a condition in which the blood sugar level is too low. In people who take insulin, this condition is called an insulin reaction. Your blood sugar level can get too low if you exercise more than usual, if you don't eat enough or if you don't eat on time. If you have an insulin reaction, you may feel some or all of these symptoms: headache, nervousness, shakiness, heavy sweating, rapid heartbeat, hunger, confusion or dizziness. Most people who take insulin have insulin reactions at some time.
If you're going to be treated with insulin lispro, you need to be aware of insulin reactions and how to treat them. Insulin lispro will help you control your blood sugar level, but it does act quickly. While you and your doctor are working together to adjust your dose of this insulin, you may have some insulin reactions.
Just in case you have an insulin reaction, you should carry at least 15 grams of a fast-acting carbohydrate with you at all times. Here are examples of quick sources of energy that can relieve the symptoms of an insulin reaction:
- Nondiet sodas—one half to three fourths of a cup
- Fruit juices and fruits—one-half cup of juice or 2 tablespoons of raisins
- Candy—five Lifesavers
- Milk—one cup
- Glucose tablets—three tablets that are 5 grams each
If you don't feel better 15 minutes after having a fast-acting carbohydrate or if monitoring shows that your blood sugar level is still too low, have another 15 grams of a fast-acting carbohydrate.
If your blood sugar level is too low and, because of some physical problem, you need help from another person, you should teach family members and friends how to give you a drug called glucagon. Glucagon comes in a powder and a liquid that must be mixed together. Then the mixture has to be injected. Be sure that you take the time to learn about using glucagon.
How can I keep my blood sugar level from becoming too high or too low?
You need to check your blood sugar level regularly using a blood glucose monitor. Your doctor or the office staff can teach you how to use the monitor. You'll need to write each measurement down and show this record to your doctor, so your doctor can tell you how much insulin to take.
Blood sugar measurements are different depending on stress, exercise, how fast you absorb your food, and hormonal changes related to puberty, menstrual cycles, pregnancy, etc. Illness, traveling or a change in your routine may mean that you have to monitor your blood sugar level more often.

