Refugees and other immigrants often present with clinical problems that are as varied as their previous experiences. Clinical presentations may range from unusual infectious diseases to problems with transition. This article describes medical conditions associated with immigrants, as well as specific screening recommendations, including history, physical examination and laboratory tests, and some of the challenges encountered by family physicians caring for refugees.
Between 1986 and 1993, 8.2 million immigrants were legally granted permanent residence in the United States. By the early 1990s, an estimated 3 to 4 million illegal foreign-born residents were also present in this country (Figures 1 and 2). An additional 20 million nonimmigrant visitors and students are present in the United States.1 Family physicians should become familiar with the different categories of immigrants, their medical problems and the necessary screening examinations.
FIGURE 1.
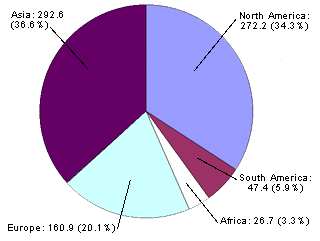
U.S. immigration patterns for 1994 by country of origin. (North America includes Central America and the Caribbean; population in thousands.)
FIGURE 2.
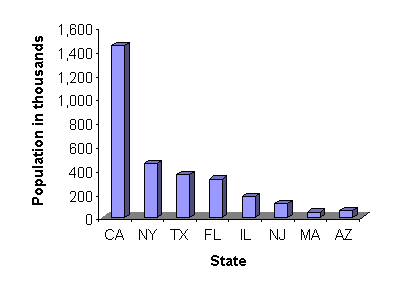
Estimated undocumented immigrants to the United States in 1994, by state.
Individuals and families arriving in the United States can be divided into three categories: legal immigrants, official refugees and undocumented residents. Legal immigrants include children placed for adoption, persons granted asylum and permanent residents. An official refugee, as defined by the United Nations' High Commission for Refugees,2 is “a person who, owing to a well-founded fear of being persecuted for reasons of race, religion, nationality, membership [in] a particular social group, or political opinion … is outside the country of his nationality.” Undocumented residents are those who enter the country illegally. Persons can change categories by modifying their legal status; for example, many political refugees who arrive as undocumented residents later apply for asylum.
In a study3 of refugee children in Buffalo, N.Y., it was determined that only 39 percent of the children had adequate evidence of vaccination. Frequent findings in these children included anemia, parasites and tuberculosis (purified protein derivative [PPD]) positivity. Since one third of the world's population is infected with tuberculosis, immigration (along with human immunodeficiency virus [HIV] infection) is a major factor in the resurgence of the disease in the United States. People arriving from Asia, Latin America and the former Soviet Union have the highest rates of infection, mostly from reactivation of disease (rather than transmission).4
Phases of Refugee Transition
The physical and psychologic effects of transition on the refugee depend on the reason for emigration (e.g., war, natural disaster, religious or political persecution, economic hardship). Unlike economic immigrants, refugees do not make a voluntary choice to leave their country. For refugees, the time following the decision to leave their homeland can be divided into five stages (Table 1).5 Initially, in the impact/preparatory stage (when the crisis occurs), the family and elements of the local community react by coming together, consolidating resources and developing a plan. The migration stage represents the period of flight. On arrival, refugees enter the overcompensation stage, where all energies are mobilized to enable them to live in a strange country. After a time (the honeymoon period), refugees often enter a decompensation stage as the challenges of life in a new environment become apparent. Finally, refugees may resolve personal issues and a period of intergenerational conflict may follow.
TABLE 1 Stages of Transition for Immigrants and Refugees
| Impact/preparatory stage |
| Migration stage |
| Overcompensation stage |
| Decompensation stage |
| Intergenerational and cultural conflict stage |
Information from Sluzki CE. Migration and family conflict. Fam Process 1979;18:379-90.
Clinical Evaluation
History
Specific screening recommendations depend on the refugee's immigration status and area of origin. Important components of a history in this population group include the following points: (1) nutritional status, including growth and development, especially in children; (2) mental health, including screening for anxiety, depression, post-traumatic stress disorder, physical abuse and substance abuse; (3) infectious diseases, including screening for diseases common to the refugee's country of origin, and (4) preventive screening, including cancer screening often not available in Third World countries (e.g., Papanicolaou [Pap] smears).
For example, a recent immigrant presenting with fever may have hepatitis, typhus, Q fever, encephalitis, dengue fever, typhoid, viral hemorrhagic fevers, helminths, malaria and/or other infectious diseases. Diarrhea may be caused by viral infection, Shigella, amebiasis, cholera or other unusual causes.
Physical Examination
The nutritional status of refugees may suffer in transit and may already be compromised as a result of parasites and other conditions in the country of origin. Growth and development of children may be affected; problems can be detected by using height/weight charts and developmental screens.
Physical examination frequently reveals dental problems (as high as 77 percent in one study6). Common problems in children include anemia, asthma, hypertension and orthopedic problems.3(p889) Refugees may have physical signs related to traditional health practices, such as coining (rubbing of coins over the skin) or cupping7 (application of heated cups to the skin) that can be mistaken for signs of abuse.8 On the other hand, the physician should look closely for physical signs of trauma and torture, including scars from beatings, whippings, burns and electric shocks, as well as lacerations. Presentations of unusual diseases are common, including congestive heart failure from cardiomyopathy in Chagas' disease. A physical deformity or radiograph may reveal old fractures, including those resulting from falanga (beating of the soles of the feet). Female genital mutilation (formerly referred to as female circumcision) is practiced in some societies.9
Specific and careful documentation of physical findings is essential, as the documentation may be needed for asylum or legal proceedings, and may represent an important supportive role for the family physician.10 Guides have been developed to assist in preparing such documentation.11
Laboratory/Screening Tests
Infectious diseases of global distribution encompass tuberculosis, including multiple drug-resistant tuberculosis, intestinal parasites and malaria.12 More “exotic” tropical diseases are less frequently encountered in the United States. The author routinely performs the following laboratory tests in screening refugee patients: complete blood cell count, hepatitis B screening, VDRL and/or rapid plasma reagin and HIV test (when indicated), stool analysis for ova and parasites, and an annual PPD test13,14 (Table 2).15 Hepatitis B infection is common in this patient group, particularly in immigrants from Asian countries. Screening for hepatitis B is recommended in all pregnant women and other high-risk persons.16
TABLE 2 Common Refugee Profiles
| Geographic region | Health problems | Screening method |
|---|---|---|
| Global | Tuberculosis | PPD |
| Trauma/rape/torture/PTSD | History, physical examination | |
| HIV disease | HIV enzyme immunoassay | |
| Measles, mumps and rubella, diphtheria, pertussis and tetanus | Update immunizations | |
| Hepatitis B | HBsAg | |
| Intestinal parasites: amebiasis, giardiasis, ascariasis, strongyloidiasis, hookworm, trichuriasis, enterobiasis | Stool analysis for ova and parasites | |
| Malnutrition/growth delay | Height and weight | |
| Neonatal tetanus | Clinical suspicion | |
| Rheumatic heart disease | Physical examination | |
| Latin America | Malaria | Thin and thick blood smears |
| Intestinal parasites (helminthic infection, amebiasis, giardiasis) | Stool analysis for ova and parasites, transparent tape prep | |
| Chagas' disease (South American trypanosomiasis) | Physical examination | |
| Leischmaniasis, onchocerciasis, lymphaticfilariasis, cysticercosis, schistosomiasis, echinococcosis | Clinical suspicion, urine and stool examination | |
| Africa | Malaria | Thin and thick blood smears |
| Sickle cell | Peripheral blood smears, hemoglobin electrophoresis | |
| Intestinal parasites (helminthic infection, amebiasis, giardiasis) | Stool analysis for ova and parasites | |
| Diarrheal illnesses | Physical examination | |
| HIV-related diseases | HIV enzyme immunoassay | |
| Viral hemorrhagic fevers,* borrelliosis | Clinical suspicion | |
| Leischmaniasis, schistosomiasis, filariasis, onchocerciasis, cysticercosis, echinococcosis | Clinical suspicion | |
| Leprosy | Physical examination | |
| Middle East | Thalassemia, G6PD deficiency | Peripheral blood smears, hemoglobin electrophoresis, G6PD enzyme activity |
| Schistosomiasis | Clinical suspicion, rectal biopsy | |
| Parasites (hookworm, amoebae, echinococcus, hydatid cyst) | Stool analysis for ova and parasites | |
| Asia | Leprosy | Physical examination |
| Parasites (roundworm, hookworm, filaria, flukes, amoebae, giardia) | Stool analysis for ova and parasites | |
| HIV-related diseases | HIV enzyme immunoassay | |
| Malaria (Southeast Asia) | Thick and thin blood smears |
PPD = purified protein derivative; PTSD = post-traumatic stress disorder; HIV = human immunodeficiency virus; G6PD = glucose-6-phosphate dehydrogenase; HBsAg = hepatitis B surface antigen.
*—Only a problem if patient currently has fever.
Information from Sandler RH, Jones TC, eds. Medical care of refugees. New York: Oxford University Press, 1987.
Commonly encountered parasites include Ascaris lumbricoides, Necator americanus, Giardia lamblia, Trichuris trichiura, Entamoeba histolytica and Schistosoma. Health care for Latin American immigrants may include screening for leprosy (examine the patient for hypopigmented macules with decreased sensation) in immigrants from high-risk areas.17
More than 6,000 children adopted internationally enter the United States each year, most from Korea, Russia, China and Latin America. Studies have shown that more than 50 percent of these children have an undiagnosed condition that is only found on arrival in this country.18 The same screening tests mentioned above for adults should be performed in these children.
Patients applying for permanent residency status are required to have a physical and mental evaluation by a physician who is listed as a civil surgeon by the Immigration and Naturalization Service (INS). The examination includes a standard medical history with questions about disabilities, substance abuse and mental health issues, as well as a physical examination. The INS requires testing for tuberculosis, syphilis and HIV. The Immigration Act of 1990 modified previous guidelines by making persons with mental disorders excludable only if their disorder is associated with harmful behavior (e.g., injury or threat to health and safety).19
Most active cases of tuberculosis occur within the first five years after an immigrant enters the United States. Under the revised guidelines, criteria for immigrants with tuberculosis were also liberalized to allow those with a chest radiograph consistent with tuberculosis but negative sputum smears to receive treatment in the United States. Screening and treatment for tuberculosis follow standard guidelines from the Centers for Disease and Control and Prevention.20
Immunization status should be reviewed and updated. Children most commonly have some diphtheria, pertussis, tetanus/oral polio-vaccine coverage, but they often lack documentation. They often need vaccination for measles, mumps, and rubella, as well as Haemophilus influenzae type b and hepatitis B. Previous immunization with bacille Calmette-Guérin vaccine should not be considered in the interpretation of the PPD results.
Cancer screening should be performed according to age-appropriate guidelines, and the physician should be particularly alert for cancer types that occur with more increased frequency in other parts of the world. These cancer types include gastric, lung (as cigarette smoking expands globally) and hepatocellular carcinoma (resulting from hepatitis B infection). For example, cervical cancer is more frequent in some countries because of infrequent or absent Pap screening programs (Table 3).
TABLE 3 Recommendations for Health Screening in Refugees
| Area | Specific screening recommendations |
|---|---|
| General history | Family status, trauma, anxiety, depression |
| Nutritional status | Dietary history, health habits (including use of tobacco and illicit substances), hemoglobin or hematocrit, height and weight |
| Physical examination | Blood pressure, oral and skin examination, signs of trauma |
| Infectious disease, review of previous immigrations | Check stool for ova and parasites, hepatitis serology, VDRL and HIV (as indicated) |
| Cancer | Age-appropriate screening for cancers that are often not screened for in Third World countries (e.g., Papanicolaou smears) |
HIV = human immunodeficiency virus.
Medical-Legal Issues
The legal issues confronting refugees depend on their status—whether they are in a foreign country seeking a refugee visa for the United States or have already gained entry to the United States and are applying for asylum. Often unofficial refugees fleeing persecution arrive in this country undocumented and then apply for asylum. As with all other applicants for visas, persons who seek to come to this country as refugees are required to undergo a physical examination at a designated center.21 Applicants are deemed inadmissible if they have certain physical or mental defects, which include AIDS and active tuberculosis.22
Potential immigrants who have close relatives in the United States who are U.S. citizens or lawful permanent residents may apply for a waiver and be admitted to the United States, where they can receive treatment. The process of determining whether a waiver will be granted is often extremely slow. A drug addict is simply inadmissible until deemed “cured.”23 Once a person is admitted as a refugee, no further medical examination is required unless he or she was admitted with a waiver.
Frequently people who have not been granted official refugee status but are nonetheless fleeing persecution arrive in this country without documentation and later apply for asylum. The asylum process does not require a physical examination. If asylum is not granted, the refugee is generally deported. Those who are granted asylum status may apply for permanent residence a year later, at which time they are required to have a physical examination. They are then subject to the same rules of inadmissibility as those who seek a refugee visa from abroad.24 If they do not apply or do not qualify for permanent residence, asylum status continues unless it has been determined that conditions in their home country have changed sufficiently that their danger of persecution has passed. At that point, they may be required to leave the United States.
Eligibility for medical services may be limited by recent legislation. Under the Welfare Reform Act of 1996, states will determine whether to provide Medicaid and Aid to Families with Dependent Children to permanent legal residents, and medical assistance and Women, Infants, and Children (WIC) support to pregnant women and children. In California, Proposition 187 calls for publicly funded health care facilities to deny care to illegal immigrants and to report them to government officials. The public health implications of such a policy are concerning, particularly with respect to infectious epidemics, tuberculosis control and prenatal care.25 The American Academy of Family Physicians in 1995 took a position opposing legislation that requires a physician to verify a patient's immigration status and opposing the implementation of California Proposition 187.26
Challenges for Health Service Delivery Systems
Cultural Aspects
Refugees often face communication barriers not always completely resolved by using family members as interpreters.27 Concerns about confidentiality and the potential modification of content arise. Finding suitable interpretation services can be challenging. People from different cultures often have a different understanding of health and may have culturally bound health problems. Often continuing to operate in “crisis mode,” refugees may not easily understand or accept routine office visits, the appointment process and the reimbursement mechanisms of our health care system. The family physician will need to become somewhat familiar with the refugee culture. A refugee may have different ways of expressing anxiety and emotions, such as the limited verbal self-revelation that is common in some cultures. Even bicultural interpreters may play into prevalent stereotypes of a particular culture.
Refugees are often seen as “somatisizers” who express underlying psychologic problems in terms of physical complaints. However, it seems that this issue is complex, because the way illness is expressed varies by culture. Refugees may fear stigmatization and deportation if they are found to have symptoms of “craziness” and thus may attempt to avoid such diagnoses. Also, it may be culturally appropriate to express illness in terms of physical symptoms rather than the psychodynamic constructions of stress that are more common in our own culture.
Mental Health Concerns
Psychologic pressures and physical events such as head injury can cause symptoms such as insomnia, memory loss, headaches, poor concentration and nightmares. Other common symptoms are anxiety, depression and fatigue. Traumatic effects on children also have been described, including withdrawal, fear, aggression and somatic complaints. Many children have witnessed violence to family members or have themselves been victims of violence.28 Most child survivors show psychologic symptoms more frequently than physical symptoms, as in the case of persons who have been tortured.
Post-traumatic stress disorder is one of the more dramatic problems physicians may encounter. This syndrome, which occurs after a traumatic event, can be divided into three categories of symptoms: (1) intrusive symptoms, (2) avoidance symptoms and (3) symptoms of increased arousal (Table 4).29 Standardized culture-specific instruments have been tested and validated in refugees.30
Community/Traditional Healing Resources
Refugees are typically shuffled by well-meaning sponsors to voluntary medical-care providers in an attempt to address the variety of symptoms they express. These symptoms may be an expression of the cultural incongruity felt by refugees in passively enduring modern hospitals and strange medical technology. An authoritarian assistance program may leave refugees feeling confined and dependent, increasing the effects of previous trauma. A self-empowerment strategy, however, that supports positive traditional values and resources may preserve a patient's sense of identity and enable socioeconomic independence. Community cohesiveness of ethnic groups has also been found to be protective.
A traditional healer can understand these patients within their cultural context, particularly within the collective cultural refugee experience. Traditional healers and community leaders are often able to restore links with the past as an antidote to cultural bereavement.31 Eisenbruch31 describes the ability of a traditional Cambodian healer to understand illness within its cultural context. Gilman and associates32 found that the Mien refugees from Southeast Asia living in California frequently used traditional healers. Since the Mien language has no words for mental illness, somatic complaints predominate among these patients. At their traditional ceremonies, ancestors are invoked and questioned about the involvement of spirits in the illness. Traditional therapies, whether herbal or other, as well as Western modalities, can be used in the treatment of refugee patients.
Health Effects of Torture
Perhaps the most devastating experience refugees have faced is torture. Torture and other human rights abuses have been documented in more than 100 countries by Amnesty International.33 The U.S. medical community has a responsibility to condemn torture and other human rights abuses and to support the survivors who have entered our country.
Final Comment
Many family physicians encounter refugees and immigrants in their clinical practices. Common health problems among these patients include anxiety, depression, adjustment reactions, trauma and effects on the family. The particular presentation depends on the trauma experienced, and the patient's area of origin and ability to adapt to a strange environment. Recommendations to physicians include screening refugees for traumatic experiences, nutritional status, infectious diseases and cancer. Survivors of torture have specific physical and psychologic effects, including post-traumatic stress disorder. Family physicians have a responsibility to protect populations from the introduction of infectious diseases, while providing compassionate care to recent arrivals in this country.

