Atopic dermatitis is a common, potentially debilitating condition that can compromise quality of life. Its most frequent symptom is pruritus. Attempts to relieve the itch by scratching simply worsen the rash, creating a vicious circle. Treatment should be directed at limiting itching, repairing the skin and decreasing inflammation when necessary. Lubricants, antihistamines and topical corticosteroids are the mainstays of therapy. When required, oral corticosteroids can be used. If pruritus does not respond to treatment, other diagnoses, such as bacterial overgrowth or viral infections, should be considered. Treatment options are available for refractory atopic dermatitis, but these measures should be reserved for use in unique situations and typically require consultation with a dermatologist or an allergist.
A topic dermatitis is a chronic inflammation of the skin that occurs in persons of all ages but is more common in children. The condition is characterized by intense pruritus and a course marked by exacerbations and remissions.
Atopic dermatitis has been reported to affect 10 percent of children.1 In the United States alone, it is estimated that more than $364 million per year is spent on the treatment of childhood atopic dermatitis.2 Although the symptoms of atopic dermatitis resolve by adolescence in 50 percent of affected children, the condition can persist into adulthood. Poor prognostic features include a family history of the condition, early disseminated infantile disease, female gender and coexisting allergic rhinitis and asthma.3
Diagnosis
The diagnosis of atopic dermatitis is based on the findings of the history and physical examination. Exposure to possible exacerbating factors, such as aeroallergens, irritating chemicals, foods and emotional stress, should be investigated.
Unfortunately, no specific laboratory findings or histologic features define atopic dermatitis. Although elevated IgE levels are found in up to 80 percent of affected patients, IgE levels are also elevated in patients with other atopic diseases.4
The diagnostic features of atopic dermatitis are listed in Table 1. The diagnosis requires the presence of at least three major features and at least three minor features.5
TABLE 1 Diagnostic Features of Atopic Dermatitis*
| Major features | |
| Pruritus | |
| Chronic or relapsing dermatitis | |
| Personal or family history of atopic disease | |
| Typical distribution and morphology of atopic dermatitis rash: | |
| Facial and extensor surfaces in infants and young children | |
| Flexure lichenification in older children and adults | |
| Minor features | |
| Eyes | |
| Cataracts (anterior subcapsular) | |
| Keratoconus | |
| Infraorbital folds affected | |
| Facial pallor | |
| Palmar hyperlinearity | |
| Xerosis | |
| Pityriasis alba | |
| White dermatographism | |
| Ichthyosis | |
| Keratosis pilaris | |
| Nonspecific dermatitis of the hands and feet | |
| Nipple eczema | |
| Positive type I hypersensitivity skin tests | |
| Propensity for cutaneous infections | |
| Elevated serum IgE level | |
| Food intolerance | |
| Impaired cell-mediated immunity | |
| Erythroderma | |
| Early age of onset | |
*—The diagnosis of atopic dermatitis should be suspected if three major criteria and three minor criteria are present.
Pruritus is a universal finding in atopic dermatitis. The pruritus can be severe, sometimes causing sleep disruption, irritability and generalized stress for affected patients and family members. Pruritus leads to scratching that results in secondary skin changes such as lichenification (thick accentuation of skin lines), excoriation and breakdown of the skin barrier. Consequently, atopic dermatitis has been referred to as “the itch that rashes” rather than the “rash that itches.”
The skin lesions observed in atopic dermatitis vary greatly, depending on the severity of inflammation, different stages of healing, chronic scratching and frequent secondary infections. Acute lesions are papules and vesicles on a background of erythema. Subacute lesions may develop scales and lichenification. Chronically involved areas become thick and fibrotic, and nodules often develop within the plaques (Figure 1). Lesions at any stage can develop secondary infections, which may resemble impetigo, with crusting and weeping lesions. When the lesions resolve, areas of hyperpigmentation or hypopigmentation persist.6
FIGURE 1.
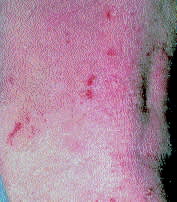
Nodules indicating chronic involvement of the skin in an adult with atopic dermatitis.
Xerosis (dry skin) is another characteristic skin finding in patients with atopic dermatitis. Because xerotic skin is unable to hold moisture, it is less pliable and more likely to crack and fissure. Resultant skin barrier breakdown increases susceptibility to irritation and infection.7 Reversing xerosis is one of the key elements in the treatment of atopic dermatitis.
In infants and young children with atopic dermatitis, pruritus commonly is present on the scalp, face (cheeks and chin) and extensor surfaces of the extremities (Figures 2 and 3). Older children and adults typically have involvement of the flexor surfaces (antecubital and popliteal fossa), neck, wrists and ankles (Figure 4). The presence of extensor distribution in older children and adults indicates a poor prognosis for ultimate cure.8
FIGURE 2.
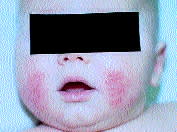
Typical facial rash of atopic dermatitis in a white infant.
FIGURE 3.
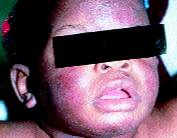
Characteristic facial rash in a black infant with atopic dermatitis.
FIGURE 4.
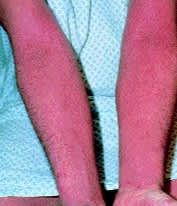
Extremity rash typifying the morphology and distribution of atopic dermatitis lesions in older children and adults.
Common periocular findings include periorbital hyperpigmentation and Dennie-Morgan folds (prominent folds of skin under the lower eyelid). Anterior subcapsular cataracts develop in 4 to 12 percent of patients with atopic dermatitis. Posterior cataracts are usually a side effect of oral corticosteroid therapy or of topical corticosteroids used in the periorbital area.9
From 50 to 80 percent of patients with atopic dermatitis have or develop asthma or allergic rhinitis. Nearly 70 percent of patients have a positive family history of atopy. Even if atopic dermatitis resolves with age, the predisposition for asthma and rhinitis persists.10
Pathogenesis and Etiology
The pathogenesis of atopic dermatitis is unknown, but the disease seems to be the result of genetic susceptibility, immune dysfunction and epidermal barrier dysfunction.11 The most current theory is that an unidentified genetic abnormality causes increased levels of cyclic adenosine monophosphate (cAMP) phosphodiesterase, which in turn leads to low levels of intracellular cAMP, a secondary messenger controlling cell activity. This change in the level of intracellular cAMP causes basophils and mast cells to be hyper-reactive, with the end result being increased histamine and leukotriene production and release. T cells are predominantly T-helper-2 subtype cells, which predispose to atopy.6,12–14
Foods, chemicals and aeroallergens may play a role in the pathogenesis and exacerbation of atopic dermatitis. However, the exact roles of aeroallergens and food allergy are controversial because of limitations of the in vitro radioallergosorbent test (RAST) and prick skin test. Both tests have a nearly 90 percent negative predictive value for atopic dermatitis, but their positive predictive value is less than 50 percent because of frequent false-positive results.15
Exposure to aeroallergens such as pollens, molds, mites and animal dander appears to be important in some patients with atopic dermatitis. Substantial clinical improvement may occur when these patients are removed from environments that contain the allergens to which they react.16 If food or aeroallergen sensitivity is suspected, patients should be evaluated with in vitro RAST or prick skin testing and possibly a withdrawal diet or controlled food challenge test.
Secondary Infections
Staphylococcal and streptococcal infections are common complications of atopic lesions. Heightened susceptibility occurs because the skin of patients with atopic dermatitis is a poor barrier against organisms, has depressed immune function and lacks normal lipophilic bacteria.17
Patients with atopic dermatitis are at increased risk for widespread herpes simplex virus infection (Kaposi's varicelliform eruption). In this infection, painful vesicles on an erythematous base can arise in areas of dermatitis or on normal-appearing skin. Constitutional symptoms can also develop. Treatment with acyclovir (Zovirax) is indicated to prevent complications.17
Differential Diagnosis
Because the skin lesions in atopic dermatitis can take many forms (papules, vesicles, plaques, nodules and excoriations), the differential diagnosis of atopic dermatitis is extensive. Conditions that need to be considered in patients with pruritus include seborrheic dermatitis, psoriasis and neurodermatitis. Features that distinguish these and other conditions from atopic dermatitis are listed in Table 2.
TABLE 2 Differential Diagnosis of Atopic Dermatitis
| Disease | Distinguishing features |
|---|---|
| Seborrheic dermatitis | Greasy, scaly lesions, absence of family history |
| Psoriasis | Localized patches on extensor surfaces, scalp, buttocks; pitted nails |
| Neurodermatitis | Usually, a single patch in an area accessible to itching; absence of family history |
| Contact dermatitis | Positive exposure history, rash in area of exposure, absence of family history |
| Scabies | Papules, finger web involvement, positive skin scraping |
| Systemic diseases | Findings on complete history and physical examination vary by disease |
| Dermatitis herpetiformis | Vesicles over extensor areas and associated enteropathy |
| Dermatophyte infection | Serpiginous plaques with central clearing, positive potassium hydroxide preparation |
| Immunodeficiency disorder | History of recurrent infection |
Systemic illnesses such as malignancy, thyroid disorders and hepatic or renal failure can also cause pruritus and excoriations. In adults with new-onset pruritus, a thorough history and a complete physical examination are necessary to exclude systemic disease.18
Occasionally, a patient with skin lesions and a history consistent with atopic dermatitis will have contact dermatitis. If the history reveals exacerbation of the rash after contact with a particular substance or if standard therapy is unsuccessful, patch testing to identify a cause of allergic contact dermatitis may be indicated.19
Treatment
The treatment of atopic dermatitis targets underlying skin abnormalities such as xerosis, pruritus, superinfection and inflammation (Figure 5). Patients should also be educated about the chronic nature of the disease and the need for continued adherence to proper skin care.
FIGURE 5. Treatment of Atopic Dermatitis
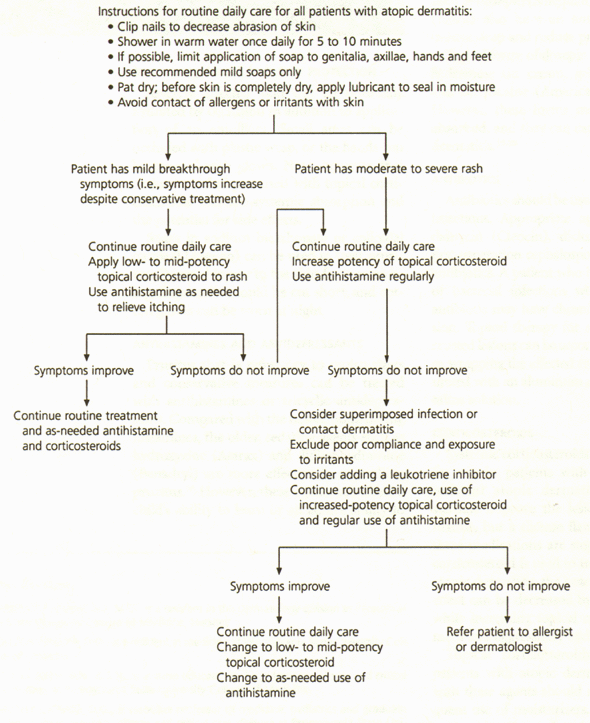
Treatment of atopic dermatitis.
BATHING AND MOISTURIZERS
A reasonable recommendation for bathing is once daily with warm (not hot) water for approximately five to 10 minutes. Soap should not be used unless it is needed for the removal of dirt. In this situation, the use of a mild cleanser (e.g., Dove, Basis, Kiss My Face or Cetaphil) is recommended.
Immediately after bathing (and before the skin is completely dry), patients should apply a moisturizer liberally (e.g., Aquaphor, Eucerin, Moisturel, mineral oil or baby oil). Ointments are superior to creams and lotions, but they are greasy and therefore poorly tolerated. Creams are effective and better tolerated than ointments. Lotions are least effective because of their alcohol content.8
OCCLUSION, SOAKS AND SKIN PROTECTION
Severely affected skin can be optimally hydrated by occlusion in addition to application of an emollient. Small areas can be occluded with plastic wrap, or the hands can be covered with gloves. Note, however, that occlusive techniques used with topical corticosteroids increase systemic absorption and the potential for side effects.
Soaks in sodium bicarbonate or colloidal oatmeal (Aveeno) can be used to treat pruritus. To avoid injury to the skin from scratching, fingernails should be cut short, and cotton gloves can be worn at night.
ANTIHISTAMINES AND ANTIDEPRESSANTS
Pruritus that is refractory to moisturizers and conservative measures can be treated with antihistamines or tricyclic antidepressants. Compared with the newer, nonsedating histamines, the older, sedating agents such as hydroxyzine (Atarax) and diphenhydramine (Benadryl) are more effective in controlling pruritus.20 However, these agents can affect a child's ability to learn or an adult's ability to drive and work.21 If drowsiness is a problem, a nonsedating antihistamine can be tried to see if it is effective. Tricyclic antidepressants such as doxepin (Sinequan) and amitriptyline (Elavil) also have an antihistaminic effect, induce sleep and reduce pruritus.22
Topical forms of doxepin (Zonalon), diphenhydramine (in cream, gel or spray forms) and benzocaine (Americaine) are available. However, these forms may be systemically absorbed, and they can cause allergic contact dermatitis.19,23
ANTIBIOTICS
Antibiotics should be used to treat secondary infections. Appropriate agents include clindamycin (Cleocin), dicloxacillin (Pathocil), first-generation cephalosporins and macrolide antibiotics. A patient who has continued flares of bacterial infections when not taking an antibiotic may have chronic immunosuppression. Topical therapy for secondarily infected crusted lesions can be accomplished by soaking or wrapping the affected areas using cloths saturated with an aluminum acetate solution or a saline solution.
CORTICOSTEROIDS
Systemic corticosteroids should be reserved for use in patients with severe treatment-resistant atopic dermatitis. Oral corticosteroids improve the lesions of atopic dermatitis, but a disease flare may occur when these medications are stopped. If a systemic corticosteroid is used to treat a severe flare of atopic dermatitis, the potential for a rebound effect can be decreased by tapering the drug while increasing topical corticosteroid treatment and aggressively hydrating the skin.24
Topical corticosteroids are effective in patients with atopic dermatitis, but therapy with these agents should not replace the frequent use of moisturizers. The local and systemic side effects of topical steroids are well recognized. Local effects include skin atrophy, striae, telangiectasias, hypopigmentation, rosacea, perioral dermatitis and acne. Systemic side effects include adrenal suppression, cataracts, glaucoma and growth retardation in children.
The risk of side effects from corticosteroids depends on multiple factors, including the potency of the steroid, the vehicle, the amount of steroid used, the concomitant use of occlusion, the area being covered and the integrity of the skin. The greatest penetration occurs with steroid use on the groin and face; the lowest penetration occurs with application on the palms and soles.25
Topical corticosteroids are grouped into seven potency categories, with group 1 containing the most potent agents and group 7 containing the least potent agents. A general principle in treating atopic dermatitis with topical steroids is to use the least potent agent possible and limit the frequency of application.
Compared with adults, children (especially infants) are at higher risk for the local and systemic side effects of topical corticosteroids. Thus, it is reasonable to use a group 6 or 7 steroid initially in infants and for intertriginous areas in patients of any age. If the dermatitis is severe and a more potent steroid is needed, the patient should be followed closely, and the strength of the steroid should be reduced as skin lesions improve.
Use of a mid-potency topical corticosteroid (group 4 or 5) is appropriate for nonintertriginous areas in children and adults. Group 1 and 2 steroids are best reserved for use on thickened plaques and for the palms and soles.
Group 1 steroids are generally best avoided in children under 12 years of age or for use with occlusion.
Topical steroids come in many vehicles, including solutions, lotions, creams, gels and ointments. The thicker preparations (ointments) penetrate the epidermis better. The same steroid in a different vehicle can differ in potency by one or two classes. Some areas of the body dictate the type of vehicle needed. For example, the scalp is best treated with solutions and lotions. Occlusion should be limited to isolated resistant areas because it significantly increases the absorption of topical steroids.9
TAR PREPARATIONS
Tar preparations have anti-inflammatory and antipruritic effects on the lesions of atopic dermatitis. These preparations are effective when used alone or with topical corticosteroids. Some tar preparations, especially gels, may contain alcohol and thus can be irritating. Shampoos, bath solutions and creams are less irritating.9 Tar preparations can be purchased over the counter (e.g., Cutar, Aquatar, Estar).
The disadvantages of tars are their odor and dark staining color. Using the products at night and covering the treated areas can decrease these problems.
PHOTOTHERAPY
Phototherapy is effective in treating refractory atopic dermatitis. This treatment may be administered as ultraviolet A (UVA), ultraviolet B (UVB) or combined UVA and UVB. Psoralen plus UVA (PUVA) photochemotherapy may be a treatment option in patients with extensive refractory disease.25
LEUKOTRIENE INHIBITORS
The U.S. Food and Drug Administration has labeled leukotriene inhibitors such as zileuton (Zyflo), zafirlukast (Accolate) and montelukast (Singulair) for the treatment of asthma. Because asthma and atopic dermatitis have a similar pathogenesis, leukotriene inhibitors may have a role in the treatment of atopic dermatitis.
A recent report described four patients with atopic dermatitis who responded to zafirlukast therapy.26 Montelukast should not be used in children under six years of age, and zafirlukast should not be given to children under 12 years of age.
IMMUNOSUPPRESSANTS AND ANTINEOPLASTICS
Cyclosporine (Sandimmune) has been effective in patients with refractory atopic dermatitis. The condition returns after the cessation of therapy, although not always at the original level of severity.27
Tacrolimus (Prograf), which is used in an oral form to prevent organ transplantation rejection, is also available in a topical form. This topical agent appears to be effective in the treatment of refractory atopic dermatitis, with few adverse effects.5
Azathioprine (Imuran) may also be efficacious in patients with atopic dermatitis. Treatment with this immunosuppressant is more cost-effective than therapy with cyclosporine or tacrolimus.28
Finally, a recent case series that included 24 patients with atopic dermatitis who were treated with human interferon gamma for two years demonstrated both safety and efficacy for this therapy.29 To date, however, large placebo-controlled studies are lacking.

