The accurate differentiation of gallstone-induced biliary colic from other abdominal disease processes is the most crucial step in the successful management of gallstone disease. Despite the availability of many imaging techniques to demonstrate the presence of gallstones, clinical judgment ultimately determines the association of symptoms with cholelithiasis and its complications. Adult patients with silent or incidental gallstones should be observed and managed expectantly, with few exceptions. In symptomatic patients, the intervention varies with the type of gallstone-induced complication. In this article, we review the salient clinical features, diagnostic tests and therapeutic options employed in the management of gallstones and their complications.
Gallstones are a major cause of morbidity worldwide, and cholecystectomy is the most commonly performed abdominal surgery in medicine. Gallstone-induced complications have a limited and overlapping pattern of clinical presentation.1
Pathogenesis of Gallstones
Gallstones found in the gallbladder are classified as cholesterol, pigmented or mixed stones, based on their chemical composition. Up to 90 percent of gallstones are cholesterol (more than 50 percent cholesterol) or mixed (20 to 50 percent cholesterol) gallstones. The remaining 10 percent of gallstones are pigmented stones, which have less than 20 percent cholesterol.
The basic mechanism underlying the formation of gallstones is supersaturation, with constituents in bile exceeding their maximum solubilities.2,3 Additional factors contributing to gallstone formation are nucleation factors, bile stasis within the gallbladder and calcium in bile. Biliary cholesterol usually exists in a soluble single phase as micellar cholesterol. As the cholesterol concentration increases, cholesterol crystals begin to form.
Mucin and a soluble glycoprotein are potential nucleation factors. Prostaglandins stimulate the synthesis and secretion of bile mucin. Inflammation and other stimuli, which enhance prostaglandin secretion, increase the risk for gallstone formation. Biliary sludge, also referred to as microlithiasis, is a viscous gel composed of mucin, precipitates of cholesterol and calcium bilirubinate. Gallstone formation is usually preceded by the presence of biliary sludge.4 Therefore, sludge should be regarded as part of the spectrum of gallstone disease. Retarded or incomplete emptying of bile from the gallbladder can promote sludge formation. The risk factors for gallstone formation are summarized in Table 1.
TABLE 1 Risk Factors for Gallstone Formation
| Age | Increasing age* |
| Body habitus | Obesity, rapid weight loss |
| Childbearing | Pregnancy |
| Drugs | Fibric acid derivatives (or fibrates), contraceptive steroids, postmenopausal estrogens, progesterone, octreotide (Sandostatin), ceftriaxone (Rocephin) |
| Ethnicity | Pima Indians, Scandinavians |
| Family | Maternal family history of gallstones |
| Gender | Females |
| Hyperalimentation | Total parenteral nutrition,† fasting |
| Ileal and other metabolic diseases | Ileal disease (Crohn's disease), resection or bypass,* high triglycerides, diabetes mellitus, chronic hemolysis,* alcoholic cirrhosis,* biliary infection,* primary biliary cirrhosis, duodenal diverticula,* truncal vagotomy, hyperparathyroidism, low level of high-density lipoprotein cholesterol |
*—Risk factors for pigment gallstone formation.
†—Risk factor for cholesterol and pigment gallstone formation.
People with diabetes have a propensity for obesity, hypertriglyceridemia and gallbladder hypomotility. Therefore, it has been difficult to prove that diabetes is an independent risk factor for gallstone formation. However, some studies have shown an increased prevalence (without statistical significance) of diabetes in patients with gallstones.5
Common bile duct stones (choledocholithiasis) may form de novo in bile ducts (primary, 5 percent of common bile duct stones) or migrate to the common bile duct from the gallbladder (secondary, 95 percent of common bile duct stones). Composition of gallstones in the common bile duct is usually the same as that of gallstones in the gallbladder, although some bile duct stones are softer and more brownish because of deposition of calcium bilirubinate and other calcium salts caused by the bacterial deconjugation of bilirubin and hydrolysis of phospholipids. Primary common bile duct stones are more common in Asian populations because of the increased prevalence of flukes and parasitic infections, such as clonorchiasis, fascioliasis and ascariasis.
Clinical Presentations
The clinical presentation of gallstone-induced complications varies. Differentiating features such as pain site and duration, presence or absence of a mass, fever and laboratory parameters can assist in establishing the correct diagnosis (Table 2).
TABLE 2 Differentiating Features of Gallstone-Induced Complications*
| Feature | Biliary colic | Acute cholecystitis | Chronic cholecystitis | Cholangitis | Pancreatitis |
|---|---|---|---|---|---|
| Pain site | Epigastrium | RUQ | RUQ | RUQ | Epigastric |
| Pain duration | < 3 hours | > 3 hours | Variable | Variable | Variable |
| Mass | No masses | RUQ mass | No masses | ± | ± |
| Fever | – | ± | ± | ± | ± |
| Increased WBC | – | ± | ± | ± | ± |
| Increased amylase level | Normal | ± | – | ± | + |
RUQ = right upper quadrant; WBC = white blood cell count; + = present; – = absent; ± = present or absent.
*—These characteristics may not always be present.
BILIARY COLIC
As many as one third of patients with gallstones will develop symptoms (Table 3). It is thought that the pain of biliary colic is caused by the functional spasm of the cystic duct when obstructed by stones, whereas pain in acute cholecystitis is caused by inflammation of the gallbladder wall.6 Pain often develops without any precipitating symptoms. Typically, the pain has a sudden onset and rapidly increases in intensity over a 15-minute interval to a plateau that can last as long as three hours. The pain may radiate to the interscapular region or to the right shoulder.
TABLE 3 Complications of Gallstones*
| Complication | Percentage |
|---|---|
| Biliary colic | 70 to 80† |
| Acute cholecystitis | 10 |
| Emphysematous cholecystitis | <1‡ |
| Mirizzi's syndrome | <1‡ |
| Hydrops of the gallbladder | <1‡ |
| Small bowel obstruction (gallstone ileus) | 1‡ |
| Gastric outlet obstruction (Bouveret's syndrome) | <1‡ |
| Perforation of gallbladder | 12‡ |
| Acute biliary pancreatitis | — |
| Acute suppurative/obstructive cholangitis | — |
*—One third of patients with gallstones develop symptoms.
†—Percentage incidence in patients with symptomatic gallstones.
‡—Percentage incidence in patients with acute cholecystitis.
It is worthwhile to clarify some misconceptions about biliary pain. First, biliary colic is a misnomer, because the pain is steady, not colicky. Second, the pain site is primarily in the epigastrium, and it is incorrect to interpret pain located in the epigastrium as nonbiliary. Third, fat intolerance is not a feature of biliary colic.
ACUTE CHOLECYSTITIS
The most common cause of acute cholecystitis is obstruction of the cystic duct by gallstones, resulting in acute inflammation. Approximately 90 percent of cases of acute cholecystitis are associated with cholelithiasis. The clinical features of acute cholecystitis may include symptoms of local inflammation (e.g., right upper quadrant mass, tenderness) and systemic toxicity (e.g., fever, leukocytosis). Most patients with acute cholecystitis have had previous attacks of biliary pain. The pain of acute cholecystitis typically lasts longer than three hours and, after three hours, shifts from the epigastrium to the right upper quadrant. This sequence of clinical features includes visceral pain from ductal impaction by stones, progressing to inflammation of the gallbladder with parietal pain.
In elderly patients, localized tenderness may be the only presenting sign; pain and fever may be absent.7 In 30 to 40 percent of patients, the gallbladder and adherent omentum can be perceived as a palpable mass. Jaundice is noted in approximately 15 percent of patients with acute cholecystitis, even without choledocholithiasis. The pathogenesis may involve edema and inflammation secondary to the impacted stone in the cystic duct. This leads to the compression of the common hepatic duct or the common bile duct (Mirizzi's syndrome).
In the event of delayed diagnosis in the setting of acute cholecystitis, the cystic duct remains obstructed, and the lumen may become distended with clear mucoid fluid (hydrops of the gallbladder). Although rare, a large gallstone in the gallbladder will sometimes erode through the gallbladder wall into an adjacent viscus, usually the duodenum. Subsequently, the stone may become impacted in the terminal ileum (small bowel obstruction) or in the duodenal bulb/pylorus, causing gastric outlet obstruction (Bouveret's syndrome). Patients with chronic cholecystitis usually have had repeated attacks of biliary pain or acute cholecystitis. This results in a thickened and fibrotic gallbladder that may not be palpable in these patients.
Acute cholecystitis may present as an acalculous disorder in 5 to 10 percent of patients. Acalculous cholecystitis typically affects critically ill, older men in the setting of major surgery, critical illness, total parenteral nutrition, extensive trauma or burn-related injury. The pathogenesis probably involves a combination of biliary stasis, chemical inflammation and ischemia. Complications develop more frequently in acalculous cholecystitis than in calculous cholecystitis.
Rarely, infectious agents can cause acute cholecystitis. Cytomegalovirus and cryptosporidia can result in cholecystitis and cholangitis in immunocompromised persons. Salmonella can colonize the gallbladder epithelium without eliciting inflammation, creating a carrier state.
CHOLEDOCHOLITHIASIS
Acute suppurative cholangitis is a common complication of choledocholithiasis. The usual clinical presentation, occurring in 70 percent of the cases of choledocholithiasis, consists of pain, jaundice and chills (i.e., Charcot's triad). Refractory sepsis characterized by altered mentation, hypotension and Charcot's triad constitutes Raynold's pentad. Depending on the progression of the illness, endotoxemia with shock or multiple liver abscesses may be noted. On the other hand, cholangitis may be a short, self-limited illness complicating choledocholithiasis. The most commonly found organisms are Escherichia coli, Klebsiella, Pseudomonas and enterococci, with a 15 percent contribution by anaerobes.
Acute biliary pancreatitis is another potential complication of choledocholithiasis.8 Differentiating acute pancreatitis from cholecystitis can be difficult because both conditions produce tenderness in an overlapping area. Although acute cholecystitis alone can be associated with hyperamylasemia, pancreatitis often has higher enzyme levels. Also, cholecystitis and pancreatitis may coexist.
Diagnostic Studies
A wide array of laboratory and radiologic studies is used for the evaluation of gallstones located in the gallbladder and the common bile duct. There are strengths and limitations to each diagnostic test.
LABORATORY TESTS
In uncomplicated biliary colic, there are usually no accompanying changes in hematologic and biochemical tests. In acute cholecystitis, leukocytosis with a “left shift” is usually observed. Serum aminotransferase, alkaline phosphatase, bilirubin and amylase levels may also be elevated. The most reliable indicator of gallstones as the cause of acute pancreatitis is an elevation of alanine aminotransferase levels greater than 2.5 times above normal.8
ULTRASONOGRAPHY
Ultrasonography should be a routine examination for the confirmation or exclusion of gallstone disease. Ultrasonography provides more than 95 percent sensitivity and specificity for the diagnosis of gallstones greater than 2 mm in diameter. Ultrasonography of the gallbladder should follow a fast of at least eight hours because gallstones are visualized better in a distended, bile-filled gallbladder.
Ultrasonography is less sensitive for the diagnosis of choledocholithiasis and may document only one half of common bile duct stones.9 Ultrasound scans may indicate dilatation of intrahepatic or extrahepatic bile ducts, which is highly suggestive of distal obstruction, with a sensitivity of 76 percent. Ultrasonographic findings that are suggestive of acute cholecystitis include the following: pericholecystic fluid (in the absence of ascites); gallbladder wall thickening greater than 4 mm (in the absence of hypoalbuminemia); and sonographic Murphy's sign (abrupt arrest of breathing during the inspiration phase secondary to pain elicited by placing the ultrasound probe in the right upper quadrant).
ENDOSCOPIC RETROGRADE CHOLANGIOPANCREATOGRAPHY
Endoscopic retrograde cholangiopancreatography (ERCP) is the best method for determining a diagnosis of choledocholithiasis.10 ERCP provides diagnostic and therapeutic options, and has a sensitivity and specificity of 95 percent for the detection of common bile duct stones.
BILE MICROSCOPY
It is essential that gallbladder bile (induced by cholecystokinin), rather than hepatic or ductal bile, be obtained to maximize sensitivity for detecting sludge. A bile sample may be obtained by aspiration through the catheter during ERCP. Bile must be centrifuged and examined under polarizing or light microscopy for detection of precipitates.
COMPUTED TOMOGRAPHY AND MAGNETIC RESONANCE IMAGING
The latest computer technology, processing computed tomographic (CT) and magnetic resonance imaging (MRI) data into a three-dimensional image of the bile duct, is now comparable to the ERCP in terms of diagnostic accuracy.11,12 Although CT and MRI provide the advantage of noninvasiveness, they offer no therapeutic options.
HEPATOBILIARY SCINTIGRAPHY
Hepatobiliary scintigraphy can confirm or exclude the diagnosis of acute cholecystitis with a high degree of sensitivity and specificity.13 After a two- to four-hour fast, the patient is given an intravenous injection of a technetium-99m–labeled iminodiacetic acid derivative (IDA agent) that is excreted into the bile ducts and sequentially imaged under a gamma camera.
In a normal study, images of the gallbladder, common bile duct and small bowel appear within 30 to 45 minutes.14 A normal Tc-99m-IDA scan virtually rules out the diagnosis of acute cholecystitis in patients who present with abdominal pain. An abnormal or “positive” Tc-99m-IDA scan can be defined as non-visualization of the gallbladder with preserved excretion into the common bile duct and small bowel. Failure to image the gallbladder within 90 minutes despite adequate views of the liver, common bile duct and small bowel strongly suggests acute obstruction of the cystic duct. False-positive findings can result from nonfasting or prolonged fasting states,14 chronic alcoholism and chronic cholecystitis. Repeat scanning after four or more hours decreases the false-positive rate.
In patients with acute acalculous cholecystitis, prolonged fasting may result in viscous (concentrated) bile and a false-positive hepatobiliary scan. Alternatively, patients with acalculous cholecystitis may not have an obstructed cystic duct, resulting in a false-negative hepatobiliary scan. False-positive results occur more frequently than false-negative results. The hepatobiliary scan has a sensitivity greater than 90 percent, but the lack of specificity in fasting, critically ill patients limits the use of the hepatobiliary scan to exclusion of acute acalculous cholecystitis rather than confirmation of the diagnosis.
Management
Cholelithiasis can be diagnosed in a variety of clinical circumstances. A patient can be asymptomatic, have a history of one or more uncomplicated biliary pain episodes or have complications of acute cholecystitis, gangrene, jaundice or even gallbladder cancer.
ASYMPTOMATIC GALLSTONES
It is estimated that 60 to 80 percent of all gallstones are asymptomatic at some point.15 Adult patients with silent or incidental gallstones should be observed and managed expectantly, including patients with diabetes.16 In diabetic patients, the natural history of gallstones is generally benign, and there is low risk of a major complication.15 There is no evidence to suggest that prophylactic cholecystectomy prolongs life expectancy. However, prophylactic cholecystectomy should be performed in patients at high risk of gallbladder carcinoma (Figure 1). The specific groups at high risk of gallbladder cancer include patients with asymptomatic gallstones who are Pima Indians or who have a calcified gall-bladder, gallbladder polyps greater than 10 mm, gallstones greater than 2.5 cm or anomalous pancreaticobiliary ductal junction, and carriers of Salmonella typhosa.
FIGURE 1. Management of Gallstones
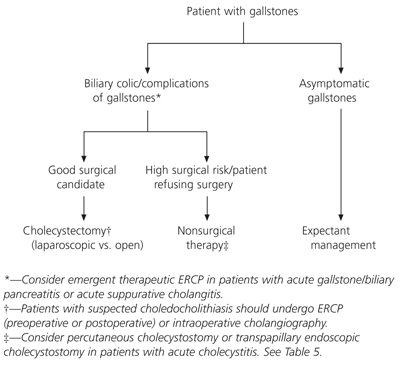
Management of gallstones and its complications. (ERCP = endoscopic retrograde cholangiopancreatography)
SYMPTOMATIC GALLSTONES
Once an episode of biliary colic has occurred, there is a high risk of repeated pain attacks. Cohort studies with follow-up of patients with symptomatic gallstones indicate a 38 to 50 percent incidence rate of recurrent biliary pain per year.17 Patients with symptomatic gallstones are more likely to develop biliary complications.18 The risk of developing biliary complications is estimated to be 1 to 2 percent per year.
As many as 30 percent of patients who are observed for several years do not have further problems. Therefore, a management plan is dependent on the patient's decision and surgical candidacy. For patients who do not want to risk the possibility of a future attack, a laparoscopic cholecystectomy is recommended.
In the 1980s, considerable interest was generated in the evaluation of nonsurgical treatment strategies for gallstone disease. Nonoperative therapy is costly and time-consuming, and should be reserved for use in the symptomatic patient who declines surgery or has a high operative risk19,20 (Table 4).
TABLE 4 Nonoperative Therapies for Symptomatic Gallstones
| Agent | Advantages | Disadvantages |
|---|---|---|
| Oral bile acid dissolution: ursodeoxycholic acid (Actigall), at 8 to 10 mg per kg per day | Stone clearance: 30 to 90 percent with zero percent mortality | 50 percent recurrence of stones; dissolves noncalcified cholesterol stones; optimal for stones < 5 mm; symptom relief does not start for 3 to 6 weeks; may take 6 to 24 months for results |
| Contact solvents: methyl tert-butyl ether/ n-propyl acetate | Stone clearance: 50 to 90 percent | 70 percent recurrence of stones; experimental, with insufficient data; duodenitis; hemolysis; nephrotoxicity; mild sedation |
| Extracorporeal shock-wave lithotripsy: electrohydraulic/electromagnetic | Stone clearance: 70 to 90 percent with < 0.1 percent mortality | 70 percent recurrence; not approved by FDA; performed only at centers with expertise; selection criteria require no more than one radiolucent stone (< 20 mm in diameter), patent cystic duct, functioning gallbladder in a patient with symptomatic gallstones without complications |
FDA = U.S. Food and Drug Administration.
ACUTE CHOLECYSTITIS
Most physicians agree that early laparoscopic cholecystectomy (within 24 to 48 hours) is indicated once the diagnosis of acute cholecystitis is secure and the patient is hemodynamically stable. Use of this surgical technique is supported by large randomized trials conclusively demonstrating its clinical superiority over open cholecystectomy.21 The potential advantages of laparoscopic cholecystectomy include a marked reduction in postoperative pain, a shorter hospital stay and a more rapid return to work and usual activities. A percutaneous cholecystostomy or transpapillary endoscopic cholecystostomy should be considered in patients with acute cholecystitis who are at excessive risk for surgery22,23 (Table 5).
TABLE 5 Contraindications for Laparoscopic Cholecystectomy
| High risk for general anesthesia |
| Morbid obesity |
| Signs of gallbladder perforation such as abscess, peritonitis or fistula |
| Giant gallstones |
| End-stage liver disease with portal hypertension and severe coagulopathy |
| Suspected gallbladder malignancy |
| Last trimester of pregnancy |
CHOLEDOCHOLITHIASIS
When a patient with known gallbladder stones has concomitant choledocholithiasis, the management varies with the severity of clinical features.24,25 In general, the presence of obstructive cholangitis or jaundice with a dilated common bile duct detected by ultrasonography should lead promptly to a preoperative ERCP with possible sphincterotomy and stone extraction. Once the bile duct has been cleared by ERCP, the patient can undergo a routine laparoscopic cholecystectomy within one or two days. However, if liver enzyme levels are only mildly elevated and there is a low suspicion for common bile duct stones, many physicians proceed directly with laparoscopic surgery. In this case, intraoperative cholangiography should be performed to rule out choledocholithiasis. If common bile duct stones are present, they can be removed intraoperatively or by a postoperative ERCP.26

