Tinea infections are superficial fungal infections caused by three species of fungi collectively known as dermatophytes. Commonly these infections are named for the body part affected, including tinea corporis (general skin), tinea cruris (groin), and tinea pedis (feet). Accurate diagnosis is necessary for effective treatment. Diagnosis is usually based on history and clinical appearance plus direct microscopy of a potassium hydroxide preparation. Culture or histologic examination is rarely required for diagnosis. Treatment requires attention to exacerbating factors such as skin moisture and choosing an appropriate antifungal agent. Topical therapy is generally successful unless the infection covers an extensive area or is resistant to initial therapy. In these cases, systemic therapy may be required. Tinea corporis and cruris infections are usually treated for two weeks, while tinea pedis is treated for four weeks with an azole or for one to two weeks with allylamine medication. Treatment should continue for at least one week after clinical clearing of infection. Newer medications require fewer applications and a shorter duration of use. The presence of inflammation may necessitate the use of an agent with inherent anti-inflammatory properties or the use of a combination antifungal/steroid agent. The latter agents should be used with caution because of their potential for causing atrophy and other steroid-associated complications.
Tinea infections are superficial fungal infections caused by the three genera of dermatophytes, Trichophyton, Microsporum and Epidermophyton.1 Commonly, the infections caused by these organisms are named for the sites involved. Tinea capitis refers to a dermatophyte infection of the head, tinea barbae affects the beard area, tinea corporis occurs on the body surface, tinea manuum is limited to the hands, tinea pedis to the feet, and tinea unguium infects the toenails. These names do not distinguish between species (for example, tinea capitis may be caused by Trichophyton or Microsporum genera).
With some pertinent exceptions, dermatomycosis is typically confined to the superficial keratinized tissue2 and, thus, can often be treated with topical antifungal medications.3 Because these agents do not penetrate hair or nails, tinea capitis, tinea barbae, and tinea unguium usually require systemic therapy. This article focuses on the diagnosis and treatment of tinea infections with topical medications. Because tinea capitis and tinea unguium are not typically amenable to topical therapy, they will not be discussed in this article.
It is important to note that nondermatophytes and yeasts may infect the sites mentioned above. For example, tinea unguium is only a subset of the onychomycoses, which include other types of fungal infections of the nails. Similarly, tinea corporis refers only to dermatophyte infection of the skin and not other superficial fungal infections such as candidiasis. Although tinea versicolor is commonly called a tinea, it is caused by the non-dermatophyte Malassezia furfur (also referred to as Pityrosporum orbiculare and Pityrosporum ovale) and is not a true tinea infection.4
Epidemiology
Because tinea infections are highly common, it is likely that the primary care physician will frequently treat affected patients. The estimated lifetime risk of acquiring dermatophytosis (tinea infection) is between 10 and 20 percent.5 In the United States, dermatophytosis is second only to acne as the most frequently reported skin disease.6 The majority of superficial fungal infections are tineas and, of those, the most common are tinea pedis, tinea corporis, and tinea cruris.7 Trichophyton rubrum is the most likely agent in these dermatomycoses. T. rubrum accounted for 76.2 percent of all superficial fungal diseases in a representative sample of the U.S. population.8 With the exception of tinea capitis (in which Trichophyton tonsurans was the most likely etiologic agent), T. rubrum was the most common dermatophyte isolated in all superficial fungal diseases studied.8
Clinical Manifestations
Clinical presentation is the most important clue to accurate diagnosis and treatment. The anthrophilic dermatophytes (commonly isolated from human infection) are the most common source of human dermatomycoses. These tend to evoke a limited host response and are less likely to be accompanied by severe inflammation or to clear spontaneously.9 Occasionally, severe inflammation is a component of dermatophytosis. This is particularly true in the case of tinea infections caused by zoophilic species (commonly isolated from animal infection). The most common of these is Microsporum canis.
TINEA CORPORIS
Tinea corporis refers to tinea anywhere on the body except the scalp, beard, feet, or hands. This lesion presents as an annular plaque with a slightly raised and often scaly, advancing border and is commonly known as ringworm. Each lesion may have one or several concentric rings with red papules or plaques in the center. As the lesion progresses, the center may clear, leaving post-inflammatory hypopigmentation or hyperpigmentation.
TINEA CRURIS
Because it affects the groin area, tinea cruris is also known as “jock itch.” It is characterized by red scaling plaques on the medial thighs and inguinal folds (Figure 1). The plaques are typically bilateral but usually spare the penis and scrotum, in contrast to candidiasis.10 Many people with tinea cruris have coincident tinea pedis, and it has been postulated that the tinea cruris is spread by hand from the tinea pedis.11
FIGURE 1.
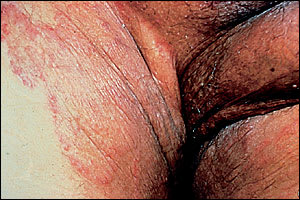
Tinea cruris with bilateral scaly patches on the inner thighs, sparing the penis.
TINEA PEDIS
Tinea pedis, or athlete's foot, is the most common dermatophyte infection (Figure 2). Its etiology is closely tied to the use of occlusive footwear.12 Most commonly, tinea pedis presents with toe-web maceration.13 This fairly subtle presentation is contrasted with the moccasin distribution affecting the soles and lateral feet that is often seen in patients with T. rubrum infection (Figure 3). In the latter cases, the feet tend to be hyperkeratotic with scale and some erythema (Figure 4). In some cases of tinea pedis, a dermatophytid (also known as “id”) reaction may occur in which small vesicles or pustules appear at distant sites. The id reaction may be the only manifestation of an otherwise asymptomatic webspace maceration and usually resolves with treatment of the primary fungal infection.
FIGURE 2.
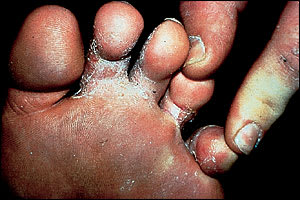
Tinea pedis presenting with toe-web maceration and minimal inflammation. A presentation like this may be accompanied by a dermatophytid (“id”) reaction.
FIGURE 3.
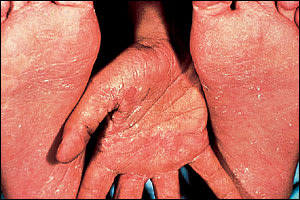
Moccasin distribution of tinea pedis with inflammation.
FIGURE 4.
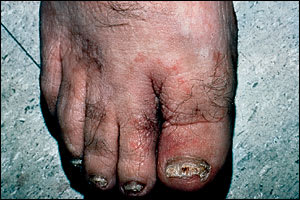
Tinea pedis with marked erythema of the first and second toes.
Diagnosis
The clinical suspicion of dermatophytosis can be confirmed with diagnostic tests. Because other entities may mimic tinea infection, treatment should not be initiated on the basis of clinical presentation alone. In most cases, a simple potassium hydroxide (KOH) preparation with mycologic examination under a light microscope can confirm the presence of dermatophytes. Occasionally, culture media (including indicator media) or histologic examination may be useful in making the diagnosis. A Wood's light is not helpful in diagnosing tinea infections of the skin and is mainly used to identify fungal elements in hairs infected with Microsporum, which is a less common dermatophyte. The latter fluoresce green under Wood's light. This light may also be helpful in diagnosing erythrasma by its coral-red fluorescence when this condition is part of the differential diagnosis of a tinea skin condition.14
KOH Preparation for Direct Microscopy
The KOH preparation, a relatively simple diagnostic method with excellent positive predictive value, is used to visualize the hyphae that characterize dermatophytes. Additional confirmatory tests are rarely needed for the diagnosis of tinea.15 The KOH helps dissolve the epithelial tissue, allowing the hyphae to be seen on microscopy.
Because the organisms live in the superficial keratinized tissue, a sample of scale should be visualized under low or medium power. Scale is collected from the active border of a lesion. This is done by scraping the lesion with the edge of a rounded scalpel blade or the edge of a glass slide. The debris is collected on another slide and concentrated in the middle. If a vesicle is being examined, it may be unroofed, and that material can be examined.
The slide should be covered with a cover slip, and KOH (5 to 20 percent) should be added to the side of the cover slip, allowing capillary action to draw the KOH to the scaly sample. The preparation may be heated gently over a flame to highlight the fungal elements. If dimethyl sulfoxide has been added to the KOH, heating is not required.
During examination of the sample, the condenser of the microscope should be in the down position. The presence of septate hyphae confirms the diagnosis of tinea. The examiner should make sure that hyphae are being seen rather than the edge of an epithelial cell. It is helpful to visualize the hyphae crossing the path of more than one cell.
If clinical decisions are to be made based on microscopic examination, practitioners must comply with Clinical Laboratory Improvement Amendments (CLIA) regulations. Performing KOH examinations requires a Provider–Performed Microscopy (PPM) certificate. Obtaining the latter requires completion of paperwork and does not require a site inspection. The American Academy of Dermatology publishes a handbook with directions for compliance with the PPM regulation.16
Culture
Mycologic culture is rarely indicated in the diagnosis of tineas other than tinea unguium and tinea capitis. In some cases, even though clinical suspicion is high, diagnosis may be a challenge. Culture, while relatively simple to perform, requires one to four weeks to grow and clinical expertise to interpret the result. The most common medium used for isolating dermatophytes is Sabouraud's peptone-glucose agar.1 Various formulations of this medium are commercially available; some have additives that inhibit bacterial and nondermatophyte growth.17 A dermatophyte test medium (DTM) indicator can also be used. The latter has the added advantage of a phenol indicator that turns red in the alkaline environment produced by dermatophytes.18 Although DTM has the advantage of simplicity, it has a high rate of false-positive and false-negative results.1
All media require collection of an adequate sample of infected material. Scale may be collected in a manner similar to that used for the KOH preparation or with a cotton swab. The swab must first be moistened with sterile water and then rubbed vigorously over the active border of the lesion. This method is best used when the lesion is not scaly or when the use of a blade or slide is impractical.19 The physician performing the culture must comply with stricter CLIA regulations. Performing cultures requires a level of certification that necessitates a laboratory inspection.
HISTOPATHOLOGIC EVALUATION
When the diagnosis of a dermatophyte infection remains in question after office testing or failure to respond to treatment, biopsy specimens may be submitted to a pathologist for evaluation. Fungal staining with periodic acid–Schiff highlights fungal elements.17
Treatment
Most tinea corporis, cruris, and pedis infections can be treated with topical agents. Consideration should be given to systemic treatment when lesions covering a large body-surface area fail to clear with repeated treatment using different topical agents.3 In treating dermatophytosis, the physician must also address environmental factors that lead to or exacerbate tinea infection and select an appropriate topical therapy for the infection.
NONPHARMACOLOGIC MEASURES
Because fungi thrive in moist warm environments, patients should be encouraged to wear loose-fitting garments made of cotton or synthetic materials designed to wick moisture away from the surface. Socks should have similar properties. Areas likely to become infected should be dried completely before being covered with clothes. Patients should also be advised to avoid walking barefoot and sharing garments.
NONSPECIFIC AGENTS
A variety of traditional agents without specific antimicrobial function are still in use, including Whitfield's ointment and Castellani's (carbol fuchsin solution) paint. The efficacy of these preparations has not been well quantified.
ANTIFUNGAL AGENTS
The antifungal agents can be grouped by structure and mechanism of action. The two principal pharmacologic groups are the azoles and the allylamines. Polyenes (amphotericin B [Fungizone] and nystatin [Mycostatin]) are not discussed in this article because this group of compounds is not effective in the treatment of dermatophyte infections. Other agents that do not fit into the two main groupings are tolnaftate (Tinactin), haloprogin (Halotex), ciclopirox (Loprox) and butenafine (Mentax).3
Because there are few direct comparisons of individual topical agents, it can be difficult to justify the choice of one preparation over another. This choice is made less clear because several genera and species may produce the same clinical condition. When treating a dermatophyte infection, it is unlikely that the physician will know the infecting species. In general, tinea corporis and tinea cruris require once- to twice-daily treatment for two weeks. Tinea pedis may require treatment for four weeks.3 Treatment should continue for at least one week after symptoms have resolved.17 Some of the newer agents require only once-daily application and shorter courses of treatment, and are associated with lower relapse rates.
The application area should include normal skin about 2 cm beyond the affected area. Guidelines regarding the optimal vehicle of treatment (e.g., cream, ointment, gel, or lotion) are given in Table 1.20 Ideally, an agent will provide clinical and mycologic cure, symptomatic relief, and low relapse rate, along with ease of use. In addition to specific anti-fungal properties, some preparations have antibacterial and anti-inflammatory properties that may influence their efficacy. Combination therapy (antifungal plus steroid) can be considered when inflammation is an issue. Combination agents should not be used when the diagnosis is in question because that may lead to their overuse or to adverse effects.
TABLE 1 Common Antifungal Medications and Their Forms
| Agent | Rx or OTC | Solution or spray* | Lotion† | Cream‡ | Gel or ointment§ | Powder* |
|---|---|---|---|---|---|---|
| Tolnaftate (Tinactin) | OTC | Yes | Yes | Yes | Yes | No |
| Haloprogin (Halotex) | Rx | Yes | No | Yes | No | No |
| Ciclopirox (Loprox; Penlac||) | Rx | Lacquer | Yes | Yes | No | No |
| Clotrimazole (Lotrimin) | OTC | Yes | Yes | Yes | No | No |
| Miconazole (Micatin) | OTC | Yes | Yes | Yes | No | Yes |
| Ketoconazole (Nizoral) | Rx | Shampoo | No | Yes | No | No |
| Sulconazole (Exelderm) | Rx | No | No | Yes | No | No |
| Oxiconazole (Oxistat) | Rx | No | Yes | Yes | No | No |
| Econazole (Spectazole) | Rx | No | No | Yes | No | No |
| Butenafine (Mentax) | Rx | No | No | Yes | No | No |
| Naftifine (Naftin) | Rx | No | No | Yes | Yes | No |
| Terbinafine (Lamisil) | Rx | Yes | No | Yes | No | No |
| Clotrimazole/BMD (Lotrisone) | Rx | No | No | Yes | No | No |
Rx = prescription; OTC = over-the-counter; BMD = betamethasone dipropionate.
*—Powders and sprays may be used to prevent reinfection.
†—Use lotions in intertriginous or hairy areas and on oozing lesions.
‡—Use creams on non-oozing and moderately scaling lesions.
§—Use ointments on hyperkeratotic lesions.
||—Ciclopirox lacquer (Penlac) is approved for treatment of onychomycosis but has limited efficacy.
Adapted with permission from Diehl KB. Topical antifungal agents: an update. Am Fam Physician 1996;54:1689.
The mechanism of action may have an effect on efficacy. The newer agents have fungicidal activity, which may translate into higher cure rates and lower relapse rates. Clinical judgment with regard to prior treatments and complicating conditions (bacterial growth or intense inflammation), along with knowledge of the agent's properties, will help guide the choice of therapy. When inflammation is a salient clinical feature, it must be considered in the selection of a treatment option.
Tolnaftate
This narrow-spectrum antifungal has no antibacterial or anticandidal activity.21 It is effective in most dermatophytoses and for treatment of tinea versicolor.22 It is available as an over-the-counter medication and requires twice-daily application.
Haloprogin
Introduced after tolnaftate, haloprogin combines equivalent efficacy with a broadened fungal spectrum (including yeasts).23 It is associated with higher rates of irritant dermatitis.24 It is applied twice daily.
Ciclopirox
This broad-spectrum agent is effective against dermatophytes, yeasts, and some bacteria.3 It has in vitro antibacterial activity against gram-negative and gram-positive bacteria. It has been shown to be more effective than the nonprescription agent clotrimazole (Lotrimin) in the treatment of tinea pedis.25 It requires twice-daily application.
Ciclopirox 8 percent lacquer (Penlac), which was approved for treatment of onychomycosis in late 1999, has limited efficacy. In two trials of daily application to infected toenails for 48 weeks, complete cure was achieved in 5.5 and 8.5 percent of patients. Only the latter was statistically significant compared with placebo. Partial clearance was also low (12 percent in the more successful trial). Penlac requires daily application for up to 48 weeks and monthly follow-up for nail debridement.26
Butenafine
This agent is similar in structure to that of the allylamines. Butenafine is fungicidal for dermatophytes in vitro.27 It is applied once daily and, after four weeks of use, is associated with high cure rates and a long disease-free interval.28
Azoles
This class includes many over-the-counter and prescription preparations. Members of this class include clotrimazole, econazole (Spectazole), ketoconazole (Nizoral), miconazole (Micatin), oxiconazole (Oxistat), and sulconazole (Exelderm). These agents have broad-spectrum activity, including activity against some gram-positive bacteria. Ketoconazole,29 sulconazole and oxiconazole30 require only once-daily application because of their long durability in the superficial layers of the skin. Clotrimazole, miconazole, and econazole require twice-daily application.
Allylamines
Naftifine (Naftin) and terbinafine (Lamisil) are applied once-daily and remain active in the skin for up to one week after application.31,32 Both agents have fungicidal activity in vitro, but the clinical significance of this point is uncertain.33,34 Terbinafine has been compared with ketoconazole and miconazole. Terbinafine was more efficacious after one week than ketoconazole was after two weeks.35 In addition, one week of terbinafine was found to be as effective as four weeks of miconazole.36 Evidence also suggests that terbinafine may be effective in curing tinea pedis in as few as three applications.37 Naftifine has intrinsic anti-inflammatory properties equivalent to members of the azole class plus 1 percent hydrocortisone.38 Evidence suggests that the fungicidal activity of naftifine and its duration of activity result in higher cure rates and a lower relapse rate.39
COMBINED STEROID/ANTIFUNGAL AGENTS
In the United States, the only combination steroid/antifungal agent indicated for the treatment of dermatophytosis is clotrimazole-betamethasone (Lotrisone). This formulation combines an effective antifungal agent with a potent steroid. Patients who have symptomatic inflammatory dermatophytosis with erythema, pruritus, and burning are optimally treated twice daily with this combination. The steroid component provides rapid symptomatic relief while the slower-acting antifungal agent eradicates the causative organism. Inflammation typically occurs in tineas caused by zoophilic dermatophytes.
The efficacy of this combination treatment has been demonstrated in two randomized controlled studies,40,41 the first treating tinea cruris and the second treating tinea cruris and corporis. In each study, the combination was better than either of the components alone in clearing the tinea infection. Because of these results, it is inferred that the steroid may enhance the antifungal activity of the clotrimazole.40
A steroid/antifungal preparation should be used only when a diagnosis of fungal infection has been confirmed, not when it is in question. An analysis of the use of this product found that nondermatologists are more likely to use combination therapy.42 In the absence of fungi or inflammation, the added expense of this preparation is not justified.
Because of the potent steroid component, this medication provides rapid relief, but it must be used judiciously.43 Potential complications associated with long-term steroid use are atrophy, steroid-induced acne, rosacea, and striae. Caution must be used when treating areas of thin skin and naturally occluded body areas, such as the groin, axillae, breast, and face. Treatment of these areas should be avoided whenever possible. When the groin is affected by dermatophytosis, the cream should be used sparingly and only for two weeks. The recommended duration of treatment for tinea pedis is four weeks. This combination should not be used in children younger than 12 years.

