Sick sinus syndrome comprises a variety of conditions involving sinus node dysfunction and commonly affects elderly persons. While the syndrome can have many causes, it usually is idiopathic. Patients may experience syncope, pre-syncope, palpitations, or dizziness; however, they often are asymptomatic or have subtle or nonspecific symptoms. Sick sinus syndrome has multiple manifestations on electrocardiogram, including sinus bradycardia, sinus arrest, sinoatrial block, and alternating patterns of bradycardia and tachycardia (bradycardia-tachycardia syndrome). Diagnosis of sick sinus syndrome can be difficult because of its nonspecific symptoms and elusive findings on electrocardiogram or Holter monitor. The mainstay of treatment is atrial or dual-chamber pacemaker placement, which generally provides effective relief of symptoms and lowers the incidence of atrial fibrillation, thromboembolic events, heart failure, and mortality, compared with ventricular pacemakers.
Sick sinus syndrome is a generalized abnormality of cardiac impulse formation that may be caused by an intrinsic disease of the sinus node that makes it unable to perform its pacemaking function, or by extrinsic causes.1 Abnormalities encompassed in this syndrome include sinus bradycardia, sinus arrest or exit block, combinations of sino-atrial and atrioventricular nodal conduction disturbances, and atrial tachyarrhythmias. Sick sinus syndrome is not a disease with a single etiology and pathogenesis but, rather, a collection of conditions in which the electrocardiogram (ECG) indicates sinus node dysfunction.2
Sick sinus syndrome is characterized by sinus node dysfunction with an atrial rate inappropriate for physiologic requirements. Although the condition is most common in the elderly, it can occur in persons of all ages, including neonates.3 The mean age of patients with this condition is 68 years, and both sexes are affected approximately equally.4 The syndrome occurs in one of every 600 cardiac patients older than 65 years and may account for 50 percent or more of permanent pacemaker placements in the United States.5
Etiology
Most cases of sick sinus syndrome are idiopathic, and the cause can be multifactorial (Table 1).3 Degenerative fibrosis of nodal tissue is the most common cause of intrinsic changes in the sinoatrial node that lead to sick sinus syndrome. Certain conditions can cause these intrinsic changes.3,5,6 There also are extrinsic causes of sinus node dysfunction and conditions that can cause this problem in children (Table 1).3
Coronary artery disease may coexist with sick sinus syndrome in a significant number of patients, although it is not considered a major cause of the syndrome. It is unclear whether inflammation, sinus node ischemia, or local autonomic neural effects lead to the development of sick sinus syndrome in patients with myocardial infarction. Sinus node dysfunction usually is temporary when it follows an acute myocardial infarction. Uncommonly, chronic ischemia may cause fibrosis and lead to symptoms of sick sinus syndrome for months to years after myocardial infarction.
Clinical Manifestations
Patients with sick sinus syndrome often are asymptomatic or have symptoms that are mild and nonspecific7 (Table 2).3 Symptoms are related to the decreased cardiac output that occurs with the bradyarrhythmias or tachyarrhythmias.3 Most of the symptoms are caused by decreased cerebral perfusion, and 50 percent of patients have syncope or pre-syncope.5
Symptoms, which may have been present for months or years, can include syncope, palpitations, and dizziness, as well as symptoms caused by the worsening of conditions such as congestive heart failure, angina pectoris, and cerebral vascular accident.8 Peripheral thromboembolism and stroke, which can occur in the presence of bradycardia-tachycardia syndrome (alternating bradyarrhythmias and tachyarrhythmias), may be related to dysrhythmia-induced emboli.3 A slow heart rate in the presence of fever, left ventricular failure, or pulmonary edema may be suggestive of sick sinus syndrome.2,9 Associated tachycardia may cause flushing of the face, pounding of the heart, and retrosternal pressure.10 Other symptoms include irritability, nocturnal wakefulness, memory loss, errors in judgment, lethargy, lightheadedness, and fatigue2,11 (Table 2).3 More subtle symptoms include mild digestive disturbances, periodic oliguria or edema, and mild intermittent dyspnea.2
ECG Manifestations
Sick sinus syndrome can produce a variety of ECG manifestations consisting of atrial bradyarrhythmias, atrial tachyarrhythmias, and alternating bradyarrhythmias and tachyarrhythmias7 (Table 3).3 Supraventricular bradyarrhythmias may include sinus bradycardia, sinus arrest with or without junctional escape, sinoatrial exit block, ectopic atrial bradycardia, and atrial fibrillation with slow ventricular response. The sinus bradycardia that occurs in patients with sick sinus syndrome is inappropriate and not caused by medications.2,5 The sino-atrial exit block that occurs in patients with sick sinus syndrome may demonstrate a Mobitz type I block (Wenckebach block) and a Mobitz type II block.2 The ECG may reveal a long pause following cardioversion of atrial tachyarrhythmias, and a greater-than three-second pause following carotid massage.5 Sixty percent of patients have tachyarrhythmias.8
Supraventricular tachyarrhythmias that occur in patients with sick sinus syndrome include paroxysmal supraventricular tachycardia, atrial flutter, atrial fibrillation, and atrial tachycardia.2,3 Atrial fibrillation is the most common tachydysrhythmia in these patients.12 Rarely, a ventricular escape tachy-arrhythmia may be seen on ECG.8 Sinus node re-entrant rhythm is another ECG manifestation.5 Bradycardia-tachycardia syndrome may be seen on ECG or cardiac rhythm strip (Figure 1); this syndrome is more common in older patients with advanced sick sinus syndrome.3
Diagnosis
The diagnosis of sick sinus syndrome may be difficult because of the slow and erratic course of the syndrome. The condition often goes undetected in the early stages because only sinus bradycardia may be present at its origin.9 Some symptoms of patients with sick sinus syndrome (e.g., fatigue, irritability, memory loss, lightheadedness, palpitations, cognitive defects) are present in several other disorders that occur in elderly patients and may be misdiagnosed as those of senile dementia.5 Symptoms of sick sinus syndrome may be variable, intermittent, and difficult to associate with ECG changes.2 If the patient is asymptomatic when ECG or ambulatory monitoring is performed, the dysrhythmias of the syndrome are often not present.5 Furthermore, there is no definitive way to distinguish patients with atrial fibrillation associated with sick sinus syndrome from patients with atrial fibrillation and normal sinus function; this distinction is clinically important because treating atrial fibrillation with cardioversion or medications can have catastrophic consequences if the sinus node is inadequate.
FIGURE 1.
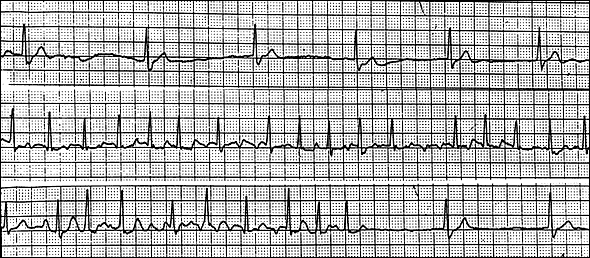
Electrocardiogram exhibiting alternating patterns of bradycardia and tachycardia as seen in patients with sick sinus syndrome.
One manifestation of serious sinus node dysfunction in patients with atrial fibrillation is a slow ventricular rate in the absence of medications such as propranolol (Inderal) or digitalis.2 Bradycardia may be misattributed to digoxin treatment in a patient with congestive heart failure. Cardioactive drugs, such as digoxin, quinidine (Quinaglute), and procainamide (Pronestyl), as well as hyperkalemia, can cause periodic sinus arrest or sinoatrial exit block.
TABLE 4 Indications for Permanent Pacemaker Implantation in Sick Sinus Syndrome
| Class I* | |
| 1. | SSS with documented symptomatic bradycardia, including frequent sinus pauses that produce symptoms. In some patients, bradycardia is iatrogenic and will occur as a consequence of essential long-term drug therapy of a type and dosage for which there are no acceptable alternatives. |
| 2. | Symptomatic chronotropic incompetence |
| Class IIa | |
| 1. | SSS occurring spontaneously or as a result of necessary drug therapy, with heart rate less than 40 bpm when a clear association between significant symptoms consistent with bradycardia and the actual presence of bradycardia has not been documented. |
| Class IIb | |
| 1. | In minimally symptomatic patients, chronic heart rate less than 30 bpm while awake |
| Class III | |
| 1. | SSS in asymptomatic patients, including those in whom substantial sinus bradycardia (heart rate less than 40 bpm) is a consequence of long-term drug treatment |
| 2. | SSS in patients with symptoms suggestive of bradycardia that are clearly documented as not associated with a slow heart rate |
| 3. | SSS with symptomatic bradycardia caused by nonessential drug therapy |
SSS = sick sinus syndrome; bpm = beats per minute.
*—Class I represents conditions for which there is evidence and/or general agreement that a given procedure or treatment is beneficial, useful, and effective. Class II represents conditions for which there is conflicting evidence and/or a divergence of opinion about the usefulness/efficacy of a procedure or treatment. Class IIa represents conditions in which the weight of evidence/opinion is in favor of usefulness/efficacy. Class IIb represents conditions in which the usefulness/efficacy is less well established by evidence/opinion. Class III represents conditions for which there is evidence and/or general agreement that a procedure/treatment is not useful/effective and in some cases may be harmful.
Information from Gregoratos G, Cheitlin MD, Conill A, Epstein AE, Fellows C, Ferguson TB Jr, et al. ACC/AHA guidelines for implantation of cardiac pacemakers and antiarrhythmia devices: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Pacemaker Implantation). J Am Coll Cardiol 1998;31:1178,1182.
Functional sinus bradycardia, enhanced vagal drive, gastrointestinal and neurologic conditions, and other causes of syncope can produce symptoms similar to those of sick sinus syndrome and must be included in the differential diagnosis of the syndrome. Sinus node dysfunction can occur perioperatively because of increased vagal tone caused by anesthesia or surgical intervention.13 All of these possibilities must be excluded before the diagnosis of sick sinus syndrome can be made.9
The diagnosis requires not only documentation of sinus node dysfunction but also correlation with the associated symptoms of sick sinus syndrome. The most common method of diagnosis is Holter monitoring. During monitoring, patients must keep a precise diary of their activities and symptoms, so that these factors can be correlated with the ECG changes.3
If two 24-hour periods of Holter monitoring fail to reveal the dysrhythmias of sick sinus syndrome, but the symptoms are severe and intermittent, it is likely that the sinus node dysfunction is severe but intermittent. In these cases, patients can carry a pocket-sized device for transmitting ECG readings via telephone when they are having symptoms. For this procedure to be successful, the arrhythmia must last for at least one minute. Another approach is to have patients activate a recording device to monitor the events of cardiac dysrhythmias when they are having symptoms.2
There are several other methods of diagnosing sick sinus syndrome. Isometric handgrip exercises or Valsalva's maneuvers normally increase the heart rate, but this effect may be minimal or absent in patients with this syndrome. If carotid massage produces abrupt sinus arrest of three seconds' duration, sinus node dysfunction may be suspected.8 These measures and monitoring cardiac response to such agents as atropine and isoproterenol (Isuprel) should only be attempted while a patient is undergoing careful ECG monitoring.3
Exercise testing may be useful in determining the response of the sinus node to physiologic demands. At an equal level of oxygen consumption, some patients with sick sinus syndrome have a decreased heart rate response to exercise compared with healthy patients.5 Intracardiac electrophysiologic tests (atrial overdrive pacing and premature atrial stimulation) can be used to elicit intrinsic sinus node disease or to document the effects of cardioactive drugs2,3; however, electrophysiologic testing is no longer routinely recommended for diagnostic purposes because of its poor sensitivity and specificity.14 The risks and benefits of these diagnostic modalities must be considered and discussed with the patient before they are used.
Treatment
Pacemaker therapy is warranted in many patients with sick sinus syndrome. Table 415 lists practice guidelines from the American College of Cardiology/American Heart Association task force on permanent pacemaker placement in patients with this condition.15 It is essential to document symptoms concurrent with the dysrhythmia when evaluating whether pacemaker placement will be beneficial.
The treatment of choice for symptomatic bradyarrhythmias in patients with sick sinus syndrome is the placement of a pacemaker.1,3 Artificial pacemakers are well tolerated in elderly patients.2 In all patients with this syndrome, except those with chronic atrial fibrillation, atrial-based pacemakers are recommended1,16 (Figure 2).16
FIGURE 2. Optimal Pacemaker Mode Recommendations in Sick Sinus Syndrome
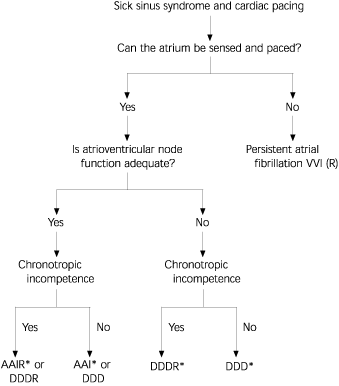
A simplified algorithm for optimal mode recommendations in patients with sick sinus syndrome (see Table 5 for codes).
Adapted with permission from Alagona P Jr. Advances in pacing for the patient with sick sinus syndrome. Curr Opin Cardiol 1997;12:7.
Table 514,17 lists the international codes describing pacemakers and implanted devices. Patients who have sick sinus syndrome with right bundle branch block have an increased risk of developing symptomatic high-degree atrioventricular block and should be treated with a dual-chamber pacemaker. Patients with no signs of atrioventricular conduction abnormalities should be treated with an atrial-based pacemaker.18 Pacing with a dual-chamber demand pacemaker with automatic mode-switching function is appropriate in patients with sick sinus syndrome who have intermittent tachyarrhythmic components. Pacing with a rate-responsive single-chamber ventricular demand pacemaker should be used in patients with the syndrome and chronic atrial fibrillation.7
Complications, including myocardial perforation, pneumothorax, wound hematoma, venous thrombosis, pacemaker lead failure, and infection, can occur with permanent endocardial pacemaker therapy, but they are uncommon.19
When tachyarrhythmias are a problem in a patient with sick sinus syndrome, a pacemaker may decrease the risk of complete heart block or asystole associated with pharmacotherapy.3 Digitalis can cause brady-arrhythmias in patients with sick sinus syndrome and should only be used in conjunction with a pacemaker in the management of supraventricular tachyarrhythmias.5 Severe sinus bradycardia, sinoatrial arrest, or sinoatrial exit block occasionally occurs with the use of beta-blocker medications in patients with this condition.2
Symptoms associated with this syndrome may be worsened in patients who are receiving digitalis, verapamil (Calan), beta blockers, sympatholytic agents such as clonidine (Catapres) and methyldopa (Aldomet), and antiarrhythmic agents.3,5 Therefore, the use of negative chronotropic drugs should be cautiously considered.7 The effects of pro-cainamide and quinidine are unpredictable. In certain patients with sick sinus syndrome and episodes of heart failure, oral theophylline therapy and dual-chamber pacemakers have been shown to reduce the occurrence of heart failure.20 In the absence of pacing, cardioversion may be dangerous because of the likelihood of prolonged sinus arrest.3
Patients with sick sinus syndrome who have bradycardia-tachycardia syndrome or chronic atrial fibrillation (especially in association with congestive heart failure, large left atria, or mitral valve disease) are at risk for embolic stroke. Although the risk-to-benefit ratio for anticoagulation is not well defined in these patients, warfarin (Coumadin) has been shown to decrease the number of strokes and embolic events in patients with sick sinus syndrome who have paroxysmal and chronic atrial fibrillation.5,11
Prognosis
Randomized controlled trials4,21 have examined morbidity and mortality in patients with sick sinus syndrome using various pacing modes. Compared with ventricular pacing, atrial pacing is associated with a lower incidence of thromboembolic complications, atrial fibrillation, heart failure, cardiovascular mortality, and total morbidity.1,18 In a retrospective study,22 patients with sick sinus syndrome who had pacemaker therapy were followed for 12 years; at eight years, mortality among those with ventricular pacing was 59 percent compared with 29 percent among those with atrial pacing. This discrepancy may well be a result of the physiologic or anatomic disorder (e.g., fibrosis of conductive tissue) leading to the requirement for the particular pacemaker rather than the type of pacemaker used.
Patients who have sick sinus syndrome with only sinus bradycardia have a better prognosis. One study3 indicated that mortality rates in these patients may not be different from mortality rates in the normal population. Researchers conducting one literature review22 concluded that patients with this syndrome who require atrial or dual-chamber pacing have a mortality rate of 3.6 percent (plus or minus 1.8 percent) per year. There is a high prevalence of cardiovascular disease in patients with sick sinus syndrome who die within the first few years of pacemaker implantation.2
Recent improvements in rate-responsive pacemaker engineering have led to improvements in maximum heart rate, exercise tolerance, functional status, suppression of dysrhythmias, and sense of well-being in patients.16 The achievement of near-physiologic rate responsiveness and atrioventricular synchrony, as well as decreased mortality and morbidity, has led to a better prognosis in patients with sick sinus syndrome.19

