
Am Fam Physician. 2006;73(3):401
The Medicare Part D prescription drug benefit aims to relieve the burden of out-of-pocket prescription drug costs for persons older than 65 years, but its effects will vary. Persons with low income and those without prior prescription coverage are projected to save the most, whereas those who lose employer-based coverage are predicted to pay more for their existing regimens.
Medicare Part D, although providing some welcome relief for older patients with high prescription costs, has a complex design reflecting significant political compromise.1 Enrollees continue to share prescription costs with Medicare through a series of mechanisms, including an enrollment premium of $32 per month; a deductible of $250 per year; a coinsurance between $250 and $2,250 per year, for which enrollees pay 25 percent of drug costs; a “doughnut hole” between $2,250 and $5,100 per year, for which enrollees are responsible for 100 percent; and a catastrophic cap of $5,100 per year, above which enrollees pay 5 percent (costs reflect 2006 estimates).2 Low-income enrollees with limited assets, if concomitantly registered for subsidies through the Social Security Administration, have nearly complete coverage with elimination of premiums, deductibles, coinsurance, and doughnut holes.
Of the 43 million eligible Medicare beneficiaries, an estimated 29 million will participate by the end of 2006.2 Although most will enroll voluntarily, more than 7 million patients with Medicare and Medicaid dual eligibility or other low-income assistance will be signed up automatically.2 On average, participants’ out-of-pocket costs will decrease by 37 percent under Part D—from $1,257 to $792—at a cost of $724 billion to the federal treasury over the next 10 years.3 However, for some beneficiaries, out-of-pocket spending will increase.
Who will benefit most? Medicare beneficiaries with no prior drug coverage (approximately one in four) will see their average annual costs cut in half, from more than $1,500 to $780.2 Low-income beneficiaries (those at less than 150 percent of the federal poverty level) will see their average annual expenses reduced by 83 percent, or $584. Low-income enrollees who previously were without Medicaid will spend an estimated $1,400 less per year. However, close to 40 percent of low-income beneficiaries are unlikely to sign up for subsidies.2
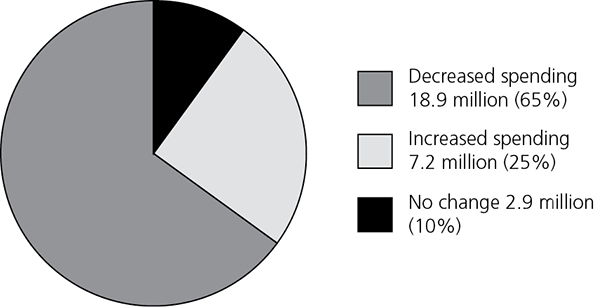
Who will face increased spending? An estimated 7 million beneficiaries will see an average annual increase in spending of $492 (see accompanying figure)2; a large portion of these will be retirees who lose employer coverage.2 Despite tax-free subsidies from Medicare, 17 to 35 percent of employers are expected to drop their prescription coverage, which typically is more comprehensive than that offered through Part D.3
Physicians should encourage Part D enrollment among patients who will benefit most, while recognizing that up to 35 percent of enrollees may have no relief or an increase in their out-of-pocket expenses for prescription medications.