Of 29 million expected Part D beneficiaries, 6.9 million are projected to have annual out-of-pocket medication expenses greater than $750. Accounting for one fourth of all Part D enrollees, these beneficiaries also are most likely to have high aggregate health care costs, putting them at continued financial risk unless additional policy options are considered.
Despite relief in spending for some patients with Medicare Part D prescription coverage, 3.8 million Part D beneficiaries are expected to have annual out-of-pocket costs between $750 and $3,600, and another 3.1 million beneficiaries may have costs exceeding $3,600.1 Of these 6.9 million, 28 percent have incomes less than 150 percent of the federal poverty level.1 Although these patients probably will qualify for low-income subsidies, poor enrollment for existing low-income assistance such as the Medicare Savings Program does not bode well for enrollment in similar programs available under Part D.2 It is estimated that as many as 40 percent of beneficiaries eligible for subsidies may not enroll1 for reasons such as inadequate outreach to the eligible population and patient confusion over the procedures. Without enrolling for these subsidies, patients with low incomes and high prescription costs could spend 25 percent of their income on prescription drugs(see accompanying figure).3
The remaining 72 percent of beneficiaries with high drug costs also may have substantial out-of-pocket spending. The median annual income for a household headed by an individual older than 65 years is approximately $23,0003;drug costs of $3,600 would account for 16 percent of the household income (see accompanying figure),3 and drug costs made up only one fourth of total out-of-pocket health care spending for Medicare patients in 2003.4 Additionally, nonmedication costs will grow. Part B premiums are projected to increase at rates greater than inflation through 2014.2
Figure. Out-of-Pocket Costs as Portion of Income
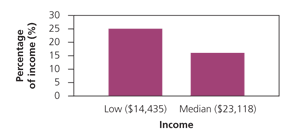
$3,600 out-of-pocket drug spending as a percentage of low and median annual incomes for Medicare patients.
Information from reference 3.
In creating this drug benefit, Congress bypassed opportunities for further prescription cost-saving such as competitive pricing that could have reduced expenditures by one half or more.5,6 Policy makers must address how to control the rise in medication costs faced by Medicare beneficiaries, many of whom operate on fixed incomes. Meanwhile, physicians should be aware that some of their older patients will face heavy out-of-pocket prescription costs despite Part D, and should facilitate the enrollment of eligible patients into low-income subsidy programs.

