Chronic plaque psoriasis, the most common form of psoriasis, is a papulosquamous disease defined by erythematous plaques with a silvery scale. The diagnosis usually is clinical, but occasionally a biopsy is necessary. Psoriasis affects 0.6 to 4.8 percent of the U.S. population, and about 30 percent of affected patients have a first-degree relative with the disease. Psoriasis is a T-cell–mediated autoimmune disease, but certain medications and infections are well-known risk factors. Management of psoriasis includes education about chronicity, realistic expectations, and use of medication. Steroids and vitamin D derivatives (e.g., calcipotriene) are the mainstays of topical therapy. Topical steroids and calcipotriene together may work better than either agent alone. Patients with psoriasis involving more than 20 percent of their skin or those not responding to topical therapy are candidates for light therapy; traditional systemic therapy; or systemic treatment with immunomodulatory drugs such as alefacept, efalizumab, and etanercept.
The prevalence of psoriasis in the United States is estimated to be 0.6 to 4.8 percent.1 Psoriasis is slightly more common in men.1 No reliable data exist to support the common assumption that psoriasis is less common in blacks.1 There is a bimodal onset (i.e., late teens and late 50s), and early-onset disease is more common.2
About 30 percent of patients with psoriasis have a first-degree relative with the disease, and those with early-onset disease are more likely to have a family history of psoriasis.1,2 These facts lend support for a genetic basis for the disease, and several chromosome loci have been implicated.3 The disease is not exclusively genetic, however, because several environmental factors also appear to play a role.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The diagnosis of psoriasis usually is based on the clinical appearance of the skin lesions. | C | 35 |
| Topical steroids and calcipotriene (Dovonex) are the mainstays of topical therapy and, when used together, they may work better than either agent alone. | A | 17,18,29,30 |
| Patients who have psoriasis involving more than 20 percent of their skin are candidates for light therapy or systemic therapy, and usually these patients are managed in conjunction with a dermatologist. | C | 30,35 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 573 orhttps://www.aafp.org/afpsort.xml.
Pathogenesis
Psoriasis is a T-cell–mediated autoimmune disorder.4 The process begins with an environmental factor, perhaps a viral antigen, which induces T cells to produce cytokines. The cytokines stimulate keratinocyte proliferation and production of antigenic adhesion molecules in the dermal blood vessels. These adhesion molecules further stimulate T cells to produce cytokines, thus perpetuating the response.5 Immunomodulatory drugs, which target the mechanism just described, offer novel treatment options for psoriasis.5 These drugs, also known as biologics, are discussed later.
Risk Factors
Psoriasis is associated with several risk factors that may provide the environmental stimulus to T-cell proliferation. They include psychological stress, certain medications (lithium, beta blockers, antimalarial drugs, nonsteroidal anti-inflammatory drugs, and oral steroid withdrawal),6 and infection. Although a link between psoriasis and stress seems to exist, evidence to support a causal relationship is lacking.7 Chronic human immunodeficiency virus infection is associated with severe psoriasis exacerbations.8
Diagnosis
The diagnosis of psoriasis is based on the clinical appearance of skin lesions. Biopsy may be necessary, however, to distinguish psoriasis from other conditions with similar appearances such as lichen simplex chronicus, nummular eczema, seborrheic dermatitis, and tinea corporis.
PLAQUES
Chronic plaque psoriasis typically is symmetric and bilateral (Figure 1). Lesions begin as papules and eventually coalesce to form plaques. Plaques are well demarcated and covered by a silvery scale (Figure 2). Plaques exhibit the Auspitz sign (bleeding after the removal of scale) and the Koebner phenomenon (lesions induced by trauma). Most patients (84 percent) with psoriasis report itching; the word psoriasis is derived from the Greek word for itching, “psora.”9
Figure 1.
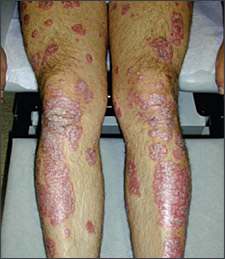
Symmetric and bilateral psoriasis plaques.
Figure 2.
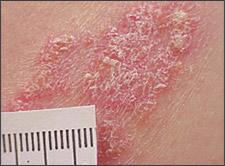
Classic silvery scale of a psoriasis plaque.
DISTRIBUTION
The extensor surfaces (elbows and knees) commonly are involved (Figure 3), as well as the lower back, scalp (Figure 4), and nails. Nail changes include onycholysis (separation of the nail from its bed; Figure 5), pitting (Figure 6), oil spots (yellow or brown spots caused by cellular debris under the nail), and nail dystrophy. Most patients eventually develop nail involvement, although nail findings precede skin findings in about 4 percent of patients.10,11 Older patients and those with longer duration of disease, extensive skin lesions, or joint involvement have more nail involvement.10,12
Figure 3.
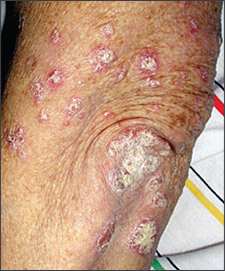
Psoriasis plaques on elbow.
Figure 4.
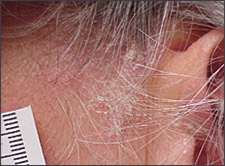
Scalp psoriasis, near the ear.
Figure 5.
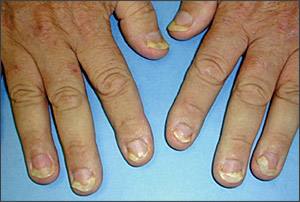
Onycholysis in a patient with psoriasis.
Figure 6.
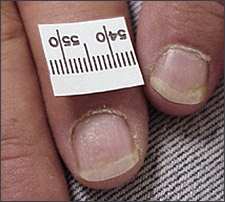
Nail pitting in a patient with psoriasis.
Inverse psoriasis, or f lexural psoriasis (Figure 7), affects intertriginous areas such as the gluteal fold, axillae, and glans of the uncircumcised penis. Scale may not appear in these areas.
Figure 7.
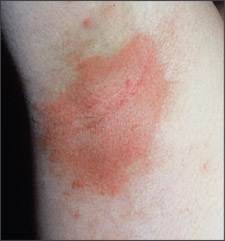
Psoriasis plaque in an intertriginous area (axilla); scale is not appreciated.
COMPLICATIONS
Chronic plaque psoriasis does not affect longevity. The condition may, however, be complicated by several comorbidities including malignancy, arthritis, and emotional distress from the cosmetic effects of the disease. Depression, anxiety, sexual dysfunction, poor self-esteem, and suicidal thoughts may coexist with psoriasis, even in patients with less severe disease.13
Cohort studies14 have shown that an increased risk of nonmelanoma skin cancers and lymphoma is associated with psoriasis.14 This risk is higher in patients with more severe disease, but it is not clear whether disease severity or treatment accounts for the increased risk.14
Psoriatic arthritis is an inf lammatory, seronegative arthritis with a variable course. The arthritis typically is asymmetric and involves the fingers and toes (Figure 8). Estimates of the prevalence of psoriatic arthritis vary widely, but the authors of one study12 at a referral center found that one third of patients with psoriasis had arthritis and that, in two thirds of those with arthritis, skin lesions preceded arthritis.
Figure 8.
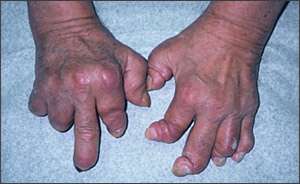
Severe psoriatic arthritis affecting the fingers.
Treatment
GENERAL APPROACH
Patients and physicians should understand that psoriasis is a chronic disease without a cure, and that it is important to have realistic expectations of treatment. Treatment should focus on improvement, not disappearance, of lesions. Complete clearing of lesions usually is not possible in patients who use only topical therapy, and overuse of topical therapies results in more side effects.15
NONDRUG THERAPIES
A variety of nondrug therapies for chronic plaque psoriasis have been suggested, including acupuncture, psychotherapy, lifestyle modifications (e.g., smoking cessation), and dietary supplementation (e.g., vitamin D, fish oil). However, there is insufficient evidence regarding the effectiveness of these treatments.16
TOPICAL THERAPIES
Topical therapies used to manage psoriasis include steroids, vitamin D derivatives, retinoids, immunosuppressants, anthralin (Anthra-Derm), coal tar ointment (Zetar), and several other agents (Table 1).17–27
TABLE 1 Topical Therapies for Chronic Plaque Psoriasis
| Drug class/drug(s) | Mechanism of action | Dosage | Common side effects | Cost (generic)* | Comment | |
|---|---|---|---|---|---|---|
| Topical steroids | ||||||
| Various potent or very potent topical steroids (e.g., mometasone [Elocon], clobetasol [Temovate]) | Controls inflammation | Mometasone: 0.1% cream, ointment, lotion; applied once a day | Hypopigmentation, striae, skin atrophy, tachyphylaxis | Mometasone: Cream, ointment: 45 g, $54 ($45 to $49) Lotion: 60 mL, $61 | Side effects increase with longer duration of use and occlusive dressings. | |
| Clobetasol: 0.05% cream, ointment, gel, solution; applied twice a day | Clobetasol: Cream, ointment: 45 g, $80 ($47 to $50) Gel: 60 g, $100 ($72 to $74) Solution: 25 mL, $36 ($27 to $28) | |||||
| Vitamin D derivatives | ||||||
| Calcipotriene (Dovonex) | Normalizes keratinocyte proliferation and differentiation | 0.005% cream, ointment, solution; applied twice a day | Skin irritation, pruritus, burning, hypercalcemia | Cream: 60-g tube, $132; 120-g tube, $241 Solution: 60-mL bottle, $116 Ointment: 60-g tube, $132; 120-g tube, $241 | Limit dosage to 100 g per week to avoid hypercalcemia. | |
| Topical retinoids | ||||||
| Tazarotene (Tazorac) | Normalizes keratinocyte proliferation and differentiation | 0.05%, 0.1% cream, gel; applied at bedtime | Skin irritation, pruritus, burning/stinging, erythema, desquamation, teratogenicity | Cream, 0.05%: 30 g, $100; 60 g, $200; 0.1%: 30 g, $106; 60 g, $213 Gel, 0.05%: 100 g, $334; 0.1%: 100 g, $354 | Obtain negative pregnancy test within two weeks of starting treatment. | |
| Topical immunosuppressants | ||||||
| Tacrolimus (Prograf)† | Inhibits T-lymphocyte cell activation | 0.1%, 0.3% ointment; applied once or twice a day | Burning/stinging, pruritus, influenza-like symptoms, erythema, acne, folliculitis, HSV infection | 0.1%: 30 g, $68 0.1%: 60 g, $136 0.1%: 100 g, $209 | Studies cited used 0.3% ointment every day and 0.1% ointment twice a day. | |
| Pimecrolimus (Elidel)† | Inhibits T-lymphocyte cell activation | 1% cream; applied twice a day | Burning, pruritus, influenza-like symptoms, erythema, HSV infection, viral infection, fever | 30 g, $57 60 g, $113 100 g, $178 | Study cited used 1% cream twice a day. | |
| Anthralin (Anthra-Derm) | Antiproliferative effect on epidermal keratinocytes | 0.1%, 0.25%, 0.5%, 1% cream, ointment; applied once or twice a day | Skin irritation, erythema, staining (skin and clothing), odor | Anthra-Derm cream, 1%: 50 g, $88 ($59) | ||
| Coal tar | ||||||
| Multiple preparations exist Zetar topical ointment | Keratolytic and probably anti-inflammatory and antiproliferative effects | Coal tar solution 10% = 2% coal tar; applied at bedtime | Skin irritation, folliculitis, odor, staining of clothing | 3.8 oz, $9 to $13 | ||
HSV = herpes simplex virus.
note: Drugs are listed from most to least clinically important.
*—Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, N.J.: Medical Economics Data, 2005. Cost to the patient will be higher, depending on prescription filling fee.
†—Not approved by the U.S. Food and Drug Administration for the management of psoriasis.
Topical Steroids
Topical steroids have been the mainstays of treatment for many years. Multiple randomized controlled trials17 (RCTs) have found that potent (e.g., fluocinonide [Lidex], mometasone [Elocon] ointment) and very potent (e.g., clobetasol [Temovate], halobetasol propionate [Ultravate]) topical steroids improve psoriasis plaques. The major limitation of these studies is their short duration, averaging only four weeks. Few studies have examined topical steroids for maintenance therapy, but one RCT28 found better control at six months when patients applied steroids once weekly.
The side effects of topical steroids include skin atrophy, striae, and tachyphylaxis. Only weak (i.e., nonfluorinated) topical steroids should be used on the face and in skinfolds. Side effects increase with longer duration of use, higher potency, and occlusive dressings.
Vitamin D Derivatives
Vitamin D derivatives, available as calcipotriol in the United Kingdom or calcipotriene (Dovonex) in the United States, work by inhibiting keratinocyte proliferation and improving keratinocyte differentiation. Two systematic reviews17,18 of RCTs found that calcipotriene is more effective than placebo and is as effective as potent topical steroids. When calcipotriene is used in combination with topical steroids, psoriasis improves more than with either agent alone.17,18,29,30 The main side effect of calcipotriene is perilesional skin irritation, although it is rarely severe enough to require cessation of treatment.18 Topical steroids used in conjunction with calcipotriene may lessen skin irritation.18
Topical Retinoids.
A topical retinoid, tazarotene (Tazorac), also improves chronic plaque psoriasis.19 The authors of one RCT20 found tazarotene to be as effective as topical steroids, with a treatment success rate at 12 weeks for knee and elbow lesions of 65 percent with tazarotene 0.1% versus 66 percent with fluocinonide. In a second RCT,21 tazarotene 0.1% plus a steroid was more effective and better tolerated than tazarotene alone. The overall response to treatment at 12 weeks was 80 percent in the tazarotene/placebo group and 95 percent in the tazarotene/steroid group (P < .05; number needed to treat [NNT] = 7).21
No studies have directly compared tazarotene with calcipotriene, but the authors of a recent systematic review22 found a higher percentage of treatment-related adverse effects in patients using tazarotene. Tazarotene causes perilesional irritation and is teratogenic.
Topical Immunosuppressants
The topical immunosuppressants tacrolimus (Prograf) and pimecrolimus (Elidel) are not approved by the U.S. Food and Drug Administration (FDA) for the treatment of psoriasis but are used by some physicians for this purpose. One small RCT23 did not find a difference between tacrolimus and placebo. Recently, two industry-sponsored RCTs found that tacrolimus improved intertriginous and facial psoriasis compared with placebo (NNT = 3),24 and that pimecrolimus improved intertriginous psoriasis compared with placebo (NNT = 3).25
Side effects of tacrolimus and pimecrolimus are mainly burning and itching, and both medications are expensive. Skin cancer and lymphoma have been reported after using these drugs, but causative associations are uncertain.26
Anthralin/Coal Tar
Anthralin and coal tar were once popular treatments for psoriasis when used in combination with ultraviolet B (UVB) light therapy. Both have fallen out of favor because of their poorly tolerated side effects, and neither is more effective than calcipotriene.18
Miscellaneous
Evidence is insufficient to support the use of aloe vera or capsaicin as treatment for psoriasis.16 Emollients and keratolytics often are used in conjunction with other topical therapies, but there is scant evidence to support their use alone.16 Good skin hygiene is important for treating most dermatologic conditions, so keeping skin hydrated with emollients and using keratolytics on flaky skin is recommended.
LIGHT THERAPY
Light therapy includes UVB phototherapy and ultraviolet A (UVA) photochemotherapy, usually administered in specialty centers. UVA photochemotherapy is the combination of ingested psoralen (a photosensitizer) followed by exposure to UVA (psoralen plus UVA [PUVA] therapy). RCTs have shown that both are beneficial, but there is an increased rate of nonmelanoma skin cancer following PUVA therapy.16 It is not clear whether tanning should be recommended as a treatment for psoriasis. Sunbathing helps clear psoriasis plaques in most patients, but it also increases the risk of skin cancers.
SYSTEMIC TREATMENTS
Systemic therapy for psoriasis includes methotrexate; cyclosporine (Sandimmune); oral retinoids; and, recently, the biologics. According to a recent review,27 there is strong RCT evidence that cyclosporine is effective and that oral retinoids are moderately effective. There was, however, a lack of RCTs to support the use of methotrexate.27 Methotrexate, cyclosporine, and oral retinoids all have serious side effects including myelosuppression, hepatotoxicity, renal impairment, and teratogenicity.
The biologics alefacept (Amevive), efalizumab (Raptiva), and etanercept (Enbrel) all have FDA approval for the management of psoriasis, and infliximab (Remicade) may gain approval soon. RCTs, including phases II and III studies, support the effectiveness of these drugs compared with placebo,31–34 but they have not yet been compared to each other or other therapies. Table 231–34 summarizes the side effects, cost, and monitoring required for the biologics.
TABLE 2 Biologic Therapies for Chronic Plaque Psoriasis
| Drug | Mechanism of action | Dosage | Common side effects | Monitoring | Cost* |
|---|---|---|---|---|---|
| Alefacept (Amevive) | Interferes with the function of antigen-presenting cells | 7.5 mg IV per week for 12 weeks or 15 mg IM per week for 12 weeks; repeat cycle may be given 12 weeks after first cycle complete | Lymphopenia, injection-site reactions, influenza-like symptoms, pruritus | Check CD4+ cell count at baseline and weekly thereafter. | $8,400 to $11,940 for a 12-week cycle |
| Efalizumab (Raptiva) | Inhibits T-cell/endothelial cell adhesion | Initial dose: 0.7 mg per kg SC | Influenza-like symptoms, URI, acne, psoriasis exacerbation; rare but serious side effect is thrombocytopenia | Monitor platelet counts every month initially, then every three months. | $18,720 for one year of continuous treatment |
| 1 mg per kg SC per week continuously thereafter | |||||
| Maximum: 200 mg per dose | |||||
| Etanercept (Enbrel) | Blocks the proinflammatory cytokine TNF-α | 50 mg SC twice per week for three months, then decrease to maintenance dosage of 50 mg SC per week | Injection-site reactions, URI symptoms, abdominal pain; potential risk of reactivating TB | Check PPD before treatment. | $20,700 (60 doses) for one year of continuous treatment |
| Infliximab (Remicade) | Blocks the proinflammatory cytokine TNF-α | 3 to 10 mg per kg IV infusions (over two hours) at weeks zero, 2, 6, and 14 | Infusion reactions, URI, pruritus, headache, sore throat; potential risk of reactivating TB | Check PPD before treatment. | $22,112 per year, based on eight treatments |
IV = intravenous; IM = intramuscular; SC = subcutaneous; URI = upper respiratory infection; TNF = tumor necrosis factor; TB = tuberculosis; PPD = purified protein derivative.
*—Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, N.J.: Medical Economics Data, 2005. Cost to the patient will be higher, depending on prescription filling fee.
Approach to the Patient
Evidence-based guidelines35 on the treatment of patients with chronic plaque psoriasis were published in 2004 by the Finnish Dermatological Society. Recommendations for the management of psoriasis in primary care, based on these guidelines, the evidence cited above, and considering common practice among American dermatologists, are shown in Figure 9.35
Figure 9 Management of Chronic Plaque Psoriasis
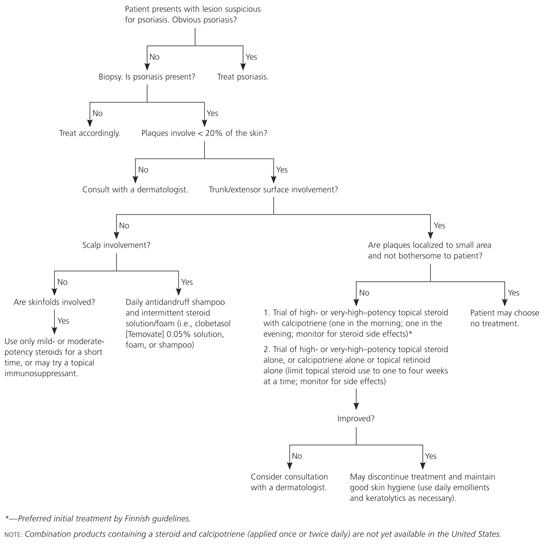
Algorithm for the management of chronic plaque psoriasis, based on recent guidelines,35 current evidence, and common practice among American dermatologists.
For the initial treatment of psoriasis on limited areas of skin, the most effective treatment is a combination of potent topical steroids and calcipotriene. This recommendation, however, is based on limited evidence.18,29,30 An alternative would be to start with a potent topical steroid, calcipotriene, or a topical retinoid alone. Calcipotriene and topical retinoids can be used long-term, but topical steroids must be used intermittently (i.e., for one to four weeks at a time) because of their side effects.35
If plaques are small and not bothersome, some patients may choose observation. For patients in whom psoriasis is limited to the scalp, the first-line therapy is usually daily antidandruff shampoo. Steroid solutions, foams, or shampoos may be used intermittently for exacerbations. Mild- to moderate-potency topical steroids or topical immunosuppressants should be used for intertriginous plaques.
Patients who do not respond to the above treatments, or who have lesions that occupy more than 20 percent of their body surface area, are candidates for light therapy, traditional systemic therapy, or the immunomodulating agents. Management of psoriasis usually is undertaken by or in conjunction with a dermatologist.35

