The incidence of hip fracture is expected to increase as the population ages. One in five persons dies in the first year after sustaining a hip fracture, and those who survive past one year may have significant functional limitation. Although surgery is the main treatment for hip fracture, family physicians play a key role as patients’ medical consultants. Surgical repair is recommended for stable patients within 24 to 48 hours of hospitalization. Antibiotic prophylaxis is indicated to prevent infection after surgery. Thromboprophylaxis has become the standard of care for management of hip fracture. Effective agents include unfractionated heparin, low-molecular-weight heparin, fondaparinux, and warfarin. Optimal pain control, usually with narcotic analgesics, is essential to ensure patient comfort and to facilitate rehabilitation. Rehabilitation after hip fracture surgery ideally should start on the first postoperative day with progression to ambulation as tolerated. Indwelling urinary catheters should be removed within 24 hours of surgery. Prevention, early recognition, and treatment of contributing factors for delirium also are crucial. Interventions to help prevent future falls, exercise and balance training in ambulatory patients, and the treatment of osteoporosis are important strategies for the secondary prevention of hip fracture.
Of those who survive one year after hip fracture, only 40 percent can perform all routine activities of daily living and only 54 percent can walk without an aid.1,2 Although surgical repair usually is needed after hip fracture, family physicians play an important role in supporting patients through the treatment process, facilitating rehabilitation and recovery, and initiating secondary prevention strategies.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Surgical management of hip fracture should begin 24 to 48 hours after hospitalization for stable patients without active comorbidities. | B | 3–5 |
| Patients undergoing hip fracture surgery should receive thromboprophylaxis; unfractionated heparin, low-molecular-weight heparin, fondaparinux (Arixtra), and warfarin (Coumadin) are effective agents. | A | 6,7,10 |
| Patients undergoing hip fracture surgery should receive perioperative antibiotic prophylaxis to prevent infection. | A | 13 |
| Indwelling urinary catheters should be removed within 24 hours of hip fracture surgery. | B | 3 |
| Patients with hip fracture should receive adequate analgesia for pain control. | B | 21,22 |
| Patients with hip fracture should begin rehabilitation on the first postoperative day and advance to ambulation as tolerated. | A | 3,20 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 2105 orhttps://www.aafp.org/afpsort.xml.
Diagnosis
A hip fracture diagnosis usually is established based on patient history, physical examination, and plain radiography. A patient with hip fracture typically presents with pain and is unable to walk after a fall. On physical examination, the injured leg is shortened, externally rotated, and abducted in the supine position. Plain radiographs of the hip (a posteroanterior view of the pelvis and a lateral view of the femur) usually confirm the diagnosis. However, when clinical suspicion for hip fracture is high and plain radiographs are normal, occult fracture should be ruled out with magnetic resonance imaging (MRI). If MRI is contraindicated, a bone scan may be useful in diagnosing fracture, but results may be normal for up to 72 hours after the injury.
Surgery
Studies have indicated that early surgery (i.e., 24 to 48 hours after hospitalization) for hip fracture is associated with lower one-year mortality,2,3 a lower incidence of pressure sores, decreased confusion,4 and a lower risk of fatal pulmonary embolism (PE).5 However, many of these studies did not control for the presence and severity of comorbidities. Although further studies are needed to identify persons who are at a high risk for surgery because of medical conditions, the risks of early surgery may outweigh the risks of delaying surgery in patients with unstable comorbidities (e.g., congestive heart failure, unstable angina, sepsis, severe hypoxia, anemia). Delaying surgery while stabilizing these patients is reasonable; however, waiting more than 72 hours should be avoided to prevent complications from prolonged immobilization.
Thromboprophylaxis
Thromboembolic complications cause significant morbidity and mortality in patients undergoing hip fracture surgery. Without prophylaxis, the rate of total deep venous thrombosis (DVT) in these patients is approximately 50 percent, and the rate of fatal PE is 1.4 to 7.5 percent.6 The effectiveness of several drug treatments (e.g., heparinoids, fondaparinux [Arixtra], warfarin [Coumadin], antiplatelet agents) for the prophylaxis of thromboembolism after hip fracture have been studied.See Online Table A for a summary of the evidence for thromboprophylaxis.
Online Table A Summary of the Evidence for Thromboprophylaxis After Hip Fracture
| Prophylactic agent | Study | Outcomes | NNT | Recommendation/comments | SORT evidence rating* |
|---|---|---|---|---|---|
| Aspirin | Evidence-based guidelinesA1,A2 | Rates of DVT and fatal PE were significantly reduced with aspirin (ARR, 0.4 percent each). | 250 | Aspirin confers much less protection compared with other prophylactic agents; aspirin should not be used alone.A1 | C |
| Fondaparinux (Arixtra) (2.5 mg SC once per day) | Double-blind randomized studyA3 | By the 11th postoperative day, the incidence of VTE was significantly reduced with fondaparinux compared with enoxaparin (Lovenox) (RRR, 56.4; 95% CI, 0.39 to 70.3) | 9 | Fondaparinux is an FDA-approved agent available for prevention of VTE in patients with hip fracture. | B |
| LMWH or unfractionated heparin | Cochrane meta-analysisA4 | Significant reduction in lower extremity DVT with LMWH (RR, 0.55; 95% CI, 0.34 to 0.88) or unfractionated heparin (RR, 0.59; 95% CI, 0.49 to 0.72) compared with control or no prophylaxis. | 7 | Slight increase in postoperative bleeding with both LMWH and unfractionated heparin | A |
| Warfarin (Coumadin) (INR, -2.0 to 2.7) | Pooled data from a review of RCTsA1 | Significant reduction in the rates of DVT with warfarin (RRR, 61 percent) when compared with placebo | - | Problems with over- or under-anticoagulation; need for frequent INR monitoring | A |
NNT = number needed to treat; SORT = strength of recommendation taxonomy; DVT = deep venous thrombosis; PE = pulmonary embolism; ARR = absolute risk reduction; SC = subcutaneous; VTE = venous thromboembolism; RRR = relative risk reduction; CI = confidence interval; FDA = U.S. Food and Drug Administration; LMWH = low-molecular-weight heparin; RR = relative risk; INR = International Normalized Ratio; RCT = randomized controlled trial.
*-A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see https://www.aafp.org/afpsort.xml.
Information from references:
A1. Geerts WH, Pineo GF, Heit JA, Bergqvist D, Lassen MR, Colwell CW, et al. Prevention of venous thromboembolism: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004;126:S338-400.
A2. Prevention of pulmonary embolism and deep vein thrombosis with low dose aspirin. Pulmonary Embolism Prevention (PEP) Trial. Lancet 2000;355:1295-302.
A3. Eriksson BI, Bauer KA, Lassen MR, Turpie AG, for the Steering Committee of the Pentasaccharide in Hip-Fracture Surgery Study. Fondaparinux compared with enoxaparin for the prevention of venous thromboembolism after hip-fracture surgery. N Engl J Med 2001;345:1298-304.
A4. Handoll HH, Farrar MJ, McBirnie J, Tytherleigh-Strong G, Milne AA, Gillespie WJ. Heparin, low molecular weight heparin and physical methods for preventing deep vein thrombosis and pulmonary embolism following surgery for hip fractures. Cochrane Database Syst Rev 2002;(4):CD000305.
PHARMACOLOGIC AGENTS
A Cochrane review7 examined the effectiveness of unfractionated heparin and low-molecular-weight heparin (LMWH) for the prevention of DVT and PE after hip fracture surgery in older patients. Patients taking unfractionated heparin or LMWH had significantly lower incidence of lower extremity DVT compared with placebo or no treatment.7 There was insufficient evidence to recommend one form of heparin over the other. Anticoagulation with both forms of heparin is associated with a slight increased risk of postoperative bleeding; however, LMWH is associated with a lower incidence of thrombocytopenia compared with unfractionated heparin.8
Studies3,6 support the use of warfarin to prevent thromboembolic complications in patients undergoing hip fracture surgery. Typically, patients receive 5 mg of warfarin per day for three days beginning on the first postoperative day. The patient’s International Normalized Ratio (INR) is used to guide further dosing. The patient’s INR should be between 2 and 3 with a target of 2.5. The need for frequent INR monitoring and the potential for overtreatment or undertreatment are disadvantages of warfarin therapy.3 Aspirin has been shown to reduce the risk of DVT and PE compared with placebo; however, aspirin was much less effective when compared with other prophylactic regimens.3,6,9
Fondaparinux is a synthetic pentasaccharide that significantly increases an antithrombin’s ability to inactivate factor Xa. A randomized double-blind study10 evaluated the effectiveness of fondaparinux for the prophylaxis of venous thromboembolism (VTE) in 1,711 patients undergoing hip fracture surgery. Patients received 40 mg of enoxaparin (Lovenox) or 2.5 mg of fondaparinux subcutaneously once per day. The incidence of VTE was significantly reduced by the 11th postoperative day in the fondaparinux group compared with the enoxaparin group (8.3 and 19.1 percent of patients, respectively;P < .001). The incidence of proximal DVT also was reduced significantly in the fondaparinux group compared with the enoxaparin group (0.9 and 4.3 percent of patients, respectively). The incidence of major bleeding was not significantly different between the two groups. The U.S. Food and Drug Administration (FDA) has approved fondaparinux for the prevention of VTE in patients with hip fracture; however, more studies are needed to evaluate the cost-effectiveness of the therapy.
MECHANICAL DEVICES
Foot and calf pumping devices7 and compression stockings11 have been shown to decrease the incidence of thromboembolic complications in persons with hip fracture compared with no treatment. However, compliance is reportedly a problem.7
TIMING AND DURATION
The appropriate timing and duration of thromboprophylaxis is controversial. It is reasonable to begin preoperative anticoagulation with unfractionated heparin or LMWH as soon as possible after the fracture occurs because of the increased risk of thromboembolism in patients with fracture. Prophylaxis should continue for 10 to 14 days after surgery.6 Anticoagulation may be delayed for 12 to 24 hours after surgery, until hemostasis is established, in patients at high risk of bleeding.6 A double-blind clinical trial12 showed that extended fondaparinux prophylaxis (four weeks) significantly reduced the incidence of documented VTE after hip fracture surgery compared with a one-week regimen (1.4 and 35 percent, respectively).
Guidelines from the American College of Chest Physicians6 recommend thromboprophylaxis for at least 10 days after surgery for patients with hip fracture. The guidelines recommend extended prophylaxis with fondaparinux, LMWH, or warfarin for 28 to 35 days after surgery, particularly for patients at high risk of thromboembolism (e.g., history of VTE, current obesity, delayed mobilization, advanced age, malignancy).
Antibiotic Prophylaxis
Antibiotic prophylaxis is recommended to prevent infection after hip fracture surgery. A Cochrane review13 showed that perioperative antibiotic use significantly reduced the incidence of deep and superficial wound infections and urinary tract infections compared with control groups. Ideally, antibiotic prophylaxis is initiated within the two hours before surgery14 and is continued for 24 hours after surgery.15 First- or second-generation cephalosporins are the agents of choice to prevent Staphylococcus aureus infection, which is common postoperatively. Vancomycin can be used in patients who are allergic to cephalosporins.16 See online Table B for a summary of the evidence for antibiotic prophylaxis.
Online Table B Summary of the Evidence for Antibiotic Prophylaxis After Hip Fracture
| Prophylactic agent | Study | Outcomes | Recommendation/comments | SORT evidence rating* | |
|---|---|---|---|---|---|
| Effectiveness of antibiotic prophylaxis | Meta-analysisB1 | Reduction in deep wound infections (RR, 0.29; 95% CI, 0.15 to 0.55) | Patients should receive antibiotics before hip fracture surgery. | A | |
| Reduction in superficial wound infections (RR, 0.48; 95% CI, 0.28 to 0.81) | |||||
| Reduction in urinary tract infections (RR = 0.66; 95% CI, 0.43 to 1.00) | |||||
| Optimal timing of antibioticadministration | Cohort studyB2 | Incidence of infection: | Antibiotic prophylaxis should be initiated within the two hours before hip fracture surgery. | B | |
| Less than two hours before surgery: 0.6 percent | |||||
| Two to 24 hours before surgery: 3.8 percent | |||||
| Three hours after surgery: 1.4 percent | |||||
| Three to 24 hours after surgery: 16 percent | |||||
| Multiple- versus single-dose perioperative antibiotic prophylaxis | Meta-analysisB3 | Trend toward reduction in postoperative infection with a multiple-dose regimen compared with a single-dose regimen (OR, 0.60; 95% CI, 0.18 to 2.02) | Multiple doses of antibiotics (e.g., three or four doses every eight hours) should be administered during the 24 to 36 hours after surgery. | B | |
SORT = strength of recommendation taxonomy; RR = relative risk; CI = confidence interval; OR = odds ratio.
*-A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see https://www.aafp.org/afpsort.xml.
Information from references:
B1. Gillespie WJ, Walenkamp G. Antibiotic prophylaxis for surgery for proximal femoral and other closed long bone fractures. Cochrane Database Syst Rev 2001;(1):CD000244.
B2. Classen DC, Evans RS, Pestotnik SL, Horn SD, Menlove RL, Burke JP. The timing of prophylactic administration of antibiotics and the risk of surgical-wound infection. N Engl J Med 1992;326:281-6.
B3. March L, Chamberlain A, Cameron I, Cumming R, Kurrle S, Finnegan T, et al. Prevention, treatment, and rehabilitation of fractured neck of femur. Report from the Northern Sydney Area Fractured Neck of Femur Health Outcomes Project. 1996. Accessed February 15, 2006, at: http://www.mja.com.au/public/issues/iprs2/march/fnof.pdf.
Urinary Tract Complications
Urinary tract infections and urinary retention are common problems after hip fracture surgery.17 Evidence supports removing indwelling urinary catheters within 24 hours of surgery to reduce the incidence of urinary retention.3 Transient urinary retention can be managed with intermittent sterile catheterization as needed. Physicians also should consider discontinuing medications that can contribute to urinary retention (e.g., anticholinergics, sedatives).
Delirium
Delirium may be the most common medical complication after hip fracture.18 Delirium may interfere with recovery and rehabilitation, increase duration of hospitalization, and increase mortality after one year.19 Common precipitating factors include electrolyte and metabolic abnormalities, inadequate pain control, infection, and psychoactive medications.
Physicians can help prevent delirium by avoiding polypharmacy, minimizing the use of anticholinergic and psychoactive medications, removing urinary catheters and intravenous lines as soon as possible, and minimizing sleep interruptions.20 If delirium occurs, a thorough evaluation and treatment of the underlying cause is needed. Patients who do not respond to conservative measures may benefit from low-dose tranquilizers (e.g., haloperidol [Haldol]) or atypical antipsychotics (e.g., risperidone [Risperdal], olanzapine [Zyprexa]). These agents should be discontinued as soon as possible after the delirium is resolved.
Pain Management
Optimal pain control is essential after hip fracture to ensure patient comfort and to facilitate rehabilitation. Routine assessment and formal charting of pain scores are important for successful pain control. Inadequate pain control after hip fracture is associated with poor short- and long-term functional recovery and longer hospitalization.21 An increased risk of delirium has been observed in patients who did not receive adequate postoperative pain control.22 Opioid analgesia in this setting does not increase the risk of delirium.23,24
Immediately after surgery, pain is best managed with patientcontrolled analgesia with morphine. Intravenous or oral opiates may be needed for subsequent pain control, particularly during physical therapy sessions. Regularly scheduled doses of stool softeners and laxatives can prevent constipation caused by opioid use. Meperidine (Demerol), propoxyphene (Darvon), and pentazocine (Talwin) should be avoided for pain control in older patients because of the risk of adverse side effects.25
Rehabilitation
Rehabilitation is essential after hip fracture. Prolonged bed rest can increase the risk of pressure sores, atelectasis, pneumonia, deconditioning, and thromboembolic complications. Weight bearing immediately after hip fracture surgery is safe in most patients.3,20 Figure 126,27 is an algorithm for rehabilitation after hip fracture surgery.
Figure 1. Rehabilitation After Hip Fracture Surgery
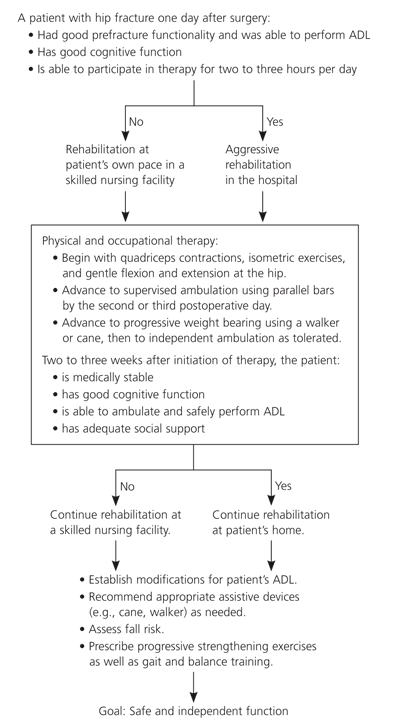
Algorithm for rehabilitation after hip fracture surgery. (ADL = activities of daily living.)
Information from references 26 and 27.
Cohort studies3,28 suggest that intense physical therapy (twice-daily therapy sessions) may help improve long-term functional outcomes. Ideally, rehabilitation should begin on the first postoperative day with quadriceps contractions, isometric exercises, and gentle flexion and extension at the hip.26 On the second or third postoperative day, the patient may begin supervised ambulation using parallel bars for support, advancing to a walker or cane and then to independent ambulation as tolerated.26
The length of the cane is important for stability and should be adjusted to allow 20 to 30 degrees of flexion at the elbow when the cane is held at the side.26 The patient should hold the cane with the hand opposite the injured hip. Typically, the cane should support approximately 15 to 20 percent of the patient’s total body weight.26 Multiple-legged canes (quadripod or tripod canes) have increased support at the base but are heavier and more difficult to use. If a cane does not offer adequate stability, a pick-up walker may be more effective. The patient lifts the pick-up walker, moves it forward, and advances before lifting the walker again. The patient must have the strength to lift the walker and the cognitive function to learn the proper coordination.27 A wheeled walker allows a smoother, more coordinated, and faster gait and may be beneficial in patients who are cognitively impaired.27 Crutches can support a patient’s full body weight but have several disadvantages. For example, patients need increased arm strength, there is a risk of brachial plexus injury, and they create an unnatural gait pattern.27 Continued physical therapy is crucial after discharge from the hospital to ensure optimal functional recovery.
Prevention
Appropriate follow-up after hospitalization includes assisting patients with recovery and instituting secondary prevention strategies. Two major risk factors for hip fracture are osteoporosis and falls.
OSTEOPOROSIS PREVENTION
Primary prevention of osteoporosis should begin with an assessment of the patient’s risk of osteoporosis to determine the need for bone mineral density (BMD) screening. Guidelines from the National Osteoporosis Foundation (NOF),29 the U.S. Preventive Services Task Force (USPSTF),30 and the American Academy of Family Physicians31 recommend routine BMD screening to detect osteoporosis in women older than 65 years. The USPSTF also recommends screening postmenopausal women 60 to 64 years of age who have risk factors for osteoporosis in addition to menopause.30 A meta-analysis32 showed that a BMD measurement at the hip that falls one standard deviation below the mean is associated with a 2.6 relative risk of hip fracture. Table 130,33 lists risk factors for hip fracture in postmenopausal women.
To reduce bone loss, physicians should encourage postmenopausal women to participate in regular weight-bearing exercise, to quit smoking, to limit alcohol intake, and to receive at least 1,500 mg of elemental calcium and 600 to 800 IU of vitamin D per day. The NOF recommends drug therapy for postmenopausal women with BMD T-scores less than −2 and no additional risk factors for osteoporosis and for those with BMD T-scores less than −1.5 and one or more additional risk factors.29 Table 229 summarizes FDA-approved therapies for the prevention and treatment of osteoporosis.
TABLE 1 Risk Factors for Hip Fracture in Postmenopausal Women
| Age older than 65 years |
| Any fracture since 50 years of age |
| Current use of benzodiazepines, anticonvulsants, or caffeine |
| High resting pulse rate |
| History of maternal hip fracture |
| Hyperthyroidism |
| Inability to rise from a chair without using arms |
| No weight gain since 25 years of age |
| Not walking for exercise |
| On feet four hours or less per day |
| Poor depth perception and visual contrast sensitivity |
| Poor health perception |
| Tall height |
TABLE 2 Therapies Approved by the FDA for the Prevention and Treatment of Osteoporosis
| Medication | Dosage | Comments | |
|---|---|---|---|
| Alendronate (Fosamax)* | 10 mg orally per day (5 mg orally per day for prevention) or 70 mg orally per week (35 mgorally per week for prevention) | Reduces the risk of vertebral and nonvertebral fracture; may cause esophageal irritation; once per week dosing may improve compliance; should be taken on an empty stomach and with 8 oz of water | |
| Calcitonin (Miacalcin) † | 200 IU per day (nasal spray) | Reduces the risk of vertebral fracture; may cause nausea or irritate the nasal mucosa | |
| Ibandronate (Boniva)* | 2.5 mg orally per day or 150 mg orally per month | Reduces the risk of vertebral fracture; may cause esophageal irritation; once a month dosing may improve compliance; should be taken on an empty stomach and with 8 oz of water | |
| Raloxifene (Evista)* | 60 mg orally per day | Reduces the risk of vertebral fracture; increases risk of thromboembolic complications; should be avoided before hip fracture surgery | |
| Risedronate (Actonel)* | 5 mg orally per day or 35 mg orally per week | Reduces the risk of vertebral and nonvertebral fracture; may cause esophageal irritation; once per week dosing may improve compliance; should be taken on an empty stomach and with 8 oz of water | |
| Teriparatide (Forteo)† | 20 mcg subcutaneously per day | Reduces the risk of vertebral and nonvertebral fracture; may cause nausea or headache; should be avoided in patients with high risk of osteosarcoma, Paget’s disease, prior radiation therapy of the skeleton, bone metastasis, hypercalcemia, or history of skeletal malignancy | |
FDA = U.S. Food and Drug Administration.
*—Indicated by the FDA for the prevention and treatment of osteoporosis.
† —Indicated by the FDA for the treatment of osteoporosis.
Information from reference 29.
FALL PREVENTION
Interventions to reduce the risk of falls should target identified risk factors (e.g., muscle weakness; history of falls; use of four or more prescription medications; use of an assistive device; arthritis; depression; age older than 80 years; impairments in gait, balance, cognition, vision, or activities of daily living). Interventions include prescribing strengthening exercises combined with gait and balance training; assessing the patient’s home and eliminating hazards; and monitoring and adjusting the patient’s medications.34 A meta-analysis35 showed that hip protectors may help prevent hip fractures in patients who have a high risk of falling and in older patients living in nursing homes.
Conservative Management
Conservative nonsurgical management of hip fracture should be considered for nonambulatory patients with advanced dementia. Returning these patients to their home environment may be the most effective way to avoid hospitalization-related complications (e.g., delirium, nosocomial infections). Treatment should focus on aggressive pain management and rehabilitation to prevent stiffness and weakness of the extremities. Patients may become mobile as tolerated.

