Pleuritic chest pain is a common presenting symptom and has many causes, which range from life-threatening to benign, self-limited conditions. Pulmonary embolism is the most common potentially life-threatening cause, found in 5 to 20 percent of patients who present to the emergency department with pleuritic pain. Other clinically significant conditions that may cause pleuritic pain include pericarditis, pneumonia, myocardial infarction, and pneumo-thorax. Patients should be evaluated appropriately for these conditions before an alternative diagnosis is made. History, physical examination, and chest radiography are recommended for all patients with pleuritic chest pain. Electrocardiography is helpful, especially if there is clinical suspicion of myocardial infarction, pulmonary embolism, or pericarditis. When these other significant causes of pleuritic pain have been excluded, the diagnosis of pleurisy can be made. There are numerous causes of pleurisy, with viral pleurisy among the most common. Other etiologies may be evaluated through additional diagnostic testing in selected patients. Treatment of pleurisy typically consists of pain management with nonsteroidal anti-inflammatory drugs, as well as specific treatments targeted at the underlying cause.
Pleurisy is inflammation of the parietal pleura that typically results in characteristic pleuritic pain and has a variety of possible causes. The term “pleurisy” is often used to refer to a symptom and a condition. It is more precise to use the term “pleurisy” for the condition and “pleuritic pain” to describe the symptom. Pleuritic pain is a key feature of pleurisy; therefore, this article reviews the physiology and classic characteristics of pleuritic pain, focusing on the presentation and diagnosis of the patient and the management of various causes of pleurisy.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A thorough history and physical examination should be performed to diagnose or exclude life-threatening causes of pleuritic pain before making a diagnosis of pleurisy. | C | 3,9,19,22,29 |
| Pulmonary embolism is the most common life-threatening cause of pleuritic chest pain and should be considered in all patients with this symptom. Evaluation should be performed using validated clinical decision rules, D-dimer testing, and imaging studies as needed. | C | 19 |
| Patients with pleuritic pain should have chest radiography to evaluate for underlying pneumonia. | C | 9 |
| Nonsteroidal anti-inflammatory drugs should be used to control pleuritic pain. | B | 30,31 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page1289 orhttps://www.aafp.org/afpsort.xml.
Pathophysiology
The visceral pleura does not contain any noci-ceptors or pain receptors. The parietal pleura is innervated by somatic nerves that sense pain when the parietal pleura is inflamed. Inflammation that occurs at the periphery of the lung parenchyma can extend into the pleural space and involve the parietal pleura, thereby activating the somatic pain receptors and resulting in pleuritic pain. Parietal pleurae of the outer rib cage and lateral aspect of each hemidiaphragm are innervated by intercostal nerves. Pain is localized to the cutaneous distribution of those nerves. The phrenic nerve supplies innervations to the central part of each hemidiaphragm; when these fibers are activated, the sensation of pain is referred to the ipsilateral neck or shoulder.
Differential Diagnosis
It is important that physicians first consider potentially life-threatening disorders such as pulmonary embolism, myocardial infarction, and pneumothorax when a patient presents with pleuritic chest pain.1–5 One study of a consecutive series of patients presenting to the emergency department with pleuritic chest pain found that 5 percent had a pulmonary embolism6; in another study, the proportion was 21 percent.7 Pericarditis and pneumonia are two other significant causes of pleuritic chest pain that should be considered before pleurisy is diagnosed.8,9 The differential diagnosis of pleurisy when these causes have been ruled out is presented in Table 1.2,10–18
Viral infection is one of the most common causes of pleurisy. Viruses that have been linked as causative agents include influenza, parainfluenza, coxsackieviruses, respiratory syncytial virus, mumps, cytomegalovirus, adenovirus, and Epstein-Barr virus.10–12 Additionally, pleurisy may be the first manifestation of some less-common disorders.
Table 1 Differential Diagnosis of Pleurisy*
| Category | Etiology |
|---|---|
| Cardiac | Post–cardiac injury syndrome, post–myocardial infarction syndrome (dressler's syndrome), postpericardiotomy syndrome (postcommissurotomy syndrome) |
| Exposure | Asbestosis, some medications† |
| Gastrointestinal | Inflammatory bowel disease, spontaneous bacterial pleuritis |
| Genetic | Familial Mediterranean fever |
| Hematologic/oncologic | Malignancy, sickle cell disease |
| Infectious | Viral (e.g., adenovirus, coxsackieviruses, cytomegalovirus, Epstein-Barr virus, influenza, mumps, parainfluenza, respiratory syncytial virus) |
| Bacterial (e.g., Mediterranean spotted fever, parapneumonic or tuberculous pleuritis) | |
| Parasitic (e.g., amebiasis, paragonimiasis) | |
| Inflammatory | Reactive eosinophilic pleuritis |
| Renal | Chronic renal failure, renal capsular hematoma |
| Rheumatologic | Lupus pleuritis, rheumatoid pleuritis, Sjögren's syndrome |
*—Assumes pulmonary embolism, myocardial infarction, pneumothorax, pericarditis, and pneumonia have been ruled out as the cause of pleuritic chest pain.
†—Drugs known to cause pleural disease include amiodarone (Cordarone), bleomycin (Blenoxane), bromocriptine (Parlodel), cyclophosphamide (Cytoxan), methotrexate, methysergide (Sansert; not available in the United States), minoxidil (Loniten), mitomycin (Mutamycin), oxyprenolol (Apsolox; not available in the United States), practolol (Eraldin; not available in the United States), procarbazine (Matulane), and sclerotherapeutic agents. Drugs that may cause lupus pleuritis include hydralazine (Apresoline), procainamide (Pronestyl), and quinidine.
Presentation
Patients with pleuritic pain present in different ways depending on the underlying cause. Pleuritic pain typically is localized to the area that is inflamed or along predictable referred pain pathways. Patients' descriptions of the pain are consistent in most cases of pleurisy. The classic feature is that forceful breathing movement, such as taking a deep breath, talking, coughing, or sneezing, exacerbates the pain
Patients often relate that the pain is sharp and is made worse with movement. Typically, they will assume a posture that limits motion of the affected area. Pain with respiration may cause patients to complain of shortness of breath or dyspnea.
Evaluation
A recommended approach for the evaluation of patients presenting with pleuritic chest pain is given in Figure 1.3–5,8,9,19–22 Evaluation of patients in whom pulmonary embolism is suspected should include an assessment of the probability of pulmonary embolism using a validated clinical decision rule, such as the Wells rule,19 and a d-dimer test. Computed tomography or ventilation-perfusion scanning may be required in patients who are at moderate or high risk or who have an abnormal D-dimer test result.20
Figure 1. Outpatient Diagnosis of Pleuritic Pain
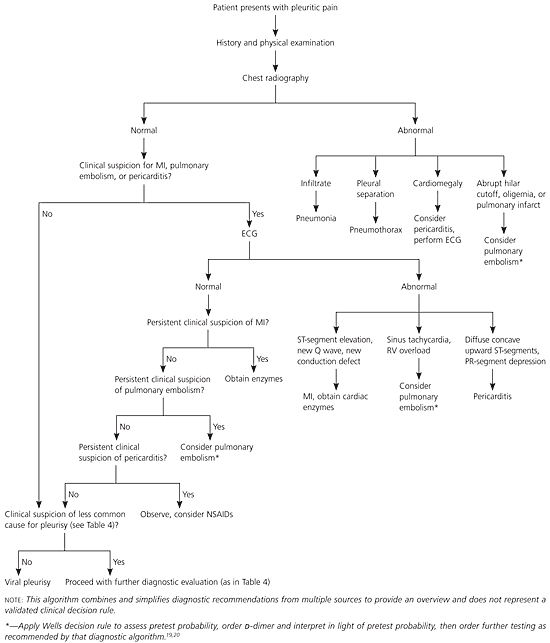
Algorithm for the outpatient diagnosis of pleuritic pain. (MI = myocardial infarction; ECG = electrocardiography; RV = right ventricular; NSAIDs = nonsteroidal anti-inflammatory drugs.)
Information from references 3 through 5, 8,9, and 19 through 22.
MEDICAL HISTORY
A careful, focused history is the first step in identifying the underlying etiology of pleuritic pain. A key question is the time course of the onset of symptoms (Table 22 ).
Although pleuritic pain decreases the likelihood that a patient with chest pain is experiencing myocardial ischemia, it does not eliminate the possibility.3 If other history findings suggest this diagnosis, further evaluation with electrocardiography (ECG) and cardiac enzymes, as well as close observation, is indicated. Pain that worsens while the patient is supine and lessens while the patient is upright should prompt consideration of pericarditis.8,21 Dyspnea associated with the pain should raise clinical suspicion for pulmonary embolism, pneumonia, and pneumothorax.5,9,23
Table 2 Etiologies of Pleuritic Pain by symptom onset
| Onset | Etiologies |
|---|---|
| Acute (i.e., minutes to hours) | Myocardial infarction |
| Pulmonary embolism | |
| Spontaneous pneumothorax | |
| Trauma | |
| Subacute (i.e., hours to days) | Infection |
| Inflammatory process | |
| Chronic (i.e., days to weeks) | Malignancy |
| Rheumatoid arthritis | |
| Tuberculosis | |
| Recurrent | Familial Mediterranean fever |
Information from reference 2.
Features that are associated with life-threatening causes of pleuritic pain are listed in Table 3.3–5,8,9,21,22 Other symptoms, such as malaise, weight loss, night sweats, and joint pains, may indicate one of the less-common causes of pleurisy. It is important to investigate the patient's underlying medical conditions, medication list, and recent travel history, and to take a history of similar symptoms in family members. A selected differential diagnosis with associated clinical results is listed in Table 4.13–18,24–27
Table 3 Findings associated with life-threatening causes of Pleuritic Pain
| Diagnosis | History | Physical examination | Chest radiography | Electrocardiography |
|---|---|---|---|---|
| Myocardial infarction | Substernal pain that radiates, dyspnea, shortness of breath | Diaphoresis, hypotension, third heart sound (S3) | Usually normal | ST-T elevations (especially if new), new Q wave, new conduction defect |
| Pleuritic pain decreases likelihood ratio | ||||
| Pericarditis | Positional pain: increases while supine and decreases when upright | Pericardial friction rub | Increased heart size with pericardial effusion greater than 250 mL | Diffuse concave upward ST-segments, PR- segment depression |
| Abnormality noted in more than 90 percent of cases | ||||
| Pneumonia | Anorexia, cough, dyspnea, fatigue, myalgia | Crackles, egophony, fremitus | Infiltrate | Typically not indicated |
| Pneumothorax | Sudden pain and dyspnea | Tachycardia, hyperresonance, decreased breath sounds, decreased wall movement | Thin pleural line | Typically not indicated |
| May be normal in small pneumothorax | Sinus tachycardia | |||
| Pulmonary embolism | Prior embolism or clot | Tachycardia, tachypnea | Abrupt hilar cutoff, oligemia, or pulmonary consolidations compatible with infarction | Sinus tachycardia, right ventricular overload (T-wave inversion in right precordial leads, S1Q3/S1Q3T3, transient right bundle branch block, pseudoinfarction, S1S2S3) |
| Cancer, immobilization, estrogen use, or recent surgery | ||||
| Dyspnea, syncope |
Table 4 Findings Associated with Selected Causes of Pleurisy
| Diagnosis | History | Physical examination | Selected diagnostic test results | |
|---|---|---|---|---|
| Connective tissue disorders | Prior diagnosis of systemic lupus erythematosus, rheumatoid arthritis, or other connective tissue disorder should raise suspicion, but pleuritic chest pain may be initial presentation Fever; arthritis or arthralgias | Decreased breath sounds | Chest radiography: small to moderate unilateral or bilateral effusion PFA: exudative effusion (rheumatoid arthritis characterized by low glucose level [< 40 mg per dL (2.2 mmol per L)], elevated lactic dehydrogenase level [> 700 U per L], and low pH [< 7.2]) Abnormal disease-specific serologic markers | |
| Drug-induced pleuritis | Use of drug known to cause drug-induced pleural disease or drug-induced lupus pleuritis* | Possible decreased breath sounds, pleural friction rub | Chest radiography: may be normal or demonstrate infiltrate, pleural effusion, or pleural thickening PFA: exudative effusion | |
| Familial Mediterranean fever | Recurrent episodes of fever (one to four days) associated with abdominal, chest, or joint pain or erysipelas-like skin disease Mediterranean descent Family history of familial Mediterranean fever | Normal between episodes During episodes: temperature of 100 to 104° F (38 to 40° C) and signs of serositis (e.g., peritoneal irritation, pleural and/or pericardial friction rub) Other possible findings: joint swelling, unilateral erythema over extensor surface of leg, ankle, or foot | Increased acute phase reactants (ESR, CRP, WBC, fibrinogen) Positive mutation analysis for MEFV gene | |
| Post–cardiac injury syndrome† | Recent myocardial infarction, cardiac procedure, or chest trauma Fever, dyspnea, pleuropericardial pain | Pleural and/or pericardial friction rub; decreased breath sounds | Chest radiography: may reveal pleural effusion PFA: exudative effusion Elevated ESR, leukocytosis Electrocardiographic abnormalities similar to pericarditis (see Table 3) | |
| Tuberculous pleuritis | Exposure to environment with high risk of Mycobacterium tuberculosis Cough, low-grade fever, weight loss, fatigue Human immunodeficiency virus infection | Unilaterally decreased breath sounds | Chest radiography: small to moderate unilateral pleural effusion, often without associated infiltrate PFA: exudative effusion with elevated adenosine deaminase levels (> 40 to 60 U per L [670 to 1,000 nkat per L]) Caseous granulomas on pleural biopsy Culture positive for M. tuberculosis on induced sputum, pleural fluid culture, or pleural biopsy Negative PPD result does not exclude diagnosis | |
| Viral pleurisy | Recent respiratory illness or undifferentiated febrile illness | Rapid, shallow respirations; pleural friction rub | Chest radiography: normal | |
PFA = pleural fluid analysis; ESR = erythrocyte sedimentation rate; CRP = C-reactive protein; WBC = white blood cell count; PPD = purified protein derivative.
*—Drugs known to cause pleural disease include amiodarone (Cordarone), bleomycin (Blenoxane), bromocriptine (Parlodel), cyclophosphamide (Cytoxan), methotrexate, methysergide (Sansert; not available in the United States), minoxidil (Loniten), mitomycin (Mutamycin), oxyprenolol (Apsolox; not available in the United States), practolol (Eraldin; not available in the United States), procarbazine (Matulane), and sclerotherapeutic agents. Drugs that may cause lupus pleuritis include hydralazine (Apresoline), procainamide (Pronestyl), and quinidine.
†—Post–cardiac injury syndrome includes post–myocardial infarction syndrome (Dressler's syndrome) and postpericardiotomy syndrome (postcommissurotomy syndrome).
Information from references 13 through 18 and 24 through 27.
PHYSICAL EXAMINATION
The normally smooth surfaces of the parietal and visceral pleurae become rough with inflammation. As these surfaces rub against one another, a rough scratching sound, or friction rub, may be heard with inspiration and expiration. This friction rub is a classic feature of pleurisy. It may also occur in about 4 percent of patients with pneumonia and 4 percent of patients with pulmonary embolism.28 Additional physical findings on the pulmonary examination may include decreased breath sounds, rales, and egophony, especially in patients with underlying pneumonia.9
Other physical examination findings that raise clinical suspicion for certain conditions include the pericardial rub of pericarditis5 and the hyperresonance and decreased wall movement that occur with pneumothorax.8 Physical examination findings associated with life-threatening conditions that cause pleuritic pain are listed in Table 3.3–5,8,9,21,22 Further physical examination is directed by the etiology suggested by the clinical history. It is important to remember that patients with any of these serious conditions who present with pleuritic pain may have a normal physical examination, and a high index of suspicion and further diagnostic testing are often indicated.
DIAGNOSTIC TESTS
Because pleuritic chest pain may be a presenting complaint for pneumonia, pulmonary embolism, or pneumothorax,1,9 all patients presenting with this symptom should have chest radiography. Additionally, pleurisy often is associated with a pleural effusion, which can be identified on a chest radiograph. Pleural fluid can be examined for further etiologic clues (Table 529 ).
Table 5 Initial evaluation of Pleural Fluid
| Quality | Test indicated | Interpretation | |
|---|---|---|---|
| Appearance | |||
| Bloody | Hematocrit | < 1 percent: nonsignificant 1 to 20 percent: cancer, pulmonary embolus, or trauma > 50 percent peripheral hematocrit: hemothorax | |
| Cloudy or turbid | Centrifugation | Turbid supernatant: chylothorax | |
| Odor | |||
| Putrid | Stain and culture | Possible anaerobic infection | |
| Distinguishing transudate from exudate | |||
| Light's criteria | Fluid is exudate if it meets one or more of the following criteria:
| ||
| Confirmation of Light's criteria assessment* | Fluid is exudate if:
| ||
LDH = lactate dehydrogenase.
*—To use when patient's clinical appearance suggests transudative effusion.
Adapted with permission from Light RW. Pleural effusion. N Engl J Med 2002; 346:1974.
ECG evaluation is recommended if there is clinical suspicion of myocardial infarction, pulmonary embolism, or pericarditis.3,21,28 Typical ECG findings associated with these conditions are listed in Table 3.3–5,8,9,21,22 When the etiology of pleurisy is other than viral, further diagnostic testing may be indicated in selected patients (Table 413–18,24–27 ).
Treatment
Management of pleurisy has two primary goals: (1) control the pleuritic chest pain, and (2) treat the underlying condition. To achieve pain control, nonsteroidal anti-inflammatory drugs (NSAIDs) commonly are prescribed as the initial therapy. Narcotic analgesics may be required to relieve severe pleuritic chest pain; however, NSAIDs do not suppress respiratory efforts or cough reflex and are the preferred first-line agent.
Although a class effect is presumed, human studies on the use of NSAIDs to treat pleuritic chest pain have been limited to indomethacin (Indocin). Indomethacin, in dosages of 50 to 100 mg orally up to three times per day with food, has been found to be effective in relieving pleural pain, with associated improvement in mechanical lung function.30,31 Supportive care with adequate pain control is the goal in the treatment of viral pleurisy.
To achieve the second management goal, therapies are selected based on the underlying condition. If a patient has suspected drug-induced pleuritis or drug-induced lupus pleuritis, the causal agent should be discontinued.16,17 Smoking cessation should be advised for patients with pleurisy caused by asbestosis.32 Antimicrobial and antiparasitic agents are selected empirically based on the suspected underlying organism. Decortication is considered in cases of pleuritis associated with refractory pleural effusions resulting from malignancy, chronic renal failure, or rheumatoid pleurisy.2 Colchicine (1.2 to 2.0 mg orally once per day, or twice per day in a divided dose) is the mainstay of treatment for familial Mediterranean fever.18
NSAIDs are first-line therapy for patients with post–cardiac injury syndrome; corticosteroids are reserved for those who are intolerant of or experience no response to NSAIDs.14 Although oral corticosteroids are recommended for patients with lupus pleuritis, they have not been demonstrated to influence the course of rheumatoid pleuritis.2,15
The role of systemic corticosteroids in the treatment of tuberculous pleuritis is controversial. Tuberculous pleuritis is associated with inflammation and fibrosis, and a small number of randomized and quasi-randomized studies with patients who did not have human immunodeficiency virus have assessed the impact of steroids on this process.33 No difference was detected in the primary outcome of an alteration in residual lung function. Although these studies did show a trend toward benefit (reduction in the number of patients with pleural effusions, thickening, or adhesions), there is insufficient evidence to determine whether steroids are an effective treatment.33

