A 61-year-old woman presented with increased muscle mass in her back (see accompanying figure) and myalgia that persisted for four months. Associated symptoms included progressive dysphagia and weight loss of 6 lb, 10 oz (3 kg) since the onset of symptoms. She was taking captopril (Capoten) for hypertension and alendronate (Fosamax) for osteoporosis. The patient had a history of renal disease, but she could not provide details.
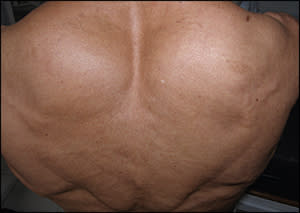
Her blood pressure was 140/80 mm Hg. Although the patient is a homemaker and does not exercise, the physical examination revealed generalized muscular hypertrophy and discrete macroglossia, but was otherwise unremarkable. The complete blood count, erythrocyte sedimentation rate, glucose level, and liver function were within normal limits. Urinalysis showed proteinuria, although serum blood urea nitrogen and creatinine levels were normal. A urine protein measurement showed an excretion of 2.9 g per 24 hours. Renal ultrasonography revealed increased renal dimensions bilaterally. Serum and urine protein electrophoresis test results were normal.
Question
Based on the patient's history, physical examination, and laboratory results, which one of the following is the most likely diagnosis?
A. Amyloidosis.
B. Duchenne's muscular dystrophy.
C. Hypothyroidism.
D. Inclusion body myositis.
E. Polymyositis.
Discussion
The answer is A: amyloidosis. Amyloidosis is a rare, heterogeneous group of illnesses characterized by the accumulation of insoluble amyloid proteins within tissues. This disrupts tissue architecture and leads to organ dysfunction.1 For example, the muscular pseudohypertrophy in this patient is caused by amyloid protein accumulation between muscle cells. There are variable clinical manifestations depending on the distribution and type of precursor protein.
Light chain–related amyloidosis (AL type) is the most common form and may cause unspecific symptoms, such as fatigue, myalgia, and weight loss. About 30 percent of patients with light chain–related amyloidosis have renal involvement, characterized by proteinuria. Nephrotic-range proteinuria or nephrotic syndrome may be the initial feature.1 Other initial features include restrictive cardiomyopathy, hepatomegaly, splenomegaly, peripheral nervous system involvement, and macroglossia. Muscle pseudohypertrophy rarely occurs.2–4
Amyloidosis can be diagnosed when the presence of amyloid protein and a plasma cell dyscrasia is demonstrated. In this patient, a Congo red test revealed the apple-green birefringence characteristic of amyloid protein. The presence of serum or urine monoclonal light chain is also diagnostic; however, immunofixation electrophoresis is preferred because concentrations may be too low for standard electrophoresis. A serum-free light chain assay is another diagnostic option. Bone marrow biopsy detects M- or L-producing plasma cells and is needed to rule out multiple myeloma.1
Although myalgia is a clinical manifestation of polymyositis and hypothyroidism, muscle hypertrophy does not occur with these disorders. Muscular hypertrophy sometimes occurs with inclusion-body myositis,5 but not in the pelvic or scapular girdle. Duchenne's muscular dystrophy is an X-linked recessive disorder; calf pseudohypertrophy is a typical clinical feature.6 Duchenne's muscular dystrophy occurs almost exclusively in males, with symptoms beginning in childhood.
Summary Table
| Condition | Characteristics |
|---|---|
| Amyloidosis | Heterogeneous; muscle pseudohypertrophy is rare |
| Duchenne's muscular dystrophy | Calf pseudohypertrophy is typical |
| Hypothyroidism | Myalgia without muscular hypertrophy |
| Inclusion body myositis | Muscular hypertrophy is present, but not in the pelvic or scapular girdle |
| Polymyositis | Myalgia without muscular hypertrophy |

