Breastfeeding provides significant health benefits for infants and mothers. However, the United States continues to fall short of the breastfeeding goals set by the Healthy People 2010 initiative. The American Academy of Family Physicians, the American Academy of Pediatrics, and the American College of Obstetrics and Gynecology have policy statements supporting breastfeeding that reflect recent advancements in understanding the mechanisms underlying the benefits of breastfeeding and in the clinical management of breastfeeding. Despite popular belief, there are few contraindications to breastfeeding. Providing maternal support and structured antenatal and postpartum breastfeeding education are the most effective means of achieving breastfeeding success. In addition, immediate skin-to-skin contact between mother and infant and early initiation of breastfeeding are shown to improve breastfeeding outcomes. When concerns about lactation arise during newborn visits, the infant must be carefully assessed for jaundice, weight loss, and signs of failure to thrive. If a work-up is required, parents should be supported in their decision to breastfeed. Certified lactation consultants can provide valuable support and education to patients. Physicians should educate working women who breastfeed about the availability of breast pumps and the proper storage of expressed breast milk. Physicians must be aware of their patients' lactation status when prescribing medications, as some may affect milk supply or be unsafe for breastfeeding infants. Through support and encouragement of breastfeeding, national breastfeeding goals can be met.
Breast milk is the preferred nutritional source for all newborns and infants through the first six months of life1 and is widely recommended through the first year.2–4 Infants who are exclusively formula-fed have higher incidence of diarrhea,3 otitis media,3 respiratory tract infections,5 urinary tract infections,1 and bacterial infections.2 Premature formula-fed infants lack the developmental benefits that have been seen in exclusively breastfed infants.3 In the United States, exclusively formula-fed infants have a 21 percent higher postneonatal mortality rate.2,6 Mothers who never breastfeed have higher rates of breast and ovarian cancer, slower return to prepregnancy weight, and increased postpartum bleeding.2,3 Therefore, the American Academy of Family Physicians (AAFP),7 the American Academy of Pediatrics (AAP),2 and the American College of Obstetrics and Gynecology8 have composed policy statements strongly supporting breastfeeding. Additionally, a systematic review performed for the Agency for Healthcare Research and Quality found that breastfeeding was strongly associated with health benefits in observational studies.9 Table 1 lists the benefits of breastfeeding.2
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should recommend that pregnant patients and their partners attend a structured prenatal breastfeeding education program that teaches feeding techniques and aims to build maternal confidence. | B | 2, 17, 22, 24 |
| Unless contraindicated by a medical condition, mothers should have immediate skin-to-skin contact with their infants through the first feeding to increase the likelihood of breastfeeding success, and should be encouraged to room-in, feed on demand, and avoid supplements and pacifiers in their infants. | A | 2, 3, 20–22 |
| Hospital systems should be encouraged to adopt the Baby-Friendly Hospital Initiative. | B | 17, 21, 22 |
| Ensure close follow-up at three to five days and again at seven to 14 days after hospital discharge for breastfed babies. | C | 2, 15, 23 |
| Women with low milk supply should first undergo intensive evaluation by a certified lactation consultant for problems in breastfeeding technique; formula supplementation may be considered as a secondline option. | C | 2 |
| Breastfeeding babies should receive a daily dose of oral vitamin D drops (200 IU) beginning in the first two months of life and persisting until 500 mL of vitamin-D fortified formula or breast milk is consumed daily. | C | 2, 28–33 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see https://www.aafp.org/afpsort.xml
Table 1 Benefits of Breastfeeding
| Disease prevention |
| Decreased risk of asthma, Hodgkin's disease, hypercholesterolemia, leukemia, obesity, type 1 and 2 diabetes |
| Decreased hospitalizations for lower respiratory illnesses and sudden infant death syndrome |
| Nutritional |
| Human milk is species-specific and superior to substitutes |
| Immunologic |
| Decrease in bacterial meningitis, bacteremia, diarrhea, late-onset sepsis, necrotizing enterocolitis, otitis media, respiratory tract infections, urinary tract infections |
| Developmental |
| Improved developmental outcomes in premature infants |
| Psychologic |
| Analgesic effects during painful procedures |
| Maternal health |
| Decrease in risk of breast and ovarian cancers, decreased postpartum bleeding, earlier return to prepregnancy weight, lactation amenorrhea |
| Economic |
| A decrease of $3.6 billion in annual health care costs, decreased cost for public supplementation programs (e.g., Women, Infants, and Children program), and decreased patient costs |
| Environmental |
| Decreased disposal of formula cans and bottles |
Information from reference 2.
The Healthy People 2010 initiative aims for 75 percent of all U.S. mothers to attempt breastfeeding, 50 percent to continue breast-feeding for six months after birth (25 percent exclusively), and 25 percent to continue breastfeeding for one year after birth.10,11 The World Health Organization (WHO),12 the AAFP,7 and the AAP2 support continued breastfeeding up to two years of age or beyond.
National Breastfeeding Rates
The Centers for Disease Control and Prevention (CDC) report that only 73.8 percent of physically capable U.S. women attempt breastfeeding.11 By three months after birth, only 30.5 percent and by six months after birth, only 11.3 percent breastfeed exclusively.11 Figure 1 illustrates the percentage of infants in the United States who are being breastfed at six months of age by state.13
Figure 1.
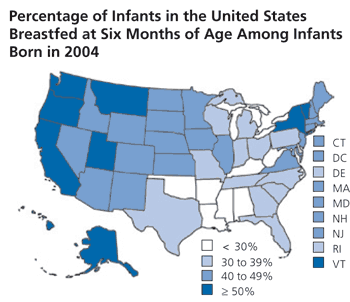
Map showing percentage of infants in the United States who are breastfed at six months of age by state among infants born in 2004.
Adapted from Centers for Disease Control and Prevention. Map 2. Percent of children breastfed at 6 months of age by state among children born in 2004. http://www.cdc.gov/breastfeeding/data/NIS_data/2004/map_2.htm. Accessed June 26, 2008.
In 2004, 21 states achieved the Healthy People 2010 objective of a 75 percent breast-feeding initiation rate in capable mothers.11 However, only nine states achieved the six-month goal and 12 states achieved the one-year goal. Alaska, California, Hawaii, Montana, Oregon, Utah, Vermont, and Washington were the only states to achieve all three of the Healthy People 2010 objectives.11 Consistent with previous research, this study also demonstrated that non-Hispanic black and socioeconomically disadvantaged groups have lower breastfeeding rates (Figure 2).14
Figure 2.
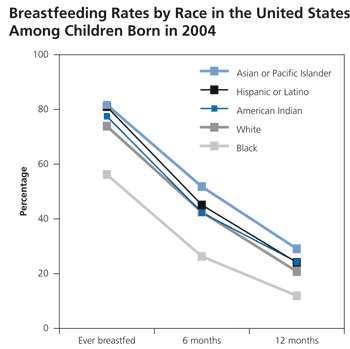
Graph showing breastfeeding rates by race in the United States among children born in 2004.
Information from reference 14.
Improving Initiation Success Rates
Most women decide by the beginning of the third trimester whether they will breast-feed.15 The single most effective intervention promoting breastfeeding initiation is an education program. A systematic review and meta-analysis found that one additional mother would initiate and continue breast-feeding for up to three months for every three to five women attending an educational program.16 The U.S. Preventive Services Task Force recommends structured breastfeeding education and behaviorally oriented counseling programs to increase breastfeeding initiation and maintenance.17 Therefore, persons who provide maternity care should encourage all patients and their partners to attend a breastfeeding education program that demonstrates the benefits of breast milk and its superiority to alternatives.
One study has shown that partner education resulted in an increase of breastfeeding initiation from 41 to 74 percent.18 A randomized controlled trial demonstrated that, with partner support, the prevalence of exclusive breastfeeding at six months was 25 percent compared with 15 percent in women who did not receive partner support.19 Breastfeeding education should begin as soon as antenatal visits commence.
Education in the immediate postpartum period is critical to facilitate breastfeeding success. A 2003 Cochrane review found that immediate skin-to-skin contact between mother and newborn improves breastfeeding outcomes.20 Postpartum breastfeeding should occur within the first hour of life, even if weighing, bathing, or administering medications (e.g., eye prophylaxis, vitamin K) are delayed.2,3,20,21
The Baby-Friendly Hospital Initiative (BFHI), an initiative of the WHO and the United Nations Children's Fund (UNICEF), recommends rooming-in (allowing mother and infant to remain together 24 hours a day), feeding on demand, and no artificial pacifiers or supplemental formula unless physician ordered.20,22 Hospital systems should be encouraged to adopt the BFHI.17,21,22 At institutions where BFHI recommendations are not used systemically, physicians should write orders specifying initiation of breast-feeding in the first hour of life, no supplementation, and no pacifier use. Twice daily formal evaluations of breastfeeding by available, skilled health care professionals also improve breastfeeding success rates.21
Postpartum Follow-up Visits
Twenty-five percent of women discontinue breastfeeding during the first week after delivery and 10 percent discontinue between weeks one and two. An additional 40 percent stop breastfeeding between two weeks and two months.15
Understanding the reasons for discontinuation is fundamental to increasing the duration of breastfeeding. A lack of maternal confidence causes early discontinuation of breastfeeding more often than lactation problems or a lack of knowledge.15 Earlier postpartum follow-up visits, at three to five days and at seven to 14 days, can provide an opportunity for the physician to intervene and reinforce the importance of continued breastfeeding.2,15,23
Nurse visits, including outpatient lactation consultant visits and telephone follow-ups, are helpful adjuncts to face-to-face physician contact. One randomized controlled trial in Mexico showed that women were more likely to breastfeed exclusively if they were supported with home visits; 64 percent of the women provided six visits were exclusively breastfeeding at three months versus 48 percent of women who were given three visits and 15 percent of those who did not receive this support.24
Parental concerns about insufficient milk production merit further evaluation. If a work-up is required, parents should be supported in their decision to breastfeed. Physicians should confirm that the infant is fed no less than every three hours and approximately 10 to 12 times daily. Every feeding should allow 10 to 15 minutes on each breast.2 Mothers should be asked about symptoms of breast engorgement and the sensation that their milk has come in, which generally occurs between 48 and 96 hours after delivery. The infant must be carefully assessed for jaundice, weight loss, and signs of failure to thrive. Percentage of birth weight lost should be calculated; a decrease in weight of more than 8 percent necessitates follow-up within 48 hours, and a bilirubin level should be drawn to assess for hyperbilirubinemia.
A loss of more than 10 percent of birth weight warrants careful assessment of other causes and consideration of admission to the hospital. In these infants, a certified lactation consultation may illuminate a cause.2 In recalcitrant patients, physicians may recommend a temporary measure of supplementation with breast milk or infant formula if breast milk is not available. Occasionally, galactagogues (e.g., metoclopramide [Reglan], fenugreek) have been used to increase breast milk supply.24 However, the evidence supporting their effectiveness is limited and they are associated with side effects in the mother and infant.25
Nipple sensitivity for the first 30 seconds to one minute of breastfeeding initiation is normal during the first week. However, patients who continue to experience nipple or breast problems after the first week must be evaluated.26 Reasons for breast pain include incorrect latch-on, cracked nipples, engorgement, and mastitis. The infant should grasp a large portion of the areola by latching on with a wide open mouth. Using breast milk and emollients to soften the nipple can reduce pain and dryness. Patients experiencing problems with engorgement or mastitis must be instructed in the importance of continued breast-feeding.26 Nonsteroidal anti-inflammatory drugs, massage, moist heat, and mechanical expression of breast milk help alleviate the acute pain associated with engorgement. After expressing milk, cold compacts and anti-inflammatory medications can reduce pain and edema. Cooled cabbage leaves have also been traditionally recommended, but show no clear benefit over placebo.27
Breast milk contains only small amounts of vitamin D.28 Therefore, physicians must be aware of the risk of rickets in infants who are breastfed.2,29 Concerns about skin damage from sun exposure appropriately compel parents to apply sunscreen and minimize sunlight exposure, thereby restricting vitamin D creation in the skin.30 Two recent case reports describe 34 modern cases of rickets, primarily in dark-skinned infants with minimal sun exposure.31,32 An observational study of 84 breastfed infants in Iowa demonstrated that 10 percent of breastfed infants had abnormally low vitamin D levels at 280 days of life. Vitamin D deficiency was more common in dark-skinned infants and during the winter months, when 78 percent of infants not given supplements were deficient.33 The AAP recommends a daily dose of oral vitamin D drops (200 IU) beginning in the first two months of life and persisting until 500 mL of vitamin-D fortified formula or milk is consumed daily.2,29 No studies show adverse effects of vitamin D supplementation at this dose.
Breastfeeding and Work
Eighteen percent of women report their job schedule as the reason for discontinuing breastfeeding.23 The Ross Mother's Trend Data (2003) showed that employed women have almost identical breastfeeding initiation rates as women who stay home (66.6 and 64.8 percent, respectively). At six months however, only 26.1 percent of women working full time are still breastfeeding compared with 35.0 percent of stay-at-home mothers.34
Physicians, nurses, and office staff can provide support to employed women in the early postpartum period. Mothers should be encouraged to start pumping and storing breast milk after breastfeeding is established and before they return to work. Breast milk can be left at room temperature for about eight hours, refrigerated for up to seven days, or be stored in a refrigerator-freezer for three to four months or in a separate freezer chest for up to one year. After thawed and gradually warmed in a container of water, breast milk should be used within 24 hours and then discarded.35 Breast milk should not be microwaved because uneven heating may denature essential proteins, detracting from the milk's beneficial health effects.36
Contraindications to Breastfeeding
The AAP recommends that women who have transmittable infections, such as human immunodeficiency virus, active untreated tuberculosis, or active herpes lesions on the breast, should not breastfeed.2 Additionally, mothers receiving diagnostic or therapeutic radioactive isotopes, antimetabolites, or chemotherapeutic agents, and mothers using illicit street drugs should not breastfeed during periods of exposure to these agents. Infants with homozygous galactosemia also should not be breastfed.1,2
Women who have breast implants or who are status postreduction mammoplasty can often breastfeed. In addition, carriers for hepatitis B or C and women who have a fever or postpartum infection, such as mastitis or endometritis, can also breastfeed.1,2,37 Although not ideal, smoking while lactating is not a contraindication.1 Tongue-tied infants38 and those with mild to moderate hyperbilirubinemia can also be breastfed.39 Table 2 lists conditions that are not contraindications to breastfeeding.2,3,8
Table 2 Conditions That Are Not Contraindications to Breastfeeding
| Condition | Comments |
|---|---|
| Breast augmentation (prior) | Consider antepartum lactation consultation |
| Fever or infection (including mastitis and endometritis) | Human immunodeficiency virus, active untreated tuberculosis, or active herpes lesions on the breast are contraindications |
| Hepatitis B or C carrier status | Infant should receive early vaccination, but breastfeeding is Encouraged |
| Hyperbilirubinemia (in the infant) | Mother must be monitored for adequate milk supply; infant should be monitored for signs of kernicterus |
| Multiple gestations | Most women can produce enough milk to fully breastfeed twins; lactation consultation is often needed |
| Women with higher-order multiple gestations may need to supplement with formula, but should be encouraged to breastfeed as much as possible | |
| Preterm birth | Expression of milk using a pump may be required early on, but a transition to breastfeeding is usually possible |
| Reduction mammoplasty (prior) | Consider antepartum lactation consultation |
| Smoking | Encourage cessation of all smoking in the household, but breastfeeding is not contraindicated |
| Tongue-tied infants | May require lactation consultation |
Breastfeeding and Medications
Most commonly prescribed postpartum medications are safe for breastfeeding women.40 Although a complete discussion of medication safety in lactation is beyond the scope of this article, Table 3 provides an overview of the safety of medications most often used by lactating women.40–43
Table 3 Safety of Medications in Mothers Who Are Breastfeeding
| Medication | Safety recommendation | Possible effect on infant | ||
|---|---|---|---|---|
| Analgesics | ||||
| Acetaminophen, ibuprofen (Motrin), opioids | Safe in commonly prescribed doses | — | ||
| High-dose aspirin | Second-line option | Platelet dysfunction; one case of metabolic acidosis | ||
| Meperidine (Demerol); naproxen (Naprosyn) | Use with caution | Long half-life may lead to accumulation in infant | ||
| Antibiotics | ||||
| Aminoglycosides | Safe | — | ||
| Cephalosporins | Safe | — | ||
| Fluoroquinolones | American Academy of Pediatrics considers safe | Possible risk of arthropathy | ||
| Macrolides | Use with caution | Erythromycin associated with increased incidence of pyloric stenosis | ||
| Concentrated in human milk | ||||
| Metronidazole (Flagyl) | Pump and discard breast milk during use and 24 hours after last dose | In-vitro mutagen; no association with cancer seen in humans | ||
| Nitrofurantoin (Furadantin) | Use with caution | Hemolysis in infant with G6PD deficiency | ||
| Penicillins | Safe | — | ||
| Sulfa drugs | Avoid use in first month | Elevates infant bilirubin levels | ||
| Tetracycline | Avoid prolonged use (greater than three weeks) | Tooth staining | ||
| Antihypertensives | ||||
| Angiotensin-converting enzyme inhibitors | Safe after four to six weeks | Possible renal toxicity in premature infants | ||
| Beta blockers | — | — | ||
| Atenolol (Tenormin) | Do not use | Cyanosis, bradycardia | ||
| Other beta blockers | Use with caution | Bradycardia | ||
| Calcium channel blockers | Use with caution | — | ||
| Antidepressants | ||||
| Fluoxetine (Prozac) | Weigh risks versus benefits | May cause colic, irritability, feeding and sleep disorders, slow weight gain | ||
| Sertraline (Zoloft), paroxetine (Paxil) | Excreted in breast milk, but infant serum levels very low or undetectable | No reported effect | ||
| Combined oral contraceptives | Avoid until breastfeeding well-established (60 to 90 days); low dose preferred | May decrease milk supply | ||
G6PD = glucose-6-phosphate dehydrogenase.
Multiple studies show that breastfeeding mothers do not adhere to prescribed medications, even when the drug is considered safe. It is important for physicians not only to discuss the safety of medication, but to reassure and support continued breastfeeding while taking medications.41

