Common signs and symptoms of streptococcal pharyngitis include sore throat, temperature greater than 100.4°F (38°C), tonsillar exudates, and cervical adenopathy. Cough, coryza, and diarrhea are more common with viral pharyngitis. Available diagnostic tests include throat culture and rapid antigen detection testing. Throat culture is considered the diagnostic standard, although the sensitivity and specificity of rapid antigen detection testing have improved significantly. The modified Centor score can be used to help physicians decide which patients need no testing, throat culture/rapid antigen detection testing, or empiric antibiotic therapy. Penicillin (10 days of oral therapy or one injection of intramuscular benzathine penicillin) is the treatment of choice because of cost, narrow spectrum of activity, and effectiveness. Amoxicillin is equally effective and more palatable. Erythromycin and first-generation cephalosporins are options in patients with penicillin allergy. Increased group A beta-hemolytic streptococcus (GABHS) treatment failure with penicillin has been reported. Although current guidelines recommend first-generation cephalosporins for persons with penicillin allergy, some advocate the use of cephalosporins in all nonallergic patients because of better GABHS eradication and effectiveness against chronic GABHS carriage. Chronic GABHS colonization is common despite appropriate use of antibiotic therapy. Chronic carriers are at low risk of transmitting disease or developing invasive GABHS infections, and there is generally no need to treat carriers. Whether tonsillectomy or adenoidectomy decreases the incidence of GABHS pharyngitis is poorly understood. At this time, the benefits are too small to outweigh the associated costs and surgical risks.
Pharyngitis is diagnosed in 11 million patients in U.S. emergency departments and ambulatory settings annually.1 Most episodes are viral. Group A beta-hemolytic streptococcus (GABHS), the most common bacterial etiology, accounts for 15 to 30 percent of cases of acute pharyngitis in children and 5 to 20 percent in adults.2 Among school-aged children, the incidences of acute sore throat, swab-positive GABHS, and serologically confirmed GABHS infection are 33, 13, and eight per 100 child-years, respectively.3 Thus, about one in four children with acute sore throat has serologically confirmed GABHS pharyngitis. Forty-three percent of families with an index case of GABHS pharyngitis have a secondary case.3 Late winter and early spring are peak GABHS seasons. The infection is transmitted via respiratory secretions, and the incubation period is 24 to 72 hours.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Use of clinical decision rules for diagnosing GABHS pharyngitis improves quality of care while reducing unwarranted treatment and overall cost. | A | 5–8, 18, 37, 38 |
| Penicillin is the treatment of choice for GABHS pharyngitis in persons who are not allergic to penicillin. | A | 2, 18–20 |
| Treatment is not typically indicated in chronic carriers of pharyngeal GABHS. | C | 39 |
GABHS = group A beta-hemolytic streptococcus.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Diagnosis of Streptococcal Pharyngitis
CLINICAL DIAGNOSIS
Because the signs and symptoms of GABHS pharyngitis overlap extensively with other infectious causes, making a diagnosis based solely on clinical findings is difficult. In patients with acute febrile respiratory illness, physicians accurately differentiate bacterial from viral infections using only the history and physical findings about one half of the time.4 No single element of the patient’s history or physical examination reliably confirms or excludes GABHS pharyngitis.5 Sore throat, fever with sudden onset (temperature greater than 100.4° F [38° C]), and exposure to Streptococcus within the preceding two weeks suggest GABHS infection. Cervical node lymphadenopathy and pharyngeal or tonsillar inflammation or exudates are common signs. Palatal petechiae and scarlatiniform rash are highly specific but uncommon; a swollen uvula is sometimes noted. Cough, coryza, conjunctivitis, and diarrhea are more common with viral pharyngitis. The diagnostic accuracy of these signs and symptoms is listed in Table 1.5
Table 1. History and Physical Examination Findings Suggesting GABHS Pharyngitis
| Factor | Sensitivity (%) | Specificity (%) | Positive likelihood ratio | Negative likelihood ratio |
|---|---|---|---|---|
| Absence of cough | 51 to 79 | 36 to 68 | 1.1 to 1.7 | 0.53 to 0.89 |
| Anterior cervical nodes swollen or enlarged | 55 to 82 | 34 to 73 | 0.47 to 2.9 | 0.58 to 0.92 |
| Headache | 48 | 50 to 80 | 0.81 to 2.6 | 0.55 to 1.1 |
| Myalgia | 49 | 60 | 1.2 | 0.84 |
| Palatine petechiae | 7 | 95 | 1.4 | 0.98 |
| Pharyngeal exudates | 26 | 88 | 2 | 0.85 |
| Streptococcal exposure in past two weeks | 19 | 91 | 2 | 0.9 |
| Temperature ≥ 100.9° F (38.3° C) | 22 to 58 | 53 to 92 | 0.68 to 3.9 | 0.54 to 1.3 |
| Tonsillar exudates | 36 | 85 | 2.3 | 0.76 |
| Tonsillar or pharyngeal exudates | 45 | 75 | 1.8 | 0.74 |
GABHS = group A beta-hemolytic streptococcus.
Adapted with permission from Ebell MH, Smith MA, Barry HC, Ives K, Carey M. The rational clinical examination. Does this patient have strep throat? JAMA. 2000;284(22):2915.
CLINICAL DECISION RULES
The original Centor score uses four signs and symptoms to estimate the probability of acute streptococcal pharyngitis in adults with a sore throat.6 The score was later modified by adding age and validated in 600 adults and children.7,8 The cumulative score determines the likelihood of streptococcal pharyngitis and the need for antibiotics (Figure 19). Patients with a score of zero or 1 are at very low risk for streptococcal pharyngitis and do not require testing (i.e., throat culture or rapid antigen detection testing [RADT]) or antibiotic therapy. Patients with a score of 2 or 3 should be tested using RADT or throat culture; positive results warrant antibiotic therapy. Patients with a score of 4 or higher are at high risk of streptococcal pharyngitis, and empiric treatment may be considered.
Figure 1. Clinical Decision Rule for Management of Sore Throat
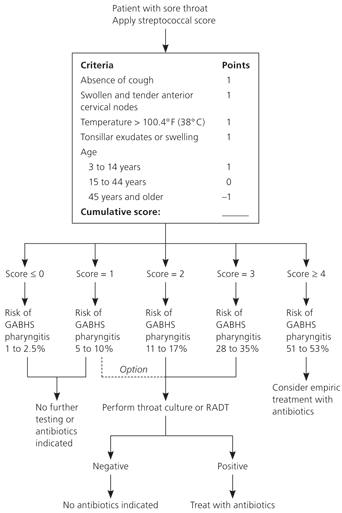
Modified Centor score and management options using clinical decision rule. Other factors should be considered (e.g., a score of 1, but recent family contact with documented streptococcal infection). (GABHS = group A beta-hemolytic streptococcus; RADT = rapid antigen detection testing.)
Adapted with permission from McIsaac WJ, White D, Tannenbaum D, Low DE. A clinical score to reduce unnecessary antibiotic use in patients with sore throat. CMAJ. 1998;158(1):79.
LABORATORY DIAGNOSIS
With correct sampling and plating techniques, a single-swab throat culture is 90 to 95 percent sensitive.10 RADT allows for earlier treatment, symptom improvement, and reduced disease spread. RADT specificity ranges from 90 to 99 percent. Sensitivity depends on the commercial RADT kit used and was approximately 70 percent with older latex agglutination assays.11,12 Newer enzyme-linked immunosorbent assays, optical immunoassays, and chemiluminescent DNA probes are 90 to 99 percent sensitive.11,12 However, newer tests may be more expensive, and not all tests are waived by the Clinical Laboratory Improvement Act of 1988.
Whether negative RADT results in children and adolescents require confirmatory throat culture is controversial. The American Academy of Pediatrics (AAP) recommends that negative RADT results in children be confirmed using throat culture unless physicians can guarantee that RADT sensitivity is similar to that of throat culture in their practice.13 False-negative RADT results may lead to misdiagnosis and GABHS spread and, very rarely, to increased suppurative and nonsuppurative complications. Other studies suggest that the sensitivity of newer optical immunoas-says approaches that of single-plate throat culture, obviating the need for back-up culture.14,15 In many clinical practices, confirmatory throat culture is not performed in children at low risk for GABHS infection. The precipitous drop in rheumatic fever in the United States, significant costs of additional testing and follow-up, and concerns about inappropriate antibiotic use are valid reasons why back-up cultures are not routinely performed.16
Streptococcal antibody titers are not useful for diagnosing streptococcal pharyngitis and are not routinely recommended. They may be indicated to confirm previous infection in persons with suspected acute poststreptococcal glomerulonephritis or rheumatic fever. They may also help distinguish acute infection from chronic carrier status, although they are not routinely recommended for this purpose.
Treatment of GABHS Pharyngitis
JUSTIFICATION FOR TREATMENT
GABHS pharyngitis is self-limited and resolves within a few days, even without treatment.17 Arguments for antibiotic treatment include acute symptom relief, prevention of suppurative and nonsuppurative complications, and reduced communicability (Table 2).2,18–21 Antibiotics shorten symptom duration by about 16 hours; the number needed to treat (NNT) for symptom relief at 72 hours is four in those with positive throat swabs.22 In addition, rates of suppurative peritonsillar and retropharyngeal abscesses are reduced (approximately one in 1,000 cases).23
Table 2. Complications of GABHS Pharyngitis
Antibiotics also reduce the incidence of acute rheumatic fever (relative risk reduction = 0.28).24 Although rheumatic heart disease is a major public health issue in low- and middle-income countries (annual incidence of five per 100,000 persons), it has largely been controlled in industrialized nations since the 1950s.25 It is estimated that 3,000 to 4,000 patients must be given antibiotics to prevent one case of acute rheumatic fever in developed nations.18 Rates of acute rheumatic fever and retropharyngeal abscess have not increased following more judicious antibiotic use in children with respiratory infections.26 Children with GABHS pharyngitis may return to school after 24 hours of antibiotic therapy.27
Non–group A beta-hemolytic streptococci (groups C and G) also can cause acute pharyngitis; these strains are usually treated with antibiotics, although good clinical trials are lacking. Fusobacterium necrophorum causes endemic acute pharyngitis, peritonsillar abscess, and persistent sore throat. Untreated Fusobacterium infections may lead to Lemierre syndrome, an internal jugular vein thrombus caused by inflammation. Complications occur when septic plaques break loose and embolize. Empiric antibiotic therapy may reduce the incidence of complications.
ANTIBIOTIC SELECTION
Effectiveness, spectrum of activity, safety, dosing schedule, cost, and compliance issues all require consideration. Penicillin, penicillin congeners (ampicillin or amoxicillin), clindamycin (Cleocin), and certain cephalosporins and macrolides are effective against GABHS. Based on cost, narrow spectrum of activity, safety, and effectiveness, penicillin is recommended by the American Academy of Family Physicians (AAFP),18 the AAP,19 the American Heart Association,20 the Infectious Diseases Society of America (IDSA),2 and the World Health Organization for the treatment of streptococcal pharyngitis.25 Options for penicillin dosing are listed in Table 3.2,17–20,28–34 When patients are unlikely to complete the entire course of antibiotics, a single intramuscular dose of penicillin G benzathine (Bicillin L-A) is an option. A premixed penicillin G benzathine/procaine injection (Bicillin C-R) lessens injection-associated discomfort. Over the past 50 years, no increase in minimal inhibitory concentration or resistance to GABHS has been documented for penicillins or cephalosporins.28
Oral amoxicillin suspension is often substituted for penicillin because it tastes better. The medication is also available as chewable tablets. Five of eight trials (1966 to 2000) showed greater than 85 percent GABHS eradication with the use of amoxicillin.29 [ corrected] Ten days of therapy is standard; common dosages are provided in Table 3.2,17–20,28–34 Amoxicillin taken once per day is likely as effective as a regimen of three times per day. One randomized controlled trial (RCT) demonstrated comparable symptom relief with once-daily dosing, although like almost all studies of pharyngitis treatment, the trial was not powered to detect nonsuppurative complications.30 A recent study of children three to 18 years of age showed that once-daily dosing of amoxicillin was not inferior to twice-daily dosing; both regimens had failure rates of about 20 percent.31 It should be noted that once-daily therapy is not approved by the U.S. Food and Drug Administration (FDA).
Table 3. Antibiotic Options for GABHS Pharyngitis
| Drug | Class of antimicrobial | Route of administration | Dosage | Duration of therapy | Cost* | ||
|---|---|---|---|---|---|---|---|
| Primary treatment (recommended by current guidelines) | |||||||
| Penicillin V (Veetids; brand no longer available in the United States) | Penicillin | Oral | Children: 250 mg two to three times per day | 10 days | $4 | ||
| Adolescents and adults: 250 mg three to four times per day | |||||||
| or | |||||||
| 500 mg two times per day | |||||||
| Amoxicillin | Penicillin (broad spectrum) | Oral | Children (mild to moderate GABHS pharyngitis): | 10 days | $4 | ||
| 12.25 mg per kg two times per day | |||||||
| or | |||||||
| 10 mg per kg three times per day | |||||||
| Children (severe GABHS pharyngitis): 22.5 mg per kg two times per day | |||||||
| or | |||||||
| 13.3 mg per kg three times per day | |||||||
| or | |||||||
| 750 mg (not FDA approved) once per day† | |||||||
| Adults (mild to moderate GABHS pharyngitis): | |||||||
| 250 mg three times per day | |||||||
| or | |||||||
| 500 mg two times per day | |||||||
| Adults (severe GABHS pharyngitis): 875 mg two times per day | |||||||
| Penicillin G benzathine (Bicillin L-A) | Penicillin | Intramuscular | Children: < 60 lb (27 kg): 6.0 × 105 units | One dose | Varies | ||
| Adults: 1.2 × 106 units | |||||||
| Treatment for patients with penicillin allergy (recommended by current guidelines) | |||||||
| Erythromycin ethylsuccinate | Macrolide | Oral | Children: 30 to 50 mg per kg per day in two to four divided doses | 10 days | $4 | ||
| Adults: 400 mg four times per day or 800 mg two times per day | |||||||
| Erythromycin estolate | Macrolide | Oral | Children: 20 to 40 mg per kg per day in two to four divided doses | 10 days | $4 | ||
| Adults: not recommended‡ | |||||||
| Cefadroxil (Duricef; brand no longer available in the United States) | Cephalosporin (first generation) | Oral | Children: 30 mg per kg per day in two divided doses | 10 days | $45 | ||
| Adults: 1 g one to two times per day | |||||||
| Cephalexin (Keflex) | Cephalosporin (first generation) | Oral | Children: 25 to 50 mg per kg per day in two to four divided doses | 10 days | $4 | ||
| Adults: 500 mg two times per day | |||||||
note: The following medications are FDA approved, but are not recommended by guidelines for primary GABHS therapy: azithromycin (Zithromax), clarithromycin (Biaxin), cefprozil (Cefzil; second-generation cephalosporin), cefpodoxime (Vantin; third-generation cephalosporin), ceftibuten (Cedax; third-generation cephalosporin), and cefdinir (Omnicef; third-generation cephalosporin).
FDA = U.S. Food and Drug Administration; GABHS = group A beta-hemolytic streptococcus.
*— Average price of generic based on http://www.pharmacychecker.com.
†— Children four to 18 years of age.
‡— Adults receiving erythromycin estolate may develop cholestatic hepatitis; the incidence is higher in pregnant women, in whom the drug is contraindicated.
Information from references 2, 17 through 20, and 28 through 34.
Current U.S. treatment guidelines recommend erythromycin for patients with penicillin allergy. Gastrointestinal side effects of erythromycin cause many physicians to instead prescribe the FDA-approved second-generation macrolides azithromycin (Zithromax) and clarithromycin (Biaxin). Azithromycin reaches higher concentrations in pharyngeal tissue and requires only five days of treatment. Macrolide resistance is increasing among GABHS isolates in the United States, likely because of azithromycin overuse.32 Reported GABHS resistance in certain areas of the United States and Canada approaches 8 to 9 percent.33 Most guidelines recommend reserving erythromycin for patients who are allergic to penicillin.
First-generation oral cephalosporins are recommended for patients with penicillin allergy who do not have immediate-type hypersensitivity to betalactam antibiotics. Bacteriologic failure rates for penicillin-treated GABHS pharyngitis increased from about 10 percent in the 1970s to more than 30 percent in the past decade.29 Several studies suggest that cephalosporins are more effective against GABHS than penicillin. Higher rates of GABHS eradication and shorter courses of therapy that are possible with cephalosporins may be beneficial. One meta-analysis of 35 trials comparing various cephalosporins against penicillin noted significantly more bacteriologic and clinical cures in the cephalosporin group (NNT = 13).34 However, the poor quality of included studies limited these findings, and results may be skewed because cephalosporins more effectively eradicate GABHS carriage than penicillin does. Although cephalosporins are effective, the shift toward expensive, broad-spectrum second- and third-generation cephalosporin use is increasing. Whether cephalosporins will replace penicillin as primary GABHS therapy remains to be seen.
Guidelines for Treatment
Although GABHS pharyngitis is common, the ideal approach to management remains a matter of debate. Numerous practice guidelines, clinical trials, and cost analyses give divergent opinions. U.S. guidelines differ in whether they recommend using clinical prediction models versus diagnostic testing (Table 4). Several international guidelines recommend not testing for or treating GABHS pharyngitis at all.35
Table 4. Comparison of GABHS Guidelines
| Recommendation | ACP (endorsed by the CDC and AAFP) | AAP | IDSA | UKNHS |
|---|---|---|---|---|
| Screening for acute pharyngitis | Use Centor criteria (see Figure 1) | Use clinical and epidemiologic findings to assess patient’s risk of GABHS (e.g., sudden onset of sore throat, fever, odynophagia, tonsillar erythema, exudates, cervical lymphadenitis, or history of streptococcal exposure) | History and physical examination to establish risk | |
| Diagnostic testing | RADT with Centor score of 2 or 3 only | RADT or throat culture in all patients at risk | None | |
| Back-up culture needed if RADT result negative? | Adults: No | Adults: NA | Adults: No | — |
| Children: Yes | Children: Yes | Children: Yes | ||
| Who requires antibiotic treatment? | Empiric antibiotics for Centor score of 3 or 4; treat patients with positive RADT result | Positive RADT result or throat culture | Only high-risk and very ill patients | |
| Antibiotic of choice | Oral penicillin V (Veetids; brand no longer available in the United States); intramuscular penicillin G benzathine (Bicillin L-A); oral amoxicillin with equal effectiveness and better palatability in children | Oral penicillin V | ||
| Penicillin allergy | Oral erythromycin; cephalosporin (first generation) | Oral erythromycin | ||
AAFP = American Academy of Family Physicians; AAP = American Academy of Pediatrics; ACP = American College of Physicians; CDC = Centers for Disease Control and Prevention; GABHS = group A beta-hemolytic streptococcus; IDSA = Infectious Diseases Society of America; NA = not applicable; RADT = rapid antigen detection testing; UKNHS = United Kingdom National Health Service.
The AAFP, the American College of Physicians (ACP), and the Centers for Disease Control and Prevention recommend using a clinical prediction model to manage suspected GABHS pharyngitis.18 Guidelines from the IDSA, conversely, state that clinical diagnosis of GABHS pharyngitis cannot be made with certainty, even by experienced physicians, and that diagnostic testing is required.2 Whereas the Centor algorithm effectively identifies low-risk patients in whom testing is unnecessary, the IDSA is concerned about its relatively low positive predictive value with higher scores (approximately 50 percent) and the risk of overtreatment.36 The ACP guidelines attempt to prevent inappropriate antibiotic use while avoiding unnecessary testing. Differences in guidelines are best explained by whether emphasis is placed on avoiding inappropriate antibiotic use or on relieving acute GABHS pharyngitis symptoms. Several U.S. guidelines recommend confirmatory throat culture for negative RADT in children and adolescents.2,18,19 This approach is 100 percent sensitive and 99 to 100 percent specific for diagnosing GABHS pharyngitis in children.37 However, because of improved RADT sensitivity, the IDSA and ACP recently omitted this recommendation for adults. A similar recommendation to omit confirmatory throat culture after negative RADT is likely for children.
Management of Recurrent GABHS Pharyngitis
RADT is effective for diagnosing recurrent GABHS infection. In patients treated within the preceding 28 days, RADT has similar specificity and higher sensitivity than in patients without previous streptococcal infection (0.91 versus 0.70, respectively; P < .001).38 Recurrence of GABHS pharyngitis within one month may be treated using the antibiotics listed in Table 3.2,17–20,28–34 Intramuscular penicillin G injection is an option when oral antibiotics were initially prescribed.
Chronic Pharyngeal Carriage
Chronic pharyngeal carriage is the persistent presence of pharyngeal GABHS without active infection or immune/inflammatory response. Patients may carry GABHS for one year despite treatment. Chronic carriers are at little to no risk of immune-mediated post-streptococcal complications because no active immune response occurs.39 Risk of GABHS transmission is very low and is not linked to invasive group A streptococcal (GAS) infections. Unproven therapies such as long-term antibiotic use, treatment of pets, and exclusion from school and other activities have proved ineffective and are best avoided.39 Carriage of one GABHS serotype does not preclude infection by another; therefore, throat culture or RADT is appropriate when GABHS pharyngitis is suspected. Testing is unnecessary if clinical symptoms suggest viral upper respiratory infection.
Antibiotic treatment may be appropriate in the following persons or situations: recurrent GABHS infection within a family; personal history of or close contact with someone who has had acute rheumatic fever or acute poststreptococcal glomerulonephritis; close contact with someone who has GAS infection; community outbreak of acute rheumatic fever, poststreptococcal glomerulonephritis, or invasive GAS infection; health care workers or patients in hospitals, chronic care facilities, or nursing homes; families who cannot be reassured; and children at risk of tonsillectomy for repeated GABHS pharyngitis.39 Small RCTs suggest that intramuscular benzathine penicillin combined with four days of oral rifampin (Rifadin) or a 10-day course of oral clindamycin effectively eradicates the carrier state.39 Oral clindamycin, azithromycin, and cephalosporins are also effective.
Tonsillectomy
The effect of tonsillectomy on decreasing risk for chronic or recurrent throat infection is poorly understood. One trial in children showed that the frequency of recurrent throat infection decreased in the tonsillectomy/adenoidectomy and control groups.40 The surgical group had one fewer episode of severe GABHS pharyngitis annually; the authors concluded that this small potential benefit did not justify the risks or cost of surgery. A meta-analysis of children and adults with chronic pharyngitis comparing tonsillectomy with nonsurgical treatment was inconclusive.41 Another retrospective study based on data from the Rochester Epidemiology Project found that children with tonsils are three times more likely to develop subsequent GABHS pharyngitis than those who had undergone tonsillectomies (odds ratio = 3.1; P < .001).42

