Excessive daytime sleepiness is one of the most common sleep-related patient symptoms, and it affects an estimated 20 percent of the population. Persons with excessive daytime sleepiness are at risk of motor vehicle and work-related incidents, and have poorer health than comparable adults. The most common causes of excessive daytime sleepiness are sleep deprivation, obstructive sleep apnea, and sedating medications. Other potential causes of excessive daytime sleepiness include certain medical and psychiatric conditions and sleep disorders, such as narcolepsy. Obstructive sleep apnea is a particularly significant cause of excessive daytime sleepiness. An estimated 26 to 32 percent of adults are at risk of or have obstructive sleep apnea, and the prevalence is expected to increase. The evaluation and management of excessive daytime sleepiness is based on the identification and treatment of underlying conditions (particularly obstructive sleep apnea), and the appropriate use of activating medications.
About 20 percent of adults in the United States report a level of daytime sleepiness sufficient to interfere with daily activities, and excessive daytime sleepiness is the leading symptom of patients presenting to sleep clinics.1 The prevalence of excessive daytime sleepiness is highest in adolescents, older persons, and shift workers,2 but assessment of its true prevalence is difficult because of the subjective nature of the symptoms, inconsistencies in terminology, and a lack of consensus on methods of diagnosis and assessment. Some persons use subjective terminology (e.g., drowsiness, languor, inertness, fatigue, sluggishness) when describing symptoms of excessive daytime sleepiness.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Treatment of OSA with CPAP therapy leads to a decline in daytime sleepiness and a lower risk for motor vehicle incidents. | B | 29, 31, 35 |
| Modafinil (Provigil) improves symptoms of persistent sleepiness in patients with OSA who are already being treated with CPAP. It also improves daytime sleepiness in patients with shift work disorder. | B | 34, 36 |
CPAP = continuous positive airway pressure; OSA = obstructive sleep apnea.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Excessive daytime sleepiness can have diverse and serious consequences. Sleep problems contribute to more than 100,000 motor vehicle incidents that result in 71,000 personal injuries and 1,500 deaths annually.4 According to the National Transportation Safety Board, up to 52 percent of single vehicle crashes involving heavy trucks are fatigue-related, with the driver falling asleep in 17.6 percent of cases.5 Most sleep-related crashes involve adolescent and young adult male drivers.6 Sleepy adolescents also have significantly lower levels of academic performance, increased school tardiness, and lower graduation rates than other students.7 Daytime sleepiness has been linked to poor health on several standardized measurements, including impairment in all domains of the Medical Outcomes Study short form health survey (36 items).8 It has also been associated with compromised professional performance, including that of physicians and judges.9,10 Reduced cognitive function related to excessive daytime sleepiness can affect the ability to gain or maintain employment, because patients with excessive daytime sleepiness may be misperceived as lazy or unmotivated.
Causes of Excessive Daytime Sleepiness
Excessive daytime sleepiness can occur secondary to sleep deprivation, medication effects, illicit substance use, obstructive sleep apnea (OSA), and other medical and psychiatric conditions (Table 1).11 Excessive sleepiness caused by a primary hypersomnia of central origin (e.g., narcolepsy, idiopathic hypersomnia) is less common.
Table 1. Common Causes of Excessive Daytime Sleepiness
| Cause | Comments | |
|---|---|---|
| Primary hypersomnias of central origin | ||
| Narcolepsy | 0.02 to 0.18 percent of population | |
| Idiopathic hypersomnia | 10 percent of patients with suspected narcolepsy | |
| Other rare primary hypersomnias | Example: Kleine-Levin syndrome | |
| Secondary hypersomnias | ||
| Sleep disorders | ||
| Sleep-related breathing disorders | Excessive daytime sleepiness secondary to obstructive sleep apnea (general population prevalence is 2 percent of women and 4 percent of men) | |
| Behavioral sleep deprivation | Especially common in adolescents and shift workers | |
| Other sleep disorders | Includes circadian rhythm sleep disorders, sleep-related movement disorders | |
| Medical or psychiatric conditions | ||
| Medication effects | Includes prescription, nonprescription, and drugs of abuse | |
| Psychiatric conditions | Especially depression | |
| Medical conditions | Includes head trauma, stroke, cancer, inflammatory conditions, encephalitis, neurodegenerative conditions | |
note: Hypersomnia due to secondary causes is much more common than primary hypersomnia.
Information from reference 11.
SLEEP DEPRIVATION
Sleep deprivation is probably the most common cause of excessive daytime sleepiness. Symptoms can occur in healthy persons after even mild sleep restriction. Studies that restricted healthy adults to six hours of sleep per night for 14 successive nights showed a cumulative significant impairment of neurobiological functions.12 Symptoms of sleep deprivation can occur after only one night of sleep loss,12 and persons who are chronically sleep deprived are often unaware of their increasing cognitive and performance deficits.8 Paradoxically, most types of chronic insomnia (including primary insomnia, psychopathological insomnia, and paradoxical insomnia) are associated with daytime hyperarousal rather than excessive daytime sleepiness. The presence of excessive daytime sleepiness in a patient with insomnia suggests a comorbidity such as a sleep-related breathing disorder or a mood disorder.13
MEDICATION AND DRUG EFFECTS
Sleepiness is the most commonly reported side effect of pharmacologic agents that act on the central nervous system. The modulation of sleep and wakefulness is a complex process involving multiple factors and systems. Although no single chemical neurotransmitter has been identified as necessary or sufficient in the control of sleep, most drugs with clinical sedative or hypnotic actions affect one or more of the central neurotransmitters implicated in the neuromodulation of sleep and wakefulness, including dopamine, epinephrine, norepinephrine, acetylcholine, serotonin, histamine, glutamate, γ-aminobutyric acid, and adenosine (Table 2).14
Table 2. Medication Classes Commonly Associated with Daytime Sleepiness
| Alpha-adrenergic blocking agents |
| Anticonvulsants (e.g., hydantoins, succinimides) |
| Antidepressants (monoamine oxidase inhibitors, tricyclics, selective serotonin reuptake inhibitors) |
| Antidiarrhea agents |
| Antiemetics |
| Antihistamines |
| Antimuscarinics and antispasmodics |
| Antiparkinsonian agents |
| Antipsychotics |
| Antitussives |
| Barbiturates |
| Benzodiazepines, other γ-aminobutyric acid affecting agents, and other anxiolytics |
| Beta-adrenergic blocking agents |
| Genitourinary smooth muscle relaxants |
| Opiate agonists and partial opiate agonists |
| Skeletal muscle relaxants |
Information from reference 14.
Ethanol is the most widely used agent with sedative effects.15 Nonprescription sleeping pills and other medications containing sedating H1 antihistamines, such as diphenhydramine (Benadryl), hydroxyzine (Atarax, brand no longer available in the United States), or triprolidine (Zymine) are also commonly used. Sedating antihistamines, longer-acting benzodiazepines, and sedating antidepressants are associated with decreased performance on driving tests and increased rates of next-day motor vehicle incidents attributed to daytime sleepiness.13,15,16 Of the antihypertensive medications in widespread use, tiredness, fatigue, and daytime sleepiness are side effects commonly associated with beta blockers such as propranolol (Inderal), but sedation is also the most common side effect reported for the alpha2-agonists clonidine (Catapres) and methyldopa (Aldomet, brand no longer available in the United States). Sedation is also commonly reported by patients taking anticonvulsant or antipsychotic medications. Among drugs of abuse, marijuana has significant sedating effects. Adolescents abusing stimulants such as amphetamines and cocaine may experience persistent daytime sedation after long episodes of drug-induced wakefulness.
OSA
Excessive daytime sleepiness is the most common symptom of OSA. A sleep disorder caused by blockage of the upper airway, OSA results in episodes of cessation of breathing (apneas) or a reduction in airflow (hypopneas), and is defined as greater than or equal to five apneic or hypopneic episodes per hour of sleep. These events induce recurrent hypoxia and repetitive arousals from sleep. For adults 30 to 60 years of age, the prevalence of OSA has been estimated to be 9 percent for women and 24 percent for men. In patients with OSA, approximately 23 percent of women and 16 percent of men experience excessive daytime sleepiness.17 Sleep-related breathing disorders may be significantly under-recognized as causes of excessive daytime sleepiness. One study estimated that 93 percent of women and 82 percent of men with moderate to severe OSA are undiagnosed.18 Furthermore, 26 to 32 percent of U.S. adults are at risk of developing or currently have OSA. Because increasing age and obesity are significant risk factors for OSA, the prevalence of OSA is set to increase rapidly.19
Persons with OSA have an increased risk of motor vehicle incidents because of their impaired vigilance.18 In 2000, more than 800,000 drivers in the United States were involved in OSA-related motor vehicle collisions, resulting in 1,400 deaths.20 Approximately 25 percent of persons with untreated OSA report frequently falling asleep while driving.21 Because of associated daytime sleepiness, reduced vigilance, and inattention, persons with OSA may have work performance difficulties and are at a high risk of being involved in occupational incidents.22
OTHER SECONDARY HYPERSOMNIAS
Many medical conditions can cause secondary excessive daytime sleepiness, including head trauma, stroke, tumors, inflammatory conditions, encephalitis, and genetic and neurodegenerative diseases. Psychiatric conditions, especially depression, can also result in excessive daytime sleepiness. Sleep disorders such as circadian rhythm disorders (e.g., jet lag, shift work disorder), periodic limb movement disorder, and restless legs syndrome can also contribute to significant levels of daytime sleepiness in some persons.
PRIMARY HYPERSOMNIAS
Narcolepsy, the most common of the primary hypersomnias, is reported to affect 0.02 to 0.18 percent of the adult population, but may be significantly underdiagnosed. Approximately 25 to 30 percent of patients with narcolepsy have associated cataplexy (i.e., sudden and transient loss of muscle tone associated with emotions).23 Less common are the other primary hypersomnias of central origin, including idiopathic hypersomnia, menstrual hypersomnia, and Kleine-Levin syndrome (a rare form of recurrent hypersomnia most common in male adolescents).11
Evaluating and Screening for Excessive Daytime Sleepiness
Although some patients present with the symptom of daytime sleepiness, most are far sleepier than they realize. Questionnaires such as the Stanford Sleepiness Scale and the Epworth Sleepiness Scale (Figure 124) are validated, patient-completed assessments of daytime sleepiness that can be used as screening tests. A test score in excess of 12 on the Epworth Sleepiness Scale or a patient history of falling asleep while driving are clear indications that further evaluation and work-up are required.
Figure 1. Patient Health Questionnaire: Excessive Daytime Sleepiness

Patient questionnaire for rating excessive daytime sleepiness using the Epworth Sleepiness Scale.
Adapted with permission from the American Academy of Sleep Medicine, and Johns MW. A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep. 1991;14(6):541.
A targeted medical history, physical examination, and laboratory assessment should be used to evaluate patients at risk of medical or psychological causes of secondary excessive daytime sleepiness. The medication history must address use of all prescription and nonprescription medications, and drugs of abuse. Sometimes treatment of excessive daytime sleepiness can be as simple as discontinuing or modifying the use of such agents. Information about sleep patterns should identify behavioral sleep deprivation. This is most common in adolescents and shift workers, and it can result in significant excessive daytime sleepiness if not addressed.
Information about sleep patterns from the patient and his or her bed partner, if applicable, may indicate restless legs syndrome or OSA, the latter of which may occur even in persons who are not obese or who do not have the common comorbidities of hypertension, diabetes, and coronary disease. In most cases, overnight polysomnography is required to confirm the diagnosis of OSA and to determine the appropriate pressure levels for treatment using continuous positive airway pressure (CPAP) or a similar system.25 Recently, the Centers for Medicare and Medicaid Services have developed protocols that can be utilized by certified sleep physicians for diagnosing OSA with respiratory screening instruments in patients with a high probability of OSA (Table 3). 26 If OSA is not confirmed by polysomnography in a patient who has significant excessive daytime sleepiness, or if sleepiness persists in a patient with OSA despite appropriate therapy, further investigation is required to quantify the level of daytime sleepiness and evaluate for the potential diagnosis of narcolepsy (Figure 2).
Table 3. 2008 Changes in CMS Regulations for OSA Home Sleep Testing and CPAP Treatment
| OSA diagnosis is based on an AHI > 15 or an AHI > 5 to 15 associated with daytime sleepiness, impaired cognition, mood disorders, or insomnia, or documented hypertension, ischemic heart disease, or history of smoking |
| AHI is based on standard polysomnography or home sleep testing |
| Home sleep testing must only be performed by a physician with board certification in sleep medicine or a physician who is an active staff member of a sleep laboratory or clinic accredited by the American Academy of Sleep Medicine or the Joint Commission |
| CPAP is initially limited to a 12-week period, with coverage extended for persons whose symptoms improve based on follow-up physician re-evaluation and with objective evidence of CPAP utilization |
note: Regional variation may exist in CMS policies for home sleep testing.
AHI = apnea-hypopnea index; CMS = Centers for Medicare and Medicaid Services; CPAP = continuous positive airway pressure; OSA = obstructive sleep apnea.
Information from reference 26.
Figure 2. Diagnosis and Management of Conditions That Cause Excessive Daytime Sleepiness
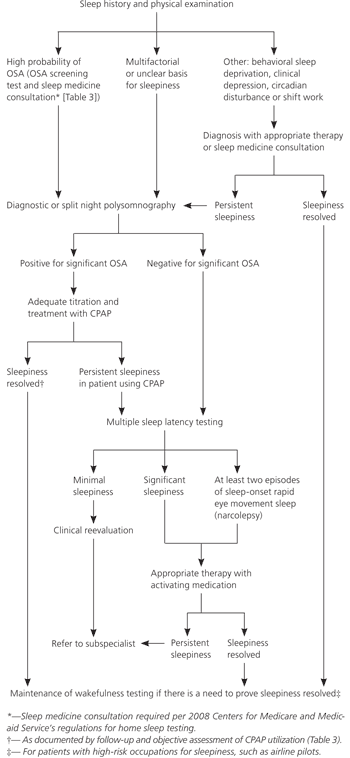
Algorithm for the diagnosis and treatment of conditions that cause excessive daytime sleepiness. (CPAP = continuous positive airway pressure; OSA = obstructive sleep apnea.)
Quantifying Excessive Daytime Sleepiness
Subjective assessment of symptoms using questionnaires and clinical assessment of behavioral impact may not accurately reflect the degree of physiologic sleepiness.27 The effects of sleepiness on daytime performance can be assessed by tests of complex reaction time and coordination, or by tests that assess complex behavioral tasks likely to be affected by sleepiness (e.g., driving performance).28 Performance measures are susceptible to influences that are not task related (e.g., motivation, distraction, comprehension of instructions); therefore, the results of performance tests and questionnaires do not always correlate.3
The most common tests for assessing psychological variations in daytime sleepiness are the Multiple Sleep Latency Test (MSLT) and the Maintenance of Wakefulness Test (MWT). Both of these tests use modified polysomnography to assess sleep onset latency (i.e., the amount of time it takes to fall asleep) during a series of waking nap periods. Overnight polysomnography is required before the MSLT or MWT to assess the disordered sleep pattern and test for significant OSA. To diagnose narcolepsy without cataplexy, the MSLT must demonstrate hypersomnolence and early onset of rapid eye movement sleep. The MWT can be used to assess improvements in waking performance after treatment in persons with excessive daytime sleepiness who could potentially be dangerous to self and others, such as commercial drivers and airplane pilots.29
Treating Excessive Daytime Sleepiness
Addressing the underlying cause is the mainstay of treatment of excessive daytime sleepiness. In OSA—the most dangerous and physiologically disruptive cause of excessive daytime sleepiness—treatment with positive pressure devices (e.g., CPAP) during sleep improves symptoms of daytime sleepiness for most patients.30 The effects of other treatments for OSA (e.g., medications, dental appliances, surgery) on daytime sleepiness have not been well documented.31–33
Modafinil (Provigil) is considered to be the first-line activating agent for the treatment of excessive daytime sleepiness. It is indicated for the treatment of persistent sleepiness associated with OSA in patients already being treated with CPAP, and for the treatment of daytime sleepiness in patients with shift work disorder.34–36 Modafinil is pharmacologically distinct from and has a much lower potential for abuse (Schedule IV) than the amphetamines, and has a generally benign side-effect profile. Other medications that must be used with caution to induce alertness in somnolent patients include the amphetamines (dextroamphetamine [Dexedrine], methylphenidate [Ritalin]) and pemoline (Cylert, not available in the United States). The amphetamines are Schedule II prescription drugs and are considered to have a high potential for abuse. Side effects of amphetamines include personality changes, tremor, hypertension, headaches, and gastroesophageal reflux.37 Pemoline can cause hepatic toxicity in susceptible patients. The use of activating agents is inappropriate in hypersomnolent patients with untreated OSA—although daytime sleepiness may be improved with these agents, the patient remains at risk from the pathophysiologic consequences of untreated OSA.
Medical and Legal Considerations
Legal requirements for reporting excessive daytime sleepiness that may impair driving vary from state to state.38 The physician treating patients with excessive daytime sleepiness (or patients using drugs likely to affect driving performance) has the responsibility to make a clinical assessment of the patient’s overall risk of unsafe driving, and to document driving recommendations and precautions. A physician should report patients who fail to comply with treatment, particularly high-risk persons such as airline pilots, truck, bus, and occupational drivers, and those with a history of recent sleepiness-associated incidents.

