Coronary heart disease is the most common cause of death in the United States. The conventional risk factor approach to primary prevention excludes many patients who could benefit from preventive therapies. A global risk approach allows more accurate estimates of risk to guide clinical primary prevention efforts. Global risk of coronary heart disease is a calculation of the absolute risk of having a coronary heart disease event (e.g., death, myocardial infarction) over a specified period. It is based on an empiric equation that combines major risk factors, such as blood pressure and cholesterol levels. When physicians know a patient’s global risk of coronary heart disease, they are more likely to prescribe risk-reducing therapies such as antihypertensives, statins, and aspirin. In addition, patients who know their risk level are more likely to initiate risk-reducing therapies. Many tools are available to estimate global risk, including several Web-based calculators. In the United States, tools based on the Framingham Heart Study are recommended.
Coronary heart disease (CHD), the leading cause of mortality in the United States, is responsible for one out of every five deaths.1 Treatment of cardiovascular risk factors has resulted in a 50 percent decrease in deaths from CHD over the past 30 years.2 However, less than two thirds of persons at increased risk of cardiovascular disease are using therapies that have been proven to reduce the risk of initial events.3–6 Thus, improving delivery and uptake of primary clinical prevention strategies is an important public health priority. One approach is to use global CHD risk to help guide discussions and decisions with patients. This article discusses the rationale behind global CHD risk and how it can be used when considering preventive care. Patients with established CHD (i.e., those who have had a CHD-related event) are in the highest risk group, and these calculations do not apply to them; such patients should receive aggressive medical treatment regardless of their risk factor levels.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should calculate the global risk of coronary heart disease when considering pharmacologic interventions for primary prevention. | C | 9, 20, 21 |
| A Framingham-based risk calculator is preferred for most U.S. populations. | C | 29 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Global CHD risk is the absolute risk of a CHD-related event over a specific period, usually 10 years. The event can be “hard” (e.g., myocardial infarction [MI], sudden cardiac death) or “soft” (e.g., chest pain). The risk estimate is based on major risk factors and is calculated using an empiric equation (Figures 1 and 2).7 In contrast, the conventional clinical approach to primary prevention of cardiovascular disease relies on identification and treatment of individual risk factors, such as hypertension and hyper-lipidemia.8,9 However, this approach does not account for the fact that major cardiovascular risk factors (Table 18–16 ) contribute multiplicatively to overall CHD risk. In addition, physicians tend to observe rather than treat small elevations in risk factors.17,18
Figure 1. Calculating Global CHD Risk in Men
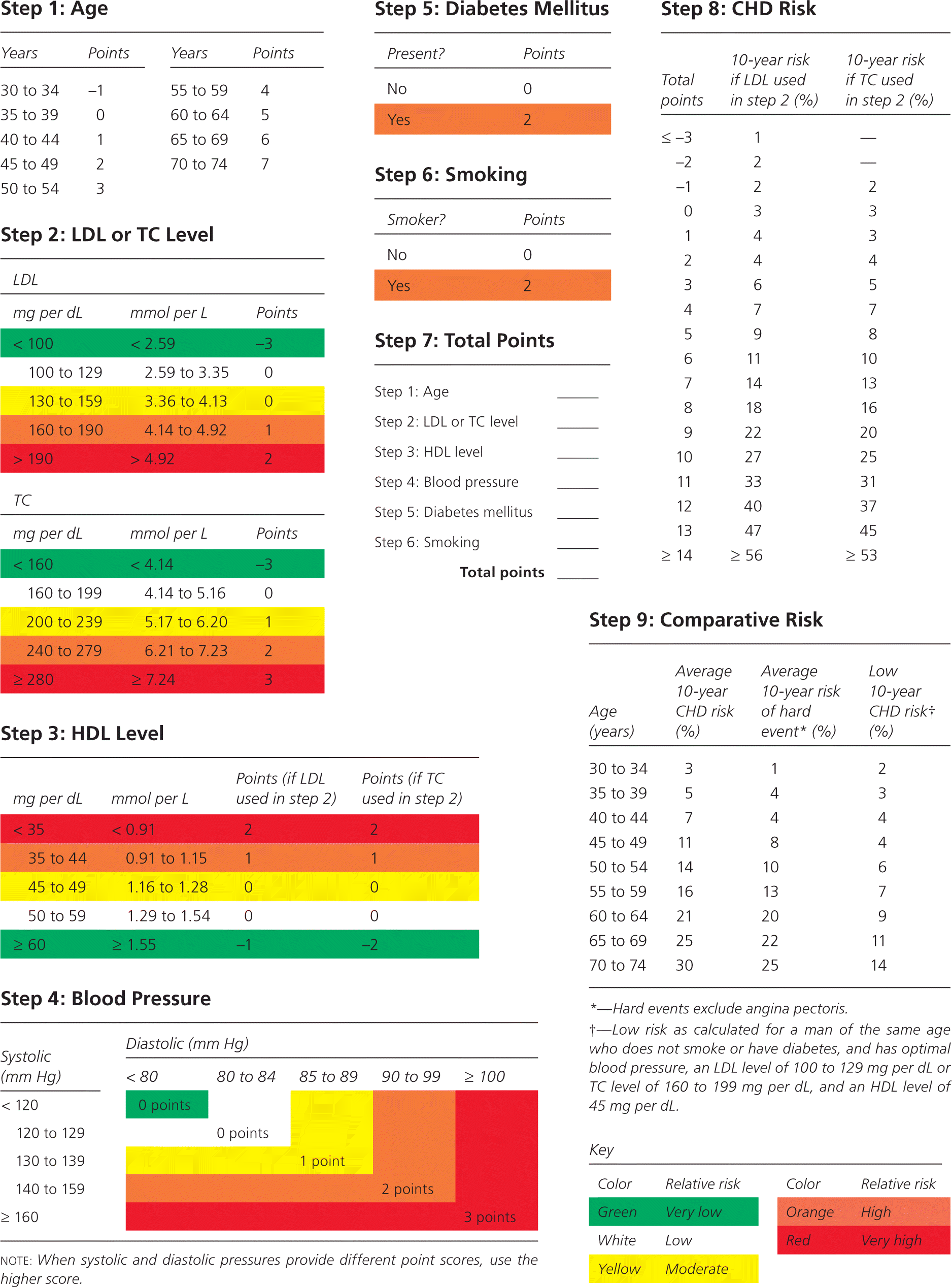
Charts for estimation of coronary heart disease (CHD) risk in men. (HDL = high-density lipoprotein; LDL = low-density lipoprotein; TC = total cholesterol.)
Adapted with permission from Wilson PW, D’Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. Prediction of coronary heart disease using risk factor categories. Circulation. 1998;97(18):1843.
Figure 2. Calculating Global CHD Risk in Women
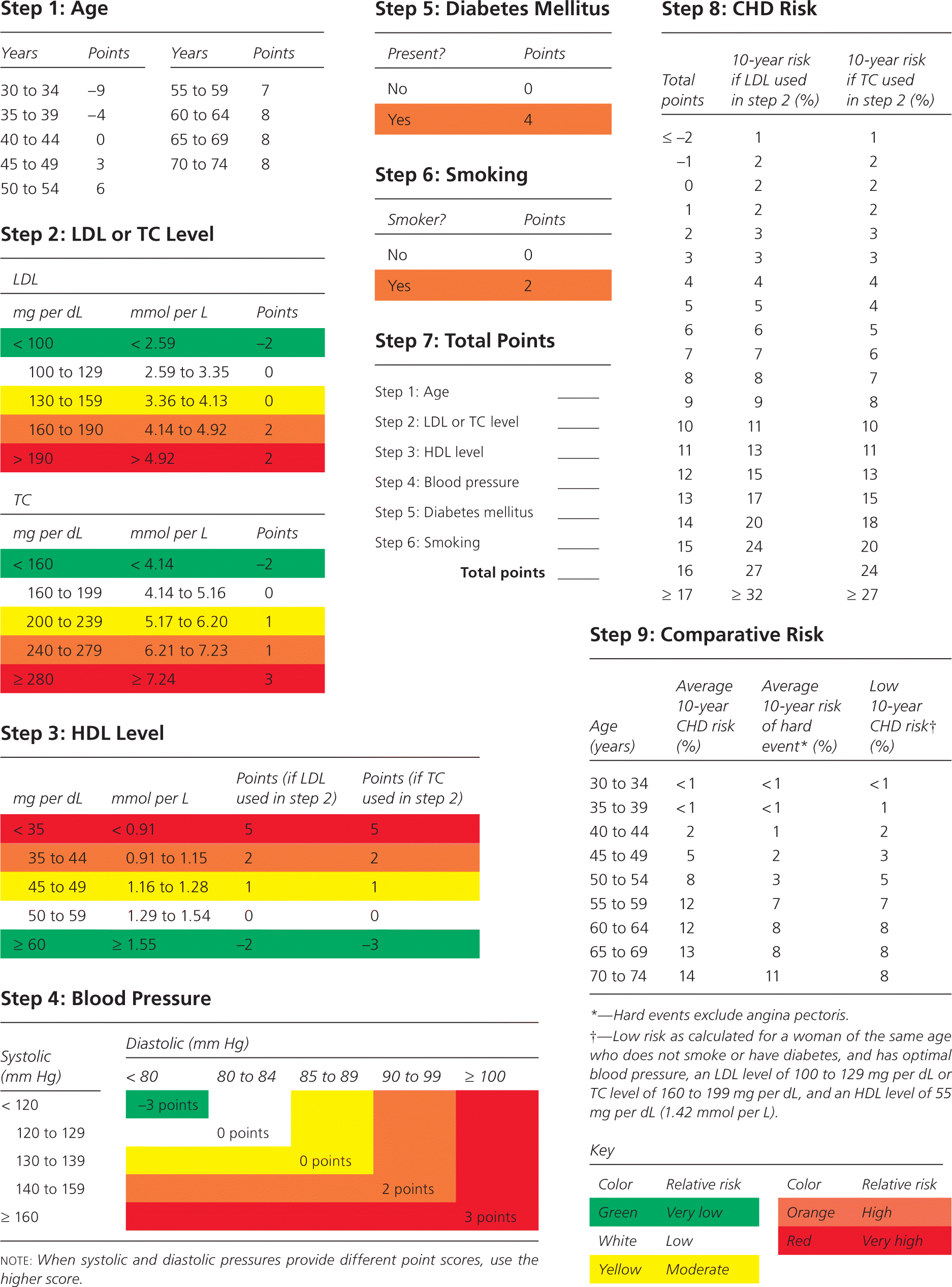
Charts for estimation of coronary heart disease (CHD) risk in women. (HDL = high-density lipoprotein; LDL = low-density lipoprotein; TC = total cholesterol.)
Adapted with permission from Wilson PW, D’Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. Prediction of coronary heart disease using risk factor categories. Circulation. 1998;97(18):1844.
Table 1. Major Risk Factors and Interventions for CHD
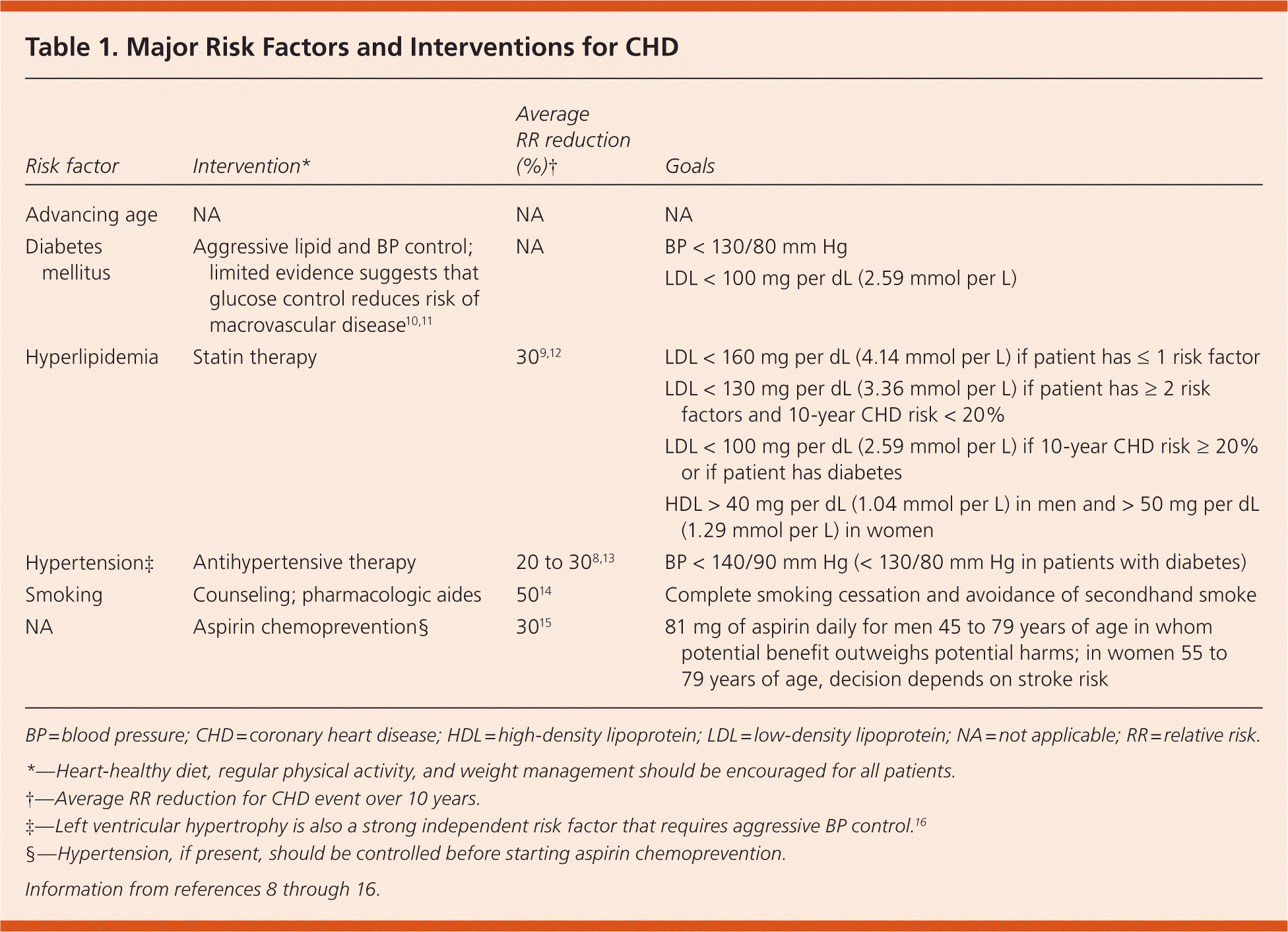
| Risk factor | Intervention* | Average RR reduction (%)† | Goals |
|---|---|---|---|
| Advancing age | NA | NA | NA |
| Diabetes mellitus | Aggressive lipid and BP control; limited evidence suggests that glucose control reduces risk of macrovascular disease10,11 | NA | BP < 130/80 mm Hg LDL < 100 mg per dL (2.59 mmol per L) |
| Hyperlipidemia | Statin therapy | 309,12 | LDL < 160 mg per dL (4.14 mmol per L) if patient has ≤ 1 risk factor |
| LDL < 130 mg per dL (3.36 mmol per L) if patient has ≥ 2 risk factors and 10-year CHD risk < 20% | |||
| LDL < 100 mg per dL (2.59 mmol per L) if 10-year CHD risk ≥ 20% or if patient has diabetes | |||
| HDL > 40 mg per dL (1.04 mmol per L) in men and > 50 mg per dL (1.29 mmol per L) in women | |||
| Hypertension‡ | Antihypertensive therapy | 20 to 308,13 | BP < 140/90 mm Hg (< 130/80 mm Hg in patients with diabetes) |
| Smoking | Counseling; pharmacologic aides | 5014 | Complete smoking cessation and avoidance of secondhand smoke |
| NA | Aspirin chemoprevention§ | 3015 | 81 mg of aspirin daily for men 45 to 79 years of age in whom potential benefit outweighs potential harms; in women 55 to 79 years of age, decision depends on stroke risk |
BP = blood pressure; CHD = coronary heart disease; HDL = high-density lipoprotein; LDL = low-density lipoprotein; NA = not applicable; RR = relative risk.
*— Heart-healthy diet, regular physical activity, and weight management should be encouraged for all patients.
†— Average RR reduction for CHD event over 10 years.
‡— Left ventricular hypertrophy is also a strong independent risk factor that requires aggressive BP control.16
§— Hypertension, if present, should be controlled before starting aspirin chemoprevention.
Preventive pharmacotherapy should take the patient’s absolute risk—not just risk factors—into consideration. In an individual risk factor approach, a patient with modest levels of a few risk factors may have a moderate or high overall risk of a CHD-related event, yet not be offered risk-reducing therapies. The approach in which individual risk factors are counted does not take into account the degree of elevation of the risk factors (e.g., blood pressure, cholesterol level) or the fact that the strongest risk factor is age. Thus, methods based on counting risk factors often misclassify millions of adults who could benefit from risk-reducing therapy.19 Finally, risk factor identification alone may not provide the physician and patient with enough information to make an informed decision about the use of pharmacologic agents, particularly aspirin, for primary prevention.
An alternative approach to addressing cardiovascular disease prevention is global risk calculation. As part of the effort to improve primary clinical prevention of cardiovascular disease, multiple national guidelines have recommended estimating the patient’s global CHD risk as a starting point (Table 2).9,20,21 In combination with risk-based treatment thresholds, global CHD risk assessment can help allocate preventive care to patients in need and may avoid harm in those who are not. An additional underlying goal is motivation of physicians and patients to address CHD risk.
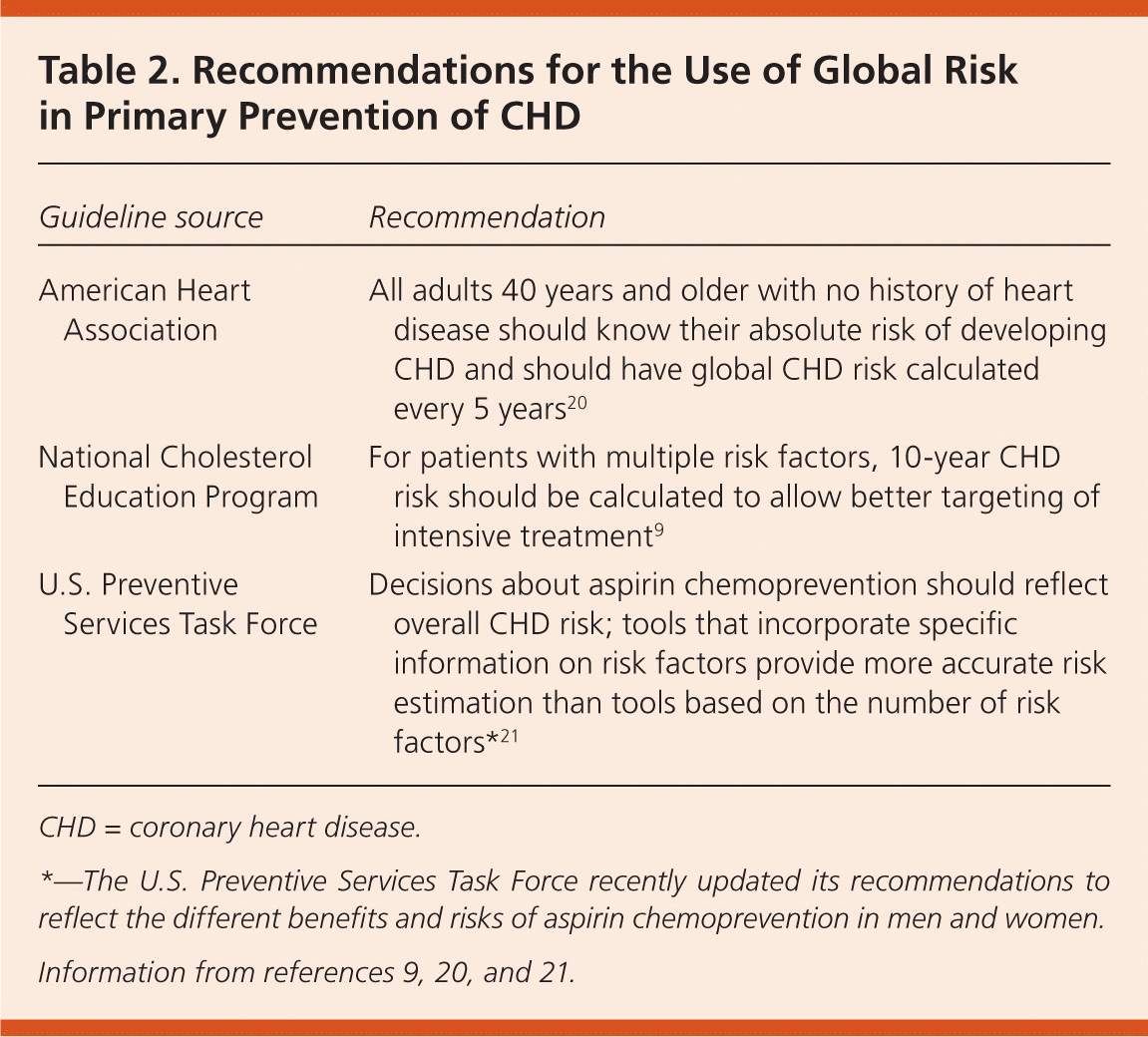
Table 2. Recommendations for the Use of Global Risk in Primary Prevention of CHD
| Guideline source | Recommendation |
|---|---|
| American Heart Association | All adults 40 years and older with no history of heart disease should know their absolute risk of developing CHD and should have global CHD risk calculated every 5 years20 |
| National Cholesterol Education Program | For patients with multiple risk factors, 10-year CHD risk should be calculated to allow better targeting of intensive treatment9 |
| U.S. Preventive Services Task Force | Decisions about aspirin chemoprevention should reflect overall CHD risk; tools that incorporate specific information on risk factors provide more accurate risk estimation than tools based on the number of risk factors*21 |
CHD = coronary heart disease.
*— The U.S. Preventive Services Task Force recently updated its recommendations to reflect the different benefits and risks of aspirin chemoprevention in men and women. Information from references 9, 20, and 21.
Evidence for Global Risk Approach
Global CHD risk calculation has been proven superior to risk estimation by physicians.22,23 Analyses of receiver operator characteristic curves (i.e., graphical techniques to assess the relative accuracy of different tests) have shown that in both men and women, global CHD risk calculation is better at predicting events than risk factor counting.7 Thus, global CHD risk calculation can assist physicians in identifying patients at moderate to high risk who stand to benefit most from preventive pharmacotherapy.
In addition to improving delivery of risk-reducing therapy to patients who are most likely to benefit, global CHD risk calculation also may reduce the chance that patients are more likely to be harmed than helped from such therapy. For example, a 40-year-old man with no risk factors whose global CHD risk is 3 percent over 10 years may be more likely to be harmed than helped by daily aspirin chemoprophylaxis.24 Of 1,000 such men, 30 will have a CHD-related event without aspirin chemoprophylaxis. If all 1,000 men take a daily aspirin, approximately 10 of the 30 will not have a CHD-related event. However, of the 1,000 men, approximately one will have a hemorrhagic stroke, and eight will have severe gastrointestinal bleeding over 10 years.15 Calculation of global CHD risk is particularly useful in situations such as this, when aspirin is considered for primary prevention. Because the risk-benefit ratio of aspirin chemoprophylaxis transitions from harmful to helpful at a 10-year CHD risk of 4 to 12 percent in men (depending on age),24 physicians must be able to estimate risk with relatively fine gradations to effectively counsel patients and make recommendations. Aspirin chemoprophylaxis seems to be more effective for MI prevention in men and for ischemic stroke prevention in women.21 Therefore, additional stroke risk calculations may be necessary to guide aspirin chemoprophylaxis in women. In addition, the risk of harms may be different in men compared with women. The U.S. Preventive Services Task Force recently updated its recommendations to reflect these differences.15
Effectiveness of Global Risk Approach
Although the rationale for using global CHD risk is sound and current guidelines recommend using it as a starting point for primary prevention of CHD, there is relatively little research on the effectiveness of this approach in clinical practice. A recent systematic review synthesized the findings of six studies of the effects of physicians knowing a patient’s global CHD risk.25 No good-quality studies addressing this issue were identified. Two fair-quality controlled trials showed that physicians who know patients’ global risk are more likely to prescribe risk-reducing therapy to those at high risk of a CHD-related event.26,27 Other studies were too methodologically limited to inform the authors’ conclusions. The same systematic review found no harms resulting from physicians knowing patients’ CHD risk if that information is accompanied by education about risk-reduction strategies.
In another recent systematic review, the authors identified 18 unique good- or fair-quality studies examining whether interventions that provided adults with an assessment of their global CHD risk improved various outcomes, including accuracy of risk perception and intent to start therapy.28 The review showed that global CHD risk information seems to improve the accuracy of risk perception and increases intent to initiate cardiovascular preventive care in those at moderate to high risk. The effect of global risk presentation on more distal outcomes (e.g., actual risk factor level, risk reduction) is less clear and may be related to the intensity of other interventions (e.g., counseling sessions), as well as repeated presentations of global CHD risk. For example, studies that examined repeated global risk presentation or repeated counseling found reductions in 10-year predicted CHD risk (0.2 to 2 percent), effects that would be clinically important on a population level (number needed to treat = 50 to 500).28
Calculating Global Risk
Because global CHD risk calculation more accurately identifies patients who will benefit from risk-reducing therapy, and because such information may motivate patients and physicians to address CHD risk, primary care physicians need tools designed to easily calculate risk with readily available clinical information. Many tools for calculating CHD risk are available.29–33 In the United States, calculators based on the Framingham Heart Study are generally recommended.29 The Framingham Heart Study included 2,439 white men and 2,812 white women, ranging from 30 to 74 years of age, and its risk equations have been proven reliable in black men and women, as well.34 However, they tend to overestimate CHD risk in Hispanic and Japanese-American men, Native American women, and Chinese men and women.35 Framingham equations have been recalibrated for use in these populations34; however, there are no readily available tools to calculate these risks in clinical practice.
Some of the easier-to-use Framingham-based CHD risk tools for whites and blacks are listed in Table 3.7,29,36 Physicians should realize that not all Framingham tools are the same. Some calculate the risk of death and MI only, whereas others calculate the risk of death, MI, and heart-related chest pain. Nearly all tools require information on the patient’s age, sex, systolic blood pressure, and total cholesterol level, and whether the patient smokes or has diabetes mellitus. Some require additional or different data (e.g., high-density and low-density lipoprotein levels, presence of left ventricular hypertrophy, hypertension treatment).29 Although family history is not included in most risk calculators, patients with a strong family history of early-onset cardiovascular disease (i.e., father with an event before 55 years of age, mother with an event before 65 years of age) are likely at greater risk than the calculations indicate.37
Table 3. Selected Framingham-Based Global CHD Risk Calculators

| Source | Type of tool | Web site | Comment |
|---|---|---|---|
| Calculators for hard CHD events* | |||
| American Heart Association | Web | http://www.americanheart.org/presenter.jhtml?identifier=3003499 | Targeted to patients rather than physicians; also evaluates for metabolic syndrome; requires fasting glucose, total cholesterol, LDL, HDL, and triglyceride levels |
| Joint British Societies | Chart | http://www.bhsoc.org/Cardiovascular_Risk_Prediction_Chart.stm | Spreadsheet calculator is also available at: http://www.bhsoc.org/Cardiovascular_Risk_Charts_and_Calculators.stm |
| National Cholesterol Education Program | Web and PDA | http://hp2010.nhlbihin.net/atpiii/calculator.asp | Downloadable tools are also available at: http://www.nhlbi.nih.gov/guidelines/cholesterol/index.htm |
| New Zealand Guidelines Group | Chart | http://www.nzgg.org.nz/guidelines/0035/CVD_Risk_Chart.pdf | Calculates 5-year risk; outcomes also include stroke and transient ischemic attack |
| Calculators for total CHD events† | |||
| Framingham Heart Study | Chart | http://www.framinghamheartstudy.org/risk/hrdcoronary.html | — |
| Heart-to-Heart | Web and PDA | http://www.med-decisions.com | For use by patients or physicians; presents risk-reducing options |
| Modified Sheffield table36 | Chart | http://www.bmj.com/content/vol320/issue7236/images/large/wale3599.f1.jpeg | — |
note: CHD risk calculators are sometimes included in other medical PDA programs, such as Epocrates.
CHD = coronary heart disease; HDL = high-density lipoprotein; LDL = low-density lipoprotein; PDA = personal digital assistant.
*— Hard events include death and myocardial infarction.
†— Total events include stable and unstable angina, as well as death and myocardial infarction.
It has been difficult to improve upon the overall predictive ability of the original Framingham tools (i.e., those including traditional risk factors) by adding other risk factors (e.g., body mass index, physical activity level) or novel risk markers (e.g., C-reactive protein, homocysteine, lipoprotein (a) levels).38 Recently there has been particular interest in using C-reactive protein levels to guide the use of statins.39 Compared with the use of Framingham or other global CHD risk calculation tools alone, there is little evidence that the use of C-reactive protein levels leads to improved outcomes or better cost-effectiveness.40
Whichever tool is used, a patient’s CHD risk should not be the sole basis for clinical decision making about whether to recommend smoking cessation or hypertension treatment. These therapies have additional benefits beyond CHD risk reduction.
Presenting Risk Information to Patients
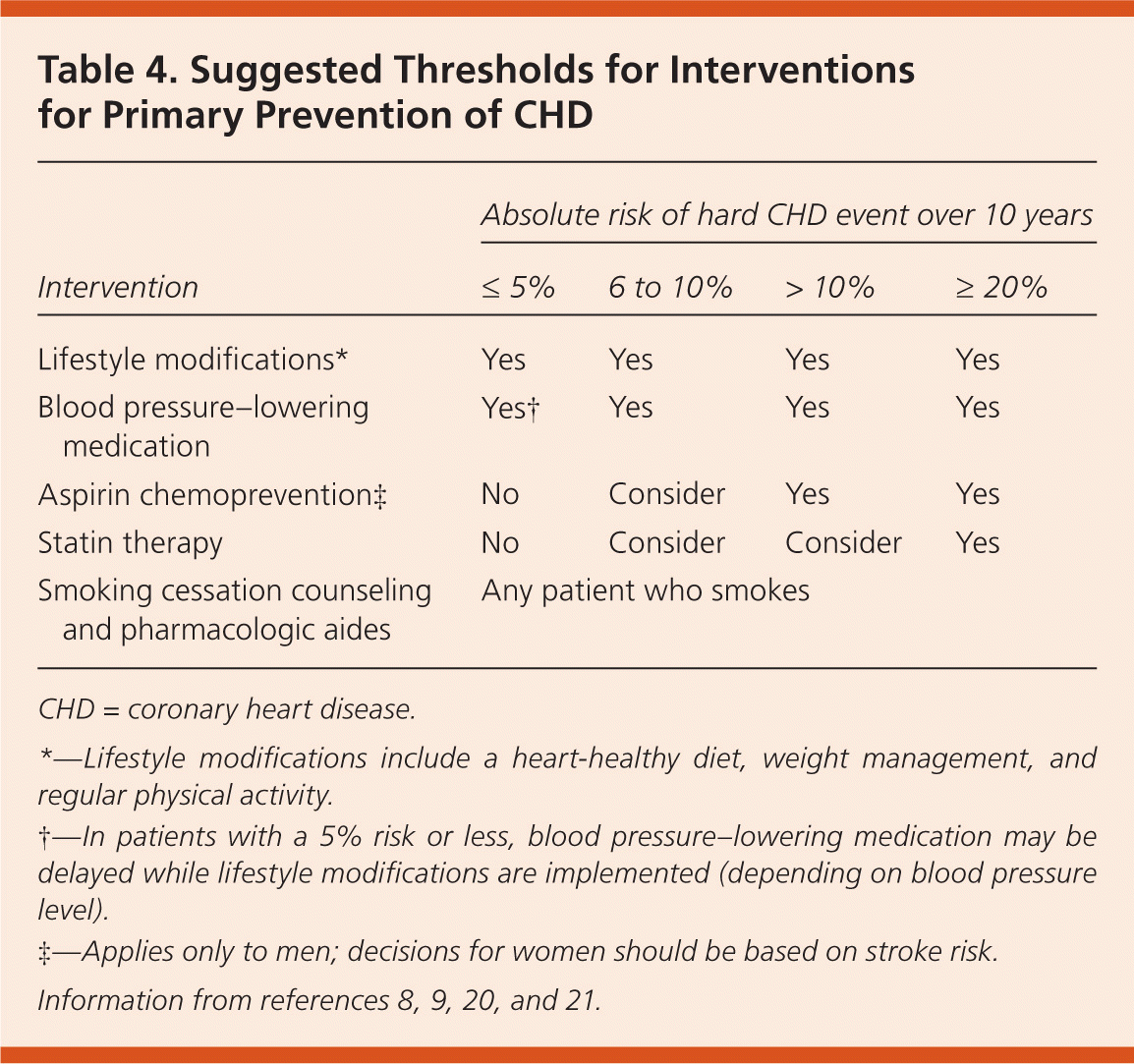
To help patients understand their risk information and to use risk information to its fullest motivational advantage, physicians must apply the principles of effective risk communication. First, risk should be presented as a percentage or frequency, along with information about the character and permanence of the events predicted and the time frame over which the risk accrues.41,42 Physicians should provide information about what constitutes an actionable level of risk based on current guidelines (Table 4).8,9,20,21
To help motivate patients, physicians should present a comparative risk for a person of the same age and sex who has no major risk factors, as well as the relative and absolute benefits of risk-reducing therapies.43,44 This allows for estimation of the total risk reduction that can be achieved by single interventions or by a combination of therapies. For example, a 53-year-old man who smokes and has hypertension has a 20 percent CHD risk over 10 years. If he stops smoking, his global risk is reduced to 10 percent (a 50 percent relative risk reduction). If he stops smoking and begins antihypertensive therapy, his 10-year global risk is reduced to about 7 percent (an additional 30 percent relative risk reduction). If he stops smoking, begins antihypertensive therapy, and takes a daily low-dose aspirin, his 10-year global CHD risk is about 5 percent (an additional 28 percent relative risk reduction).
Table 4. Suggested Thresholds for Interventions for Primary Prevention of CHD
| Intervention | Absolute risk of hard CHD event over 10 years | |||
|---|---|---|---|---|
| ≤ 5% | 6 to 10% | > 10% | ≥ 20% | |
| Lifestyle modifications* | Yes | Yes | Yes | Yes |
| Blood pressure–lowering medication | Yes† | Yes | Yes | Yes |
| Aspirin chemoprevention‡ | No | Consider | Yes | Yes |
| Statin therapy | No | Consider | Consider | Yes |
| Smoking cessation counseling and pharmacologic aides | Any patient who smokes | |||
CHD = coronary heart disease.
*— Lifestyle modifications include a heart-healthy diet, weight management, and regular physical activity.
†— In patients with a 5% risk or less, blood pressure–lowering medication may be delayed while lifestyle modifications are implemented (depending on blood pressure level).
‡— Applies only to men; decisions for women should be based on stroke risk.
Risks and benefits can also be presented in graphical formats, such as pictographs (e.g., a plot of faces representing benefits and harms [Figure 345 ]).46 Some evidence suggests that patients prefer graphical to numeric formats.47,48 However, patient comprehension seems to be best with numeric formats.49 Other recommendations for presenting CHD risk to patients are shown in Table 5.9,20,24,28,41–44,46–49
Figure 3. Cates Plot Showing Risks and Benefits of Aspirin Chemoprevention

Picture display of the benefits of 10 years of aspirin chemoprevention among 1,000 persons with a 10 percent 10-year global risk of coronary heart disease (CHD). Green faces represent the number of patients who would not benefit because they are not among the 10 percent predicted to have a CHD-related event. The red faces represent the number of patients who would have an event despite taking aspirin. The yellow faces represent patients who would not have an event because they took aspirin (i.e., the number of patients who would benefit).
Reprinted with permission from Dr. Chris Cates’ EBM Web site. http://nntonline.net/visualrx. Accessed April 28, 2010.
Table 5. Current Best Practices for Presenting Global CHD Risk Information to Patients

| Global CHD risk should be presented with comparative information for persons of the same age and sex who have no risk factors |
| In addition to presenting the absolute risk as a percentage, consider presenting in other numerical formats (e.g., number of persons per 1,000 over a specific period) or picture format (e.g., number of smiley/sad faces out of 100 persons) |
| Rather than categorizing risk as low, moderate, or high, a person’s risk should be placed in the context of what is considered an actionable level (see Table 4) |
| Global CHD risk should be presented in isolation of other risks (or with emphasis on the CHD risk) |
| Global CHD risk should be presented with information about controlling risk |
| Global CHD risk appears to be more influential when presented by physicians (as opposed to non-physician personnel or a computer program) |
CHD = coronary heart disease.
Information from references 9, 20, 24, 28, 41 through 44, and 46 through 49.
Uncertainties and Future Direction
Despite increasing evidence on the benefits of risk calculation and communication, many issues remain unresolved. First, it is unclear whether risk should be calculated for certain patient subgroups. Although some studies have suggested that diabetes is a CHD risk equivalent,50,51 others, including a recent meta-analysis, suggest that risk calculation may be a better approach, particularly in younger patients with diabetes and few risk factors.52–54 However, patients with chronic kidney disease are at increased risk of CHD, and current guidelines recommend treating these patients as high risk.55
It is unclear which particular risk outcomes are best calculated. There may be differences in the predictive abilities of calculators with different outcomes (e.g., hard versus total CHD-related events, CHD versus all cardiovascular disease risk, 10-year versus lifetime risk). The use of these different calculators may result in different prescribing decisions, although this possibility has not been studied. Finally, there is still much to be learned about the best methods of presenting risk to patients, particularly those with low literacy or numeracy skills. Nevertheless, it is a patient’s actual risk (e.g., 20 percent risk of CHD-related event in the next 10 years) rather than an isolated risk factor (e.g., elevated low-density lipoprotein level) that should guide discussions and decisions about preventive medical therapies.

