Migraine headache is a common and potentially debilitating disorder often treated by family physicians. Before diagnosing migraine, serious intracranial pathology must be ruled out. Treating acute migraine is challenging because of substantial rates of nonresponse to medications and difficulty in predicting individual response to a specific agent or dose. Data comparing different drug classes are relatively scarce. Abortive therapy should be used as early as possible after the onset of symptoms. Effective first-line therapies for mild to moderate migraine are nonprescription nonsteroidal anti-inflammatory drugs and combination analgesics containing acetaminophen, aspirin, and caffeine. Triptans are first-line therapies for moderate to severe migraine, or mild to moderate migraine that has not responded to adequate doses of simple analgesics. Triptans should be avoided in patients with vascular disease, uncontrolled hypertension, or hemiplegic migraine. Intravenous antiemetics, with or without intravenous dihydroergotamine, are effective therapies in an emergency department setting. Dexamethasone may be a useful adjunct to standard therapy in preventing short-term headache recurrence. Intranasal lidocaine may also have a role in relief of acute migraine. Isometheptene-containing compounds and intranasal dihydroergotamine are also reasonable therapeutic options. Medications containing opiates or barbiturates should be avoided for acute migraine. During pregnancy, migraine may be treated with acetaminophen or nonsteroidal anti-inflammatory drugs (prior to third trimester), or opiates in refractory cases. Acetaminophen, ibuprofen, intranasal sumatriptan, and intranasal zolmitriptan seem to be effective in children and adolescents, although data in these age groups are limited.
Migraine headache is one of the most common, yet potentially debilitating disorders encountered in primary care. Approximately 18 percent of women and 6 percent of men in the United States have migraine headaches, and 51 percent of these persons report reduced work or school productivity.1 Patients typically describe recurrent headaches with similar symptoms, and approximately one-third describe an aura preceding the headache.1 This article reviews treatment options for acute migraine headache.
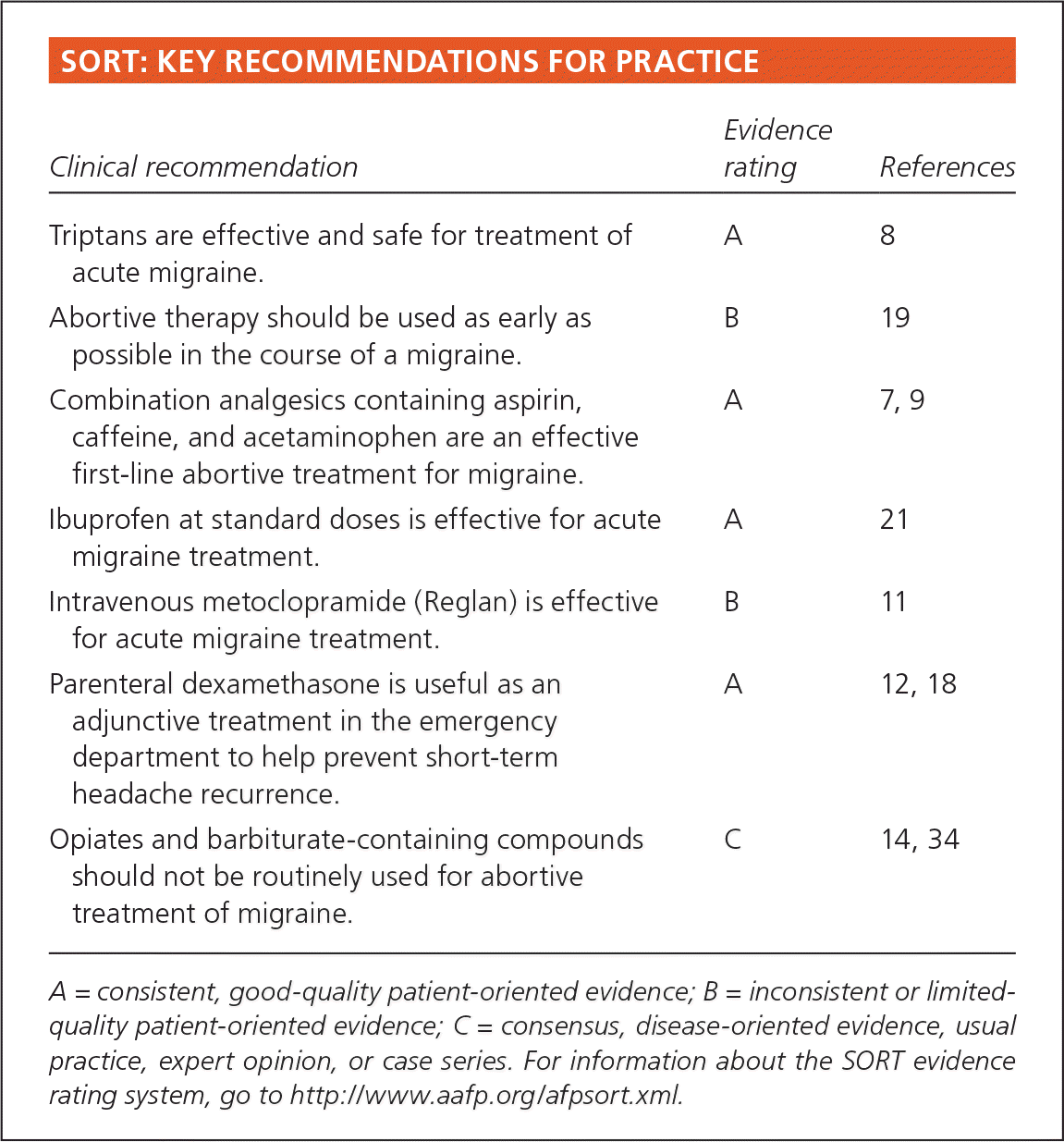
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Triptans are effective and safe for treatment of acute migraine. | A | 8 |
| Abortive therapy should be used as early as possible in the course of a migraine. | B | 19 |
| Combination analgesics containing aspirin, caffeine, and acetaminophen are an effective first-line abortive treatment for migraine. | A | 7, 9 |
| Ibuprofen at standard doses is effective for acute migraine treatment. | A | 21 |
| Intravenous metoclopramide (Reglan) is effective for acute migraine treatment. | B | 11 |
| Parenteral dexamethasone is useful as an adjunctive treatment in the emergency department to help prevent short-term headache recurrence. | A | 12, 18 |
| Opiates and barbiturate-containing compounds should not be routinely used for abortive treatment of migraine. | C | 14, 34 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limitedquality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Diagnosis
Table 1 lists International Headache Society diagnostic criteria for migraine with and without aura.2 A thorough history and physical examination can help confirm the diagnosis of migraine and rule out emergent conditions. The mnemonic POUND is an evidence-based aid for migraine diagnosis3:
- Pulsatile quality of headache
- One-day duration (four to 72 hours)
- Unilateral location
- Nausea or vomiting
- Disabling intensity
In a primary care setting, the probability of migraine is 92 percent in patients who report at least four of the five POUND symptoms.4 The probability decreases to 64 percent in patients with three of the symptoms, and 17 percent in patients with two or less symptoms.4
Table 1. International Headache Society Diagnostic Criteria for Migraine Headache With and Without Aura

| Migraine without aura | |
| Diagnostic criteria: | |
| Headache lasts four to 72 hours (untreated or unsuccessfully treated) | |
Headache has at least two of the following:
| |
During headache, at least one of the following:
| |
| Not attributed to another disorder | |
| History of at least five attacks fulfilling above criteria | |
| Migraine with aura | |
| Recurrent disorder manifesting in headaches of reversible focal neurologic symptoms that usually develop gradually over five to 20 minutes and last for less than 60 minutes | |
| Headache with the features of migraine without aura usually follows the aura symptoms | |
| Less commonly, headache lacks migrainous features or is completely absent | |
| Diagnostic criteria: | |
Aura consisting of at least one of the following, but no motor weakness:
| |
At least two of the following:
| |
| Headache fulfilling criteria for migraine without aura begins during the aura or follows aura within 60 minutes | |
| Not attributed to another disorder | |
| History of at least two attacks fulfilling above criteria |
Information from reference 2.
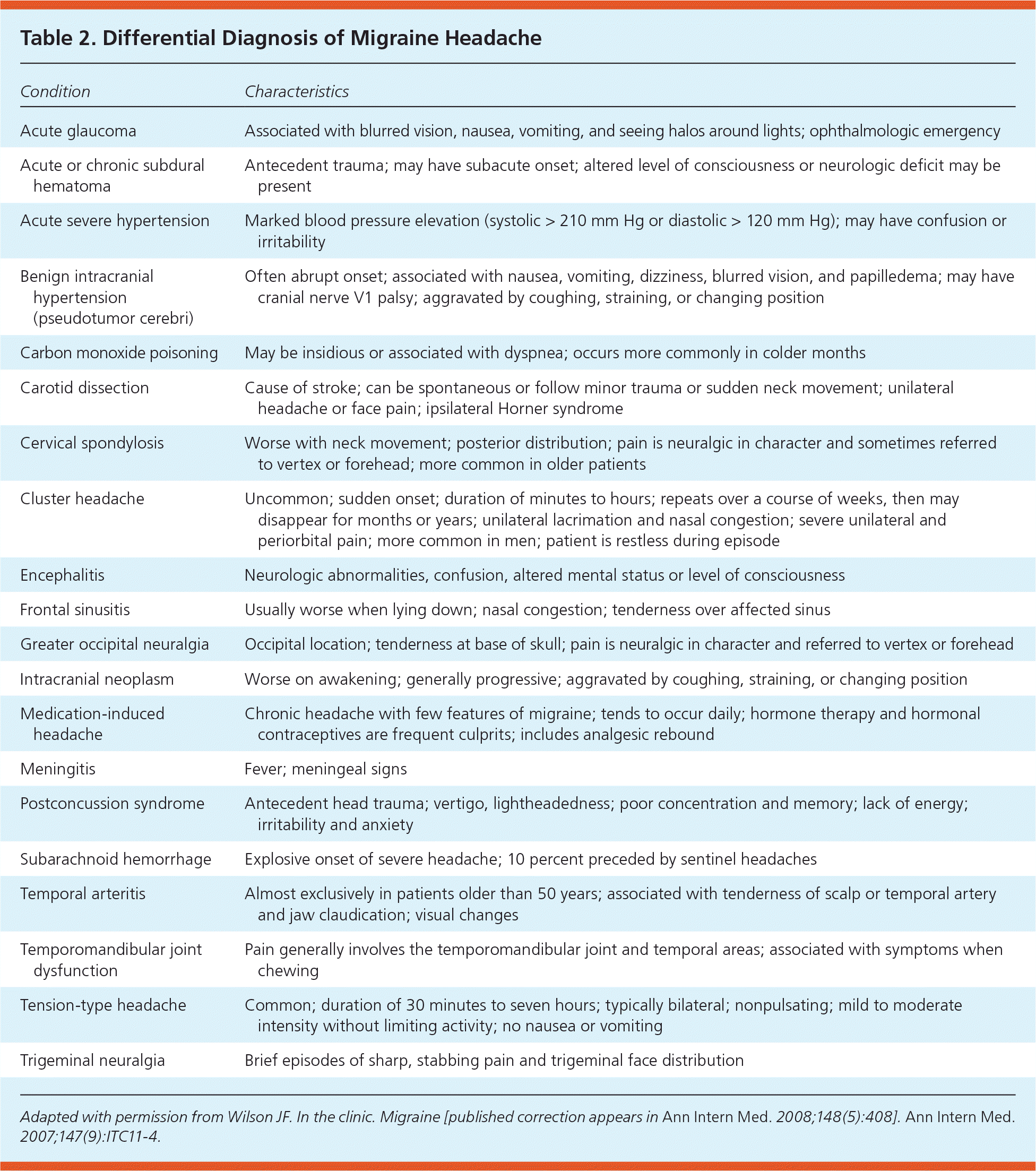
Table 2 outlines other serious causes of headache that must be considered in the differential diagnosis of migraine, such as temporal arteritis, cluster headache, and acute glaucoma.3 Fever, meningismus, or altered mental status should prompt investigation for meningitis or subarachnoid hemorrhage. The U.S. Headache Consortium recommends considering neuroimaging in patients with an unexplained abnormal finding on neurologic examination and in patients with atypical headache features or headaches that do not fulfill the strict definition of migraine or other primary headache disorder.5 The Consortium notes that neuroimaging generally is not indicated for patients with migraine and a normal neurologic examination.
In one study, age older than 50 years, sudden onset, and abnormal neurologic examination predicted serious intracranial pathology in adults presenting to an emergency department with nontraumatic headache; the presence of any one of these three features detected serious intracranial pathology with 98.6 percent sensitivity.6
Table 2. Differential Diagnosis of Migraine Headache
| Condition | Characteristics |
|---|---|
| Acute glaucoma | Associated with blurred vision, nausea, vomiting, and seeing halos around lights; ophthalmologic emergency |
| Acute or chronic subdural hematoma | Antecedent trauma; may have subacute onset; altered level of consciousness or neurologic deficit may be present |
| Acute severe hypertension | Marked blood pressure elevation (systolic > 210 mm Hg or diastolic > 120 mm Hg); may have confusion or irritability |
| Benign intracranial hypertension (pseudotumor cerebri) | Often abrupt onset; associated with nausea, vomiting, dizziness, blurred vision, and papilledema; may have cranial nerve V1 palsy; aggravated by coughing, straining, or changing position |
| Carbon monoxide poisoning | May be insidious or associated with dyspnea; occurs more commonly in colder months |
| Carotid dissection | Cause of stroke; can be spontaneous or follow minor trauma or sudden neck movement; unilateral headache or face pain; ipsilateral Horner syndrome |
| Cervical spondylosis | Worse with neck movement; posterior distribution; pain is neuralgic in character and sometimes referred to vertex or forehead; more common in older patients |
| Cluster headache | Uncommon; sudden onset; duration of minutes to hours; repeats over a course of weeks, then may disappear for months or years; unilateral lacrimation and nasal congestion; severe unilateral and periorbital pain; more common in men; patient is restless during episode |
| Encephalitis | Neurologic abnormalities, confusion, altered mental status or level of consciousness |
| Frontal sinusitis | Usually worse when lying down; nasal congestion; tenderness over affected sinus |
| Greater occipital neuralgia | Occipital location; tenderness at base of skull; pain is neuralgic in character and referred to vertex or forehead |
| Intracranial neoplasm | Worse on awakening; generally progressive; aggravated by coughing, straining, or changing position |
| Medication-induced headache | Chronic headache with few features of migraine; tends to occur daily; hormone therapy and hormonal contraceptives are frequent culprits; includes analgesic rebound |
| Meningitis | Fever; meningeal signs |
| Postconcussion syndrome | Antecedent head trauma; vertigo, lightheadedness; poor concentration and memory; lack of energy; irritability and anxiety |
| Subarachnoid hemorrhage | Explosive onset of severe headache; 10 percent preceded by sentinel headaches |
| Temporal arteritis | Almost exclusively in patients older than 50 years; associated with tenderness of scalp or temporal artery and jaw claudication; visual changes |
| Temporomandibular joint dysfunction | Pain generally involves the temporomandibular joint and temporal areas; associated with symptoms when chewing |
| Tension-type headache | Common; duration of 30 minutes to seven hours; typically bilateral; nonpulsating; mild to moderate intensity without limiting activity; no nausea or vomiting |
| Trigeminal neuralgia | Brief episodes of sharp, stabbing pain and trigeminal face distribution |
Adapted with permission from Wilson JF. In the clinic. Migraine [published correction appears in Ann Intern Med. 2008;148(5):408]. Ann Intern Med. 2007;147(9):ITC11-4.
General Treatment Principles
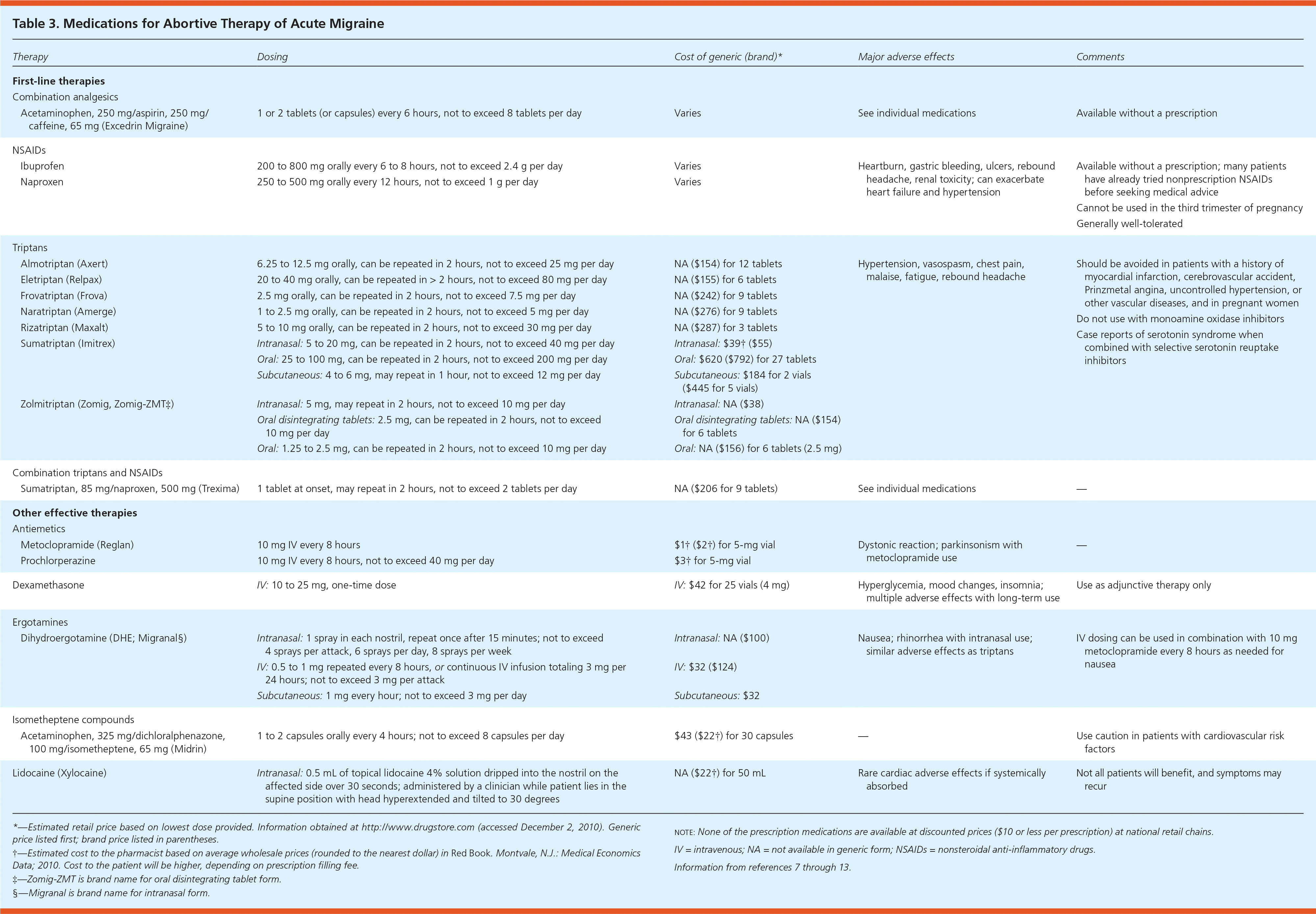
Several medications from different classes are available to treat acute migraine (Table 37–13 ). Because relatively few trials have directly compared the different medication classes available to treat acute migraine, definitive treatment algorithms cannot be developed. More than one-half of persons treat their migraine headaches with nonprescription medications, and patients often present to physicians after unsuccessfully trying multiple nonprescription therapies.7 The U.S. Headache Consortium guidelines offer a general strategy based on expert consensus.14 Nonsteroidal anti-inflammatory drugs (NSAIDs) or caffeine-containing combination analgesics may be first-line treatment for mild to moderate migraine, or severe migraine that has previously responded to these agents. Triptans are considered first-line abortive treatment of moderate to severe migraine, or mild attacks that have not responded to nonprescription medicines. Ergotamine-containing compounds may also be reasonable in this situation.14 Figure 1 provides a suggested algorithm for management of acute migraine headaches.5,6,11,12,14–18
Table 3. Medications for Abortive Therapy of Acute Migraine
| Therapy | Dosing | Cost of generic (brand)* | Major adverse effects | Comments | |
|---|---|---|---|---|---|
| First-line therapies | |||||
| Combination analgesics | |||||
| Acetaminophen, 250 mg/aspirin, 250 mg/caffeine, 65 mg (Excedrin Migraine) | 1 or 2 tablets (or capsules) every 6 hours, not to exceed 8 tablets per day | Varies | See individual medications |
| |
| NSAIDs | |||||
| Ibuprofen | 200 to 800 mg orally every 6 to 8 hours, not to exceed 2.4 g per day | Varies | Heartburn, gastric bleeding, ulcers, rebound headache, renal toxicity; can exacerbate heart failure and hypertension |
| |
| Naproxen | 250 to 500 mg orally every 12 hours, not to exceed 1 g per day | Varies | |||
| Triptans | |||||
| Almotriptan (Axert) | 6.25 to 12.5 mg orally, can be repeated in 2 hours, not to exceed 25 mg per day | NA ($154) for 12 tablets | Hypertension, vasospasm, chest pain, malaise, fatigue, rebound headache |
| |
| Eletriptan (Relpax) | 20 to 40 mg orally, can be repeated in > 2 hours, not to exceed 80 mg per day | NA ($155) for 6 tablets | |||
| Frovatriptan (Frova) | 2.5 mg orally, can be repeated in 2 hours, not to exceed 7.5 mg per day | NA ($242) for 9 tablets | |||
| Naratriptan (Amerge) | 1 to 2.5 mg orally, can be repeated in 2 hours, not to exceed 5 mg per day | NA ($276) for 9 tablets | |||
| Rizatriptan (Maxalt) | 5 to 10 mg orally, can be repeated in 2 hours, not to exceed 30 mg per day | NA ($287) for 3 tablets | |||
| Sumatriptan (Imitrex) | Intranasal: 5 to 20 mg, can be repeated in 2 hours, not to exceed 40 mg per day | Intranasal: $39† ($55) | |||
| Oral: 25 to 100 mg, can be repeated in 2 hours, not to exceed 200 mg per day | Oral: $620 ($792) for 27 tablets | ||||
| Subcutaneous: 4 to 6 mg, may repeat in 1 hour, not to exceed 12 mg per day | Subcutaneous: $184 for 2 vials ($445 for 5 vials) | ||||
| Zolmitriptan (Zomig, Zomig-ZMT‡) | Intranasal: 5 mg, may repeat in 2 hours, not to exceed 10 mg per day | Intranasal: NA ($38) | |||
| Oral disintegrating tablets: 2.5 mg, can be repeated in 2 hours, not to exceed 10 mg per day | Oral disintegrating tablets: NA ($154) for 6 tablets | ||||
| Oral: 1.25 to 2.5 mg, can be repeated in 2 hours, not to exceed 10 mg per day | Oral: NA ($156) for 6 tablets (2.5 mg) | ||||
| Combination triptans and NSAIDs | |||||
| Sumatriptan, 85 mg/naproxen, 500 mg (Trexima) | 1 tablet at onset, may repeat in 2 hours, not to exceed 2 tablets per day | NA ($206 for 9 tablets) | See individual medications |
| |
| Other effective therapies | |||||
| Antiemetics | |||||
| Metoclopramide (Reglan) | 10 mg IV every 8 hours | $1† ($2†) for 5-mg vial | Dystonic reaction; parkinsonism with metoclopramide use |
| |
| Prochlorperazine | 10 mg IV every 8 hours, not to exceed 40 mg per day | $3† for 5-mg vial | |||
| Dexamethasone [ | 10 to 25 mg IV, one-time dose | $42 for 25 vials (4 mg) | Hyperglycemia, mood changes, insomnia; multiple adverse effects with long-term use |
| |
| Ergotamines | |||||
| Dihydroergotamine (DHE; Migranal§) | Intranasal: 1 spray in each nostril, repeat once after 15 minutes; not to exceed 4 sprays per attack, 6 sprays per day, 8 sprays per week | Intranasal: NA ($100) | Nausea; rhinorrhea with intranasal use; similar adverse effects as triptans |
| |
| IV: 0.5 to 1 mg repeated every 8 hours, or continuous IV infusion totaling 3 mg per 24 hours; not to exceed 3 mg per attack | IV: $32 ($124) | ||||
| Subcutaneous: 1 mg every hour; not to exceed 3 mg per day | Subcutaneous: $32 | ||||
| Isometheptene compounds | |||||
| Acetaminophen, 325 mg/dichloralphenazone, 100 mg/isometheptene, 65 mg (Midrin) | 1 to 2 capsules orally every 4 hours; not to exceed 8 capsules per day | $43 ($22†) for 30 capsules | – |
| |
| Lidocaine (Xylocaine) | Intranasal: 0.5 mL of topical lidocaine 4% solution dripped into the nostril on the affected side over 30 seconds; administered by a clinician while patient lies in the supine position with head hyperextended and tilted to 30 degrees | NA ($22†) for 50 mL | Rare cardiac adverse effects if systemically absorbed |
| |
note: None of the prescription medications are available at discounted prices ($10 or less per prescription) at national retail chains.
IV = intravenous; NA = not available in generic form; NSAIDs = nonsteroidal anti-inflammatory drugs.
*—Estimated retail price based on lowest dose provided. Information obtained at http://www.drugstore.com (accessed December 2, 2010). Generic price listed first; brand price listed in parentheses.
†—Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, N.J.: Medical Economics Data; 2010. Cost to the patient will be higher, depending on prescription filling fee.
‡—Zomig-ZMT is brand name for oral disintegrating tablet form.
§—Migranal is brand name for intranasal form.
Figure 1. Management of Acute Migraine Headache
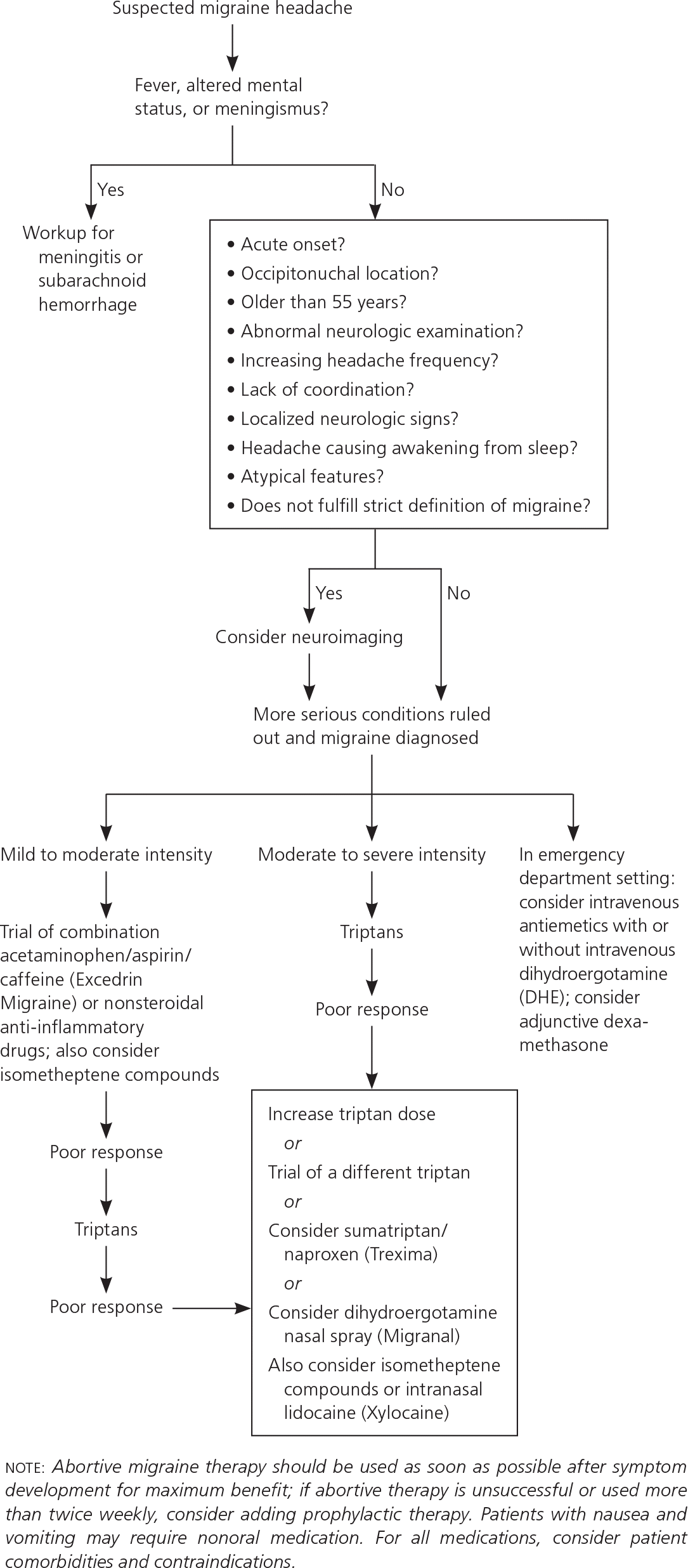
Algorithm for management of suspected migraine headache.
Information from references 5, 6, 11, 12, and 14 through 18
Predicting individual response to a specific medication is difficult. Complete pain relief is not always achievable. For example, studies report complete pain relief within two hours in 45 to 77 percent of patients taking triptans.1,8 Potential adverse effects, contraindications, pharmacokinetics, and route of administration are often primary determinants of medication choice. Patients with severe nausea and vomiting often require nonoral medication.
Evidence suggests that abortive therapy works best if taken soon after the onset of migraine or during aura, before pain progresses. A trial using almotriptan (Axert) showed that early users (i.e., therapy initiated within one hour of headache onset) had greater relief and lower recurrence rates of pain than non-early users.19 Nonprescription analgesics have shown comparable effectiveness with triptans if used in adequate doses soon after headache onset.9
Prophylactic therapy may be appropriate for selected patients. The U.S. Headache Consortium's recommended indications for prophylactic therapy in patients with migraine headache are20:
- Contraindications or intolerance to abortive therapies
- Headache symptoms occurring more than two days per week
- Headaches that severely limit quality of life despite abortive therapy
- Presence of uncommon migraine conditions, including hemiplegic migraine, basilar migraine, migraine with prolonged aura, or migrainous infarction.
First-Line Therapies
COMBINATION ANALGESICS
The combination analgesic acetaminophen/aspirin/caffeine (Excedrin Migraine) is effective, inexpensive, available without prescription, and free from most vascular contraindications associated with triptans. Its use in migraine treatment has shown favorable results when compared with 50 mg of sumatriptan (Imitrex) in one trial and with placebo in previous trials.9 Patients with severe pain were included, but patients requiring bed rest or who were consistently vomiting during headaches were excluded.9 A study that included these more severe cases reported that acetaminophen/aspirin/caffeine is superior to 400 mg of ibuprofen.7
NSAIDS
NSAIDs are a convenient first-line therapy for mild to moderate migraine or historically responsive severe attacks. A 2007 meta-analysis of ibuprofen for moderate to severe migraine showed that 200-mg and 400-mg doses were effective for short-term pain relief, but had 24-hour pain-free rates similar to placebo.21 The 400-mg dose also helped relieve photophobia and phonophobia. A study comparing ketoprofen with zolmitriptan (Zomig) showed zolmitriptan to be modestly more effective (two-hour relief in 61.6 versus 66.8 percent of participants, respectively), but it was associated with more adverse events, such as tight throat and flushing.22 Ketorolac, a parenteral NSAID commonly used in emergency departments, was found to be effective in reducing self-reported headache symptoms one hour after injection, including one study showing more effectiveness than intranasal sumatriptan.23
TRIPTANS
Triptans are migraine-specific drugs that bind to serotonergic receptors. They are considered first-line therapy for moderate to severe migraine, or mild to moderate attacks unresponsive to nonspecific analgesics.14 Seven triptans are currently available, but data guiding which to select for an individual patient are limited. A Cochrane review found that all triptans are similar in effectiveness and tolerability.24 A meta-analysis of 53 trials using oral triptans found that the three most effective agents for pain relief were 10 mg of rizatriptan (Maxalt), 80 mg of eletriptan (Relpax), and 12.5 mg of almotriptan. 8 A Cochrane review found a dose of 100 mg of sumatriptan to be more effective than lower doses.24 It is sometimes necessary to increase the dose of an individual agent before judging response. Trials suggest that nonresponders to one triptan may respond to another; therefore, switching triptans is also reasonable.25
Triptans differ from one another in pharmacokinetics. Rizatriptan has a quicker onset of action than sumatriptan; frovatriptan (Frova), naratriptan (Amerge), and eletriptan have longer half-lives than sumatriptan.26 In practice, route of administration or pharmacokinetics often guide choice. Some triptans are available as nasal sprays, rapidly dissolving tablets (absorbed despite vomiting), or subcutaneous injections. Some physicians choose a triptan by matching pharmacokinetics to the temporal pattern of their patient's migraine (e.g., rapid-onset medication for short course of migraine versus longer-acting medication with slower onset for longer lasting symptoms); however, there is no definitive evidence to support this approach.
The vasoconstrictive properties of triptans preclude their use in patients with ischemic heart disease, stroke, uncontrolled hypertension, or hemiplegic or basilar migraine. However, the chest pain occurring in 3 to 5 percent of oral triptan users has not been associated with electrocardiographic changes and is rarely ischemic.8 A post-marketing study of subcutaneous sumatriptan in 12,339 patients without ischemic heart disease revealed 36 cardiac events, only two of which occurred within 24 hours of sumatriptan use.27 Nonetheless, if patients taking triptans develop suspected cardiac symptoms, triptans should be discontinued pending further evaluation. Cardiac evaluation is reasonable before triptan initiation in patients with multiple vascular risk factors.28
Triptans are contraindicated in patients taking monoamine oxidase inhibitors.14 Combining triptans with selective serotonin reuptake inhibitors can lead to serotonin syndrome, a potentially life-threatening condition characterized by altered mentation, autonomic instability, diarrhea, neuromuscular hyperactivity, and fever. The true incidence of serotonin syndrome in this setting is unknown. A 2006 U.S. Food and Drug Administration (FDA) alert cited 29 case reports over five years, although almost 700,000 patients per year are prescribed both selective serotonin reuptake inhibitors and triptans.29 Physicians treating patients who are taking triptans and selective serotonin reuptake inhibitors should be vigilant for serotonin syndrome, and should minimize drug dosages.
COMBINATION TRIPTANS AND NSAIDS
A fixed-dose combination of sumatriptan, 85 mg/naproxen, 500 mg (Trexima) is an option for acute treatment. One trial showed that the combination provided superior pain relief compared with either monotherapy.10 Another trial found similar results in previous nonresponders to triptans.15 Patients also may take triptans and NSAIDs concurrently.
Other Effective Therapies
ANTIEMETICS
Evidence supports a role for parenteral antiemetics in acute migraine, independent of their antinausea effects. A meta-analysis of 13 randomized controlled trials concluded that intravenous metoclopramide (Reglan) should be considered a primary agent in the treatment of migraine in emergency departments.11 Given the potential for rebound and dependence associated with opiates, antiemetics offer a reasonable alternative in acute settings. No evidence supports migraine-specific effects of oral antiemetics, other than relieving nausea.
DEXAMETHASONE
Intravenous dexamethasone has been used as adjunctive therapy for migraine in emergency departments. Two meta-analyses, each with seven randomized controlled trials in which dexamethasone was added to other standard therapies, showed that about 10 patients needed treatment to prevent headache recurrence within 24 to 72 hours12,18. [ corrected]
ERGOTAMINES
Like triptans, ergotamines and dihydroergotamine (DHE) are migraine-specific drugs that bind to serotonergic receptors. Although their use has been largely supplanted by triptans, ergot alkaloids still have a role in selected patients. Little evidence supports the use of oral ergotamines. Poor absorption and high rates of adverse events preclude their use in most situations. Combination medications containing ergotamines (e.g., ergotamine/caffeine [Cafergot]) may have fewer adverse effects than pure ergotamines.30
Nine placebo-controlled trials have demonstrated the effectiveness of dihydroergotamine nasal spray (Migranal), making it an option for nonoral medication.30 Comparison with subcutaneous sumatriptan showed lower effectiveness but fewer adverse effects.31 Intravenous dihydroergotamine, combined with antiemetics, may be a reasonable option in emergency departments. A meta-analysis showed comparable effectiveness to opiates and ketorolac when combined with an antiemetic, but inferiority to phenothiazines and triptans when used alone.16 Trials comparing subcutaneous dihydroergotamine with subcutaneous sumatriptan showed that dihydroergotamine had inferior effectiveness but fewer adverse events and headache recurrences.32
ISOMETHEPTENE COMPOUNDS
The combination drug acetaminophen/isometheptene/dichloralphenazone (Midrin) includes a sympathomimetic (isometheptene) and a muscle relaxant (dichloralphenazone). One trial showed similar effectiveness to low-dose sumatriptan when used early in mild to moderate migraine.17 Due to sympathomimetic effects, it should be used cautiously in patients with cardiac risk factors.
LIDOCAINE
Intranasal lidocaine (Xylocaine) has a rapid onset of action and may be useful as a temporizing measure until longer-acting treatment can take effect. Lidocaine 4% solution administered into the nostril, either by a clinician or self-administered by patients, resulted in rapid symptom reduction compared with control, although recurrences were common.13,33
Non-Preferred Therapies
Acetaminophen alone is not effective therapy for acute migraine.30 There are no placebo-controlled trials documenting the effectiveness of barbiturate-containing analgesics (e.g., butalbital/aspirin/caffeine [Fiorinal]) for acute migraine.30 The U.S. Headache Consortium recommends limiting opiate use in migraine treatment because of its potential for abuse and rebound headache.14 Intranasal butorphanol is effective, but its use should be limited because of these concerns.14 One study linked opiate or barbiturate use with an increased risk of episodic migraine becoming chronic.34 Opiates or barbiturate-containing medications should be used only in patients with migraine headaches resistant to other therapies.
Experimental Therapies
Calcitonin gene-related peptide is a neuropeptide thought to be central to migraine pathogenesis. Intravenous infusion of a calcitonin gene-related peptide antagonist showed promising results in one small study.35 Transcranial magnetic stimulation, a modality where a magnetic field is generated on the scalp to create currents in the adjacent cortex, seems promising. A controlled trial of 200 patients who had migraine with aura showed that this therapy is superior to sham in two-hour pain relief and sustained responses over 24 to 48 hours.36 Further research is needed to evaluate its role in treating migraine without aura and in migraine prophylaxis.
Special Populations
PREGNANCY
Acetaminophen, despite questionable effectiveness, is reasonable in the treatment of migraine in pregnant women because of its established safety. NSAIDs are effective and generally considered safe until the third trimester. The combination analgesic acetaminophen, 250 mg/aspirin, 250 mg/caffeine, 65 mg also must be used with caution; aspirin is FDA pregnancy category C, but is downgraded to category D for third trimester use, and consuming more than 100 mg of caffeine daily is associated with mild fetal growth restriction, although the clinical significance of this is unclear.37 The American Congress of Obstetricians and Gynecologists recommends limiting daily caffeine consumption to 300 mg during pregnancy.38 Avoidance of triptans is recommended during pregnancy, although limited data on first-trimester exposures are reassuring. 17,25 Metoclopramide is FDA pregnancy category B and may be used intravenously for migraine or orally for associated nausea. Opiates may be used for intractable cases, but pose risks of neonatal withdrawal and maternal dependence. The safety of isometheptene in pregnancy is unknown, so its use is not recommended. Ergotamines are abortifacients and are therefore absolutely contraindicated in pregnant women and women of childbearing age who are not using reliable contraception. Given scant data and cautions regarding medication safety, preventive approaches are key.
MENSTRUAL MIGRAINE
Many women report migraine or migraine exacerbations occurring exclusively near the time of menses. Long-acting triptans frovatriptan and naratriptan, taken perimenstrually around-the-clock for short-term prevention, have been found effective in reducing frequency and severity of menstrual migraine.39 For abortive therapy, the highest-quality evidence supports the use of sumatriptan, rizatriptan, and the NSAID mefenamic acid (Ponstel).39
CHILDREN AND ADOLESCENTS
Limited evidence is available to guide pharmacologic treatment of acute migraine in children and adolescents.40 A systematic review found acetaminophen and ibuprofen safe and effective in children.41 Triptans are often prescribed, although this is not FDA-approved or recommended by drug manufacturers. Intranasal sumatriptan and nasal zolmitriptan, but not oral formulations, have shown effectiveness in children and adolescents, perhaps because of the quicker onset of nasal formulations and shorter duration of migraines in children.40,41 Given limited data, prevention is important.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms migraine and treatment, with separate searches for specific drug classes. A similar search was performed using Google Scholar. The Cochrane database was searched for relevant reviews, and the National Guideline Clearinghouse was searched for relevant guidelines. We also searched the Evidence Summary provided by AFP for relevant articles. Search date: January 4, 2010, repeated September 20, 2010.

