A 61-year-old woman presented with a waxing and waning eruption that she noticed one year prior. Initially, the eruption was characterized by annular, eczematous plaques on the extremities. Findings from biopsies of these areas were consistent with allergic contact dermatitis; however, the lesions did not appear to be caused by contact with allergens. The rash did not resolve after multiple courses of topical and systemic steroids. Over a short period, the eruption generalized. The patient's medical history was significant for hidradenitis suppurativa, and she was allergic to penicillin and sulfa medications. She did not have constitutional symptoms or recent illness.
Physical examination revealed generalized erythematous, arcuate plaques studded with small, tense pustules (see accompanying figure) involving the flexural surfaces bilaterally. Crusts were present at the center of the plaques. Some plaques formed polycyclic lesions with serpiginous borders.
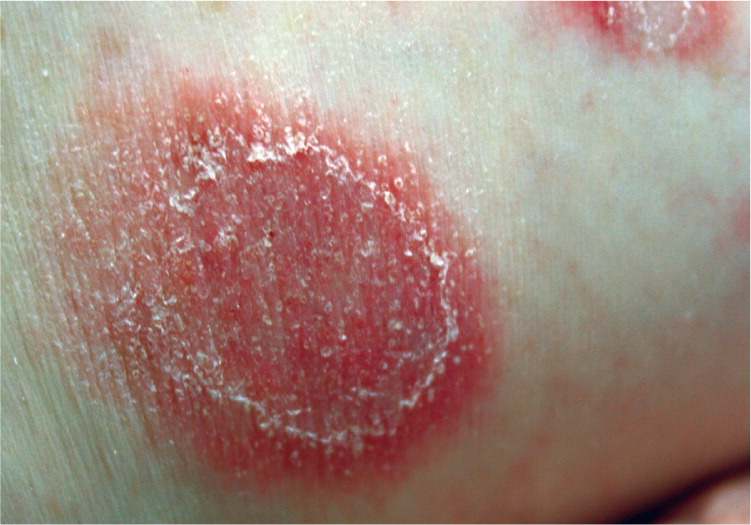
Results of bacterial and viral cultures were negative. A repeat skin biopsy was performed. Hematoxylin-eosin staining revealed mounds of neutrophils in the stratum corneum and superficial stratum granulosum. Results of direct immunofluorescence were negative for immunoglobulin deposition.
Question
Based on the patient's history, physical examination, and laboratory results, which one of the following is the most likely diagnosis?
A. Erythema annulare centrifugum.
B. Generalized pustular psoriasis.
C. Immunoglobulin A pemphigus.
D. Impetigo.
E. Subcorneal pustular dermatosis (Sneddon-Wilkinson disease).
Discussion
The answer is E: subcorneal pustular dermatosis (SCPD). SCPD, or Sneddon-Wilkinson disease, is a chronic eruption that typically affects women older than 40 years. It has a symmetric distribution of sterile, pea-sized pustules on erythematous plaques that are located in the axillae, groin, and inframammary folds. Scaling and crusting occur secondarily after rupture of the pustules. Histologic examination shows an accumulation of neutrophils under the stratum corneum. SCPD has a benign and chronic course. Lesions tend to wax and wane over several years.
The workup includes biopsy of perilesional skin for direct immunofluorescence to rule out immunoglobulin A (IgA) pemphigus. Repeat skin biopsies for direct immunofluorescence should be performed periodically during follow-up. In addition, screening for urine and serum monoclonal gammopathies should be performed to help exclude an underlying myeloma. Oral dapsone, 50 to 150 mg daily, is considered the first-line treatment for SCPD, but it may take several weeks to produce significant results.1 SCPD refractory to dapsone has been treated with phototherapy or acitretin (Soriatane), but isotretinoin is not effective.1
Erythema annulare centrifugum appears as arcuate or annular plaques with central clearing and a trailing collarette of scale. The lesions may be polycyclic and usually involve the trunk, buttocks, or lower extremities. Pustules typically are not present. Histologic examination shows a dermal lymphocytic infiltrate.2
Generalized pustular psoriasis is difficult to distinguish clinically from SCPD.1,3 Patients with generalized pustular psoriasis may have annular plaques studded with vesicles. However, patients usually present with systemic symptoms, such as fever, and may require hospitalization. Patients may have a history of psoriasis.3
IgA pemphigus is an autoimmune, blistering disease with vesiculopustular lesions commonly on the trunk, proximal extremities, and/or intertriginous areas. It is clinically indistinguishable from SCPD. Both diseases lead to neutrophil collections in the epidermis.1,4 In IgA pemphigus, direct immunofluorescence shows IgA deposition in the epidermis.1
Nobullous impetigo usually occurs during childhood and is typically characterized by localized vesicles that rupture and form honey-colored crusts. Culture is positive for staphylococcal and/or streptococcal organisms. Bullous impetigo commonly occurs in the neonatal period, often resolving within weeks.5
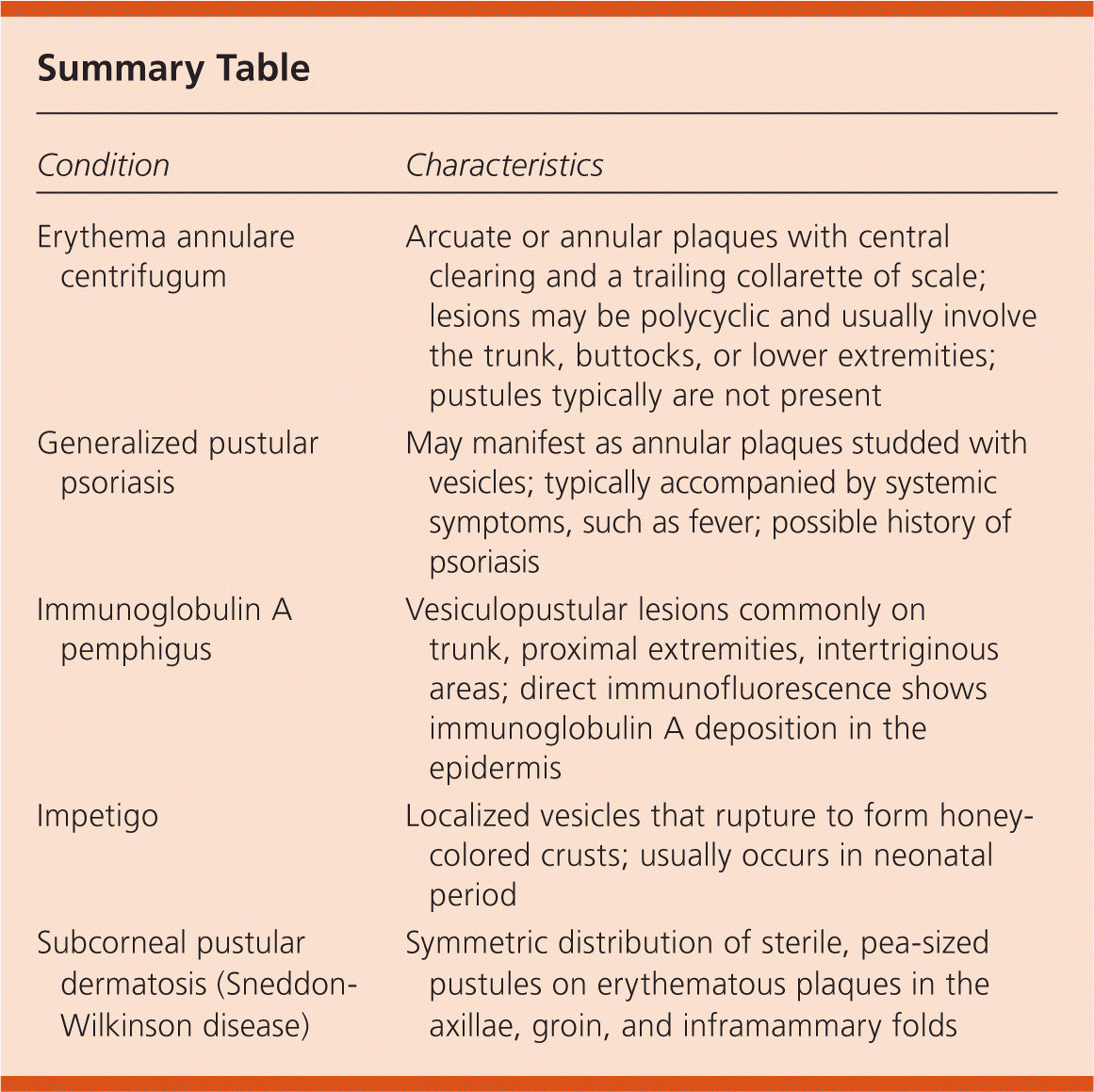
Summary Table
| Condition | Characteristics |
|---|---|
| Erythema annulare centrifugum | Arcuate or annular plaques with central clearing and a trailing collarette of scale; lesions may be polycyclic and usually involve the trunk, buttocks, or lower extremities; pustules typically are not present |
| Generalized pustular psoriasis | May manifest as annular plaques studded with vesicles; typically accompanied by systemic symptoms, such as fever; possible history of psoriasis |
| Immunoglobulin A pemphigus | Vesiculopustular lesions commonly on trunk, proximal extremities, intertriginous areas; direct immunofluorescence shows immunoglobulin A deposition in the epidermis |
| Impetigo | Localized vesicles that rupture to form honey-colored crusts; usually occurs in neonatal period |
| Subcorneal pustular dermatosis (Sneddon- Wilkinson disease) | Symmetric distribution of sterile, pea-sized pustules on erythematous plaques in the axillae, groin, and inframammary folds |

