Clinical Question
What is the role of antibody testing in the diagnosis of systemic lupus erythematosus (SLE)?
Evidence-Based Answer
Antibody testing plays an important role when assessing patients, but should not be used alone to diagnose SLE. (Strength of Recommendation: C, based on expert opinion.) The antinuclear antibody (ANA) test is the most commonly used screening test for SLE. The presence of anti-DNA, anti-Sm, and antiphospholipid antibodies is more specific for diagnosing SLE.
Evidence Summary
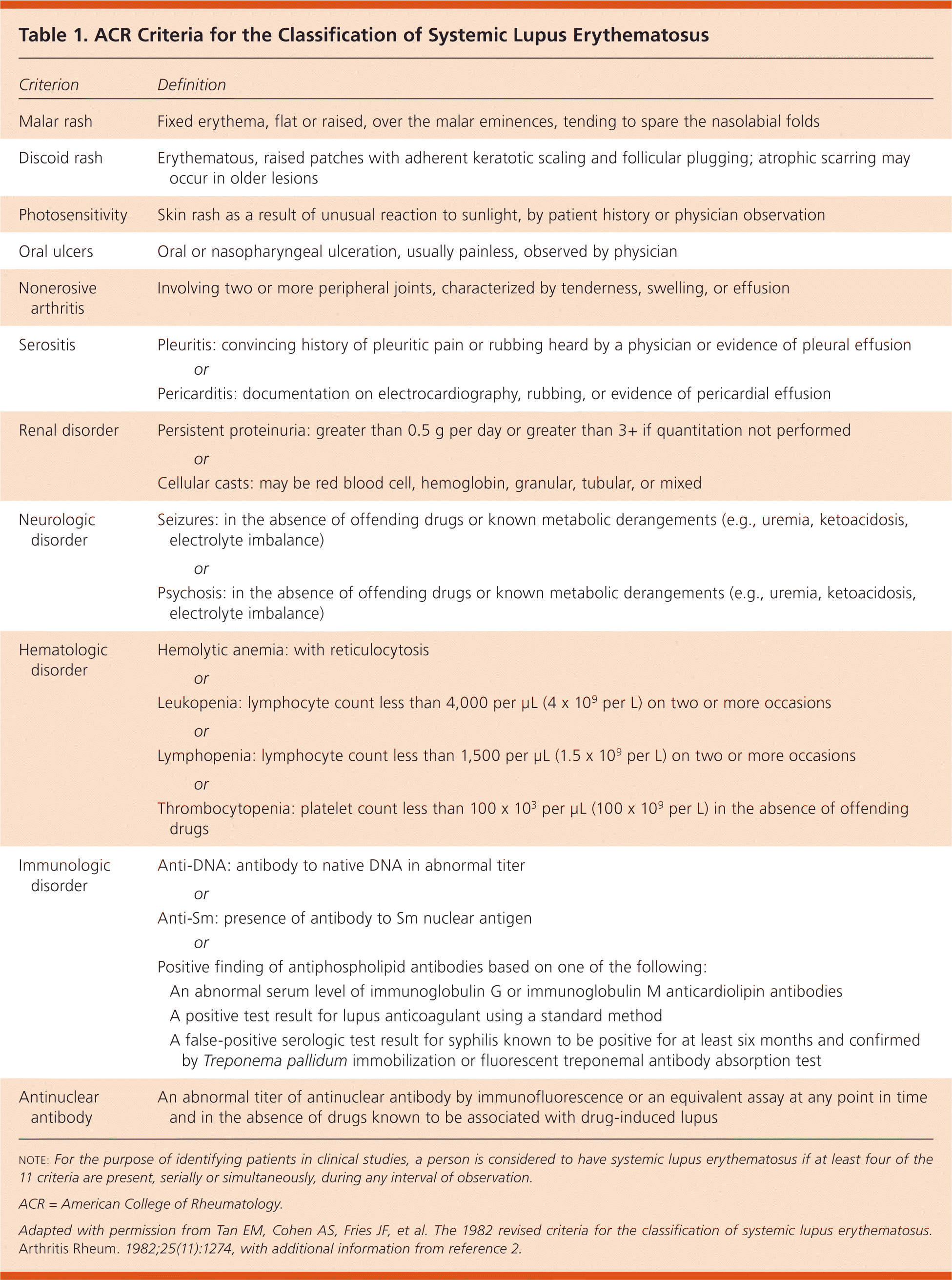
The diagnosis of SLE is made in patients who meet four of the 11 criteria outlined by the American College of Rheumatology (ACR).1,2 Table 1 shows the revised ACR classification criteria for SLE.1,2 Two of the criteria are the presence of antibodies (i.e., ANA and either antibody to DNA antigen [anti-DNA], antibody to Sm nuclear antigen [anti-Sm], or anticardiolipin antibody). Therefore, positive values on antibody tests can represent one-half of the criteria for a diagnosis of SLE.
Initial evaluation for suspected autoimmune disease often includes an ANA test, which is positive in 95 percent of patients with SLE.3 The ANA test has a false-negative rate of only 5 percent, but the specificity is low because many healthy patients and those with chronic liver disease, a neoplasm, or active infection also may have a positive test. Consequently, a positive ANA test result can be used only as part of the diagnosis.4–6 A prospective blind comparison of the sera of 213 patients in India was performed to determine the best screening dilution to distinguish between healthy persons and those with SLE.7 A dilution of 1:80 maximized the sensitivity and specificity. Using this standard, testing was positive for ANA in 95.3 percent of those with SLE and in 4.3 percent of those without SLE. This study was limited by age, sex, ethnicity, and environmental factors, which can affect ANA testing.
In patients with a suspected rheumatologic disorder, anti-DNA, anti-Sm, and antiphospholipid antibodies are more specific than ANA for diagnosing SLE. A retrospective study of 127 patients with various connective tissue disorders found elevated titers of anti-DNA antibody (82 percent), anti-Sm antibody (60 percent), and antiphospholipid antibody (62 percent) in the 50 patients with SLE who had an ANA titer of at least 1:128, but not in patients with other connective tissue disorders.8 In this study, 80 percent of all patients with SLE tested positive for at least two of three antibodies, whereas patients with other connective tissue disorders had no more than one positive test result.
The antichromatin antibody is under investigation as an additional marker for SLE. In a retrospective study of 78 patients with SLE, antichromatin antibody had a sensitivity of 64 percent and a specificity of 99 percent.9
Recommendations from Others
The ACR revised criteria for the classification of SLE have become the standard for categorizing SLE around the world.10 An alternative to the ACR classification is the Boston Weighted Criteria system. In one study, these criteria identified 190 of 271 patients with SLE, whereas the ACR criteria identified 171 of 271.11 The Boston Weighted Criteria have a sensitivity of 93 percent and a specificity of 69 percent for diagnosing SLE.11
Table 1. ACR Criteria for the Classification of Systemic Lupus Erythematosus
| Criterion | Definition | ||
|---|---|---|---|
| Malar rash | Fixed erythema, flat or raised, over the malar eminences, tending to spare the nasolabial folds | ||
| Discoid rash | Erythematous, raised patches with adherent keratotic scaling and follicular plugging; atrophic scarring may occur in older lesions | ||
| Photosensitivity | Skin rash as a result of unusual reaction to sunlight, by patient history or physician observation | ||
| Oral ulcers | Oral or nasopharyngeal ulceration, usually painless, observed by physician | ||
| Nonerosive arthritis | Involving two or more peripheral joints, characterized by tenderness, swelling, or effusion | ||
| Serositis | Pleuritis: convincing history of pleuritic pain or rubbing heard by a physician or evidence of pleural effusion | ||
| or | |||
| Pericarditis: documentation on electrocardiography, rubbing, or evidence of pericardial effusion | |||
| Renal disorder | Persistent proteinuria: greater than 0.5 g per day or greater than 3+ if quantitation not performed | ||
| or | |||
| Cellular casts: may be red blood cell, hemoglobin, granular, tubular, or mixed | |||
| Neurologic disorder | Seizures: in the absence of offending drugs or known metabolic derangements (e.g., uremia, ketoacidosis, electrolyte imbalance) | ||
| or | |||
| Psychosis: in the absence of offending drugs or known metabolic derangements (e.g., uremia, ketoacidosis, electrolyte imbalance) | |||
| Hematologic disorder | Hemolytic anemia: with reticulocytosis | ||
| or | |||
| Leukopenia: lymphocyte count less than 4,000 per μL (4 × 109 per L) on two or more occasions | |||
| or | |||
| Lymphopenia: lymphocyte count less than 1,500 per μL (1.5 × 109 per L) on two or more occasions | |||
| or | |||
| Thrombocytopenia: platelet count less than 100 × 103 per μL (100 × 109 per L) in the absence of offending drugs | |||
| Immunologic disorder | Anti-DNA: antibody to native DNA in abnormal titer | ||
| or | |||
| Anti-Sm: presence of antibody to Sm nuclear antigen | |||
| or | |||
| Positive finding of antiphospholipid antibodies based on one of the following: | |||
| An abnormal serum level of immunoglobulin G or immunoglobulin M anticardiolipin antibodies | |||
| A positive test result for lupus anticoagulant using a standard method | |||
| A false-positive serologic test result for syphilis known to be positive for at least six months and confirmed by Treponema pallidum immobilization or fluorescent treponemal antibody absorption test | |||
| Antinuclear antibody | An abnormal titer of antinuclear antibody by immunofluorescence or an equivalent assay at any point in time and in the absence of drugs known to be associated with drug-induced lupus | ||
note: For the purpose of identifying patients in clinical studies, a person is considered to have systemic lupus erythematosus if at least four of the 11 criteria are present, serially or simultaneously, during any interval of observation.
ACR = American College of Rheumatology.
Adapted with permission from Tan EM, Cohen AS, Fries JF, et al. The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum. 1982;25(11):1274, with additional information from reference2.

