
Am Fam Physician. 2012;85(12):1186-1187
Related letter: Does the HPV Vaccine Prevent Cervical Cancer?
Author disclosure: Dr. Wood has been reimbursed by Sanofi Pasteur, the manufacturer of Gardasil.
Worldwide, cervical cancer is the third most common cancer in women.
In the United Kingdom, the incidence of cervical cancer fell after the introduction of the cervical screening program to approximately 2,334 women in 2008, with a mortality-to-incidence ratio of 0.33.
About 80 percent of tumors are squamous type, and staging is based on the International Federation of Gynecology and Obstetrics (FIGO) classification.
Survival rates range from almost 100 percent five-year disease-free survival for treated stage Ia disease to 5 to 15 percent in stage IV disease. Survival is also influenced by tumor bulk, patient age, and comorbid conditions.
Development of cervical cancer is strongly associated with human papillomavirus (HPV) infection, acquired mainly by sexual intercourse.
The peak prevalence of HPV infection is 20 to 40 percent in women 20 to 30 years of age, but the infection resolves within 12 to 18 months in 80 percent of cases.
Other risk factors for cervical cancer include early onset of sexual activity, multiple sex partners, long-term use of oral contraceptives, tobacco smoking, low socioeconomic status, micronutrient deficiency, and immunosuppressive therapy.
Vaccination against HPV is effective in preventing certain types of oncogenic HPV infection and at reducing rates of cervical intraepithelial neoplasia, but there has been insufficient long-term follow-up to assess effects on cervical cancer rates.
Conization with adequate excision margins is considered effective for microinvasive carcinoma (stage Ia1) and can preserve fertility, unlike simple hysterectomy; however, it has been associated with an increased risk of preterm delivery and low birth weight.
Conization is often performed for stage Ia1 disease, but evidence for its benefit is from observational studies only.
We do not know how conization of the cervix with pelvic lymphadenectomy and simple or radical hysterectomy compare with each other for stage Ia2 and low volume stage Ib cervical cancer, as we found no randomized controlled trials (RCTs).
We do not know how simple hysterectomy plus lymphadenectomy and radical hysterectomy plus lymphadenectomy compare with each other in early cervical cancer, as we found no RCT evidence.
Limited observational evidence shows that radical trachelectomy plus lymphadenectomy results in similar disease-free survival as radical hysterectomy in women with early-stage cervical cancer; however, we found no RCTs.
Radical trachelectomy plus lymphadenectomy can preserve fertility.
Limited RCT evidence shows that radiotherapy is as effective as surgery in early-stage disease.
Overall and disease-free survival rates are similar after radiotherapy or radical hysterectomy plus lymphadenectomy, but radiotherapy is less likely to cause severe adverse effects.
Chemoradiotherapy improves survival compared with radiotherapy in women with bulky early-stage cervical cancer.
Combined chemoradiotherapy improves overall and progression-free survival when used either before or after hysterectomy, but is associated with more hematologic and gastrointestinal toxicity compared with radiotherapy alone.
The benefits of neoadjuvant chemotherapy plus surgery compared with radiotherapy alone are unknown.
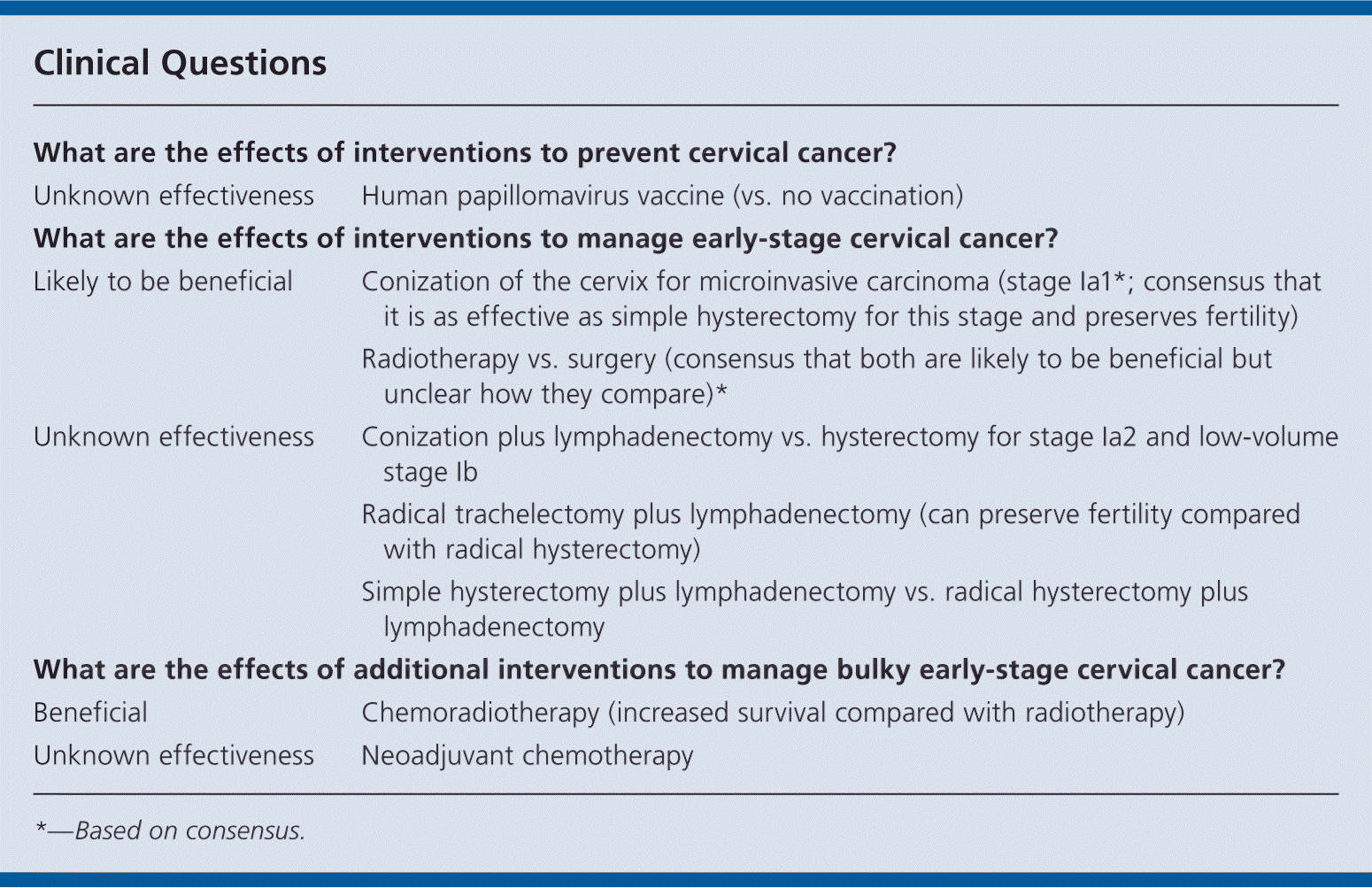
| What are the effects of interventions to prevent cervical cancer? | |
| Unknown effectiveness | Human papillomavirus vaccine (vs. no vaccination) |
| What are the effects of interventions to manage early-stage cervical cancer? | |
| Likely to be beneficial | Conization of the cervix for microinvasive carcinoma (stage Ia1*; consensus that it is as effective as simple hysterectomy for this stage and preserves fertility) |
| Radiotherapy vs. surgery (consensus that both are likely to be beneficial but unclear how they compare)* | |
| Unknown effectiveness | Conization plus lymphadenectomy vs. hysterectomy for stage Ia2 and low-volume stage Ib |
| Radical trachelectomy plus lymphadenectomy (can preserve fertility compared with radical hysterectomy) | |
| Simple hysterectomy plus lymphadenectomy vs. radical hysterectomy plus lymphadenectomy | |
| What are the effects of additional interventions to manage bulky early-stage cervical cancer? | |
| Beneficial | Chemoradiotherapy (increased survival compared with radiotherapy) |
| Unknown effectiveness | Neoadjuvant chemotherapy |
Definition
Cervical cancer is a malignant neoplasm arising from the uterine cervix. About 80 percent of cervical cancers are of the squamous type; the remainder are adenocarcinomas, adenosquamous carcinomas, and other rare types. Staging of cervical cancer is based on clinical evaluation. Management is determined by tumor bulk and stage.
This review deals with treatments for early-stage cancer (defined as FIGO stage Ia1, Ia2, Ib1, and small IIa tumors) and bulky early-stage disease (defined as FIGO stage Ib2 and larger IIa tumors).
Incidence and Prevalence
Cervical cancer is the third most common cancer in women, with about 529,000 new cases diagnosed worldwide in 2008. Most cases (85 percent) occur in resource-poor countries that have no effective screening programs. The incidence of cervical cancer in the United Kingdom and Europe has decreased greatly since the introduction of a screening program for detecting precancerous cervical intraepithelial neoplasia. Cervical cancer incidence fell by 42 percent between 1988 and 1997 in England and Wales. This decrease has been reported to be related to the cervical screening program. In England, cervical cancer had an annual incidence of 2,334 women in 2008, with a mortality-to-incidence ratio of 0.33.
Etiology and Risk Factors
Risk factors for cervical cancer include sexual intercourse at an early age, multiple sex partners, tobacco smoking, long-term oral contraceptive use, low socioeconomic status, immunosuppressive therapy, and micronutrient deficiency. Persistent infection by oncogenic, high-risk strains of HPV is strongly associated with the development of cervical cancer. HPV strains 16 and 18 cause about 70 percent of cervical cancers and high-grade cervical intraepithelial neoplasia. The virus is acquired mainly by sexual intercourse, and has a peak prevalence of 20 to 40 percent in women 20 to 30 years of age, although in 80 percent of cases the infection is transient and resolves within 12 to 18 months. Women with persistent oncogenic HPV are at risk of developing high-grade precancer and ultimately cervical cancer.
Prognosis
Overall, the five-year disease-free survival rate is 50 to 70 percent for stages Ib2 and IIb, 30 to 50 percent for stage III, and 5 to 15 percent for stage IV. In women who receive treatment, the five-year survival rate in stage Ia approaches 100 percent, falling to 70 to 85 percent for stage Ib1 and smaller IIa tumors. Survival in women with more locally advanced tumors is influenced by tumor bulk, the person's age, and coexistent medical conditions. Mortality in untreated, locally advanced disease is high.
editor's note: The FIGO classification for cervical cancer staging is available at http://www.cancer.gov/cancertopics/pdq/treatment/cervical/HealthProfessional/page3.
