A 38-year-old obese man presented with a large pedunculated lesion on his right lower abdomen. The lesion had been present for at least 10 years and had been gradually growing. He had a history of a right inguinal hernia repair, but it was not associated with the lesion. There was no history of trauma or infection to the area. He had no fever or weight loss.
Physical examination revealed a flesh-colored, pedunculated skin lesion on the right lower abdominal wall that was 3 × 3 × 4 cm in size, soft, mobile, and nontender (Figures 1 and 2). It was not reducible. There was no surrounding erythema or warmth, and no inguinal adenopathy. There were no other similar lesions or hyperpigmentation.
Figure 1.
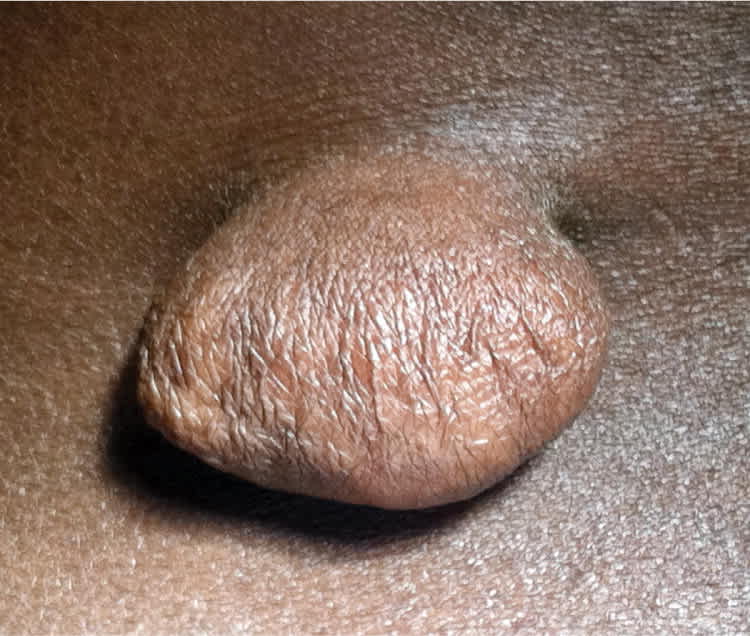
Figure 2.
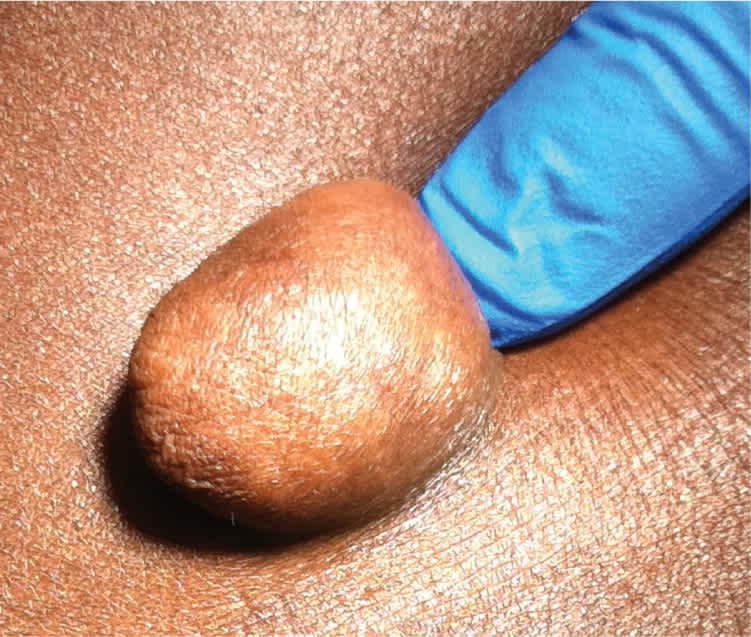
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Acrochordon.
B. Epidermal inclusion cyst.
C. Fibrokeratoma.
D. Lipoma.
E. Neurofibroma.
Discussion
The answer is A: Acrochordon. Acrochordons, commonly called skin tags, represent a hyperplastic epidermis that originates from both the ectoderm and mesoderm. About one-fourth of persons will get an acrochordon, and the number of acrochordons increases with age.1 Obesity is a common predisposing factor.2 The neck, axilla, and inguinal regions are most commonly affected. Acrochordons are generally connected to the skin by a stalk (peduncle), but they may also be sessile. They usually range from 1 mm to 1 cm in diameter, but can be larger. They are typically brown or flesh-colored, but may become red or black.
Acrochordons have no risk of malignancy, but often are treated because of irritation or cosmetic reasons. Sharp excision with scissors or scalpel at the base of the stalk is effective, although very small lesions can be treated with cryotherapy. Acrochordon recurrences are common. Specimens do not need to be sent for pathologic analysis unless the clinical diagnosis is uncertain or acrochordons were present in childhood, because this could be the initial presentation for nevoid basal cell carcinoma syndrome.3
Epidermal inclusion cysts are painless, elevated, round, firm cysts that most commonly occur on the back, face, and chest. They are filled with keratin and lined with stratified squamous epithelium, and are attached to the skin through a small, round, keratin-filled plug. They are slow growing and not pedunculated.
Fibrokeratoma is an acquired, benign skin lesion consisting of fibrous tissue. It generally occurs on the fingers; however, it can appear on the hands, toes, and soles. It appears as a skin-colored, dome-shaped papule or tall finger-like protrusion surrounded by a hyperkeratotic collar. It is hypothesized that these lesions arise as a response to subclinical trauma.4 They generally are not pedunculated.
Lipomas are benign, subcutaneous soft tissue tumors that are compressible and lobulated and composed of adipocytes. They typically occur on the trunk, shoulders, posterior neck, and axilla, but they are not tumors of the skin. Because they are subcutaneous, they never have a stalk.
Neurofibroma is a benign nerve sheath tumor in the peripheral nervous system that is composed of spindle cells. It can be associated with neurofibromatosis 1 or 2, and often presents as multiple lesions.5 Nodules can become large and pedunculated, and some may have overlaying hyperpigmentation. Neurofibromas are often accompanied by café au lait spots.
Summary Table
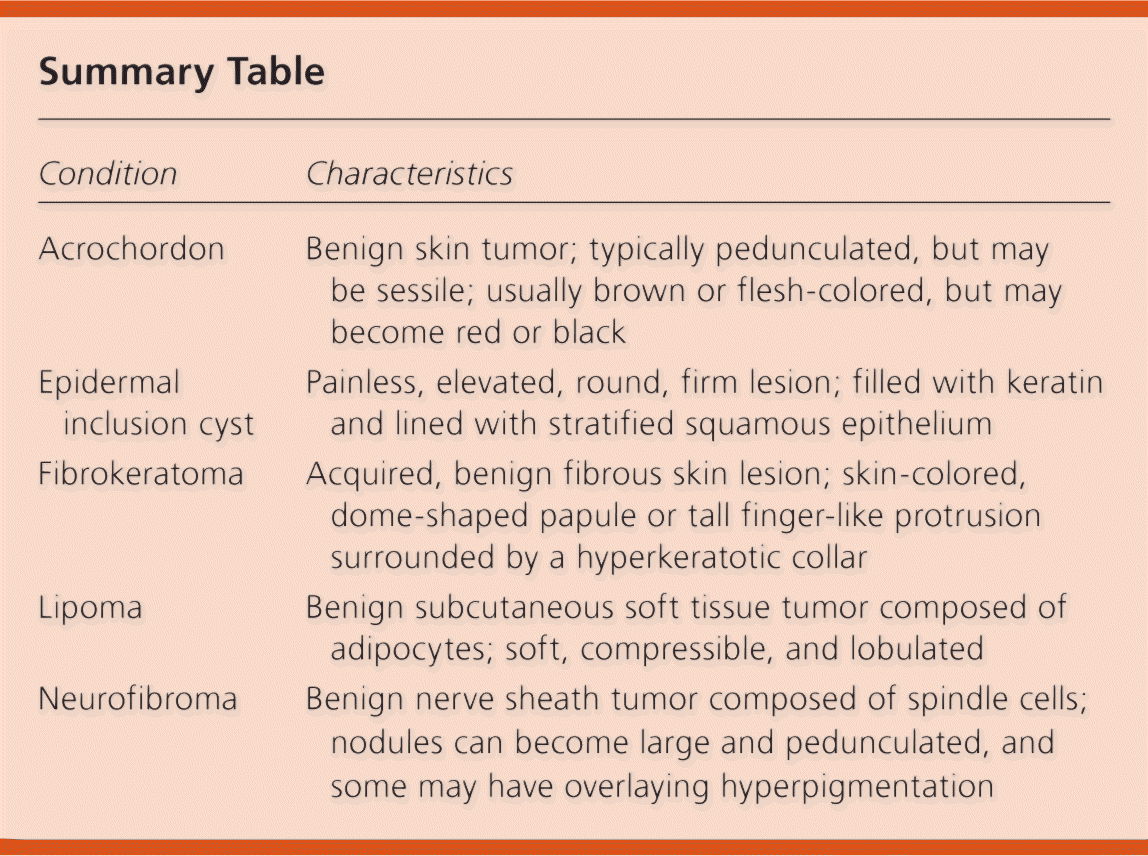
| Condition | Characteristics |
|---|---|
| Acrochordon | Benign skin tumor; typically pedunculated, but may be sessile; usually brown or flesh-colored, but may become red or black |
| Epidermal inclusion cyst | Painless, elevated, round, firm lesion; filled with keratin and lined with stratified squamous epithelium |
| Fibrokeratoma | Acquired, benign fibrous skin lesion; skin-colored, dome-shaped papule or tall finger-like protrusion surrounded by a hyperkeratotic collar |
| Lipoma | Benign subcutaneous soft tissue tumor composed of adipocytes; soft, compressible, and lobulated |
| Neurofibroma | Benign nerve sheath tumor composed of spindle cells; nodules can become large and pedunculated, and some may have overlaying hyperpigmentation |

