Major depressive disorder in children and adolescents is a common condition that affects physical, emotional, and social development. Risk factors include a family history of depression, parental conflict, poor peer relationships, deficits in coping skills, and negative thinking. Diagnostic criteria are the same for children and adults, with the exception that children and adolescents may express irritability rather than sad or depressed mood, and weight loss may be viewed in terms of failure to reach appropriate weight milestones. Treatment must take into account the severity of depression, suicidality, developmental stage, and environmental and social factors. Cognitive behavior therapy and interpersonal therapy are recommended for patients with mild depression and are appropriate adjuvant treatments to medication in those with moderate to severe depression. Pharmacotherapy is recommended for patients with moderate or severe depression. Tricyclic antidepressants are not effective in children and adolescents. Antidepressants have a boxed warning for the increased risk of suicide; therefore, careful assessment, follow-up, safety planning, and patient and family education should be included when treatment is initiated.
The prevalence of depression is estimated to be 2.8 percent in children younger than 13 years and 5.6 percent in adolescents 13 to 18 years of age.1 The incidence of depression among children and adolescents is of great concern because of the acute and lasting consequences associated with depressive disorders. Approximately 60 percent of adolescents with depression have recurrences throughout adulthood.2 Furthermore, adults with a history of adolescent depression have a higher rate of suicide than those without such a history.2 Adolescent-onset depression has been associated with abuse and neglect3; poor academic performance; substance use; early pregnancy; and disruptions in social, employment, and family settings into adulthood.4–6 Although the prevalence of adolescent depression is high, it is significantly underdiagnosed and undertreated.7 Because of the lack of mental health care professionals, family physicians are often responsible for detecting and treating childhood and adolescent depression.8–10
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Cognitive behavior therapy and interpersonal therapy should be used for the treatment of mild depression. Psychotherapy should be used in combination with medication for the treatment of moderate to severe depression in children and adolescents. | A | 36, 39, 40 | Meta-analysis,36 randomized controlled trials39,40 |
| Tricyclic antidepressants should not be used in the treatment of childhood and adolescent depression. | A | 46 | Cochrane review |
| Fluoxetine (Prozac), citalopram (Celexa), and sertraline (Zoloft) are recommended as first-line treatments for childhood and adolescent depression. | C | 47, 49, 50 | Consensus guidelines |
| Treatment of major depression in children and adolescents should continue for at least six months. | C | 51 | Consensus guideline |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Risk Factors
Although risk factors for childhood and adolescent depression can be categorized as biologic, psychologic, or environmental (Table 1), these factors are often intertwined.7,8,11,12 For example, parental depression is strongly associated with childhood and adolescent depression; children of parents with depression have a threefold greater risk of developing depression than those whose parents have no such history.13,14 Furthermore, the age when risk factors occur may predict future depression. Children diagnosed with a health condition such as diabetes mellitus or asthma between the ages of three and five years are likely to have a major depressive episode.12 Likewise, children five years of age who were rated by teachers as being hostile were at greater risk of depression.12
Table 1. Risk Factors for Depressive Disorders in Children and Adolescents

| Biologic |
| Family history of depression7,8 |
| Female sex11 |
| Hormonal changes during puberty11 |
| Low birth weight7 |
| Maternal age younger than 18 years7 |
| Medical illness (e.g., asthma, diabetes mellitus, migraines)7 |
| Obesity11 |
| Other psychological disorders (e.g., anxiety, learning disorders)11,12 |
| Sleep disruptions11 |
| Psychological |
| Emotional dependence12 |
| History of suicide attempts11,12 |
| Ineffective coping skills11,12 |
| Low self-esteem11,12 |
| Negative body image12 |
| Negative thinking styles (e.g., “Things like this always happen to me,” “Nothing will ever go as planned”)11,12 |
| Self-consciousness12 |
| Environmental |
| Antisocial peer group11 |
| Decreased physical activity11 |
| Increased parental conflict8,12 |
| Loss of relationship (e.g., death of family member or friend, romantic relationship, friendship)8,12 |
| Low socioeconomic status7,8 |
| Overeating11 |
| Poor academic performance11,12 |
| Poor peer relationships8,12 |
| Substance use11 |
| Traumatic event (e.g., physical or sexual abuse, accident)8 |
Screening
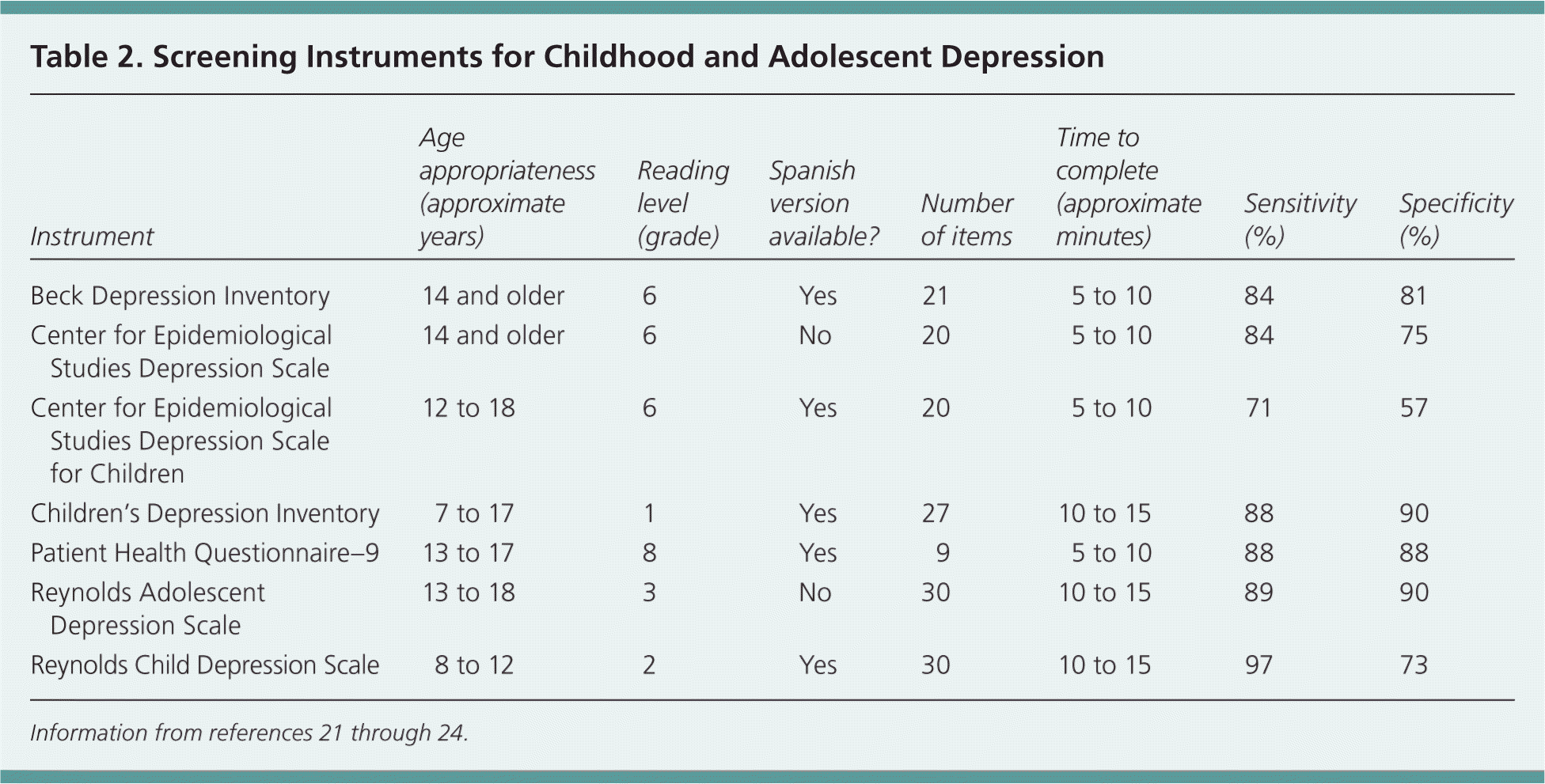
The U.S. Preventive Services Task Force concluded that screening adolescents 12 to 18 years of age may lead to earlier detection and treatment of depression.15 There was insufficient evidence to recommended routine screening for younger children in primary care settings. The use of screening tools in children with at least one risk factor may be more helpful than universal screening. These tools can also indicate the severity of depressive symptoms. Screening tools include the Beck Depression Inventory for Primary Care for adolescents 12 to 18 years of age, and the Children's Depression Inventory for children and adolescents seven to 17 years of age.16,17 The Beck Depression Inventory for Primary Care is a self-report tool that includes seven questions that are scored from zero to three points each (Figure 1).17,18 A score of at least 4 warrants further evaluation for depression.19 The Children's Depression Inventory is available in self-report, parent-report, and teacher-report versions; scores are converted to a T-score, with scores of 65 or more indicating clinical significance.20 Additional screening tools are described in Table 2.21–24 Screening tools should be selected based on patient's age, reading level, and time available to complete the measures.
Figure 1. Patient Self-Evaluation

Beck Depression Inventory for Primary Care.
Information from references 17 and 18.
Table 2. Screening Instruments for Childhood and Adolescent Depression
| Instrument | Age appropriateness (approximate years) | Reading level (grade) | Spanish version available? | Number of items | Time to complete (approximate minutes) | Sensitivity (%) | Specificity (%) |
|---|---|---|---|---|---|---|---|
| Beck Depression Inventory | 14 and older | 6 | Yes | 21 | 5 to 10 | 84 | 81 |
| Center for Epidemiological Studies Depression Scale | 14 and older | 6 | No | 20 | 5 to 10 | 84 | 75 |
| Center for Epidemiological Studies Depression Scale for Children | 12 to 18 | 6 | Yes | 20 | 5 to 10 | 71 | 57 |
| Children's Depression Inventory | 7 to 17 | 1 | Yes | 27 | 10 to 15 | 88 | 90 |
| Patient Health Questionnaire–9 | 13 to 17 | 8 | Yes | 9 | 5 to 10 | 88 | 88 |
| Reynolds Adolescent Depression Scale | 13 to 18 | 3 | No | 30 | 10 to 15 | 89 | 90 |
| Reynolds Child Depression Scale | 8 to 12 | 2 | Yes | 30 | 10 to 15 | 97 | 73 |
Presentation
Although diagnostic criteria for depression are the same for children and adults (Table 325 ), the manner in which these symptoms present may be different.25 Adolescents with depression are more likely to experience anhedonia, boredom, hopelessness, hypersomnia, weight change (including failure to reach appropriate weight milestones), alcohol or drug use, and suicide attempts. Younger children are more likely to have somatic symptoms, restlessness, separation anxiety, phobias, and hallucinations.26 The child's cognitive level should be considered; for example, younger children may appear sad but have difficulty verbalizing their mood.27 Differences have been found between parent reports and self-reports of depressive symptoms. Parents are more likely to indicate externalized symptoms such as irritability, whereas children are more likely to report internalized symptoms such as depressed mood.8
Table 3. Criteria for Major Depressive Episode in Adults, Children, and Adolescents

| A. Five (or more) of the following symptoms have been present during the same two-week period and represent a change from previous functioning; at least one of the symptoms is (1) depressed mood or (2) loss of interest or pleasure | |
| (1) Depressed mood most of the day, nearly every day, as indicated by subjective report (e.g., feels sad or empty) or observation made by others (e.g., appears tearful) | |
| (2) Markedly diminished interest or pleasure in all or almost all activities most of the day, nearly every day (as indicated by subjective account or observation made by others) | |
| (3) Significant weight loss when not dieting, or weight gain (e.g., a change of more than 5 percent of body weight in one month), or decrease or increase in appetite nearly every day | |
| (4) Insomnia or hypersomnia nearly every day | |
| (5) Psychomotor agitation or retardation nearly every day (observable by others, not merely subjective feeling of restlessness or being slowed down) | |
| (6) Fatigue or loss of energy nearly every day | |
| (7) Feeling of worthlessness or excessive or inappropriate guilt (which may be delusional) nearly every day (not merely self-reproach or guilt about being sick) | |
| (8) Diminished ability to think or concentrate, or indecisiveness, nearly every day (by subjective account or as observed by others) | |
| (9) Recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan, or a suicide attempt or a specific plan for committing suicide | |
| B. Symptoms do not meet the criteria for mixed bipolar disorder | |
| C. Symptoms cause clinically significant distress or impairment in social, occupational, or other important areas of functioning | |
| D. Symptoms are not caused by the direct physiologic effects of a substance (e.g., drug of abuse, medication) or a general medical condition (e.g., hypothyroidism) | |
| E. Symptoms are not caused by bereavement (i.e., after the loss of a loved one, the symptoms persist for longer than two months or are characterized by marked functional impairment, morbid preoccupation with worthlessness, suicidal ideation, psychotic symptoms, or psychomotor retardation) | |
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders . 4th ed., text rev. Copyright © 2000. Washington, DC: American Psychiatric Association; 2000:356.
Diagnosis
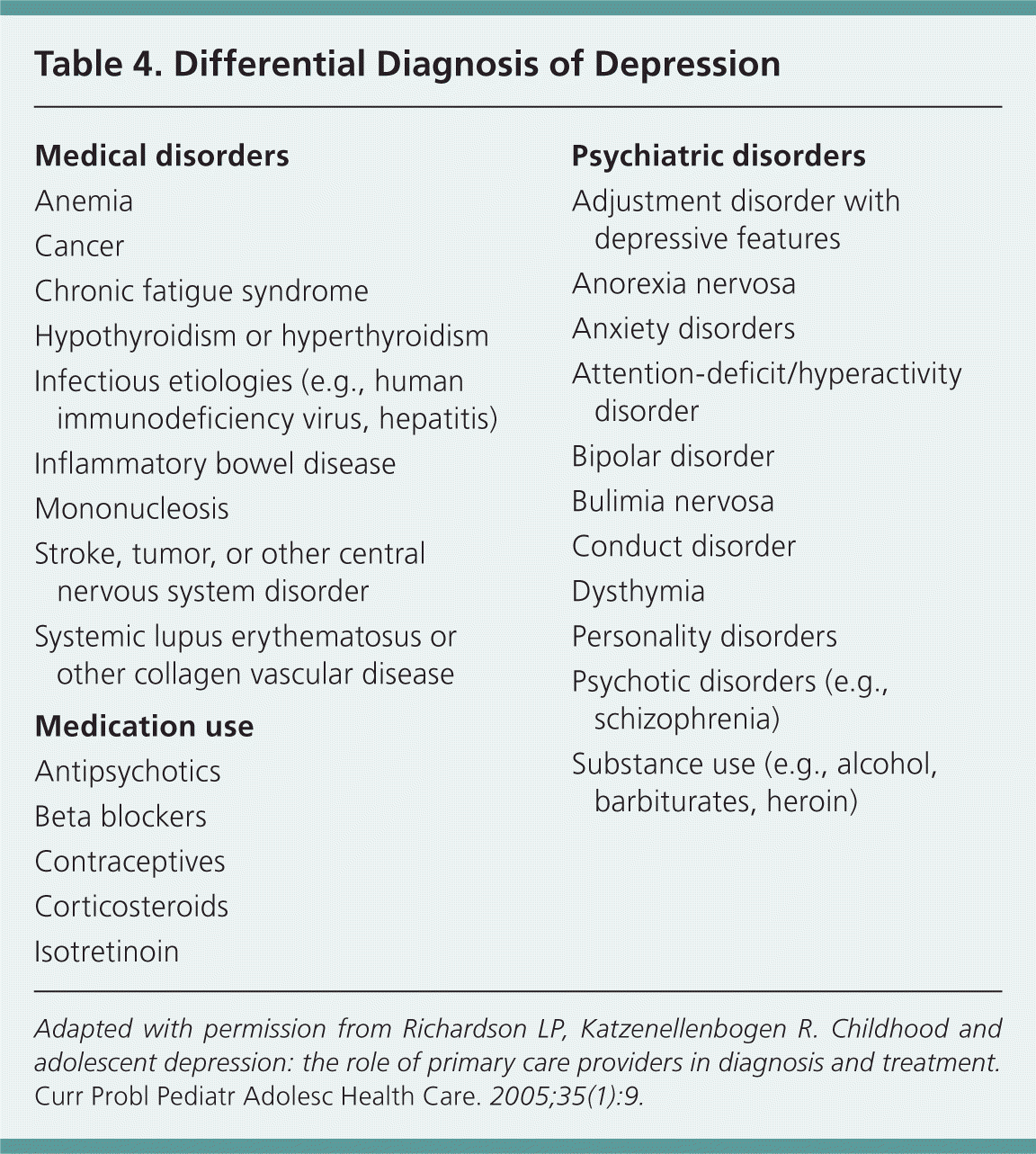
When considering a diagnosis of depression, physicians must also consider likely medical causes of the presenting symptoms, such as hyper- or hypothyroidism, anemia, or use of certain medications, including isotretinoin (Table 4).8 If the patient's mood is better explained by medical causes, the diagnosis of major depressive disorder is not appropriate.25
Table 4. Differential Diagnosis of Depression
| Medical disorders |
| Anemia |
| Cancer |
| Chronic fatigue syndrome |
| Hypothyroidism or hyperthyroidism |
| Infectious etiologies (e.g., human immunodeficiency virus, hepatitis) |
| Inflammatory bowel disease |
| Mononucleosis |
| Stroke, tumor, or other central nervous system disorder |
| Systemic lupus erythematosus or other collagen vascular disease |
| Medication use |
| Antipsychotics |
| Beta blockers |
| Contraceptives |
| Corticosteroids |
| Isotretinoin |
| Psychiatric disorders |
| Adjustment disorder with depressive features |
| Anorexia nervosa |
| Anxiety disorders |
| Attention-deficit/hyperactivity disorder |
| Bipolar disorder |
| Bulimia nervosa |
| Conduct disorder |
| Dysthymia |
| Personality disorders |
| Psychotic disorders (e.g., schizophrenia) |
| Substance use (e.g., alcohol, barbiturates, heroin) |
Adapted with permission from Richardson LP, Katzenellenbogen R. Childhood and adolescent depression: the role of primary care providers in diagnosis and treatment. Curr Probl Pediatr Adolesc Health Care. 2005;35(1):9.
Other psychological illnesses have presentations in children and adolescents that are similar to depression, especially adjustment, dysthymic, and bipolar disorders. Adjustment disorders are characterized by “a psychological response to an identifiable stressor or stressors.”25 Symptoms develop within three months of the stressor and are in excess of what would be expected, or they cause significant impairment. Adjustment disorder with depressed mood can be mistaken for major depressive disorder; symptoms of both conditions include depressed mood, tearfulness, and feelings of hopelessness. However, the symptoms of adjustment disorder are related to a specific event and do not meet all criteria of a major depressive episode.25
Dysthymic disorder in children and adolescents is characterized by depressed mood on most days for one year. Patients with dysthymia meet a subset of criteria for major depression, but the course of the illness is longer and the symptoms are less severe. Depressive symptoms may manifest as irritability in children and adolescents, and patients often have low self-esteem and poor social skills.
Bipolar disorder consists of periods of major depression alternating with mania or hypomania, during which patients have increased irritability, energy, grandiosity, and/or racing thoughts. It is important to rule out bipolar disorder when diagnosing depression, because antidepressant medications can initiate manic symptoms.
Risk Assessment for Suicide
The presence of a psychiatric disorder is one of the strongest correlates for suicide across age groups.28 According to the Centers for Disease Control and Prevention, the incidence of suicide in children 10 to 14 years of age was approximately 0.9 per 100,000 in 2007, and the incidence in adolescents 15 to 19 years of age was 6.9 per 100,000.29 The methods by which suicide was completed include firearms, suffocation, and poisoning; children most often use suffocation, whereas adolescents are more likely to use firearms.29 Therefore, routine and ongoing assessment of suicidality in children and adolescents with depression is recommended, especially in patients who are receiving antidepressant medication.30,31
Asking about suicide or using depression screening tools can be a means for assessing suicidal ideation in children and adolescents in the primary care setting. However, further inquiry into patient symptoms may be required because some tools lack specificity or are prone to oversensitivity. If a patient has suicidal thoughts, further assessment should include questions about the frequency of thoughts; the presence and specificity of a plan; the lethality or availability of means to follow through with the plan; whether there are protective factors, such as social support; and whether there are any other factors, such as substance use or a previous suicide attempt. If it is determined that a patient is at risk of self-harm, urgent referral to a mental health professional or emergency department is warranted.
Interventions for patients at lower risk of self-harm include involving parents or caregivers to provide close observation of the patient, and removing any weapons or means to self-harm. The frequency of follow-up visits may be increased, and patients may benefit from education on how to seek assistance after hours (e.g., emergency departments, crisis hotlines).8,30–32 Parents and family members should be educated about behaviors that would warrant immediate follow-up, such as increased suicidal ideation, impulsivity, irritability, restlessness, pressured speech, or psychomotor agitation.31,33
Treatment
Treatment of childhood and adolescent depression consists of psychotherapy, pharmacotherapy, or a combination of these. Treatment should correspond to the level of depression, patient preferences, the developmental level of the patient, associated risk factors, and availability of services.8 Patient and family education about the associated risks and benefits of treatment, expectations regarding patient monitoring, and follow-up should be included.33
PSYCHOTHERAPY
The American Psychiatric Association and the American Academy of Child and Adolescent Psychiatry recommend that psychotherapy always be a component of treatment for childhood and adolescent depression.33 They recommend psychotherapy as an acceptable treatment option for patients with milder depression, and a combination of medication and psychotherapy in those with moderate to severe depression.
Cognitive behavior therapy (CBT) and interpersonal therapy have been proven effective in the treatment of adolescent depression, and CBT has been proven effective in the treatment of childhood depression. CBT usually consists of behavioral activation techniques and methods to increase coping skills, improve communication skills and peer relationships, solve problems, combat negative thinking patterns, and regulate emotions.8,34–36 In contrast, interpersonal therapy generally focuses on adapting to changes in relationships, transitioning personal roles, and forming interpersonal relationships.8,36 The effects of CBT on depressive symptoms are moderate,37,38 but it has not been proven more effective than placebo for treating acute depression in adolescents.39 A combination of CBT and medication has been shown to be more effective than medication alone in attaining remission of depression.37,40 Interpersonal therapy has not been compared with medication, combination treatment, or placebo, but it has been proven more effective than wait-list control groups with no therapy, and as effective or more effective than CBT.41,42
PHARMACOTHERAPY
Although psychotherapy is a major component in the treatment of childhood and adolescent depression, adjuvant use of medication is sometimes appropriate. Considerations for initiating antidepressant therapy include depression severity and history (Table 5).43,44 Extrapolation of adult data on antidepressant medications to children and adolescents may not be accurate, because neural pathways may not be fully developed, and serotonin and norepinephrine systems have different maturation rates.45
Table 5. Questions to Guide Initiation of Pharmacotherapy in Children and Adolescents with Depression

| Is the depression of moderate to severe severity? |
| Has there been a prior episode of depression? |
| Has the patient been treated for depression with medication in the past? |
| Is there a family history of depression? |
| Is there a family history of depression with significant response to medication? |
| Have environmental stressors been modified with no associated improvements in mood? |
| Has evidence-based psychotherapy (i.e., cognitive behavior therapy, interpersonal therapy) been attempted without success? |
note: If the patient answers “yes” to any question, consider initiating pharmacotherapy.
Tricyclic antidepressants were previously used to treat depression in children, but studies have shown little to no benefit in adolescents and children.46 Consensus guidelines recommend fluoxetine (Prozac), citalopram (Celexa), and sertraline (Zoloft) as first-line treatments for moderate to severe depression in children and adolescents.47 A Cochrane review found that fluoxetine was the only agent with consistent evidence (from three randomized trials) that it is effective in decreasing depressive symptoms.48 Escitalopram (Lexapro) is also licensed for the treatment of depression in adolescents 12 years and older. Treatment should begin at the lowest dosage available and titrated according to the patient's response and adverse effects. If initial first-line therapy is ineffective, another first-line agent should be considered. All antidepressants have a boxed warning for an increased risk of suicide; therefore, close monitoring is recommended (e.g., weekly telephone calls, scheduled visits for the first month of therapy) to assess for suicidality and other adverse effects, such as gastrointestinal effects, nervousness, headache, and restlessness.47,49 If there is limited improvement or no remission of symptoms after all first-line medications have been attempted, a psychiatric consultation is strongly recommended.50
Treatment Duration and Referral
Treatment of depression in children and adolescents should continue for six months after remission.49,51 A double-blind, placebo-controlled trial of adolescents receiving fluoxetine found that those who received placebo after treatment had a shorter time to relapse than those who continued therapy.52 Patients in the fluoxetine group were significantly less likely to have a relapse of depressive symptoms (34 versus 60 percent). The decision to continue treatment for four to six months after remission of symptoms should be based on prior recurrent episodes of depression and current psychological and social stressors. Children younger than 11 years and those with chronic depression, comorbid substance use, psychiatric disorders, suicidality with plan, or lack of parental engagement in treatment should be referred to a psychiatrist.44,52
Data Sources: We searched Essential Evidence Plus, the Agency for Healthcare Research and Quality evidence reports, the Cochrane Database of Systematic Reviews, Clinical Evidence, the National Guideline Clearinghouse, the U.S. Preventive Services Task Force, PubMed, Ovid Medline, and PsycINFO using the keywords childhood and adolescent depression, major depression and adolescents, major depression and childhood, major depression and children, depression and children, and depression and adolescents. The search included reviews, meta-analyses, randomized controlled trials, and clinical trials. Search dates: March 5 and 11, 2011.

