Guideline source: American College of Physicians
Evidence rating system used? Yes
Literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Published source:Annals of Internal Medicine, February 2012
Available at: http://annals.org/article.aspx?volume=156&page=218
Endorsed by the AAFP, May 2013. https://www.aafp.org/patient-care/clinical-recommendations/all/endorsed.html
Diabetes mellitus is the seventh leading cause of death in the United States. The most common form is type 2, which affects about 25.8 million Americans. Type 2 diabetes increases with age—nearly 27 percent of U.S. adults older than 65 years have the disease. In 2007, the costs associated with diabetes reached $174 billion in the United States. Most persons diagnosed with diabetes take more than one class of medication to treat complications such as hyperglycemia and retinopathy; 58 percent take only oral medications, and 14 percent take oral medications and insulin.
The American College of Physicians (ACP) has published an updated guideline on the oral pharmacologic management of type 2 diabetes. Recommendations are based on a systematic evidence review of head-to-head comparisons of oral pharmacologic treatments for type 2 diabetes, and an evidence report sponsored by the Agency for Healthcare Research and Quality.
Recommendations
When lifestyle modifications, including diet, exercise, and weight loss, do not adequately improve hyperglycemia in patients diagnosed with type 2 diabetes, physicians should add oral pharmacologic therapy.
Initiating oral pharmacologic therapy is important for managing type 2 diabetes effectively. Because there are no data on the best time to add oral therapies to lifestyle modifications, other factors such as the patient's life expectancy and preferred method of receiving medications, the presence or absence of microvascular and macrovascular complications, and the risk of adverse events related to glucose control should be considered to avoid placing an unacceptable burden on the patient. An A1C level less than 7 percent based on individualized assessment is a reasonable goal for many, but not all, patients. The A1C goal should be set after assessing risk of comorbidity, complications from diabetes, life expectancy, and patient preferences.
Physicians should prescribe metformin (Glucophage) as the initial pharmacologic therapy to treat most patients with type 2 diabetes.
Unless contraindicated, metformin is considered the preferred choice for patients with type 2 diabetes. Evidence shows that metformin is the most effective pharmacologic agent as monotherapy and in combination with other medications. It is more effective than other pharmacologic agents in reducing glycemic, low-density lipoprotein cholesterol, and triglyceride levels, and it does not cause weight gain. Metformin has been associated with slightly lower all-cause mortality and cardiovascular mortality compared with sulfonylureas. In addition, it is associated with fewer hypoglycemic episodes, and is less expensive than other pharmacologic agents.
Metformin is contraindicated in patients with impaired kidney function, decreased tissue perfusion or hemodynamic instability, liver disease, alcohol abuse, heart failure, and any condition that may lead to lactic acidosis. It is also associated with an increased risk of adverse gastrointestinal effects.
Other diabetes medications may also cause adverse effects. Sulfonylureas and meglitinides are associated with an increased risk of hypoglycemia. Thiazolidinediones are associated with an increased risk of heart failure, but there is no conclusive evidence that they increase ischemic cardiovascular risk. Physicians and patients should discuss adverse events before selecting a medication regimen.
When lifestyle modifications and monotherapy do not adequately control hyperglycemia, physicians should add a second agent to metformin to treat patients with persistent hyperglycemia.
All dual-therapy regimens reviewed by the ACP were more effective than monotherapies in reducing A1C levels by approximately one additional percentage point. Although some evidence suggests that the combination of metformin and another agent tends to be more effective than any other monotherapy or combination therapy, there is no good evidence to support one particular combination therapy over another.
Combination therapies are associated with an increased risk of adverse effects compared with mono-therapy. Although generic sulfonylureas are the least expensive second-line therapy, evidence suggests that adverse effects are generally worse with combination therapies that include a sulfonylurea. Some patients with persistent hyperglycemia may also need insulin therapy.
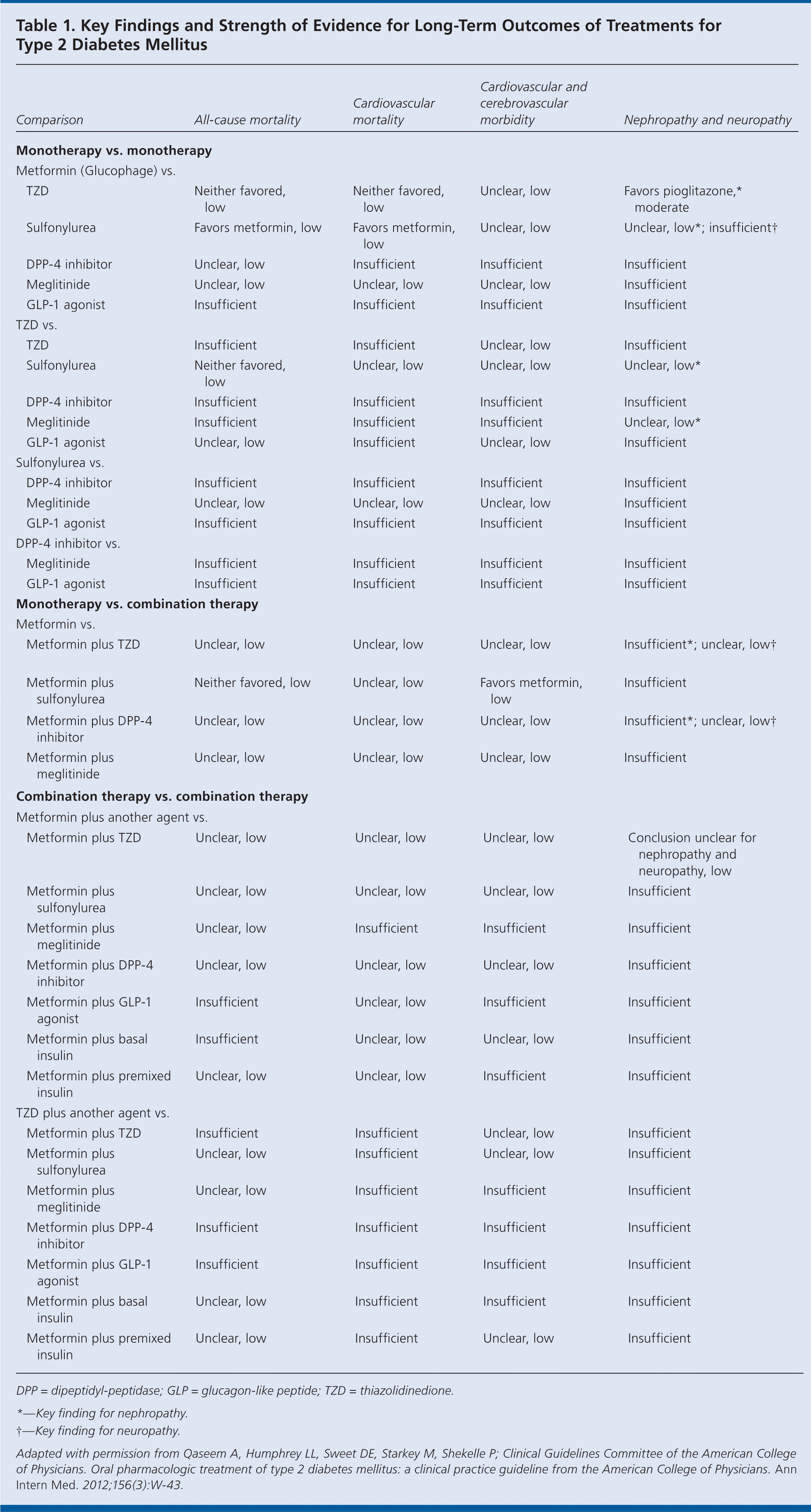
A comparison of pharmacologic therapies for the treatment of diabetes is included in Table 1.
Table 1. Key Findings and Strength of Evidence for Long-Term Outcomes of Treatments for Type 2 Diabetes Mellitus
| Comparison | All-cause mortality | Cardiovascular mortality | Cardiovascular and cerebrovascular morbidity | Nephropathy and neuropathy | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Monotherapy vs. monotherapy | |||||||||||
| Metformin (Glucophage) vs. | |||||||||||
| TZD | Neither favored, low | Neither favored, low | Unclear, low | Favors pioglitazone,* moderate | |||||||
| Sulfonylurea | Favors metformin, low | Favors metformin, low | Unclear, low | Unclear, low*; insufficient† | |||||||
| DPP-4 inhibitor | Unclear, low | Insufficient | Insufficient | Insufficient | |||||||
| Meglitinide | Unclear, low | Unclear, low | Unclear, low | Insufficient | |||||||
| GLP-1 agonist | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| TZD vs. | |||||||||||
| TZD | Insufficient | Insufficient | Unclear, low | Insufficient | |||||||
| Sulfonylurea | Neither favored, low | Unclear, low | Unclear, low | Unclear, low* | |||||||
| DPP-4 inhibitor | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| Meglitinide | Insufficient | Insufficient | Insufficient | Unclear, low* | |||||||
| GLP-1 agonist | Unclear, low | Insufficient | Unclear, low | Insufficient | |||||||
| Sulfonylurea vs. | |||||||||||
| DPP-4 inhibitor | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| Meglitinide | Unclear, low | Unclear, low | Unclear, low | Insufficient | |||||||
| GLP-1 agonist | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| DPP-4 inhibitor vs. | |||||||||||
| Meglitinide | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| GLP-1 agonist | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| Monotherapy vs. combination therapy | |||||||||||
| Metformin vs. | |||||||||||
| Metformin plus TZD | Unclear, low | Unclear, low | Unclear, low | Insufficient*; unclear, low† | |||||||
| Metformin plus sulfonylurea | Neither favored, low | Unclear, low | Favors metformin, low | Insufficient | |||||||
| Metformin plus DPP-4 inhibitor | Unclear, low | Unclear, low | Unclear, low | Insufficient*; unclear, low† | |||||||
| Metformin plus meglitinide | Unclear, low | Unclear, low | Unclear, low | Insufficient | |||||||
| Combination therapy vs. combination therapy | |||||||||||
| Metformin plus another agent vs. | |||||||||||
| Metformin plus TZD | Unclear, low | Unclear, low | Unclear, low | Conclusion unclear for nephropathy and neuropathy, low | |||||||
| Metformin plus sulfonylurea | Unclear, low | Unclear, low | Unclear, low | Insufficient | |||||||
| Metformin plus meglitinide | Unclear, low | Insufficient | Insufficient | Insufficient | |||||||
| Metformin plus DPP-4 inhibitor | Unclear, low | Unclear, low | Unclear, low | Insufficient | |||||||
| Metformin plus GLP-1 agonist | Insufficient | Unclear, low | Insufficient | Insufficient | |||||||
| Metformin plus basal insulin | Insufficient | Unclear, low | Unclear, low | Insufficient | |||||||
| Metformin plus premixed insulin | Unclear, low | Unclear, low | Insufficient | Insufficient | |||||||
| TZD plus another agent vs. | |||||||||||
| Metformin plus TZD | Insufficient | Insufficient | Unclear, low | Insufficient | |||||||
| Metformin plus sulfonylurea | Unclear, low | Insufficient | Unclear, low | Insufficient | |||||||
| Metformin plus meglitinide | Unclear, low | Insufficient | Insufficient | Insufficient | |||||||
| Metformin plus DPP-4 inhibitor | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| Metformin plus GLP-1 agonist | Insufficient | Insufficient | Insufficient | Insufficient | |||||||
| Metformin plus basal insulin | Unclear, low | Insufficient | Insufficient | Insufficient | |||||||
| Metformin plus premixed insulin | Unclear, low | Insufficient | Unclear, low | Insufficient | |||||||
DPP = dipeptidyl-peptidase; GLP = glucagon-like peptide; TZD = thiazolidinedione.
*—Key finding for nephropathy.
†—Key finding for neuropathy.
Adapted with permission from Qaseem A, Humphrey LL, Sweet DE, Starkey M, Shekelle P; Clinical Guidelines Committee of the American College of Physicians. Oral pharmacologic treatment of type 2 diabetes mellitus: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2012;156(3):W-43.

