Case Scenario
An 86-year-old woman with significant hearing loss presents for a follow-up visit for diabetes mellitus. She is also increasingly forgetful and needs assistance with her daily care, including insulin injections. Her husband is having trouble managing her diabetes and her daily needs. He recognizes the need for further assistance, but they have been unsuccessful in obtaining daily home health aide or nursing service coverage through their health insurance. They are unable to afford the assistance out of pocket. He reluctantly accepts help from a social worker to facilitate placement of his wife in a nursing home.
Nearly two months later, the husband returns for his own medical appointment. He appears depressed. On further questioning, he adds that his wife's health is deteriorating rapidly. He feels that she is socially isolated during the times he is not at the nursing home. She does not have any friends at the home, and eats some meals by herself because of difficulties communicating with others. The husband also believes that because of a previous miscommunication with the nursing home staff, she was sent to the local emergency room for possible delirium. He is afraid that he made a poor choice by placing his wife in the nursing facility.
Commentary
This scenario illustrates issues related to end-of-life care and placement in a long-term care facility for older individuals with significant hearing loss. An analysis of data from the 1999 to 2006 cycles of the National Health and Nutrition Examination Survey, and statistics from the National Institute on Deafness and Other Communication Disorders, indicate that 26.7 percent of persons 50 years and older (including 30 percent of persons 65 to 74 years of age, and 47 percent of persons 75 years and older) struggle with hearing loss.1,2 Hearing loss can result in a number of adverse outcomes, including social isolation, depression, lower self-esteem, poorer quality of life, decreased functional status, and dementia.3,4 Addressing these issues, as well as cognitive testing difficulties, poor health knowledge, and limited health care communication, presents a set of unique challenges for family physicians who care for patients who are deaf or hard of hearing.
BREAKDOWNS IN COMMUNICATION
Older patients who are deaf or hard of hearing are at high risk of breakdowns in health care communication. To reduce this risk, family physicians must be cognizant of patients' communication and language needs. These patients should be identified by an easy-to-recognize sign or flag in the medical record to remind physicians and staff members of the need for potential accommodations. Individuals with significant hearing loss are heterogeneous in their degree of hearing loss, language and communication needs, and perceptions of their disabilities. Physicians should avoid assuming what these patients may require, and ask them directly about their needs and preferences. A variety of strategies and accommodations are available for improving communication with this population (Table 1).
Table 1. Strategies for Treating Older Patients Who Are Deaf or Hard of Hearing
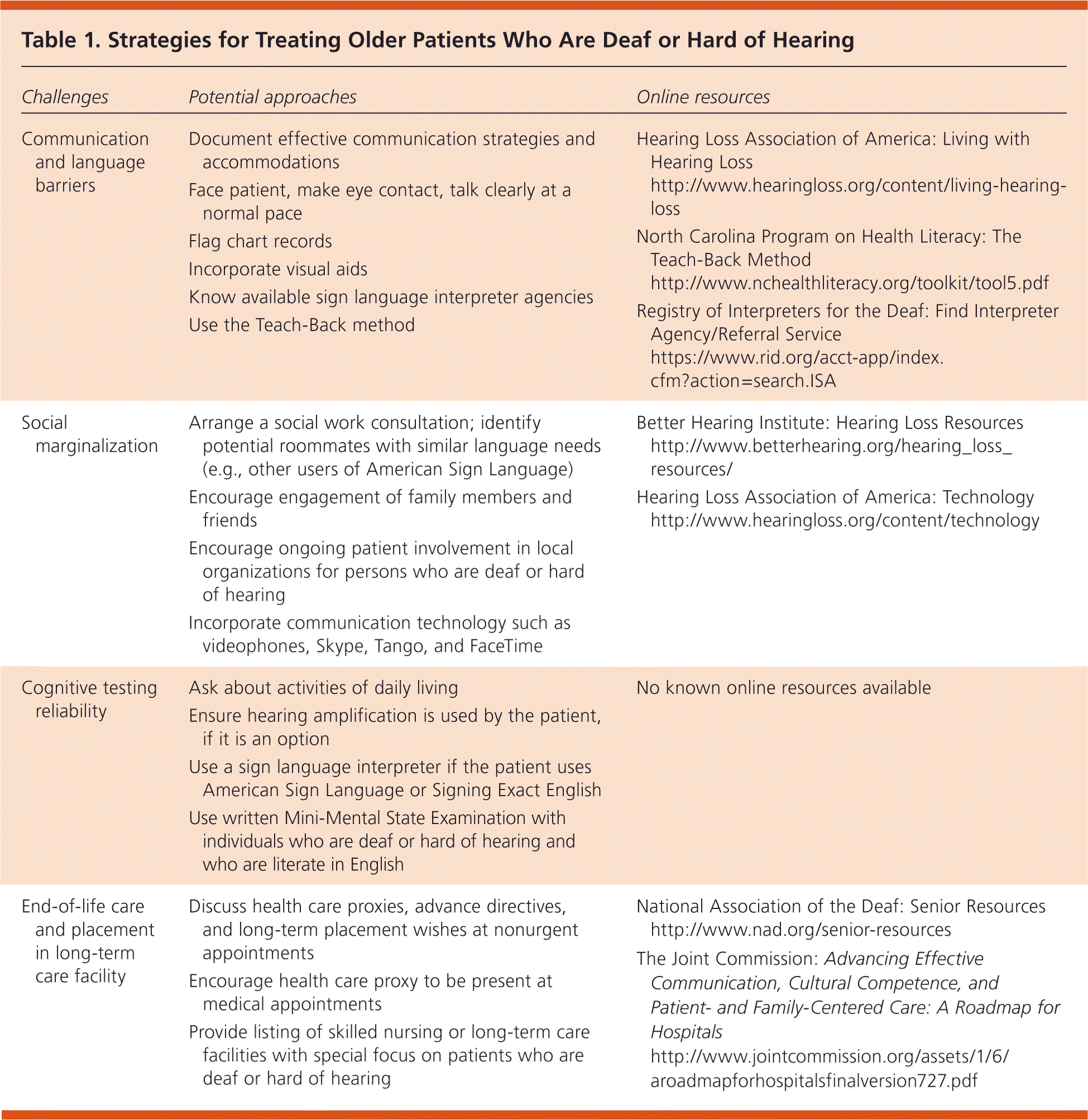
| Challenges | Potential approaches | Online resources | |
|---|---|---|---|
| Communication and language barriers |
| Hearing Loss Association of America: Living with Hearing Loss North Carolina Program on Health Literacy: The Teach-Back Method Registry of Interpreters for the Deaf: Find Interpreter Agency/Referral Service | |
| Social marginalization |
| Better Hearing Institute: Hearing Loss Resources Hearing Loss Association of America: Technology | |
| Cognitive testing reliability |
| No known online resources available | |
| End-of-life care and placement in long-term care facility |
| National Association of the Deaf: Senior Resources The Joint Commission: Advancing Effective Communication, Cultural Competence, and Patient- and Family-Centered Care: A Roadmap for Hospitals | |
Social isolation is a primary concern for these patients. Communication and language needs vary dramatically among patients with postlingual deafness (i.e., persons who lost their hearing later in life) and those with prelingual deafness (i.e., persons who were born deaf or became deaf before the acquisition of language). For example, patients with postlingual deafness may prefer to rely on assistive hearing devices and speechreading to help facilitate communication, whereas patients with prelingual deafness may require a sign language interpreter. Each patient should be assessed individually to identify the most effective communication and language strategies.
COGNITIVE TESTING
Cognitive testing for individuals with significant hearing loss (especially those who communicate by sign language) can be problematic for several reasons, including the lack of clinically validated cognitive test measures, and language and communication barriers that limit or preclude the ability to use cognitive tests.5,6 The Mini-Mental State Examination and the Mini-Cognitive Assessment Instrument are widely used tools to screen for the degree of cognitive function in older adults. The written version of the Mini-Mental State Examination can be used with some success in individuals who have significant hearing loss and who are literate in English.
Before performing any cognitive testing in patients who have hearing loss, it is important to ensure that appropriate hearing amplification (if an option for the patient) and communication strategies (including sign language) are utilized. Poor patient-physician communication may result in test scores that are inaccurately interpreted as cognitive decline.7 This is reflected in studies showing that individuals with hearing loss and dementia appear to improve their cognitive testing scores and behaviors simply through the use of hearing aids.8,9 Physicians should also be aware of test-taking and communication anxiety that may affect cognitive testing results. Patients who misunderstand or experience communication difficulties during instructions and test administration may become increasingly nervous or have trouble concentrating on the task, which further impairs the accuracy of the test results.
LONG-TERM CARE
It is crucial for family physicians to discuss potential long-term care with patients who are deaf or hard of hearing before the need arises. This provides patients and their families with adequate time to decide on an optimal strategy before such care is needed. For patients requiring long-term care, working closely with a social worker is instrumental in finding an option that can maximize the patient's stay at home, or in locating a specialized residential facility that may be better equipped to serve persons who are deaf or hard of hearing (Table 1). Some parts of the country now have housing groups that focus on designing and developing retirement and long-term care communities specifically for older persons with significant hearing loss, which may particularly benefit sign language users.
END-OF-LIFE CARE
As with any patient, it is important that end-of-life care discussions, including health care proxies and advance directives, are reviewed regularly during nonurgent appointments, such as physical examinations. Deteriorating communication can be particularly important for individuals with significant hearing loss during times of medical crisis, and can lead to decisions that patients and their family members may regret later. Some hospices and organizations that work with individuals with hearing loss maintain lists of volunteers who are deaf or hard of hearing themselves. These volunteers can be helpful in meeting the social needs of these patients at the end of their lives.

