A 61-year-old woman presented with easy bruising that had progressed to spontaneous development of painful bruises covering approximately 10 percent of her body. The symptoms began one month earlier.
She had a history of depression, migraines, coronary artery disease, and two transient ischemic attacks. She had been taking the same regimens of butalbital/aspirin/caffeine (Fiorinal), prescribed and over-the-counter aspirin, and clopidogrel (Plavix) for years, but had recently started desvenlafaxine (Pristiq) for refractory depression. She did not have recent illness, fevers, or other pain.
Physical examination revealed large, diffuse hematomas on all aspects of her body (Figures 1 and 2). The hematomas appeared spontaneously and rapidly with minimal pressure. Complete blood count was unremarkable.
Figure 1.
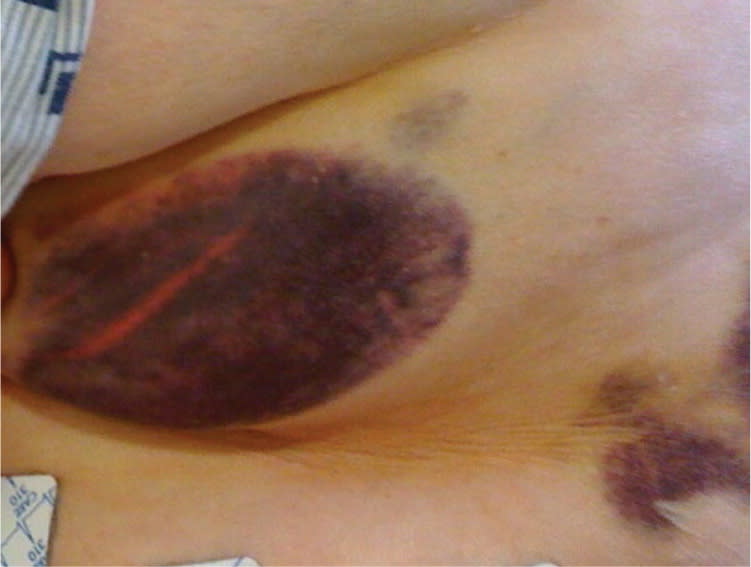
Figure 2.
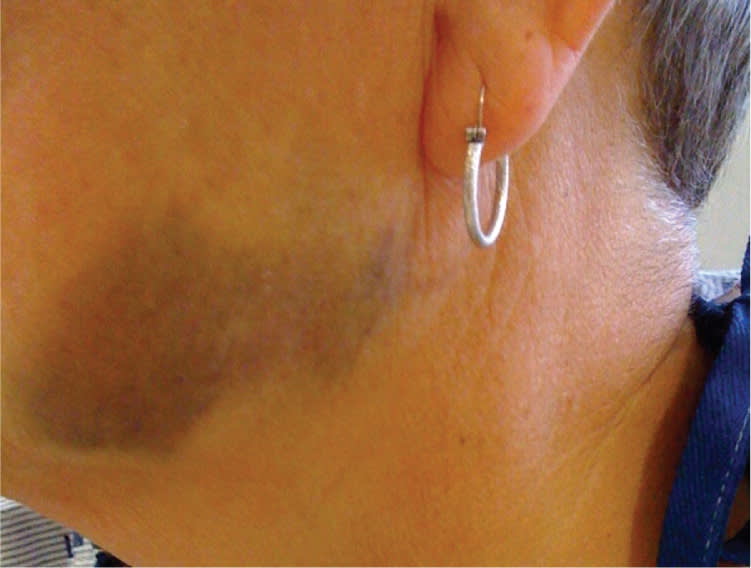
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Hemophilia.
B. Iatrogenic coagulopathy.
C. Physical abuse.
D. Senile purpura.
E. Thrombocytopenic purpura.
Discussion
The answer is B: iatrogenic coagulopathy. Coagulopathy with clopidogrel and aspirin is well described.1,2 Selective serotonin reuptake inhibitors (SSRIs) and selective norepinephrine reuptake inhibitors (SNRIs) may increase bleeding in patients who are on concurrent antiplatelet therapy.3
Newer formulations of SSRIs and SNRIs have been developed to reduce adverse effects and drug-drug interactions,4 but they may not reduce the bleeding risk. As the use of these medications increases, it is important to recognize their potential interactions with antiplatelet medications. Patients should be monitored closely for bleeding risk, particularly at initiation and dosage changes. Treatment is the discontinuation of one of the medications.
Hemophilia is a group of genetic disorders associated with decreased coagulation.5 The spectrum of hemophilia runs from mild (typically occurs only after surgery or trauma) to severe (often evident at birth). Moderate disease can present later in life with spontaneous bleeding, but this is rare. Hemophilia typically leads to hemarthrosis, causing pain in weight-bearing joints.
Physical abuse of older persons is common, and can present as unexplained bruises or welts.6 Other signs include malnutrition, open sores, dehydration, sudden patchy hair loss, and unexplained fractures.7 Other clinical signs and spontaneous bruising would not be present.
Senile purpura appears as dark, irregularly shaped hemorrhagic areas caused by abnormal skin elasticity and mobility that lead to tearing of small, superficial blood vessels.8 These hemorrhagic areas are typically limited to the extensor surfaces of the hands and arms. The condition is associated with aging because of gradual atrophy of the perivascular connective tissue on the extensor surfaces of the hands and arms.
Thrombocytopenic purpura can be idiopathic or have a thrombotic etiology.9,10 Both types are characterized by thrombocytopenia, and patients may have a history of recent viral infection, upper respiratory tract illness, malignancy, or use of antiplatelet drugs. The acute idiopathic type is rare in adults, and the thrombotic type typically is accompanied by other clinical signs, including neurologic findings, decreased renal function, and fever. Diagnosis can be excluded with a normal platelet count or possibly the absence of supporting clinical evidence.
Summary Table
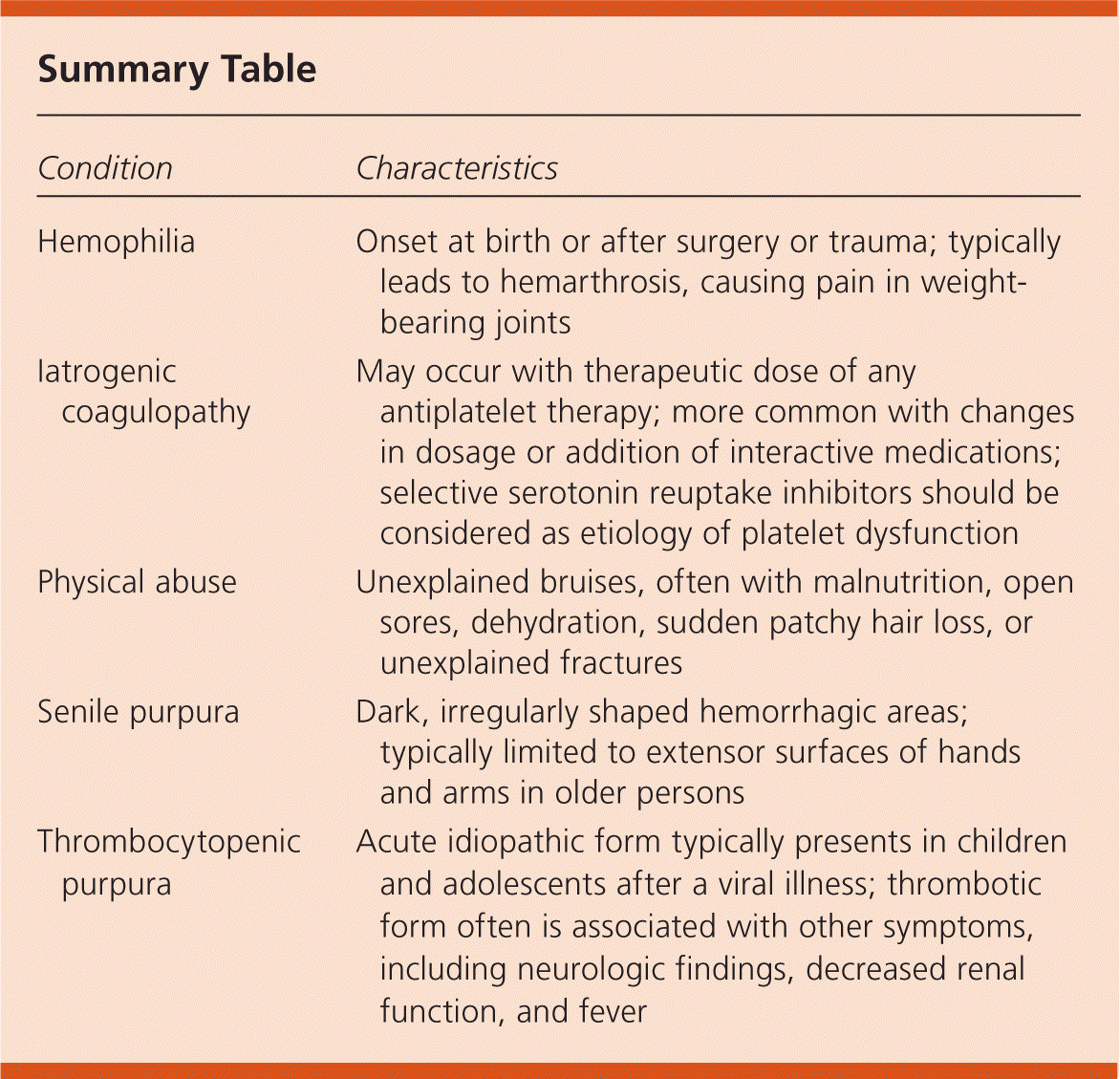
| Condition | Characteristics |
|---|---|
| Hemophilia | Onset at birth or after surgery or trauma; typically leads to hemarthrosis, causing pain in weight-bearing joints |
| Iatrogenic coagulopathy | May occur with therapeutic dose of any antiplatelet therapy; more common with changes in dosage or addition of interactive medications; selective serotonin reuptake inhibitors should be considered as etiology of platelet dysfunction |
| Physical abuse | Unexplained bruises, often with malnutrition, open sores, dehydration, sudden patchy hair loss, or unexplained fractures |
| Senile purpura | Dark, irregularly shaped hemorrhagic areas; typically limited to extensor surfaces of hands and arms in older persons |
| Thrombocytopenic purpura | Acute idiopathic form typically presents in children and adolescents after a viral illness; thrombotic form often is associated with other symptoms, including neurologic findings, decreased renal function, and fever |

