Urinary incontinence is common, increases in prevalence with age, and affects quality of life for men and women. The initial evaluation occurs in the family physician's office and generally does not require urologic or gynecologic evaluation. The basic workup is aimed at identifying possible reversible causes. If no reversible cause is identified, then the incontinence is considered chronic. The next step is to determine the type of incontinence (urge, stress, overflow, mixed, or functional) and the urgency with which it should be treated. These determinations are made using a patient questionnaire, such as the 3 Incontinence Questions, an assessment of other medical problems that may contribute to incontinence, a discussion of the effect of symptoms on the patient's quality of life, a review of the patient's completed voiding diary, a physical examination, and, if stress incontinence is suspected, a cough stress test. Other components of the evaluation include laboratory tests and measurement of postvoid residual urine volume. If the type of urinary incontinence is still not clear, or if red flags such as hematuria, obstructive symptoms, or recurrent urinary tract infections are present, referral to a urologist or urogynecologist should be considered.
Urinary incontinence affects millions of persons, and the prevalence increases with age. Roughly 20 million American women and 6 million American men experience urinary incontinence at some time in their lives.1
Although women report incontinence more often than men,2,3 after 80 years of age, both sexes are affected equally.3 Women commonly experience stress or urge incontinence (i.e., overactive bladder), or a combination of the two, with approximately equal frequency.4 In men, prostate problems, which lead to overflow incontinence, and their treatments, which lead to stress incontinence, are the most common causes.5
Despite what many patients believe, urinary incontinence is not a normal result of aging. It is a pathologic condition that affects quality of life. Patients who have incontinence are more likely to have depression, limited social and sexual function, and dependence on caregivers.3,6,7 Guidelines for diagnosis and treatment of urinary incontinence were published in 2012 by the American Urological Association.8 This article reviews the diagnosis; a separate article in an upcoming issue of AFP reviews management options in women.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
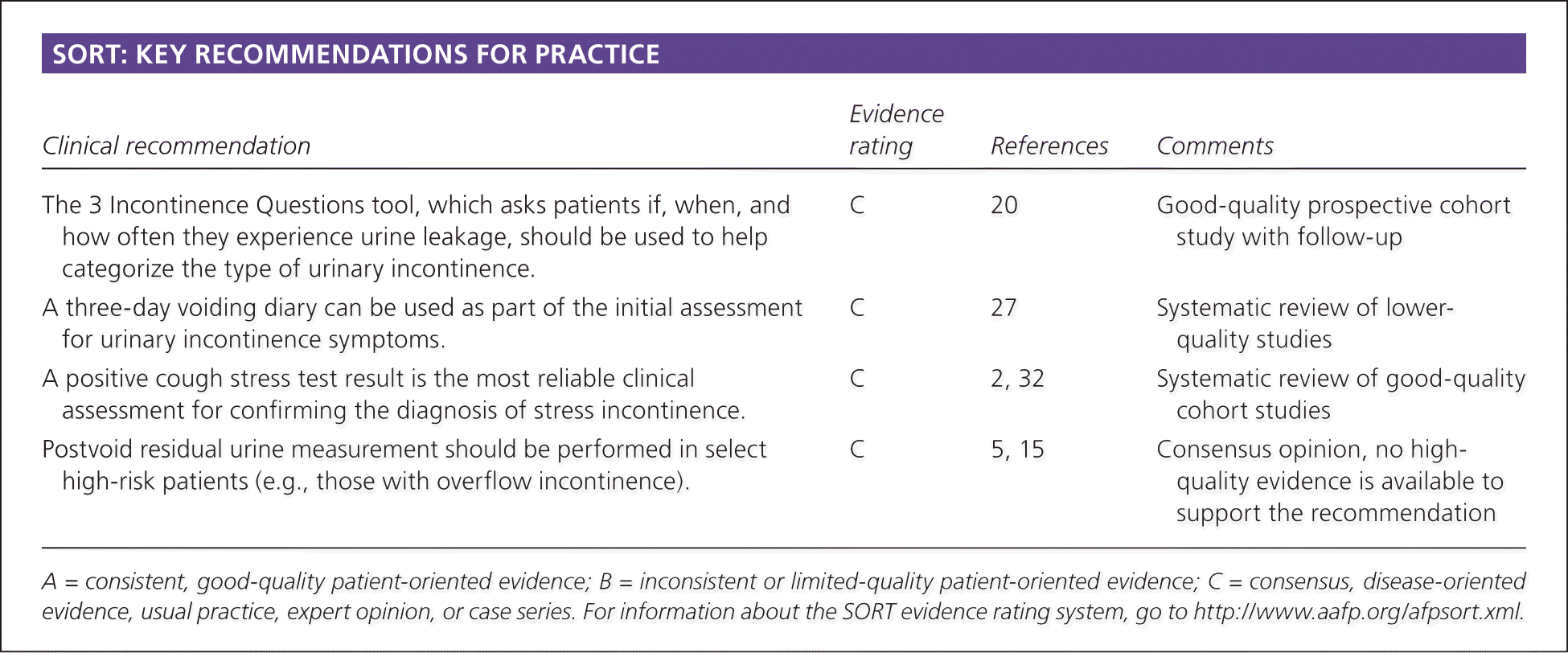
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| The 3 Incontinence Questions tool, which asks patients if, when, and how often they experience urine leakage, should be used to help categorize the type of urinary incontinence. | C | 20 | Good-quality prospective cohort study with follow-up |
| A three-day voiding diary can be used as part of the initial assessment for urinary incontinence symptoms. | C | 27 | Systematic review of lower-quality studies |
| A positive cough stress test result is the most reliable clinical assessment for confirming the diagnosis of stress incontinence. | C | 2, 32 | Systematic review of good-quality cohort studies |
| Postvoid residual urine measurement should be performed in select high-risk patients (e.g., those with overflow incontinence). | C | 5, 15 | Consensus opinion, no high-quality evidence is available to support the recommendation |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Classification
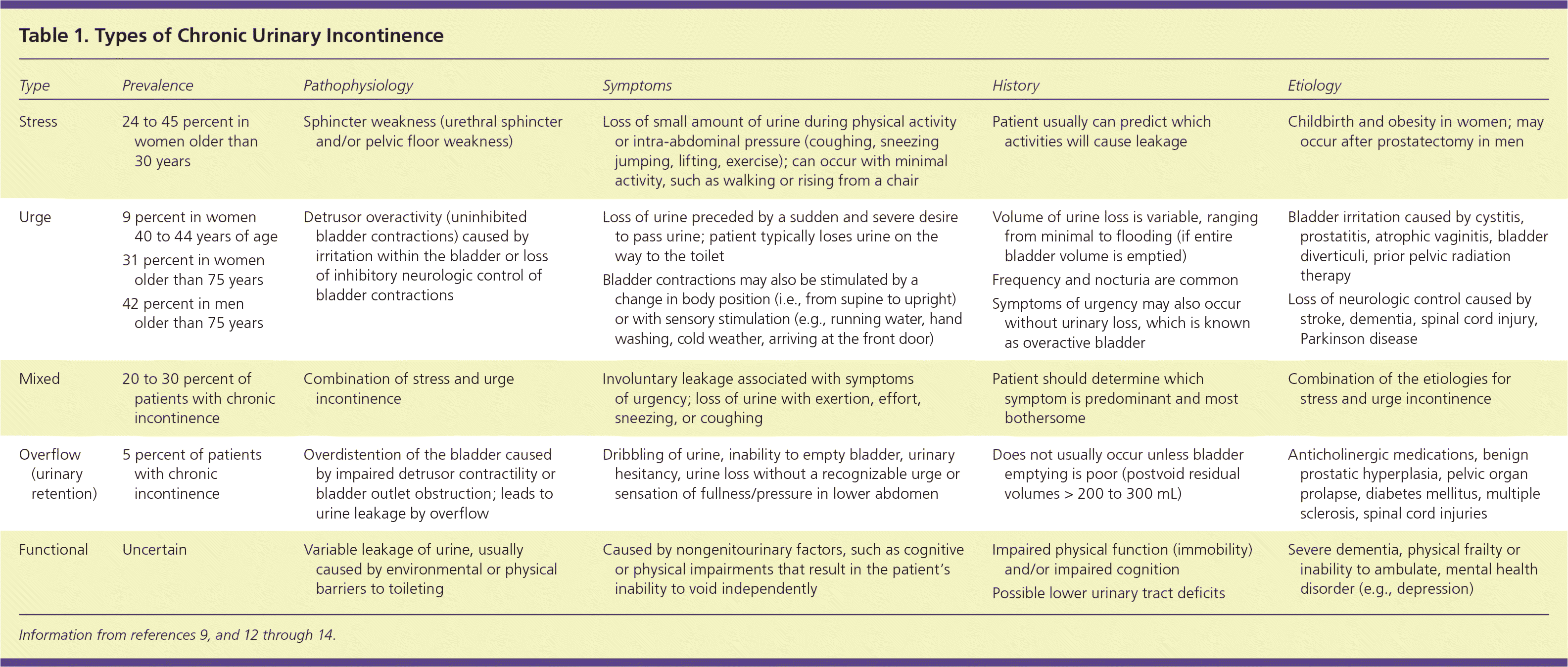
Incontinence can be classified as transient or chronic.5,9 Transient incontinence is urinary leaking that spontaneously reverses after the underlying cause is resolved.10 Chronic urinary incontinence does not typically resolve spontaneously, and is classified into five types: stress, urge, mixed, overflow, or functional.2,11 Characteristics of each type are shown in Table 1.9,12–14
Table 1. Types of Chronic Urinary Incontinence
| Type | Prevalence | Pathophysiology | Symptoms | History | Etiology |
|---|---|---|---|---|---|
| Stress | 24 to 45 percent in women older than 30 years | Sphincter weakness (urethral sphincter and/or pelvic floor weakness) |
|
|
|
| Urge |
| Detrusor overactivity (uninhibited bladder contractions) caused by irritation within the bladder or loss of inhibitory neurologic control of bladder contractions |
|
|
|
| Mixed |
| Combination of stress and urge incontinence |
|
|
|
| Overflow (urinary retention) |
| Overdistention of the bladder caused by impaired detrusor contractility or bladder outlet obstruction; leads to urine leakage by overflow |
|
|
|
| Functional |
| Variable leakage of urine, usually caused by environmental or physical barriers to toileting |
|
|
|
Stress incontinence is caused by sphincter weakness, which leads to ineffective function. It is the most common cause of urinary incontinence in younger women and the second most common cause in older women.15 It also occurs in men after prostate surgery. Urge incontinence is a result of detrusor overactivity, and can be further divided into two subtypes: sensory (a result of local irritation, inflammation, or infection within the bladder) or neurologic (most often caused by loss of cerebral inhibition of detrusor contractions).12 Aging increases the prevalence of urge and stress incontinence, and the two often coexist, leading to mixed incontinence. This occurs in about one-third of adults who have incontinence.9,15
Overflow incontinence is caused by impaired detrusor contractility, bladder outlet obstruction, or both, resulting in overdistension of the bladder.2,5 Chronic overflow incontinence is common in men because of prostatic hyperplasia, but it is uncommon in women.15 Functional incontinence is caused by cognitive, functional, or mobility difficulties that impair patients' ability to use the toilet, but without a failure of bladder function or neurologic control of urination.2,16 This type of incontinence is also referred to as toileting difficulty.16
Evaluation
Patients can be evaluated for urinary incontinence in a family physician's office. Although most incontinence research excludes men and children, a standardized approach is recommended for guiding the initial evaluation.17 An algorithm for the diagnosis of urinary incontinence is shown in Figure 1.
Figure 1. Diagnosis of Urinary Incontinence
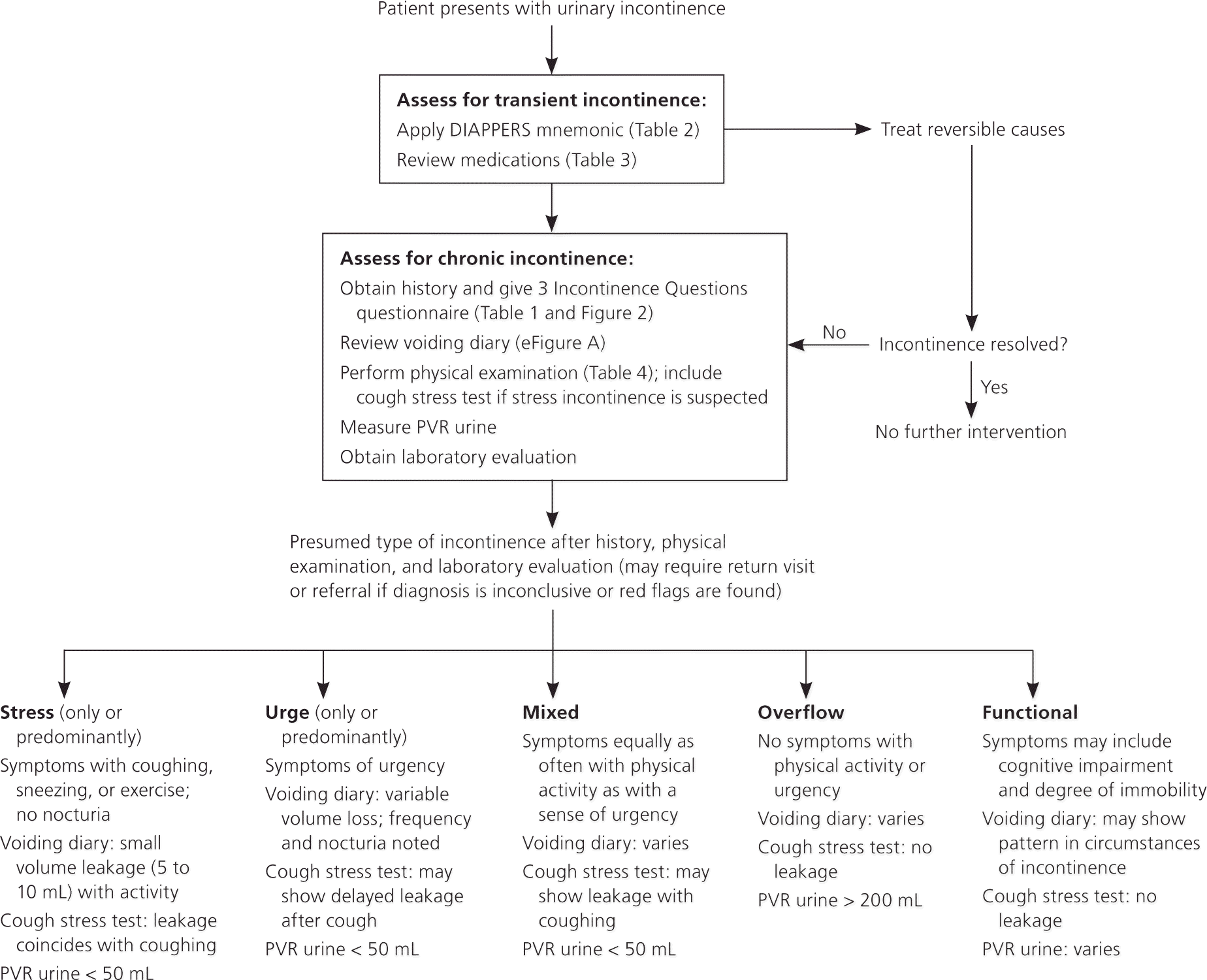
Algorithm for the diagnosis of urinary incontinence. (PVR = postvoid residual.)
The patient history is often the most important factor in identifying the type, severity, and burden of incontinence for patients.6 Generally, more than one office visit is required to perform the physical examination and necessary tests.11
Transient Urinary Incontinence
The first step in the evaluation is to identify transient or reversible causes of urinary incontinence.10,11,13 Reversible incontinence usually has a sudden onset and has been present for less than six weeks at the time of evaluation.18 The mnemonic DIAPPERS is useful for recalling the common reversible causes of urinary incontinence (Table 2).19
Table 2. Differential Diagnosis of Transient Causes of Urinary Incontinence (DIAPPERS Mnemonic)

| Delirium |
| Infection (acute urinary tract infection) |
| Atrophic vaginitis |
| Pharmaceuticals (Table 3) |
| Psychological disorder, especially depression |
| Excessive urine output (e.g., hyperglycemia) |
| Reduced mobility (i.e., functional incontinence) or reversible (e.g., drug-induced) urinary retention |
| Stool impaction |
Adapted with permission from Resnick NM, Yalla SV. Management of urinary incontinence in the elderly. N Engl J Med. 1985;313(13):801.
Physicians should take note of patients' medications, especially those started recently. Medication-induced incontinence often can be reversed by stopping the medication. Table 3 lists the most important medications to consider.6,13 Certain drugs (e.g., diuretics, alcohol) have no pharmacologic action on the lower urinary tract, but may contribute to incontinence by increasing urine production or impairing nervous system function.9,11
Table 3. Common Medications and Substances That Can Cause Urinary Incontinence

| Class | Mechanism of effect |
|---|---|
| Antihypertensives | |
| Alpha-adrenergic antagonists | Decrease sphincter tone, causing stress incontinence |
| Angiotensin-converting enzyme inhibitors | May increase coughing, causing stress incontinence |
| Calcium channel blockers | Relax the bladder, causing retention and overflow incontinence |
| Diuretics | High urine flow that leads to bladder contractions, causing urge incontinence |
| Pain relievers | |
| Cyclooxygenase-2 selective nonsteroidal anti-inflammatory drugs | Increase fluid retention, causing nocturnal diuresis and functional incontinence |
| Opioids | Relax the bladder, causing fecal impaction, sedation, retention, and overflow incontinence |
| Skeletal muscle relaxants | Inhibit bladder contractions, causing sedation, retention, and overflow incontinence |
| Psychotherapeutics | |
| Antidepressants, antiparkinsonian agents, antipsychotics | Inhibit bladder contractions, causing retention and overflow incontinence |
| Sedatives and hypnotics | Lead to sedation and impaired cognition, causing functional or overflow incontinence |
| Others | |
| Alcohol | Leads to diuretic effect and depressed central inhibition, causing urge incontinence, overflow incontinence, or both |
| Antihistamines, anticholinergics | Inhibit bladder contractions, causing sedation, retention, and overflow incontinence |
| Medications for urinary urgency | Inhibit bladder contractions, causing sedation, retention, and overflow incontinence |
| Thiazolidinediones | Increase fluid retention, causing nocturnal diuresis and functional incontinence |
If the incontinence is determined to be related to an acute condition, correcting the transient causes may resolve the symptoms.10,13 However, if symptoms persist, further evaluation is needed.
Chronic Urinary Incontinence
PATIENT QUESTIONNAIRES
Several questionnaires are available to determine which type of chronic urinary incontinence is present.2 The 3 Incontinence Questions is a reliable questionnaire available free of charge (Figure 2).20 It asks three multiple choice questions about if, when, and how often patients experience urine leakage. This questionnaire has been validated in studies that show it to be reasonably accurate in categorizing urinary incontinence in middle-aged to older women.20 It has a sensitivity of 0.86 and 0.75, and a specificity of 0.60 and 0.77, for classifying stress and urge incontinence, respectively.20
Figure 2. The 3 Incontinence Questions

Questionnaire for the evaluation of urinary incontinence.
Adapted with permission from Brown JS, Bradley CS, Subak LL, et al.; Diagnostic Aspects of Incontinence Study (DAISy) Research Group. The sensitivity and specificity of a simple test to distinguish between urge and stress urinary incontinence. Ann Intern Med. 2006;144(10):716.
ASSESSMENT OF MEDICAL PROBLEMS
The patient history should include an assessment of other medical conditions and symptoms, with their temporal relationship to urinary incontinence.15 For example, a history of bowel, back, gynecologic, or bladder surgery could affect the anatomy and innervation of the lower urinary tract, leading to incontinence.6,15 Gynecologic history can assess estrogen status; estrogen deficiency may result in atrophic vaginitis or atrophic urethritis, a potentially reversible cause of urinary incontinence.6
Physicians should also inquire about other comorbidities, such as chronic obstructive pulmonary disease (chronic cough can result in stress incontinence); cardiovascular disease (volume status or diuretic therapy can increase urine flow and cause incontinence in patients with an overactive bladder); neurologic conditions (central nervous system dysfunction can impair inhibition of detrusor contractions, or lead to denervation of the detrusor muscle with resultant retention and overflow incontinence); and musculoskeletal conditions (impaired mobility can cause functional incontinence). Treating these conditions may not eliminate incontinence, but it may lessen the severity.2,9,15
ASSESSMENT OF QUALITY OF LIFE
The severity of symptoms and their effect on quality of life determines the aggressiveness of treatment.6,15 Patients should be asked about the effects of incontinence on work, activities of daily living, sleep, sexual activity, social interactions, interpersonal relationships, and general perception of health and quality of life.6,15
Identifying the most bothersome symptom will help direct management. For example, one patient may be most concerned about managing nocturia (often caused by urge incontinence), whereas another patient may be most concerned about incontinence that occurs during exercise (typically caused by stress incontinence).
VOIDING DIARY
Because many patients provide an unclear voiding history, a voiding diary can be helpful (eFigure A). The simplest voiding diaries ask patients to record the frequency of incontinence episodes, but diaries also can be used to assess the situations in which incontinence occurs, which can help clarify the type of incontinence. For example, the diary may reveal leakage during times of increased abdominal pressure, suggestive of stress incontinence, or dribbling that is indicative of overflow incontinence.21 Patients with stress incontinence usually wake once or not at all at night to void; patients with urge incontinence usually wake more than twice and as often as every hour.21,22
A voiding diary can also serve as a baseline for comparing the severity of incontinence after treatment, thereby assessing the effectiveness of management.23,24 A three-day diary is as informative as a longer-term assessment, has good reliability, and may be more feasible than longer diaries in routine clinical settings.25–27
More sophisticated diaries, such as a frequency-volume voiding diary for assessing bladder activity, can also be used.10,24 A frequency-volume voiding diary requires recording the amount of fluid intake, the volume of urine voided (in mL) of each continent episode (using a measuring cup or plastic hat placed below the toilet seat), and an estimation of the volume of each incontinent episode.28 This approach can reliably discriminate between urge and stress incontinence. Urge incontinence typically involves a large volume of urine loss, whereas stress incontinence is often a smaller volume and is associated with increased abdominal pressure.29,30 A frequency-voiding diary can reveal whether the patient is experiencing frequent large volume voids, which are typically associated with conditions causing polyuria (e.g., excess fluid intake, diabetes mellitus).
PHYSICAL EXAMINATION
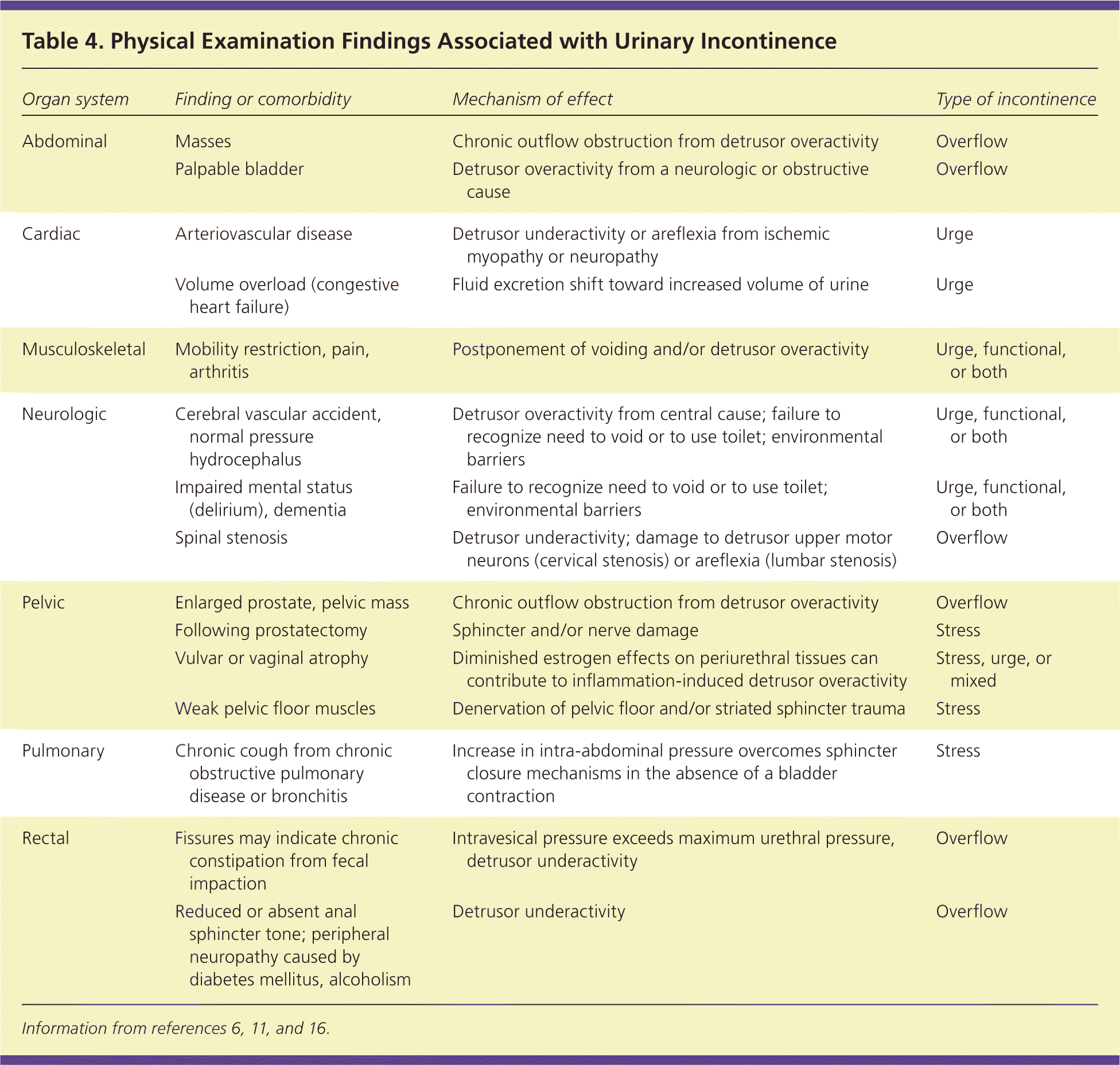
The physical examination can identify anatomic abnormalities or transient causes that may not have been considered after applying the DIAPPERS mnemonic. Findings associated with incontinence are listed in Table 4.6,11,16 In particular, the cardiovascular examination should look for evidence of volume overload (e.g., rales, pedal edema) that might result in increased urine flow, which aggravates urge incontinence. The abdomen should be palpated for masses and tenderness, and the bladder percussed for distention that would indicate overflow.11,17 The extremities should be examined for joint mobility and function (impairment of which might indicate functional incontinence), and peripheral edema that might indicate volume overload.
Table 4. Physical Examination Findings Associated with Urinary Incontinence
| Organ system | Finding or comorbidity | Mechanism of effect | Type of incontinence |
|---|---|---|---|
| Abdominal | Masses | Chronic outflow obstruction from detrusor overactivity | Overflow |
| Palpable bladder | Detrusor overactivity from a neurologic or obstructive cause | Overflow | |
| Cardiac | Arteriovascular disease | Detrusor underactivity or areflexia from ischemic myopathy or neuropathy | Urge |
| Volume overload (congestive heart failure) | Fluid excretion shift toward increased volume of urine | Urge | |
| Musculoskeletal | Mobility restriction, pain, arthritis | Postponement of voiding and/or detrusor overactivity | Urge, functional, or both |
| Neurologic | Cerebral vascular accident, normal pressure hydrocephalus | Detrusor overactivity from central cause; failure to recognize need to void or to use toilet; environmental barriers | Urge, functional, or both |
| Impaired mental status (delirium), dementia | Failure to recognize need to void or to use toilet; environmental barriers | Urge, functional, or both | |
| Spinal stenosis | Detrusor underactivity; damage to detrusor upper motor neurons (cervical stenosis) or areflexia (lumbar stenosis) | Overflow | |
| Pelvic | Enlarged prostate, pelvic mass | Chronic outflow obstruction from detrusor overactivity | Overflow |
| Following prostatectomy | Sphincter and/or nerve damage | Stress | |
| Vulvar or vaginal atrophy | Diminished estrogen effects on periurethral tissues can contribute to inflammation-induced detrusor overactivity | Stress, urge, or mixed | |
| Weak pelvic floor muscles | Denervation of pelvic floor and/or striated sphincter trauma | Stress | |
| Pulmonary | Chronic cough from chronic obstructive pulmonary disease or bronchitis | Increase in intra-abdominal pressure overcomes sphincter closure mechanisms in the absence of a bladder contraction | Stress |
| Rectal | Fissures may indicate chronic constipation from fecal impaction | Intravesical pressure exceeds maximum urethral pressure, detrusor underactivity | Overflow |
| Reduced or absent anal sphincter tone; peripheral neuropathy caused by diabetes mellitus, alcoholism | Detrusor underactivity | Overflow |
In men, a prostate examination should be included to identify prostate enlargement, which may contribute to an outlet obstruction.14,15 In women, an external gynecologic examination can assess for atrophic vaginitis or other vulvar signs of irritation caused by incontinence.14,31 Estrogen deficiency may predispose women to urinary frequency, urgency, or both, and can cause or exaggerate sensory urge incontinence.6,31 Pelvic organ prolapse (with cystocele, urethral polyps, or rectocele) may not lead to incontinence, but it often accompanies atrophic vaginitis.6,14,17,31 A rectal examination is important to assess for fecal impaction, which can exert pressure on the urethra, impair bladder emptying, and precipitate overflow incontinence caused by retention.10,11 In select patients, primarily older adults, a cognitive and functional assessment should be included to evaluate for functional incontinence.3,11,16
COUGH STRESS TEST
If stress incontinence is suspected, the cough stress test is the most reliable clinical assessment for confirming the diagnosis.2,28,32 When compared with more sophisticated multichannel urodynamic studies, the cough stress test demonstrates good sensitivity and specificity for stress incontinence,32–34 although it requires further confirmatory urodynamic evaluation if the results are inconclusive.35
With a full bladder (although not to the point of abrupt urination), the patient should be in the lithotomy position. Women should separate the labia.13,35 The patient should relax the pelvic muscles and forcibly cough once.13 If the test is initially performed supine and no leakage is observed, the test should be repeated in the standing position. The patient stands while wearing a pad or with his or her legs shoulder-width apart over a cloth or paper sheet on the floor to see the leakage. If urine leaks with the onset of the cough and terminates with its cessation, the test is positive for stress incontinence.35
A negative test shows no leak or a delayed leak by five to 15 seconds, and rules out most cases of stress incontinence.36 False-negative results may occur if a patient's bladder is empty, if the cough is not forceful enough, if the pelvic floor muscles contract to override urethral sphincter incompetence, or if severe prolapse masks the leakage.35,36 Furthermore, a delayed leak may suggest a bladder spasm triggered by the cough, and not a weakness of the sphincter. This indicates possible urge incontinence13
LABORATORY TESTS
Laboratory tests should include a serum creatinine level, which may be elevated if there is urinary retention (overflow bladder) caused by bladder outlet obstruction or denervation of the detrusor. If not already performed to exclude acute urinary tract infection as a cause of reversible incontinence, a urinalysis should be obtained to rule out hematuria, proteinuria, and glycosuria, any of which require a diagnostic workup.6
POSTVOID RESIDUAL URINE
A measurement of postvoid residual (PVR) urine is recommended to diagnose overflow incontinence.10 Although overflow incontinence is present in only a minority of patients with incontinence, it is important to exclude this diagnosis because chronic failure of bladder emptying can lead to hydronephrosis and irreversibly impaired renal function. Overflow is more common in older persons, but it can also occur in young adults as a manifestation of neurologic disorders, such as multiple sclerosis. Expert opinion recommends that PVR urine always be measured in patients who may have overflow incontinence, and some experts recommend measuring PVR urine when another cause is not obvious.5,15
To measure PVR urine, the patient empties the bladder, and then the amount of urine remaining in the bladder is measured. This can be performed with a handheld ultrasound unit, which is the preferred method if available. The alternative is in-and-out urethral catheterization.28 In-and-out catheterization requires training to decrease the risk of infection and urethral trauma, which is important in men with significant prostate enlargement.11 If PVR urine cannot be measured in the office setting and if overflow incontinence is strongly suspected, further urodynamic evaluation is warranted.10,12
A PVR urine measurement less than 50 mL is negative for overflow; 100 to 200 mL is considered indeterminate (and the measurement should be repeated on another occasion); and greater than 200 mL is suggestive of over-flow as a main contributing factor of incontinence.6
Referral for Further Evaluation
If the cause of urinary incontinence is unclear after the assessment, referral to a urologist or urogynecologist is recommended (Table 518,36 ). Patients with typical stress or urge incontinence usually do not have any of the red flags of hematuria, obstructive symptoms (straining to void or sensation of incomplete bladder emptying), or recurrent urinary tract infections. If any of these are present, further evaluation is recommended.36
Table 5. Indications for Urologic Referral

| Incontinence associated with relapse or recurrent symptomatic urinary tract infections |
| Incontinence with new-onset neurologic symptoms, muscle weakness, or both |
| Marked prostate enlargement |
| Pelvic organ prolapsed past the introitus |
| Pelvic pain associated with incontinence |
| Persistent hematuria |
| Persistent proteinuria |
| Postvoid residual volume > 200 mL |
| Previous pelvic surgery or radiation |
| Uncertain diagnosis |
Routine referral for urodynamic testing is not recommended, even if a patient is a candidate for surgical treatment of stress incontinence. Studies show that routine preoperative urodynamic testing in patients who have uncomplicated stress incontinence does not result in better surgical outcomes.37
Data Sources: A literature search for scientific evidence supporting evaluation of urinary incontinence was performed in PubMed Clinical Queries using the key terms diagnosis, physical examination, urinary incontinence, and causes. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. We also searched the Agency for Healthcare Research and Quality evidence reports, Clinical Evidence, the Cochrane database, Essential Evidence Plus, and the National Guideline Clearinghouse database. Search date: June 6, 2012.

