Skin of color traditionally refers to that of persons of African, Asian, Native American, Middle Eastern, and Hispanic backgrounds. Differences in cutaneous structure and function can result in skin conditions with distinct presentations and varying prevalence that require unique treatment. Skin cancers have different presentations in these populations. The ability to recognize and diagnose skin cancer in a timely manner is important for reducing morbidity and mortality. Basal cell carcinoma often is pigmented, squamous cell carcinoma occurs in areas of chronic scarring and inflammation, and melanoma presents in non–sun-exposed areas, such as the soles and nail beds. Diagnosis requires biopsy, with the technique depending on size and location of the lesion. Treatment options range from topical to surgical. Acne commonly results in postinflammatory hyperpigmentation and keloids. Combination therapy with topical antibiotics and benzoyl peroxide is generally more effective than monotherapy for treating acne. Use of retinoids at lower concentrations and at less frequent dosing can help prevent postinflammatory hyperpigmentation.
Skin of color, also known as ethnic skin, traditionally refers to that of persons of African, Asian, Native American, Middle Eastern, and Hispanic backgrounds. These skin types are usually categorized as Fitzpatrick types III to VI, and are more richly pigmented1 (Table 12 ). There are notable differences in skin disease incidence, presentation, and treatment based on skin type. This is related to structural and functional differences in the skin and hair, as well as the influence of cultural practices.1,3 For example, increased levels of melanin and larger melanosomes provide greater photoprotection, resulting in a lower incidence of skin cancers.4,5 Higher levels of melanin correlate with increased postinflammatory hyperpigmentation (i.e., darkening of the skin secondary to previous trauma and inflammation).6 Increases in pigment may make it difficult to recognize erythema. Additionally, the curved hair follicle in persons of African descent is related to a greater prevalence of pseudofolliculitis barbae.7 Cultural grooming practices are influenced by the curly, typically kinkier hair in those of African descent, which is often styled with chemicals, traction, or heat, likely contributing to development of scarring alopecias.8
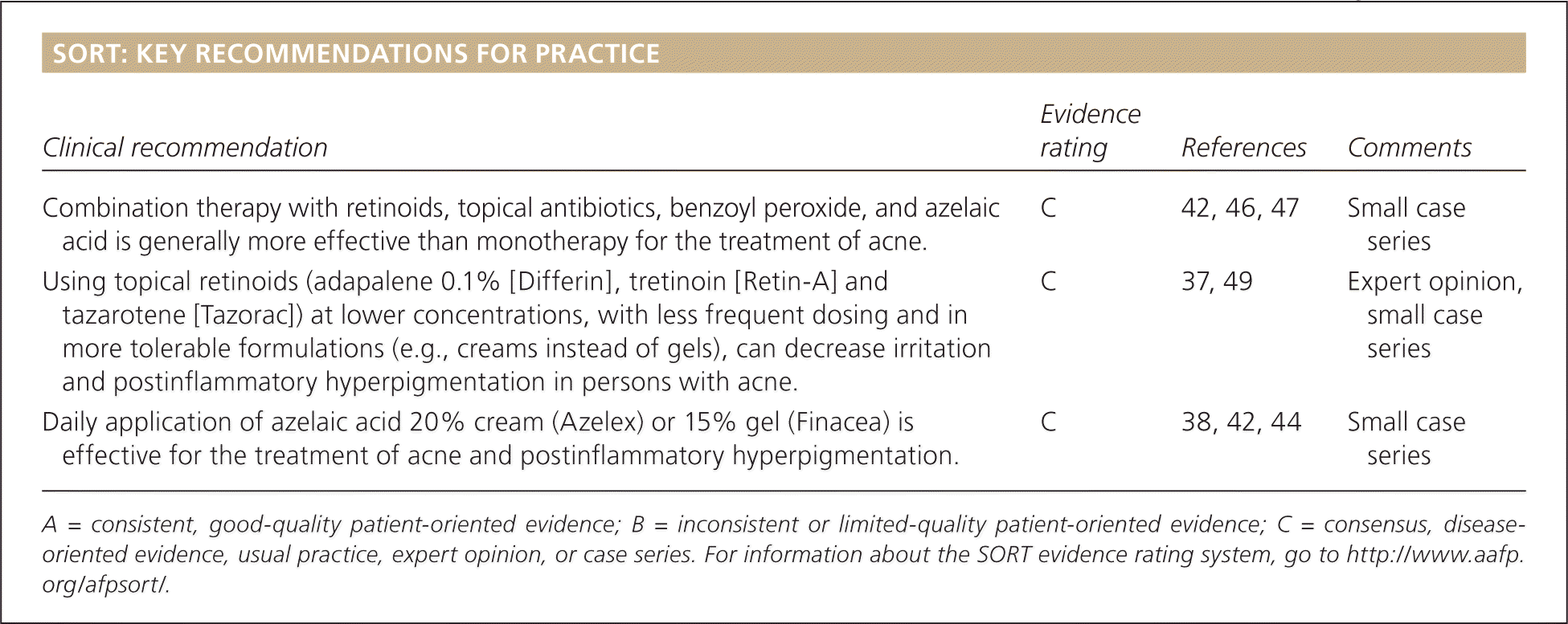
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Combination therapy with retinoids, topical antibiotics, benzoyl peroxide, and azelaic acid is generally more effective than monotherapy for the treatment of acne. | C | 42, 46, 47 | Small case series |
| Using topical retinoids (adapalene 0.1% [Differin], tretinoin [Retin-A] and tazarotene [Tazorac]) at lower concentrations, with less frequent dosing and in more tolerable formulations (e.g., creams instead of gels), can decrease irritation and postinflammatory hyperpigmentation in persons with acne. | C | 37, 49 | Expert opinion, small case series |
| Daily application of azelaic acid 20% cream (Azelex) or 15% gel (Finacea) is effective for the treatment of acne and postinflammatory hyperpigmentation. | C | 38, 42, 44 | Small case series |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort/.
Table 1. Fitzpatrick Skin Types

By 2050, nearly one-half of the U.S. population will be nonwhite.9 Part I of this two-part article discusses common skin conditions that require special consideration in skin of color, including basal cell carcinoma, squamous cell carcinoma, melanoma, acne, and postinflammatory hyperpigmentation. Part II is a review of skin conditions relatively unique to persons with skin of color, including dermatosis papulosa nigra, pseudofolliculitis barbae, acne keloidalis, keloids, and hair disorders.10
Basal Cell Carcinoma
Basal cell carcinoma is the most common skin cancer in whites, Asians, and Hispanic persons11,12 (Table 25,11–15 ). After squamous cell carcinoma, it is the second most common skin cancer in blacks. The primary risk factor for basal cell carcinoma is ultraviolet (UV) radiation. The incidence of basal cell carcinoma is lower in persons with darkly pigmented skin because the increased levels of melanin provide UV protection.16 However, the incidence is increasing in some Asian and Hispanic populations.15
Table 2. Basal Cell Carcinoma Key Points

| Most common skin cancer among whites, Asians, and Hispanic persons11,12 |
| Typical characteristics include a solitary pearly papule with a rolled border and telangiectasias; may be difficult to recognize in skin of color |
| Increased number of pigmented lesions in persons of color13 |
| In Asians, lesions are reported as brown to glossy black with a pearly appearance14 |
| Incidence is increasing in some Asian and Hispanic populations15 |
| Lesions most commonly present on sun-exposed areas of the head and neck |
| Physicians should encourage sun protection, including use of sunscreen and avoidance of tanning booths5 |
Classically, basal cell carcinoma is described as a solitary pearly papule with a rolled border and telangiectasias. These features can be difficult to recognize in dark skin. Lesions may be papules, nodules, plaques, or ulcers; in persons with darker skin, lesions are often asymptomatic, translucent, and have central ulceration.13 Persons with skin of color have an increased number of pigmented basal cell carcinomas (Figure 1). About 50% of lesions may be pigmented in persons with skin of color compared with only 6% in whites.13 In Asians, basal cell carcinomas are reported as brown to glossy black with a pearly appearance.14 These different presentations may result in inaccurate diagnoses, such as seborrheic keratosis or melanoma. Regardless of skin type, basal cell carcinomas most commonly occur in sun-exposed areas of the head and neck. Generally, there is increased risk of basal cell carcinoma in scars and previously radiated sites, as well as in persons with albinism, with xeroderma pigmentosa, or who are immunosuppressed.13 In the Indian population, physical and thermal trauma are important risk factors for basal cell carcinoma.17
Figure 1.
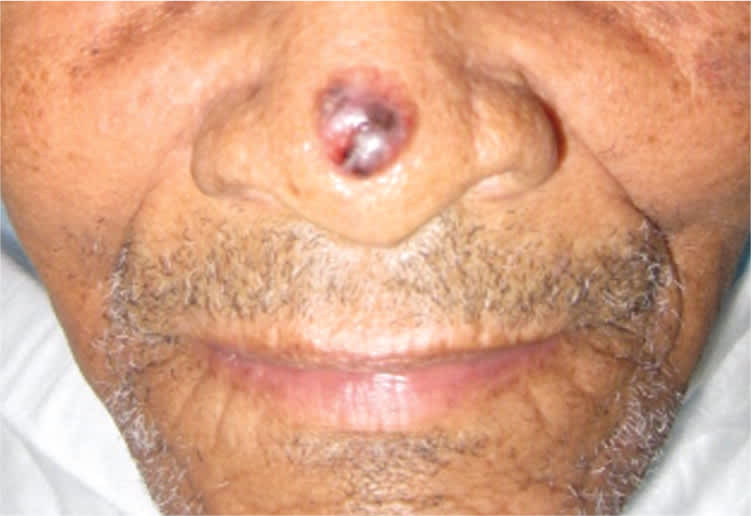
Pigmented basal cell carcinoma. Erythematous plaque with brown, black, and violaceous components on the tip of the nose of a black man.
Diagnosis requires a biopsy, and shave biopsy is usually adequate. Treatment modality depends on the size, location, and histopathologic type of the lesion. Superficial basal cell carcinoma may be treated with topical imiquimod (Aldara), topical fluorouracil, electrodesiccation and curettage, or surgical excision. Generally, Mohs micrographic surgery is the treatment of choice for recurrent lesions, lesions in high-risk areas (e.g., face, scalp, neck), or lesions with high-risk histopathologic subtypes. Basal cell carcinoma has a good prognosis. It rarely metastasizes, with rates of only 0.003% to 0.6%.18 Physicians play a role in managing skin cancer by encouraging sun-protective behaviors and avoidance of tanning booths.5
Squamous Cell Carcinoma
Squamous cell carcinoma is the most common skin cancer in blacks and Indians13 (Table 313,19 ), and the second most common in Chinese, Japanese, and Hispanic persons.12,20 UV exposure is a known risk factor in whites, with most lesions in sun-exposed areas.5 In comparison, the influence of UV light on the etiology of squamous cell carcinoma in skin of color is unclear, and lesions commonly occur in non–sun-exposed sites. There are increased rates of squamous cell carcinoma in Chinese persons who have fairer skin, compared with Indians of Singapore who have darker skin,12 suggesting that UV light does play a role in development. However, the most important risk factors in skin of color include chronic inflammation and scarring.13
Table 3. Squamous Cell Carcinoma Key Points

| Most common skin cancer in blacks and Indians13 |
| In skin of color, lesions commonly occur in non–sun-exposed sites, such as the lower extremities, anogenital area, and scalp19 |
| Chronic scarring and inflammation are risk factors in skin of color13 |
| Lesions are typically erythematous patches, plaques, or nodules and often have a varied appearance |
Squamous cell carcinoma lesions are typically erythematous patches, plaques, or nodules, and often have a varied appearance. In one study of blacks, lesions were usually erythematous with degrees of scale and crust.16 These lesions could be confused with psoriasis, eczema, cutaneous infections, or trauma. There is an increasing incidence of squamous cell carcinoma among Asians older than 60 years.15 The peak incidence in blacks is 40 to 49 years of age.16 Squamous cell carcinoma often occurs at non–sun-exposed sites, such as the lower extremities, anogenital area, and scalp.19 In one study, 65% of lesions in blacks were in covered areas, including 15% in the anus.16 Development in chronic ulcers, lesions of discoid lupus erythematosus, and scars among blacks is well documented.13,20 Biopsy of all nonhealing lesions within or adjacent to chronic scarring or inflammation is important.
Shave biopsy is recommended. Treatment options include topical fluorouracil or imiquimod for superficial lesions, and routine surgical excision or Mohs micrographic surgery for invasive lesions. Squamous cell carcinoma has the potential to metastasize, especially for lesions associated with scars, discoid lupus erythematosus, non–sun-exposed areas, or mucous membranes.21–23
Melanoma
Melanoma is one of the most deadly forms of skin cancer (Table 424–29 ). During recent years, the incidence of cutaneous melanoma among the general population has been increasing,24 although the mortality rate has decreased. Survival rates are directly related to stage at diagnosis, and diagnoses are being made at earlier stages. This is thought to be secondary to increased awareness, education, and early intervention. However, in comparison with the general population, persons with skin of color continue to have more advanced stages at the time of diagnosis, lower survival rates, and generally poorer outcomes.24–27 Perceived risk of skin cancer among those with skin of color appears to affect behavior and outcome; therefore, it is beneficial to educate patients about the risk of developing skin cancer and how to perform a self-examination of the skin.30,31
Table 4. Melanoma Key Points

| Often diagnosed at later stages in persons with skin of color 24–27 |
| Acral lentiginous melanoma is common among persons with skin of color 28,29 |
| Skin examinations should include evaluation of the mucous membranes, hands, feet, and nails |
| Immediate biopsy of suspicious lesions is critical |
| ABCDEs of melanoma: asymmetry, border irregularity, color variation, diameter (> 6 mm), evolution |
Typically, melanoma presents as an isolated, rapidly changing, pigmented macule, patch, papule, or nodule. Melanomas more commonly arise de novo, but can also develop within an existing nevus. Common locations include the back and lower legs. In persons with skin of color, non–sun-exposed sites are the most common location. Palmar, plantar, subungual, and mucous membrane lesions are common. Acral lentiginous melanoma (melanoma involving the palms, soles, or nail beds) is the most common subtype of melanoma in blacks and Asians28,29 (Figures 2 and 3). Superficial spreading melanoma is the most common subtype in Hispanic persons and in whites.13 Evaluation of melanoma of the nail bed can be difficult because many persons with darkly pigmented skin have melanonychia (benign linear pigmentation of the nails). Hutchinson sign, an extension of pigment onto the proximal nail fold, is suggestive of subungual melanoma.13 Pigmentation of the nail plate without extension to the proximal nail fold or involvement of multiple nails is more suggestive of melanonychia.
Figure 2.
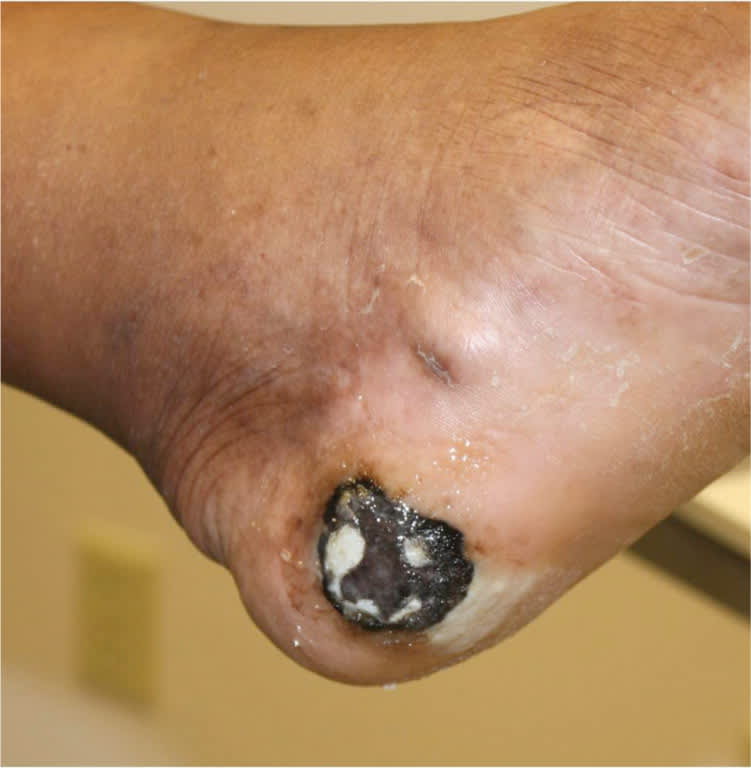
Acral lentiginous melanoma. Hyperpigmented plaque on the heel of a black patient.
Figure 3.
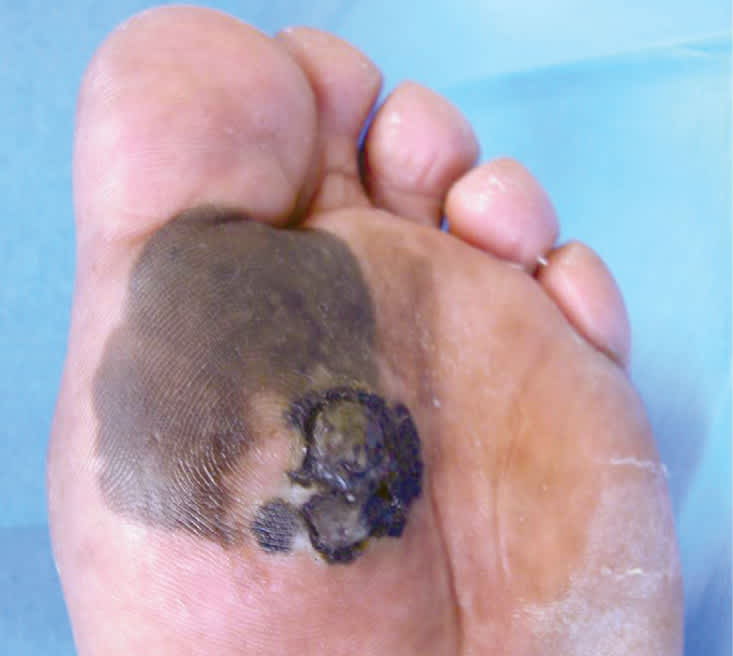
Acral lentiginous melanoma. Large hyperpigmented lesion on the sole of a black patient. The inferior portion is eroded.
Biopsy technique for lesions suspicious for melanoma depends on location and size, and typically involves removing the entire lesion with 2-mm margins. Immediate biopsy of suspicious lesions is critical. Management is widely variable based on the histopathologic depth of the tumor (Breslow depth).
Acne
Acne is one of the most common skin conditions for which patients present for evaluation32–36 (Table 534,37–45 ). In persons with skin of color, the sequelae of postinflammatory hyperpigmentation, keloids, and scarring are common.37–39 Many patients are prone to dryness and irritation as a result of treatment, and this leads to further inflammation and postinflammatory hyperpigmentation. Use of skin and hair care products may exacerbate acne and postinflammatory hyperpigmentation.40
Table 5. Acne Key Points

| Increased potential for postinflammatory hyperpigmentation, scarring, and keloids among persons with darkly pigmented skin37–39 |
| Skin and hair care products may be comedogenic or contribute to irritation, leading to postinflammatory hyperpigmentation34,37,40,41 |
| Start retinoids at lower concentrations with infrequent dosing; cream formulations are better tolerated than gels |
| Use lower concentrations of benzoyl peroxide to limit postinflammatory hyperpigmentation |
| Azelaic acid 20% cream (Azelex) and 15% gel (Finacea) are well-tolerated and effective for acne and postinflammatory hyperpigmentation42–44 |
| Topical retinoids and chemical peels also may be useful in the treatment of acne and postinflammatory hyperpigmentation37,45 |
The presentation of acne is varied. Lesions include open and closed comedones (white-heads and blackheads), papules, pustules, nodules, and cysts. Evaluation begins with determining the predominant lesion type and identifying the presence of post-inflammatory hyperpigmentation and scarring. Taking a history of skin and hair care product use is important. Makeup to cover lesions and emollients to moisturize the hair and skin, such as cocoa butter and olive oil, may be comedogenic.34,37,41
The basic acne therapies are similar for all skin colors. Topical antimicrobials, including benzoyl peroxide and topical antibiotics, and retinoids are first-line therapy for mild to moderate acne. Oral antibiotics are typically reserved for moderate to severe acne. Isotretinoin is used for treatment of resistant, nodular, and cystic acne. Combination therapy (i.e., topical antibiotics and benzoyl peroxide, with or without a topical retinoid for the comedonal component) is generally more effective than monotherapy.42,46–48
To prevent treatment-induced postinflammatory hyperpigmentation, therapies that cause irritation or inflammation should be avoided. When prescribing a retinoid, physicians should start at lower concentrations and titrate up as tolerated. It is best to begin with infrequent dosing (e.g., twice weekly to every other day), and to choose more tolerable formulations, such as creams over gels. Examples of topical retinoids include adapalene 0.1% (Differin), tretinoin (Retin-A), and tazarotene (Tazorac).37,49 Benzoyl peroxide can be drying and irritating; using lower concentrations (less than 5%) can limit irritation and subsequent postinflammatory hyperpigmentation. For patients presenting with acne and postinflammatory hyperpigmentation, azelaic acid 20% cream (Azelex), azelaic acid 15% gel (Finacea), topical retinoids, and chemical peels may be helpful in doses that do not cause irritation or inflammation.37,38,42–45,50 If treatment with topical agents is unsuccessful, physicians may consider prescribing systemic antibiotics, hormonal therapies such as spironolactone (Aldactone) or oral contraceptives, or isotretinoin for recalcitrant cases.
Postinflammatory Hyperpigmentation
Postinflammatory hyperpigmentation can occur in anyone, but is most common in persons with dark skin (Table 63,6 ). It is a result of inflammation from a condition such as eczema or acne, or a therapeutic intervention. Often, it causes more anxiety for the patient than the underlying inflammatory disorder.
Table 6. Postinflammatory Hyperpigmentation Key Points

| Does not require treatment and will likely improve with time |
| Management should focus on treating the underlying inflammatory condition |
| Encourage sun protection |
| Avoid irritants that may exacerbate the condition (e.g., alcohol, witch hazel, irritating makeups and cleansers) |
| Daily application of hydroquinone 4% cream may be helpful |
| A combination of a topical steroid, retinoid, and hydroquinone cream is a treatment option3,6 |
| Talk with the patient about the challenges of treatment and the need for patience |
Clinically, patients may present with dark spots. Postinflammatory hyperpigmentation appears as ill-defined, hyperpigmented macules and patches in the distribution and shape of prior lesions (Figure 4). Depending on the depth of the pigment within the skin, the color may be tan, brown, dark brown, or blue-gray. Persons with darker skin types tend to have increased intensity of postinflammatory hyperpigmentation.
Figure 4.
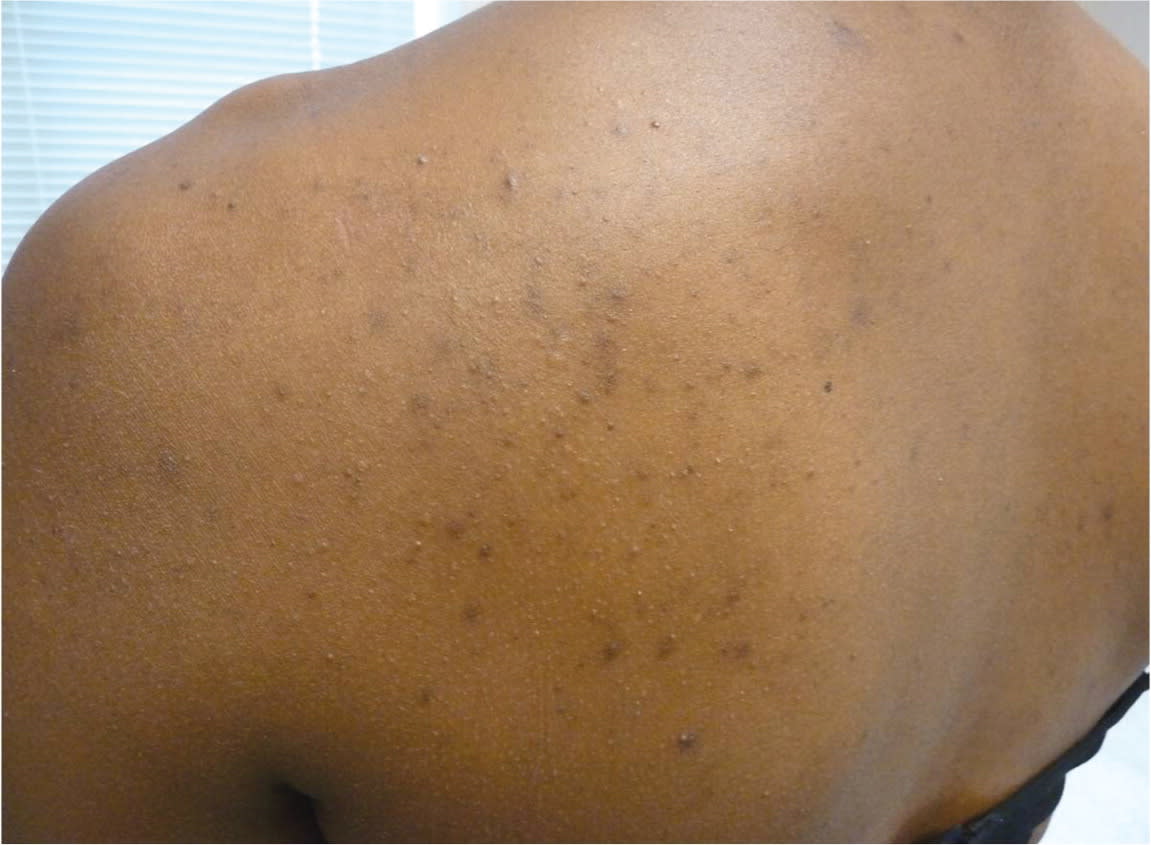
Postinflammatory hyperpigmentation. Hyperpigmented macules and papules on the back of a black patient with acne.
The most important aspect of managing postinflammatory hyperpigmentation is treatment of the underlying inflammatory condition to prevent exacerbation. To guide treatment, it can be helpful to survey the entire involved area for signs of the primary condition. Existing postinflammatory hyperpigmentation will usually improve with time and does not require therapy. If left untreated, epidermal postinflammatory hyperpigmentation will take six to 12 months to fade. Deeper pigment may take years. Patient counseling should include a discussion about the need for time and patience while managing this condition.
An important part of therapy is sunscreen with a minimum sun protection factor (SPF) of 30 to prevent darkening of postinflammatory hyperpigmentation. This may not be a common practice among dark-skinned persons and should be emphasized. Possible irritants to avoid include irritating topical medications, alcohol, witch hazel, astringents, fragrances, and cosmeceuticals. Medical therapy includes use of topical hydroquinone, retinoids, kojic acid, azelaic acid, chemical peels, corticosteroids, and combination therapy.3,6 The preferred treatment is hydroquinone 4%.6 However, there have been concerns about potential adverse effects. In rodents, oral ingestion may be linked to malignant tumors, and in humans, there is concern for exogenous ochronosis (progressive darkening of the skin in areas of hydroquinone application).51 The U.S. Food and Drug Administration proposed a ban of over-the-counter hydroquinone in 2006. Investigation by the National Toxicology Program is ongoing.52
Data Sources: A PubMed search was completed in Clinical Queries using the key terms skin of color, ethnic skin, basal cell carcinoma, squamous cell carcinoma, melanoma, postinflammatory hyperpigmentation, and acne. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the U.S. Preventive Services Task Force database, the Cochrane database, and the National Guideline Clearing-house using the key terms skin, skin cancer, and skin of color. Search dates: April, September, and October 2011.

