Inguinal hernias are one of the most common reasons a primary care patient may need referral for surgical intervention. The history and physical examination are usually sufficient to make the diagnosis. Symptomatic patients often have groin pain, which can sometimes be severe. Inguinal hernias may cause a burning, gurgling, or aching sensation in the groin, and a heavy or dragging sensation may worsen toward the end of the day and after prolonged activity. An abdominal bulge may disappear when the patient is in the prone position. Examination involves feeling for a bulge or impulse while the patient coughs or strains. Although imaging is rarely warranted, ultrasonography or magnetic resonance imaging can help diagnose a hernia in an athlete without a palpable impulse or bulge on physical examination. Ultrasonography may also be indicated with a recurrent hernia or suspected hydrocele, when the diagnosis is uncertain, or if there are surgical complications. Although most hernias are repaired, surgical intervention is not always necessary, such as with a small, minimally symptomatic hernia. If repair is necessary, the patient should be counseled about whether an open or laparoscopic technique is best. Surgical complications and hernia recurrences are uncommon. However, a patient with a recurrent hernia should be referred to the original surgeon, if possible.
Hernia is a general term describing a bulge or protrusion of an organ or tissue through an abnormal opening within the anatomic structure. Although there are many different types of hernias, they are usually related to the abdomen, with approximately 75% of all hernias occurring in the inguinal region.1 Abdominal wall hernias account for 4.7 million ambulatory care visits annually. More than 600,000 surgical repairs for inguinal hernias are performed nationwide each year,2 making it one of the most common general surgical procedures performed in the United States.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Although imaging techniques such as ultrasonography, computed tomography, and magnetic resonance imaging are rarely needed to diagnose inguinal hernias, they may be useful in certain clinical situations. | C | 18 |
| Ultrasonography has good sensitivity and specificity for the detection of groin hernias. | C | 8 |
| Small, minimally symptomatic, first hernias do not necessarily require repair, and these patients may be followed expectantly. They should be counseled on symptoms of incarceration or strangulation, and to seek prompt evaluation if these occur. | C | 16, 17 |
| Patients with symptomatic, large, or recurrent inguinal hernias should be referred for repair, generally within one month of detection. | C | 18 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Inguinal hernias have a 9:1 male predominance,3 with a higher incidence among men 40 to 59 years of age. It has been estimated that more than one-fourth of adult men in the United States have a medically recognizable inguinal hernia.4 Men with a diagnosed hiatal hernia have been shown to have double the risk of an inguinal hernia. Among women, taller height, chronic cough, umbilical hernia, older age, and rural residence have been associated with a higher incidence of inguinal hernia. Neither smoking nor alcohol use has been shown to affect hernia occurrence. Several studies have demonstrated that men who are overweight or obese have a lower risk of inguinal hernia than men of normal weight.4,5
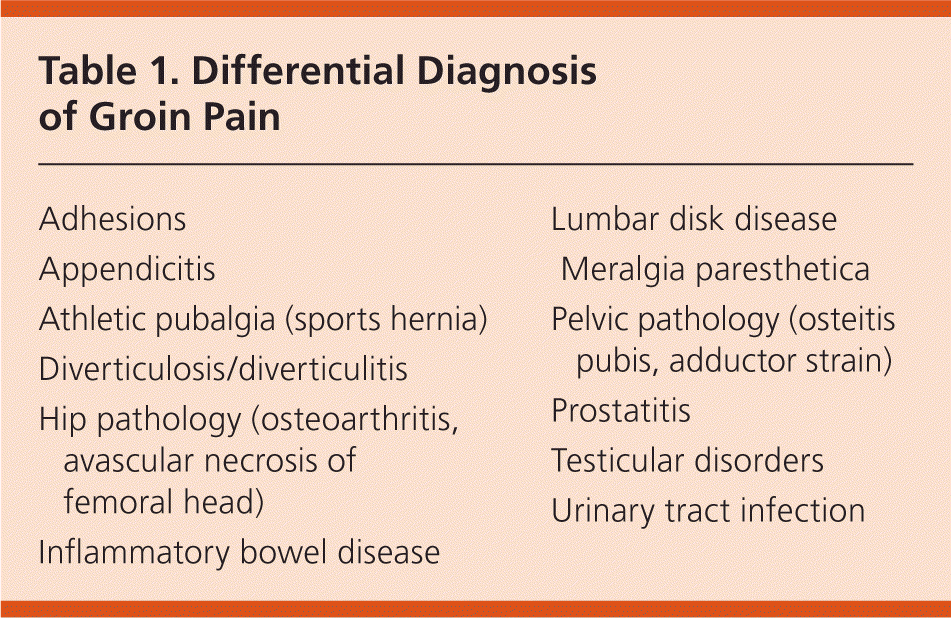
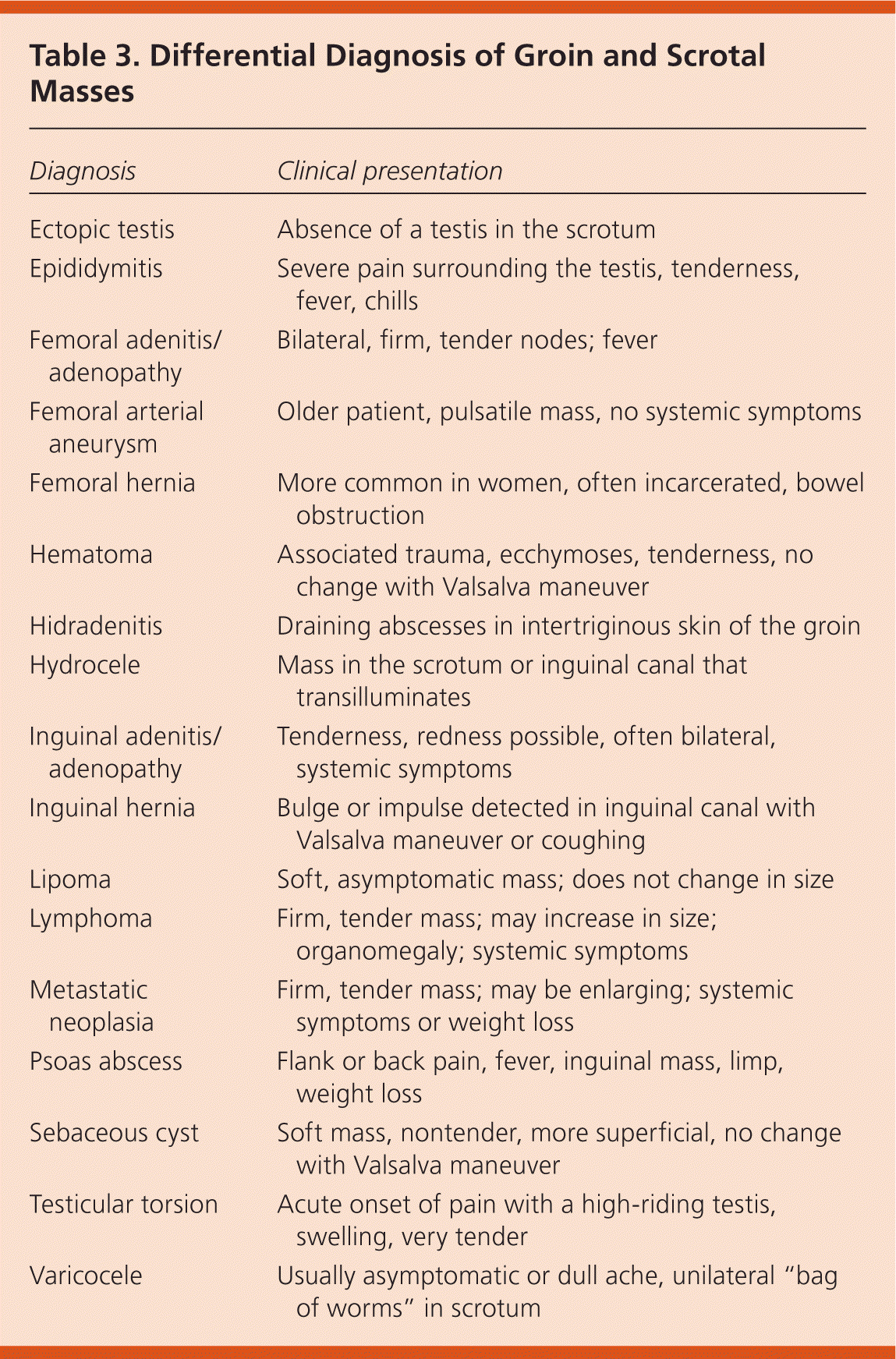
Although this article focuses on inguinal hernias, other diagnostic possibilities should be considered in a patient with groin pain (Table 1). In athletes, groin pain most commonly results from an overuse injury associated with adductor tendons and muscles, and a specific differential diagnosis should be considered in these patients (Table 2).6,7 Any mass palpated in the inguinal region should prompt a thorough clinical evaluation because there are many possible diagnoses (Table 3).
Table 1. Differential Diagnosis of Groin Pain
| Adhesions |
| Appendicitis |
| Athletic pubalgia (sports hernia) |
| Diverticulosis/diverticulitis |
| Hip pathology (osteoarthritis, avascular necrosis of femoral head) |
| Inflammatory bowel disease |
| Lumbar disk disease |
| Meralgia paresthetica |
| Pelvic pathology (osteitis pubis, adductor strain) |
| Prostatitis |
| Testicular disorders |
| Urinary tract infection |
Table 2. Differential Diagnosis of Groin Pain in Athletes

| Diagnosis | Clinical presentation |
|---|---|
| Avulsion fractures | History of sudden or forceful muscle contraction, tenderness over bony prominence, ecchymoses |
| Ligamentous sprains | History of trauma or fall, sudden onset |
| Muscle strains | History of sudden onset during muscle contraction |
| Nerve entrapment syndromes | Associated paresthesias or numbness |
| Osteitis pubis | Tenderness over symphysis pubis |
| Referred pain from lumbar, hip, or sacroiliac area | Associated findings in these areas |
| Sports hernia | History of high-intensity athletic activity, typical symptoms of hernia with no evidence on physical examination, pain with forced adduction against examiner's resistance |
| Stress fractures | History of repetitive motion activity or overuse, tenderness over bone |
| Tendinopathies | Pain with motion and contraction of specific muscle |
Table 3. Differential Diagnosis of Groin and Scrotal Masses
| Diagnosis | Clinical presentation |
|---|---|
| Ectopic testis | Absence of a testis in the scrotum |
| Epididymitis | Severe pain surrounding the testis, tenderness, fever, chills |
| Femoral adenitis/adenopathy | Bilateral, firm, tender nodes; fever |
| Femoral arterial aneurysm | Older patient, pulsatile mass, no systemic symptoms |
| Femoral hernia | More common in women, often incarcerated, bowel obstruction |
| Hematoma | Associated trauma, ecchymoses, tenderness, no change with Valsalva maneuver |
| Hidradenitis | Draining abscesses in intertriginous skin of the groin |
| Hydrocele | Mass in the scrotum or inguinal canal that transilluminates |
| Inguinal adenitis/adenopathy | Tenderness, redness possible, often bilateral, systemic symptoms |
| Inguinal hernia | Bulge or impulse detected in inguinal canal with Valsalva maneuver or coughing |
| Lipoma | Soft, asymptomatic mass; does not change in size |
| Lymphoma | Firm, tender mass; may increase in size; organomegaly; systemic symptoms |
| Metastatic neoplasia | Firm, tender mass; may be enlarging; systemic symptoms or weight loss |
| Psoas abscess | Flank or back pain, fever, inguinal mass, limp, weight loss |
| Sebaceous cyst | Soft mass, nontender, more superficial, no change with Valsalva maneuver |
| Testicular torsion | Acute onset of pain with a high-riding testis, swelling, very tender |
| Varicocele | Usually asymptomatic or dull ache, unilateral “bag of worms” in scrotum |
Symptoms and Physical Findings
The diagnosis of an inguinal hernia is usually made through history and physical examination findings. Although data are limited, in one report, the sensitivity and specificity of the physical examination were 75% and 96%, respectively.8
Symptoms of an inguinal hernia may appear gradually over time or develop suddenly, as with incarceration (i.e., the contents of the hernia sac cannot be returned to the abdominal cavity). Inguinal hernias may be asymptomatic and found incidentally on routine physical examination. Symptomatic patients often present with groin pain, which can be severe. Stretching or tearing of the tissue at and around the hernia defect can lead to a burning, gurgling, or aching sensation in the groin. This usually causes localized pain directly at the site of the hernia. Pain may worsen with Valsalva maneuvers. Patients may experience a heavy or dragging sensation in the groin, especially toward the end of the day and after prolonged activity.1 Activities that increase intra-abdominal pressure, such as coughing, lifting, or straining, cause more abdominal contents to be pushed through the hernia defect. As this occurs, the bulge of the hernia gradually increases in size. If the patient indicates that this bulge disappears while he or she is in the supine position, clinical suspicion of a hernia should be increased. [ corrected]
Hernias may be easily diagnosed with an adequate physical examination. The physical examination should begin by carefully inspecting the femoral and inguinal areas for bulges while the patient is standing. Then, the patient should be asked to strain down (i.e., Valsalva maneuver) while the physician observes for bulges. This may be accomplished by using the right hand to examine the patient's right side and the left hand to examine the patient's left side. The physician invaginates the loose skin of the scrotum with the index finger on the ipsilateral side of the patient, starting at a point low enough on the scrotum to reach as far as the internal inguinal ring. Starting on the scrotum, the examining finger follows the spermatic cord upward above the inguinal ligament to the triangular, slit-like opening of the external inguinal ring. The external inguinal ring is medial to and just below the pubic tubercle. The inguinal canal is gently followed laterally in its oblique course. While the examining finger is in the canal next to the internal inguinal ring, the patient strains down or coughs as the physician feels for any palpable herniation.9 The diagnosis of an inguinal hernia is confirmed if an “impulse” or bulge is felt.
If no bulge is detected with a Valsalva maneuver, a hernia is unlikely. However, athletic pubalgia (sports hernia) may be considered in athletes with groin pain and no bulge. A sports hernia is not a true hernia, but rather a tearing of tissue fibers. This typically occurs in patients with a history of high-intensity athletic activity. Although these patients have typical hernia symptoms, there is no evidence on physical examination. Further follow-up and reexamination are needed to diagnose a sports hernia. Pain along the symphysis pubis suggests osteitis pubis, whereas pain along the adductor tendons suggests adductor tendinopathy.
It is more challenging to diagnose a hernia in female patients. Direct palpation with an open hand over the groin area might detect the impulse of a hernia during a Valsalva maneuver. However, further workup with diagnostic testing or referral to a surgeon is often indicated. Rarely, diagnostic laparoscopy is necessary.
Incarceration may be managed in the office setting if there is no associated pain. The standard of care is to place the patient in the Trendelenburg position while holding gentle pressure on the area for up to 15 minutes. If acute onset of groin pain occurs, the hernia may have become strangulated (i.e., the blood supply to the entrapped contents is compromised). Strangulation should be suspected in the presence of tenderness, redness, nausea, and vomiting and is a surgical emergency.10
Imaging
Although imaging is rarely needed to diagnose a hernia, it may be useful in certain clinical situations (e.g., suspected sports hernia; recurrent hernia or possible hydrocele; uncertain diagnosis; surgical complications, especially chronic pain).8 The clinical use of ultrasonography has shown promise in these situations.11,12 The sensitivity of ultrasonography for the detection of groin hernias is greater than 90%, and the specificity is 82% to 86%.8,13
Use of higher resolution axial computed tomography in the diagnosis of inguinal hernia is being investigated.14 Magnetic resonance imaging may be useful in differentiating inguinal and femoral hernias with a high sensitivity and specificity (greater than 95%).8 The use of magnetic resonance imaging is helpful in the diagnosis of athletic pubalgia or sports hernias, which may occur at any age with potentially more than one cause. The physician may consider magnetic resonance imaging in the workup of patients with activity-related groin pain when no inguinal hernia can be identified on physical examination.15
Surgical Management
In the past, surgical repair was recommended for all inguinal hernias because of the risk of complications such as incarceration or strangulation. However, recent studies have proved that small, minimally symptomatic, first occurrence hernias do not necessarily require repair, and these patients can be followed expectantly. However, they should be counseled on the symptoms of incarceration and strangulation, and to seek prompt evaluation if these occur.16,17 Patients with symptomatic, large, or recurrent hernias should be referred for repair, generally within one month of detection.18 Hernia repair almost always involves some type of prosthetic material (i.e., mesh), with the possible exception of women of childbearing age because stretching of tissues during pregnancy may result in a recurrent hernia. The choice of mesh material used in the repair is based on the surgeon's preference.
The choice of open vs. laparoscopic repair depends on surgeon preference, but only about 10 percent of inguinal hernia repairs in the United States are performed via a laparoscopic technique.19 Open repair may be particularly beneficial in older, less healthy patients.20 Laparoscopic repair is usually reserved for recurrent or bilateral hernias. Open and laparoscopic techniques have similar results (Table 4).21–24 Both procedures are effective if performed by an experienced surgeon, and have a recurrence rate from 0% to 9.4%.25,26
Table 4. Comparison of Laparoscopic and Open Techniques to Repair Primary Inguinal Hernias

| Outcome | Comparison |
|---|---|
| Operative time | Longer with laparoscopy 21–23 |
| Equal24 | |
| Length of hospital stay | Shorter with laparoscopy 22,23 |
| Equal21,24 | |
| Complications | More common with open technique23 |
| Equal21,22,24 | |
| Return to usual activity | Earlier with laparoscopy 21–23 |
| Chronic pain | More common with laparoscopy 21 |
| Equal24 | |
| Chronic numbness | More common with laparoscopy 21 |
| Equal24 | |
| Hernia recurrence | Equal21–24 |
note: It appears that laparoscopic repair increases operative time, but is associated with better patient outcomes and equal recurrence rates compared with open repair.
The most common complications of hernia repair are hematomas, including penile or scrotal ecchymosis; seromas; and wound infection. Although these are uncommon, family physicians should be vigilant because patients may present to them postoperatively. Chronic pain is the most common long-term problem after hernia repair, occurring in 5% to 12% of patients, and is related to nerve scarification, mesh contraction, chronic inflammation, or osteitis pubis.27,28 Treating hernia repair complications can be challenging, and these patients are often referred to the operating surgeon.29
Postoperative Care
The current standard of care after hernia repair is general wound care. The length of required inactivity varies greatly based on the surgeon's preference, but activity is usually permitted within two to four weeks for laborers and within 10 days as tolerated for professionals.30,31
Data Sources: The literature search was conducted using the keywords hernia, hernia surgery, groin pain, and laparoscopic repair. We searched the Centers for Disease Control and Prevention, Cochrane Database of Systematic Reviews, Agency for Healthcare Research and Quality Evidence Reports, National Guidelines Clearinghouse, Institute for Clinical Systems Improvement, U.S. Preventive Services Task Force, and Essential Evidence Plus. Search date: May 2, 2011, through May 6, 2011.

