Am Fam Physician. 2013;88(5):328-330
Author disclosure: No relevant financial affiliations.
Case Scenario
When I first began as a solo family physician in a small rural town, I got to know one of the residents, a shop owner, who became a patient. When we first met, she told me she was closing her shop as a result of being cheated by her business partners. About six years later, this same patient informed me that she had left her job at another establishment because the owners were not treating her fairly. I knew the owners, as they were also my patients, and her account was not consistent with their character. Four years later, this patient developed diabetes mellitus. Her diabetes was poorly controlled, and she always had an excuse as to why she could not change her eating habits, exercise, or take the medicine I prescribed. I noted this as a pattern of self-defeating behavior. She also reported having nightmares and difficulty sleeping. I suspected that some of her behaviors might have been caused by early childhood experiences—in particular, by sexual abuse or related trauma. I would like to talk with her about this. What is the best way to discuss this subject? If sexual trauma is revealed, how do I proceed?
Commentary
It is essential for physicians to understand the relevance of childhood sexual trauma to adult medical conditions. Recognizing this connection can help physicians begin to manage the resulting damage. Exposure to childhood sexual trauma is highly prevalent in the United States, but is vastly underreported.1,2 One in four females and one in six males experience sexual trauma before 18 years of age.3 One large study found that 22% of adult women were victims of past trauma, but only 3% of these patients ever revealed that fact to their primary care physician.1
The Adverse Childhood Experiences (ACE) study is one of the largest investigations to assess associations between childhood maltreatment and health and well-being later in life. This study found that the more types of childhood trauma a person experiences (i.e., the higher one's ACE score), the more likely a person will have a chronic disease in adulthood.4,5 The cumulative exposure of a person's developing brain to severe stress, combined with years of maladaptive coping behaviors to past trauma, puts patients at high risk of deteriorating health. The resulting impairment of multiple brain structures and functions can manifest in a variety of physical and psychiatric health outcomes (Table 16–8 ).
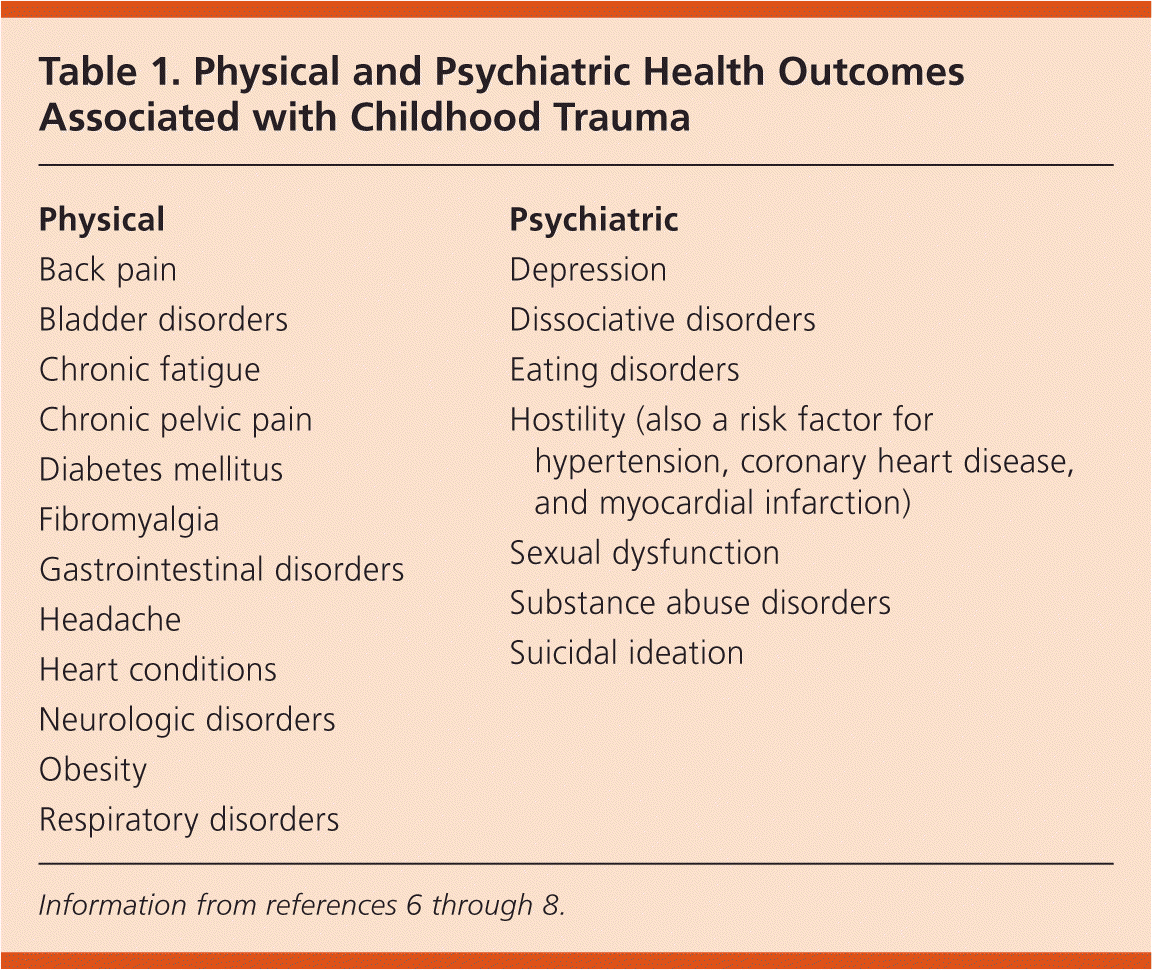
| Physical |
| Back pain |
| Bladder disorders |
| Chronic fatigue |
| Chronic pelvic pain |
| Diabetes mellitus |
| Fibromyalgia |
| Gastrointestinal disorders |
| Headache |
| Heart conditions |
| Neurologic disorders |
| Obesity |
| Respiratory disorders |
| Psychiatric |
| Depression |
| Dissociative disorders |
| Eating disorders |
| Hostility (also a risk factor for hypertension, coronary heart disease, and myocardial infarction) |
| Sexual dysfunction |
| Substance abuse disorders |
| Suicidal ideation |
A number of medical conditions have been reported to have higher prevalence among women with a history of sexual trauma, including sexually transmitted disease, pelvic inflammatory disease, diabetes, obesity, arthritis, asthma, irritable bowel syndrome, eating disorders, and hypertension.7
It is not uncommon for health care professionals to be anxious or nervous about broaching the subject of sexual trauma. Many have little experience doing so.2 Building a trusting physician-patient relationship over time often allows for gentle inquiry about past traumatic experiences.9 After trust has been established, there are some cues commonly cited in the literature that physicians can use to facilitate a brief, purposeful inquiry into childhood trauma. These cues include self-defeating or self-harming behavior, rage or uncontrolled anger, somatization disorder, and chronic pain in association with drug-seeking behavior.9 If appropriate, and in consultation with the patient, physicians can then make a referral for trauma-informed mental health counseling.
Referral and subsequent treatment can have substantial positive effects by improving patients' adherence to recommendations for disease prevention or self-management. Trauma-informed therapy has been shown to help patients develop better methods of coping and self-empowerment.9 The negative health effects of past trauma are apparent in the literature, and the effectiveness of trauma-informed care has been demonstrated for women with co-occurring mental health and substance abuse disorders.10,11
Most trauma survivors are not offended if they are asked open-ended empathetic questions, and instead feel relieved to talk about it.12 In numerous studies, many women have indicated that they would like to be asked about sexual trauma history.9,12 Simply asking a patient about a trauma history and responding empathetically to disclosure lets the patient feel validated and removes a mental barrier. As part of this initial discussion, it is important to convey the message that the abuse was not the patient's fault. Physicians can also talk about how common childhood sexual abuse is and the typical long-term effects of abuse.2 These may include the patient's symptoms.
In cases such as the one described here, physicians may continue to “spin their wheels” urging patients to take control of their health. But if the patient answers affirmatively to gentle inquiries about sexual trauma, it is likely that after the trauma is recognized and treated, she will be better able to follow recommended lifestyle changes and develop more effective self-management strategies.
Case Resolution
The patient in this scenario did have a history of childhood sexual abuse. She reported being abused by her grandfather, and that she had never shared this information before. It was hard for her to live with the resulting shame and anger. She agreed to attend counseling, and was referred to a therapist who specialized in trauma. The counseling went well, and from that point on, she cooperated with her medical treatment. She subsequently lost 25 lb, and her diabetes was much better controlled. In addition to improving her physical health, she found a new job where she has been able to excel.