A 29-year-old woman presented with an erythematous furuncle on her left leg that appeared three weeks earlier. She had a similar lesion near her left knee that healed spontaneously. She had a history of polycystic ovary syndrome and was taking oral contraceptives, metformin (Glucophage), and spironolactone (Aldactone). She used a whirlpool footbath during a pedicure two months earlier.
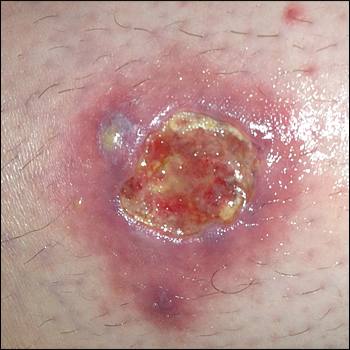
On examination, the patient was afebrile and had no lymphadenopathy or edema. There was a 1- to 2-cm, tender, nonfluctuant furuncle on the lateral portion of her left leg. She was prescribed oral trimethoprim/sulfamethoxazole twice daily, and incision and drainage were performed because the area became more fluctuant. After 10 days of antibiotics, an ulcer with seropurulent drainage and a sinus tract formed (see accompanying figure). Clindamycin was prescribed. A preliminary organism was identified on wound culture.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Erythema nodosum.
B. Methicillin-resistant Staphylococcus aureus (MRSA) skin infection.
C. Rapidly growing mycobacterial skin infection.
D. Venous stasis ulcer.
Discussion
The answer is C: rapidly growing mycobacterial skin infection. The nontuberculous mycobacteria that most commonly cause skin and soft tissue infections are Mycobacterium fortuitum, Mycobacterium abscessus, and Mycobacterium chelonae. These species can grow in a culture within one week. Infection typically results from direct inoculation and causes nodules, papules, or furuncles; lesions can be single but are often multiple. M. fortuitum and M. chelonae are more likely than M. abscessus to cause skin and soft tissue infections, and have been associated with exposure to nail salon whirlpool baths.1–4
In this patient, M. chelonae was isolated from the wound. Treatment requires prolonged antibiotic therapy. All three rapidly growing mycobacteria are resistant to several antibiotics.
Erythema nodosum presents as multiple painful, erythematous nodules, typically on the lower legs. Diagnosis is usually made clinically. It is associated with several autoimmune disorders, medication use (e.g., oral contraceptives, sulfa antibiotics), and infections.5 There is no fluctuance with erythema nodosum.
Most skin abscesses are caused by S. aureus. Incision and drainage may be sufficient for small abscesses, but antibiotics are necessary for more extensive infections.6 Community-acquired S. aureus infections are often caused by MRSA, which is resistant to betalactam antibiotics. Culture with sensitivities is necessary for definitive antibiotic treatment. MRSA skin infections typically present acutely as a fluctuant, erythematous furuncle or abscess, with or without cellulitis. Purulent drainage may be present.
Venous stasis ulcers occur in older persons who have had trauma to the lower extremity and who have a history of smoking. They are common between the knee and ankle and in the malleolar regions,7 and they have erythema and central ulceration with granulation tissue. The ulcers may occur with stasis dermatitis. The initial appearance of a fluctuant papule is not characteristic of venous stasis ulcers. Diagnosis is generally confirmed by history and physical examination findings, but biopsy may be necessary.
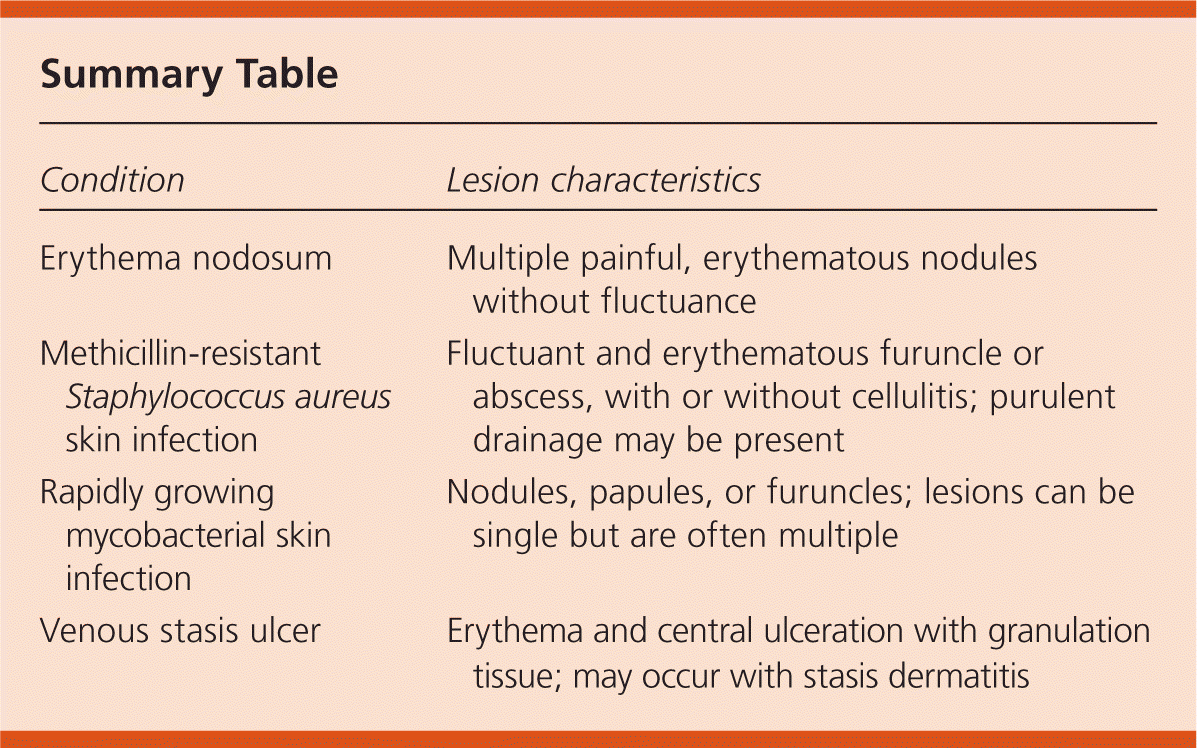
Summary Table
| Condition | Lesion characteristics |
|---|---|
| Erythema nodosum | Multiple painful, erythematous nodules without fluctuance |
| Methicillin-resistant Staphylococcus aureus skin infection | Fluctuant and erythematous furuncle or abscess, with or without cellulitis; purulent drainage may be present |
| Rapidly growing mycobacterial skin infection | Nodules, papules, or furuncles; lesions can be single but are often multiple |
| Venous stasis ulcer | Erythema and central ulceration with granulation tissue; may occur with stasis dermatitis |

