Given that nearly one-half of pregnancies are unintended, preconception care should be considered an integral part of primary care for women of reproductive age. Common issues in preconception care include family planning, achieving a healthy body weight, screening and treatment for infectious diseases, updating appropriate immunizations, and reviewing medications for teratogenic effects. Women who want to become pregnant should take folic acid supplements to reduce the risk of neural tube defects. Control of chronic diseases is essential for optimizing pregnancy outcomes. Family physicians should work with patients to control conditions such as diabetes mellitus, hypertension, and seizure disorders while simultaneously offering family planning services to avoid unintended pregnancies. Bariatric surgery is increasingly common and may improve fertility in many women with previous insulin resistance. Family physicians should counsel women undergoing bariatric surgery to prevent pregnancy during rapid weight loss and provide assistance with contraception. In addition, patients have special nutritional requirements after bariatric surgery.
The Centers for Disease Control and Prevention defines preconception care as a set of interventions aimed at identifying and modifying biomedical, behavioral, and social risks to a woman's health or pregnancy outcome through prevention and management. The goal is to ensure that the woman is as healthy as possible before conception to promote her health and the health of her future children. Preconception care is integral to primary care for women in their reproductive years. It is not a single medical visit, but rather should be incorporated into every medical decision and treatment recommendation for these women.1
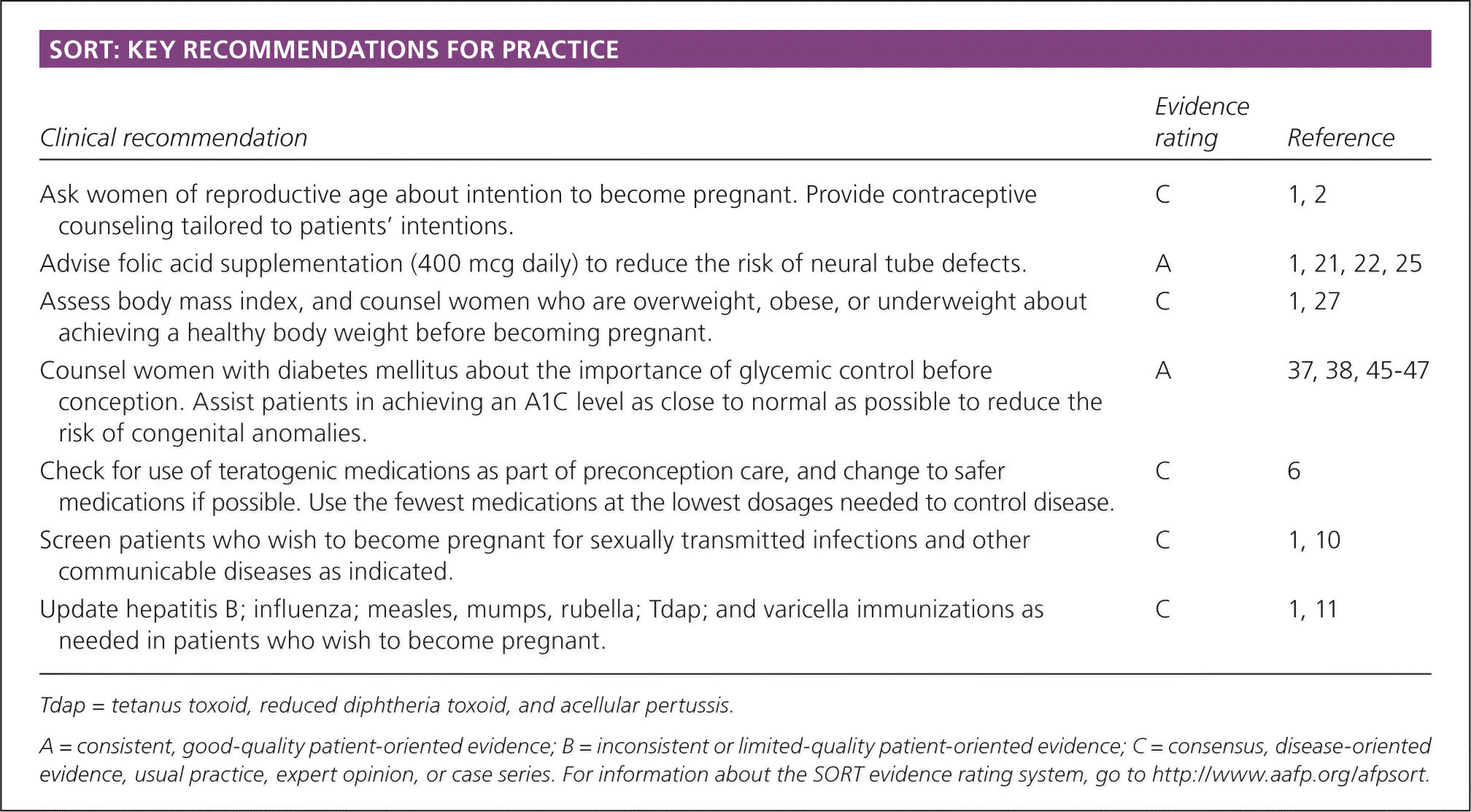
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Reference |
|---|---|---|
| Ask women of reproductive age about intention to become pregnant. Provide contraceptive counseling tailored to patients' intentions. | C | 1, 2 |
| Advise folic acid supplementation (400 mcg daily) to reduce the risk of neural tube defects. | A | 1, 21, 22, 25 |
| Assess body mass index, and counsel women who are overweight, obese, or underweight about achieving a healthy body weight before becoming pregnant. | C | 1, 27 |
| Counsel women with diabetes mellitus about the importance of glycemic control before conception. Assist patients in achieving an A1C level as close to normal as possible to reduce the risk of congenital anomalies. | A | 37, 38, 45–47 |
| Check for use of teratogenic medications as part of preconception care, and change to safer medications if possible. Use the fewest medications at the lowest dosages needed to control disease. | C | 6 |
| Screen patients who wish to become pregnant for sexually transmitted infections and other communicable diseases as indicated. | C | 1, 10 |
| Update hepatitis B; influenza; measles, mumps, rubella; Tdap; and varicella immunizations as needed in patients who wish to become pregnant. | C | 1, 11 |
Tdap = tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Nearly one-half of all pregnancies in the United States are unintended. Family planning is an essential component of preconception care and allows optimal opportunity for health promotion and preventive care. Primary care clinicians should consider asking all patients of reproductive age about intention to become pregnant and providing contraceptive counseling tailored to patients' intentions.1,2
The Centers for Disease Control and Prevention's U.S. medical eligibility criteria for contraceptive use can assist clinicians in counseling patients about contraceptive choices, and provides evidence-based guidance on the safety of contraceptive methods for women with specific characteristics and medical conditions.3 All women and men should be encouraged to develop a reproductive life plan, including individual goals about childbearing and a plan for achieving them.1 Reproductive life planning tools are available for patients and clinicians at https://www.cdc.gov/preconception/planning.html.
For primary care physicians, caring for a woman of reproductive age should include identifying health risks to her and her future children, and implementing interventions to reduce these risks. General issues in preconception care are summarized in Table 1.4–9 Screening and treatment for infectious diseases, and providing appropriate immunizations are also important in these patients (Table 2).1,10–20 [ corrected]
Table 1. General Issues in Preconception Care

| Issue | Recommendations |
|---|---|
| Environmental exposures | Assess for workplace exposures to toxicants; industries that are known to use toxic chemicals include clinical and laboratory health care, dry cleaning, printing, manufacturing, and agriculture |
| Assess for household exposures to potentially harmful agents such as heavy metals, solvents, and pesticides | |
| Counsel patients about avoiding mercury exposure by not consuming large fish (e.g., shark, swordfish, tilefish, king mackerel) and limiting other fish intake4 | |
| Family genetic history | Screen for personal or family history of congenital anomalies or genetic disorders |
| Refer couples for genetic counseling when risk factors are identified, and provide carrier testing when appropriate to determine risk to future pregnancy5 | |
| Medications | Assess for the use of teratogenic medications |
| For women with chronic diseases, switch to safer medications when possible, and use the fewest medications at the lowest dosages needed to control the disease6 | |
| Psychiatric illness | Screen for depression and anxiety disorders |
| Counsel patients about the risks of untreated depression during pregnancy, as well as the risks of treatment7 | |
| Psychosocial factors | Screen for intimate partner violence |
| Evaluate the patient's safety, and provide referral to appropriate resources8 | |
| Substance use | Screen for alcohol use, and provide referral for women with alcohol dependence |
| Screen for tobacco use, and provide smoking cessation treatment when needed; counsel patients about the effect of smoking on pregnancies and child health | |
| Provide brief behavioral interventions to reduce tobacco, alcohol, and drug use9 |
Table 2. Infectious Disease Screening and Immunizations in Preconception Care

| Screening/immunization | Recommendations |
|---|---|
| Infectious disease | |
| Chlamydia12 | Screen all women younger than 25 years and women who are at risk of infection |
| Treat infected patients | |
| Gonorrhea13 | Screen high-risk women |
| Treat infected patients | |
| Herpes simplex virus infection | Counsel about the risk of vertical transmission |
| Human immunodeficiency virus infection14 | Universal screening |
| Counsel about the risk of vertical transmission (treatment reduces this risk) | |
| Syphilis15 | Screen high-risk women |
| Treat infected patients | |
| Tuberculosis | Screen high-risk women |
| Treat women with active and latent disease before pregnancy | |
| Immunization | |
| Hepatitis B16 | Vaccinate all high-risk women before pregnancy |
| Counsel chronic carriers about prevention of vertical transmission | |
| Influenza17 | Vaccinate all women who will be pregnant during influenza season and women at risk of influenza-related complications |
| Measles, mumps, rubella18 | Screen for immunity |
| Vaccinate all nonimmune women who are not pregnant | |
| Counsel patients to avoid pregnancy for three months after vaccination | |
| Tetanus, diphtheria, pertussis19 | Tetanus vaccination may protect against neonatal tetanus |
| Vaccinate with Tdap during pregnancy (optimal timing is 27 to 36 weeks' gestation) to reduce the risk of neonatal pertussis | |
| Varicella20 | Screen for immunity |
| Vaccinate all nonimmune women who are not pregnant | |
| Counsel patients to avoid pregnancy for one month after vaccination | |
Tdap = tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis.
Nutritional Considerations
FOLIC ACID
Folic acid supplementation of 400 mcg daily started before pregnancy and continued until six to 12 weeks postconception reduces the rate of neural tube defects by nearly 75%.1,21,22 One study showed that women receiving preconception counseling from their primary care physicians are five times more likely to take folic acid before conception.23 Women taking folic acid antagonists or who have carried a fetus affected by a neural tube defect or other birth defects linked with folic acid deficiency (e.g., oral facial cleft, structural heart disease, limb defect, urinary tract anomaly, hydrocephalus) should take 4 to 5 mg of folic acid daily starting three months before conception and continuing until 12 weeks postconception.24,25 Women with certain health risks (e.g., epilepsy, insulin-dependent diabetes mellitus, obesity with a body mass index [BMI] greater than 35 kg per m2, family history of a neural tube defect) should also take this higher dosage.24
OVERWEIGHT
In the United States, 26% of women 20 to 39 years of age are overweight (BMI of 25 to 29.9 kg per m2), and 29% are obese (BMI of 30 kg per m2 or higher).26 Women who are overweight or obese are at risk of diabetes, gestational diabetes, and hypertension. These conditions are associated with adverse pregnancy outcomes, including macrosomia, shoulder dystocia, operative delivery, congenital anomalies, intrauterine growth restriction, spontaneous abortion, stillbirth, preeclampsia, and eclampsia.27
There are numerous effective interventions for women who are overweight or obese. A systematic review found that out of five commercial diets, Weight Watchers was the least costly, and women maintained a 3.2% weight loss two years after intervention. The review noted that medically supervised programs are more expensive and have higher rates of attrition, but are associated with greater weight loss (15% to 25%), compared with other types of programs.28
Women who are overweight or obese are more likely to have difficulty with conception because of insulin resistance and oligomenorrhea. Weight loss and medications can improve these symptoms, as well as fertility.29,30
BARIATRIC SURGERY
There were 220,000 bariatric surgeries in 2008; one-half were performed in women of reproductive age.31 Many women undergoing gastric surgery have a history of oligomenorrhea or amenorrhea from insulin resistance, and they should be advised that fertility may return as they lose weight. Women are generally directed to prevent pregnancy for 12 to 18 months after surgery to stabilize weight loss and optimize nutrition status,32 but observational studies have shown that the time from surgery to conception does not increase obstetric and neonatal complications.33 Oral contraceptives may be less effective after malabsorptive bariatric surgery.
There is little evidence-based data to guide preconception care of women who have had bariatric surgery. These patients are at risk of nutrient deficiencies, including vitamins A, D, E, K, C, B1, B6, B12; folic acid; and iron. It is generally recommended that they take at least two multivitamins per day in addition to extra iron (approximately 65 mg), folic acid (400 mcg), vitamin D (400 to 800 IU), and vitamin B12 (350 mcg). Women should be assessed for common nutrient deficiencies before pregnancy with a complete blood count.31,32
UNDERWEIGHT
Low prepregnancy weight (BMI less than 18.5 kg per m2) is associated with preterm birth and low birth weight. Low body weight is also associated with nutrient deficiencies, osteoporosis, amenorrhea, infertility, and arrhythmias. Infants whose mothers had low prepregnancy body weight are at higher risk of gastroschisis. Women with low BMI should be assessed for eating disorders and counseled about how being underweight can affect their health and pregnancy.1,34
Chronic Medical Conditions
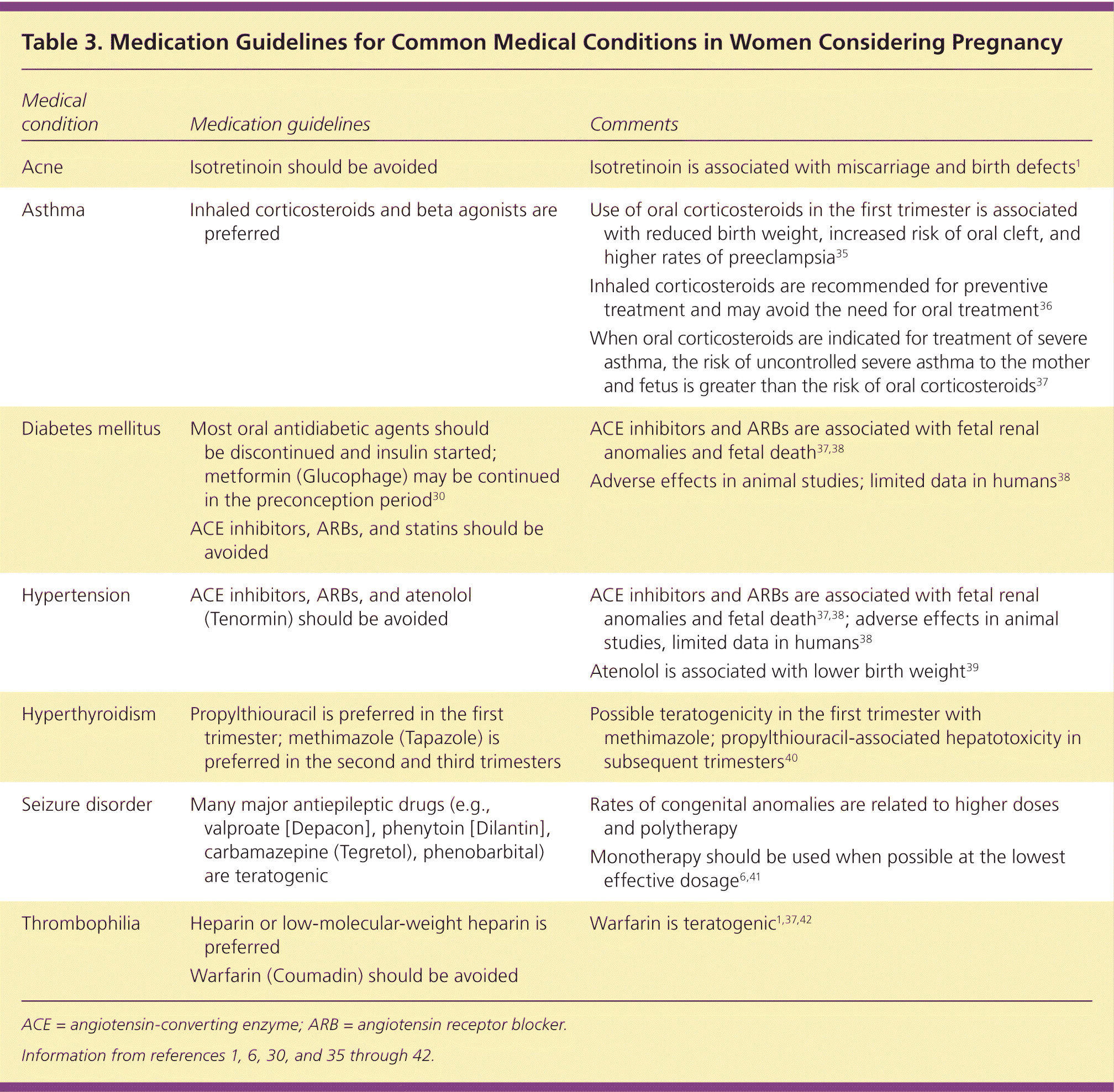
Table 3 includes preferred medications for chronic diseases and those to avoid during pregnancy.1,6,30,35–42
Table 3. Medication Guidelines for Common Medical Conditions in Women Considering Pregnancy
| Medical condition | Medication guidelines | Comments |
|---|---|---|
| Acne | Isotretinoin should be avoided |
|
| Asthma | Inhaled corticosteroids and beta agonists are preferred |
|
| Diabetes mellitus | Most oral antidiabetic agents should be discontinued and insulin started; metformin (Glucophage) may be continued in the preconception period30 | |
| ACE inhibitors, ARBs, and statins should be avoided | ||
| Hypertension | ACE inhibitors, ARBs, and atenolol (Tenormin) should be avoided | |
| Hyperthyroidism | Propylthiouracil is preferred in the first trimester; methimazole (Tapazole) is preferred in the second and third trimesters |
|
| Seizure disorder | Many major antiepileptic drugs (e.g., valproate [Depacon], phenytoin [Dilantin], carbamazepine (Tegretol), phenobarbital) are teratogenic | |
| Thrombophilia | Heparin or low-molecular-weight heparin is preferred | |
| Warfarin (Coumadin) should be avoided |
ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker.
DIABETES
Diabetes is the most common serious disease to affect the maternal-fetal dyad. The disease affects nearly 10% of women of reproductive age,43 and about 1% of pregnancies are complicated by pregestational diabetes.37 Pregestational diabetes increases the risk of miscarriage, congenital fetal anomalies, and perinatal death.44
Glucose is teratogenic at high levels, and rates of congenital fetal anomalies are directly related to glycemic control in the first trimester. Good glycemic control during organogenesis reduces rates of congenital malformations.44–46 Preconception A1C levels should approach those considered normal in patients without diabetes; national organizations recommend varying targets of 7% or lower.38,47 Pregnancy is associated with higher rates of hypoglycemia, decreased hypoglycemic awareness, increased rates of diabetic ketoacidosis, and the progression of diabetic retinopathy and nephropathy.38
Preconception counseling improves pregnancy outcomes in women with diabetes and should be part of diabetes care for reproductive-aged women. Preconception care should include educating women about the impact of diabetes on pregnancy outcomes and the impact of pregnancy on diabetes,38 optimizing glycemic control, screening for vascular complications of diabetes, evaluating medication use, and encouraging effective family planning.37
HYPERTENSION
Chronic hypertension affects 3% of women of reproductive age.43 Chronic hypertension in pregnancy is associated with higher rates of preterm birth, placental abruption, intrauterine growth restriction, preeclampsia, and fetal death.48 Women with chronic hypertension are at risk of worsening hypertension and end-organ damage, and 25% of women with hypertension develop superimposed preeclampsia during pregnancy.49
Pregnancy outcome is related to the degree of hypertension.50 There is no evidence that treating mild to moderate hypertension in pregnancy improves perinatal outcomes.48 Treating severe hypertension (systolic blood pressure of 180 mm Hg or higher, or diastolic blood pressure of 110 mm Hg or higher) improves pregnancy outcomes.51
Caring for women of reproductive age with hypertension should include educating them about the risks of hypertension during pregnancy and that their medication regimen may need to be changed before conception. Women with long-standing hypertension who are planning pregnancy should be assessed for retinopathy, renal disease, and ventricular hypertrophy.37
THYROID DISEASE
Thyroid disease can significantly impact pregnancy outcomes. Hypothyroidism affects 2.5% of women of reproductive age, and even more have subclinical disease.52 Many patients with hypothyroidism are inadequately treated. Hypothyroidism in the first trimester is associated with cognitive impairment in children. Hypothyroidism (clinical and subclinical) in pregnant women increases the risk of preterm birth, low birth weight, placental abruption, and fetal death.53,54
Women who are adequately treated before pregnancy and those diagnosed and treated early in pregnancy have no increased risk of perinatal morbidity.55 It is essential to monitor women on thyroid replacement therapy and educate them about its impact on pregnancy. During pregnancy, thyroid replacement dosages typically need to be increased by four to six weeks' gestation, possibly by 30% or more. Routine screening for subclinical hypothyroidism is not recommended; however, women with risk factors and symptoms of thyroid diseases should be screened, and subclinical hypothyroidism should be treated.40
Hyperthyroidism can result in significant maternal and neonatal morbidity, and outcomes correlate with disease control. Guidelines recommend achieving euthyroidism before pregnancy.40
ASTHMA
Women with poorly controlled asthma before pregnancy are more likely to experience worsening symptoms during pregnancy.56 Poorly controlled asthma poses risks to the fetus, such as neonatal hypoxia, intrauterine growth restriction, preterm birth, low birth weight, and fetal and neonatal death.57 Preconception care should focus on optimizing asthma control with medications, and identifying and reducing exposure to allergens. Patients should be counseled on smoking cessation and avoidance of secondhand smoke exposure.6
THROMBOPHILIA
Women with thrombophilia are more likely to develop venous and arterial clots during pregnancy and are at risk of preeclampsia. Effects on the fetus include placental infarction, intrauterine growth restriction, placental abruption, recurrent miscarriage, fetal stroke, and fetal death.42 Warfarin (Coumadin), an anticoagulant commonly used in the treatment of thrombophilia, is teratogenic. It is important to educate women with thrombophilia about the risks of pregnancy so that they can make informed decisions about conception. Preconception care allows women to change to a treatment regimen that is safer for the fetus before pregnancy and to consider genetic testing for inherited thrombophilia.37
SEIZURE DISORDERS
Seizure disorders are the most common neurologic diseases to affect pregnant women, and both the diseases and its treatments can adversely affect pregnancy. Approximately one-third of women with a seizure disorder will experience more frequent seizures in pregnancy. Seizure disorders are associated with miscarriage, low birth weight, developmental disabilities, microcephaly, and hemorrhagic disease of the newborn (induced by antiepileptic drugs). Seizure disorders increase the risk of congenital anomalies, whether or not the mother is taking medication.41 Given increased rates of neural tube defects with many antiepileptic drugs, supplementation with 4 mg of folic acid daily should be initiated at least one month before conception and continued in the first trimester.37
Approach to the Patient
A 32-year-old woman with diabetes and hypertension presented for follow-up. She was interested in gastric bypass surgery. Her blood pressure was 154/89 mm Hg, her BMI was 41 kg per m2, and her A1C level was 7.9%. She was taking metformin (Glucophage) and lisinopril (Zestril). She had never been pregnant and was not using contraception. She would like to have children, but had been unable to conceive for many years and considered herself infertile.
The patient was encouraged to develop a reproductive life plan, and she and her partner determined that they wished to delay having children until she was healthier. After discussion of her contraceptive options, she elected to have an intrauterine device (Mirena) placed. She was counseled about dietary changes, physical activity, and weight loss, and was referred for evaluation for gastric bypass surgery. Her medications were titrated to optimize treatment of diabetes and hypertension, with a goal of discontinuing medications when she lost weight.
One year after surgery, the patient's BMI was 29 kg per m2, and she no longer required medications for diabetes or hypertension. Her A1C level was 6.5%. She had been taking multiple vitamins, including folic acid, since her surgery to avoid nutrient deficiencies, and she wished to have her intrauterine device removed.
For more information on preconception care, visit https://www.cdc.gov/ncbddd/index.html and http://www.beforeandbeyond.org.
Data Sources: A PubMed search was completed in Clinical Queries using the keyword preconception care, alone and with chronic disease, diabetes, hypertension, thyroid disease, seizure disorder, asthma, thrombophilia, obesity, underweight, bariatric surgery, weight loss, nutrition, folic acid, diet, immunization, and infectious disease. PubMed searches were completed using the term pregnancy with chronic disease, diabetes, hypertension, thyroid disease, seizure disorder, asthma, thrombophilia, immunization, and infectious disease. PubMed searches were completed using the term obstetrics with obesity, underweight, bariatric surgery, weight loss, nutrition, folic acid, and diet. Also searched were the Cochrane database, Essential Evidence Plus, the Agency for Healthcare Research and Quality evidence reports, and UpToDate. Search dates: December 15, 2011; February 1, 2012; and August 5, 2013.

