Palliative care improves the quality of life for patients with a life-threatening illness and for their families. It aims to relieve suffering by identifying, assessing, and treating pain and other physical, psychosocial, and spiritual problems. Palliative care can be provided whether an illness is potentially curable, chronic, or life-threatening; is appropriate for patients with noncancer diagnoses1; and can be administered in conjunction with curative-aimed therapies at any stage of the illness. Hospice is a type of palliative care provided when curative treatment is no longer beneficial or desired, and when life expectancy is measured in months or less. It supports patients and their families while focusing on symptom relief and comfort.
Despite documented benefits, palliative care is underutilized in the management of advanced or terminal illnesses. It is estimated that more than 1 million deaths (or 45% of all deaths in the United States) in 2011 occurred in patients who were in a hospice program.2 Although this represents a gradual upward trend, 36% of those patients died or were discharged within seven days of admission, and nearly two-thirds (63%) received hospice care for less than one month.
Benefits
Hospice care provides better symptom management and quality of life compared with usual (cure-directed) care (Table 13 ). Studies show that patients who receive hospice care have improved quality of life, with less depression and symptom burden; feel more in control; are able to avoid risks associated with treatment and hospitalization; and have decreased costs with improved utilization of health care resources.4–6 Benefits also extend to caregivers, family, and friends, which demonstrates greater satisfaction with the quality of care and attention to caregiver needs.7,8 Paradoxically, in a widely publicized study of patients with metastatic non–small-cell lung cancer, those who received palliative care had improved survival rates compared with matched controls who received standard treatment.9
Table 1. World Health Organization Definition of Palliative Care

| Provides relief from pain and other distressing symptoms |
| Affirms life and regards dying as a normal process |
| Intends neither to hasten nor postpone death |
| Integrates the psychological and spiritual aspects of patient care |
| Offers a support system to help patients live as actively as possible until death |
| Offers a support system to help the family cope during the patient's illness and in their own bereavement |
| Uses a team approach to address the needs of patients and their families, including bereavement counseling, if indicated |
| Enhances quality of life and may positively influence the course of illness |
| Is applicable early in the course of illness, in conjunction with therapies that are intended to prolong life (e.g., chemotherapy, radiation therapy), and includes investigations needed to better understand and manage distressing clinical complications |
Adapted with permission from World Health Organization. WHO definition of palliative care. http://www.who.int/cancer/palliative/definition/en. Accessed November 20, 2012.
Barriers
Several factors may account for the underutilization of hospice care, including confusion about terminology, misperception about its intent and scope, concerns about cost and insurance coverage, and potential mistrust because of perceived economic motives10,11 (Table 210–14 ). A lack of physician comfort with end-of-life conversations, including the fear of depriving patients of hope, can also create a barrier to hospice referrals.15
Table 2. Potential Barriers and Solutions to Physician Referrals for Palliative Care

| Barrier | Solution |
|---|---|
| Confusion about terminology (e.g., hospice vs. palliative care); misperceptions about the intent and scope of hospice care (thought to be for patients with only terminal malignant diagnoses [e.g., cancer], or administered only in inpatient hospice centers rather than at home or in skilled nursing facilities); fear that palliative care will deny the patient of life-prolonging therapy; concerns about compromised access to costly and life-prolonging treatments (e.g., radiation and chemotherapy, transfusions, antibiotics, hyperalimentation)10,11 | Clarify that decisions are flexible and are ultimately made by a local hospice program, in conjunction with the patient, his or her family, and the primary care physician |
| Mistrust of health care professionals; perception that hospice care is economically motivated (concern about health care rationing)11 | Explain that the cost of hospice care is likely equal to that of usual care |
| Prognostic uncertainty (unpredictable disease trajectories, often with waxing and waning courses; physician overestimation of remaining life expectancy)12 | Educate physicians about illness trajectories, prognostic indicator tools, and current hospice admission guidelines for patients with noncancer diagnoses; promote early, clear communication with patients |
| Psychology of decision making (patients and physicians tend to have a bias toward optimism)13,14 | Contextualize decisions in terms of goals of care; discuss advance care planning periodically during routine office visits |
Uncertainty about prognosis poses an additional challenge for physicians. Studies show that although the physician–patient relationship provides a meaningful context for addressing end-of-life issues, the degree of uncertainty about prognosis directly correlates with the longevity of this relationship.12 Insufficient training for physicians and nurses, including a lack of familiarity with various prognostic tools, may also have a role.
A more subtle barrier surrounds the psychology of decision making. Patients tend to be overly optimistic, believing that prescribed treatments will cure even incurable diseases.13 For physicians, the fear of causing harm by failing to do something may overshadow the fear of actively doing something harmful (i.e., therapeutic optimism).14
Best Practices
To achieve the goal of improved hospice utilization when appropriate, some guidelines recommend that palliative care be incorporated into standard-of-care treatment approaches.16,17 One validated model that has been proven effective in patients with terminal illness includes the following actions: stating the prognosis at the first visit; appointing someone in the physician's office to ensure that advance directives are discussed; scheduling a hospice information visit within the first three visits; and offering to discuss the patient's prognosis, coping strategies, and goals of care at each transition.18
Physicians should contextualize decisions around goals of care, which preserves hope and optimism but reorients treatment toward appropriate aims. Palliative care should be part of a broader continuum of care, thereby avoiding abrupt changes in the medical course. Family physicians are well-positioned to discuss advance care planning during routine office visits; several increasingly nuanced approaches are available to facilitate this discussion (eTable A).
eTable A. Resources for Hospice and Palliative Care
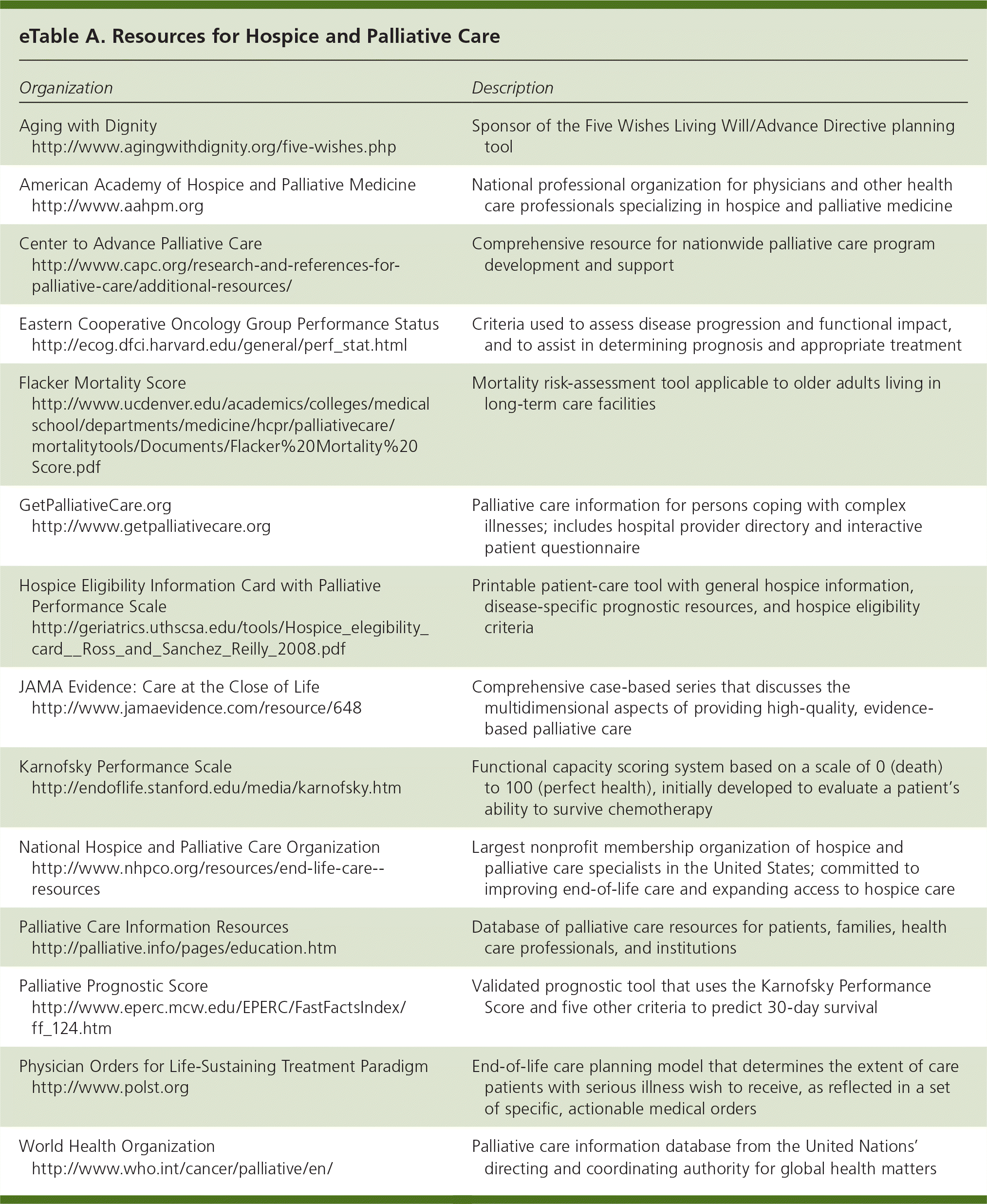
| Organization | Description | |
|---|---|---|
| Aging with Dignity | Sponsor of the Five Wishes Living Will/Advance Directive planning tool | |
| http://www.agingwithdignity.org/five-wishes.php | ||
| American Academy of Hospice and Palliative Medicine | National professional organization for physicians and other health care professionals specializing in hospice and palliative medicine | |
| http://www.aahpm.org | ||
| Center to Advance Palliative Care | Comprehensive resource for nationwide palliative care program development and support | |
| http://www.capc.org/research-and-references-for-palliative-care/additional-resources/ | ||
| Eastern Cooperative Oncology Group Performance Status | Criteria used to assess disease progression and functional impact, and to assist in determining prognosis and appropriate treatment | |
| http://ecog.dfci.harvard.edu/general/perf_stat.html | ||
| Flacker Mortality Score | Mortality risk-assessment tool applicable to older adults living in long-term care facilities | |
| http://www.ucdenver.edu/academics/colleges/medicalschool/departments/medicine/hcpr/palliativecare/mortalitytools/Documents/Flacker%20Mortality%20Score.pdf | ||
| GetPalliativeCare.org | Palliative care information for persons coping with complex illnesses; includes hospital provider directory and interactive patient questionnaire | |
| http://www.getpalliativecare.org | ||
| Hospice Eligibility Information Card with Palliative Performance Scale | Printable patient-care tool with general hospice information, disease-specific prognostic resources, and hospice eligibility criteria | |
| http://geriatrics.uthscsa.edu/tools/Hospice_elegibility_card__Ross_and_Sanchez_Reilly_2008.pdf | ||
| JAMA Evidence: Care at the Close of Life | Comprehensive case-based series that discusses the multidimensional aspects of providing high-quality, evidence-based palliative care | |
| http://www.jamaevidence.com/resource/648 | ||
| Karnofsky Performance Scale | Functional capacity scoring system based on a scale of 0 (death) to 100 (perfect health), initially developed to evaluate a patient's ability to survive chemotherapy | |
| http://endoflife.stanford.edu/media/karnofsky.htm | ||
| National Hospice and Palliative Care Organization | Largest nonprofit membership organization of hospice and palliative care specialists in the United States; committed to improving end-of-life care and expanding access to hospice care | |
| http://www.nhpco.org/resources/end-life-care--resources | ||
| Palliative Care Information Resources | Database of palliative care resources for patients, families, health care professionals, and institutions | |
| http://palliative.info/pages/education.htm | ||
| Palliative Prognostic Score | Validated prognostic tool that uses the Karnofsky Performance | |
| http://www.eperc.mcw.edu/EPERC/FastFactsIndex/ff_124.htm | Score and five other criteria to predict 30-day survival | |
| Physician Orders for Life-Sustaining Treatment Paradigm | End-of-life care planning model that determines the extent of care patients with serious illness wish to receive, as reflected in a set of specific, actionable medical orders | |
| http://www.polst.org | ||
| World Health Organization | Palliative care information database from the United Nations' directing and coordinating authority for global health matters | |
| http://www.who.int/cancer/palliative/en/ | ||
Family physicians should be familiar with disease trajectories of common chronic illnesses, as well as tools that aid in prognostication. There are several validated tools that rely on performance status in conjunction with other clinical indicators (e.g., Palliative Prognostic Score,19 Flacker Mortality Score20 eTable A), as well as disease-specific tools (e.g., Model for End-Stage Liver Disease,21 Charlson Comorbidity Index for End-stage Renal Disease22). The Patient-Reported Outcome Mortality Prediction Tool has had promising results in predicting six-month mortality in older adults, but still requires validation for routine clinical use.23 Institutions should also consider implementing protocols that trigger hospice referrals based on specific clinical features (e.g., repeated or lengthy hospitalization, decline in cognitive or functional status, unacceptable pain, emotional distress), and palliative care utilization should be a key quality measure. Physician and nursing education must continue to incorporate these elements in clinical training.
We should be careful to avoid blaming the patient or the physician for the ways in which end-of-life care is approached. For an illuminating perspective, see a video on end-of-life communication at http://www.youtube.com/watch?v=al2h_1cBnWw. A physician's desire to cure is often coupled with frustration over futility, and a patient's desire to live is balanced with a concern for comfort. These competing goals can create tensions among the patient, family, and physician. Adequate access to palliative measures, including early palliative care given in conjunction with curative therapy as part of a broader, guideline-directed management strategy, is one way that family physicians can balance these tensions.

