Purpose
In AFP Journal Club, three presenters review an interesting journal article in a conversational manner. These articles involve “hot topics” that affect family physicians or “bust” commonly held medical myths. The presenters give their opinions about the clinical value of the individual study discussed. The opinions reflect the views of the presenters, not those of AFP or the AAFP.
Article
Nwaru BI, Takkinen HM, Niemelä O, et al. Timing of infant feeding in relation to childhood asthma and allergic diseases. J Allergy Clin Immunol. 2013;131(1):78–86.
What does this article say?
Jill: This Finnish cohort study is a subanalysis of an original study that included 4,075 consecutively born infants with a human leukocyte antigen–conferred susceptibility to type 1 diabetes mellitus. They were followed until five years of age. Dietary records were kept to help determine influences on the onset of diabetes. This subanalysis of 3,781 patients (93% of the original cohort) evaluates whether the early introduction of specific foods affects a child's risk of developing asthma or other atopic conditions. The study included the following foods: cow's milk; roots (potatoes, carrots, and turnips); fruits and berries; wheat, rye, oats, barley, and other cereals; meat; fish; and eggs. The diagnoses of asthma, allergic rhinitis, or atopic eczema were assessed by parental report of physician diagnosis or treatment, and serum immunoglobulin E (IgE) levels were obtained to assess for atopic sensitization. Regression analysis adjusted for some other potential variables, such as parental history of asthma.
Asthma was diagnosed in 6.2% of the cohort, with allergic rhinitis occurring in 14% and atopic eczema in 37% of patients. Based on IgE levels, 38% were sensitized. Hazard ratios were calculated for the development of asthma, eczema, etc., using the cohort as its own control. The authors used different time periods for each comparison based on tertiles (or perhaps quartiles—the study authors are inconsistent) of when foods were introduced. For example, for cow's milk, they looked at introduction at about 1 to 4 months of age vs. older than 4 months, whereas for wheat, rye, oats, and barley, they looked at introduction at 5 to 5.5 months of age vs. older than 5.5 months. The authors claim that there may be some benefit from early exposure to potential allergens.
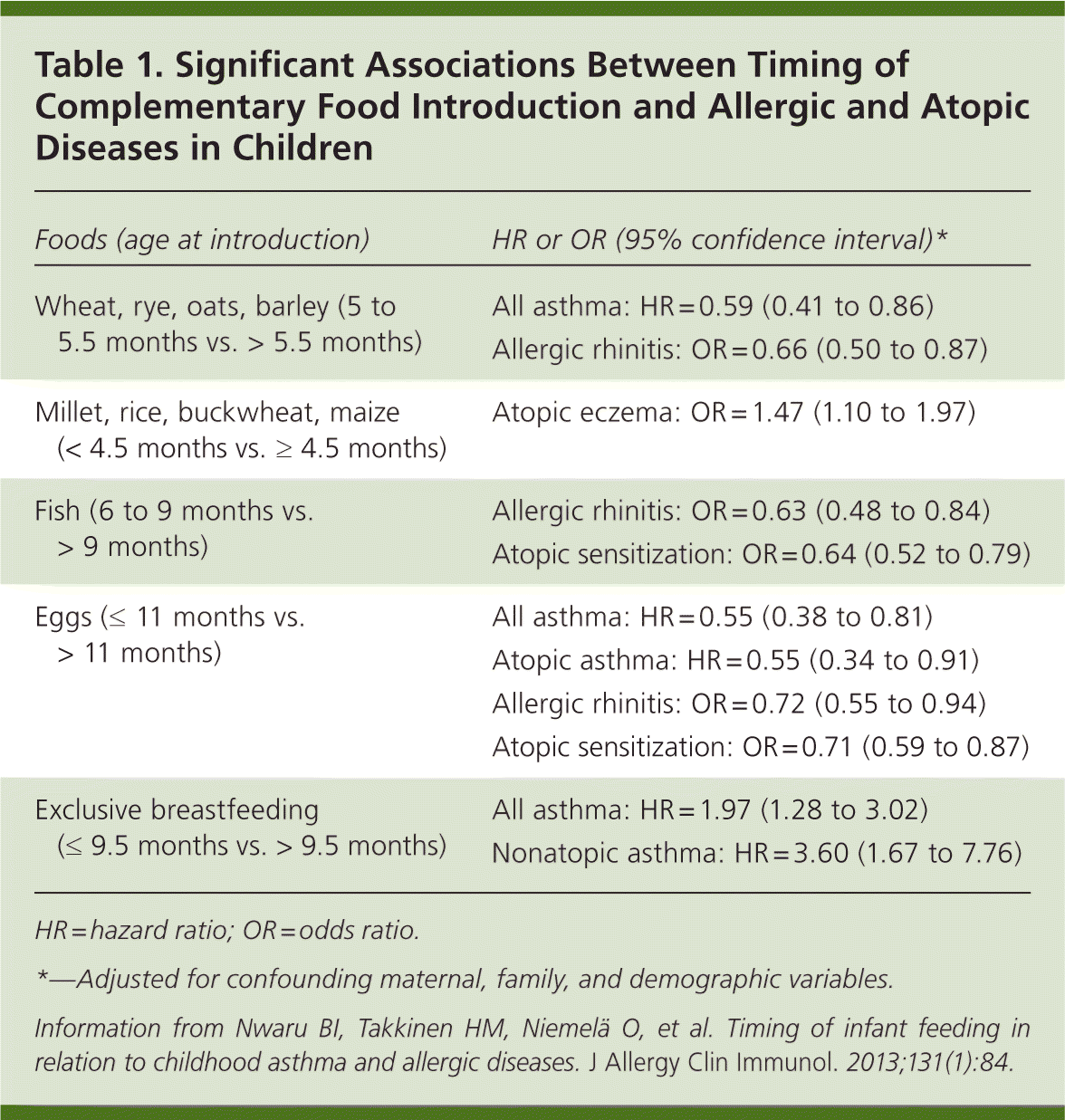
These results add to a growing body of evidence that challenges current policy recommendations (e.g., from the American Academy of Pediatrics, American Academy of Family Physicians, Centers for Disease Control and Prevention, and World Health Organization) and traditional wisdom about protecting infants' immature mucosal immune systems. Table 1 shows the significant associations between the timing of food introduction and allergic or atopic disease that were identified in this study. Similarly, the importance of exclusive breastfeeding has long been touted to help prevent asthma and atopic illnesses in children. This study suggests that the duration of breastfeeding, rather than its exclusivity, may be the most important protective factor (Table 1).
Table 1. Significant Associations Between Timing of Complementary Food Introduction and Allergic and Atopic Diseases in Children
| Foods (age at introduction) | HR or OR (95% confidence interval)* |
|---|---|
| Wheat, rye, oats, barley (5 to 5.5 months vs. > 5.5 months) | All asthma: HR = 0.59 (0.41 to 0.86) |
| Allergic rhinitis: OR = 0.66 (0.50 to 0.87) | |
| Millet, rice, buckwheat, maize (< 4.5 months vs. ≥ 4.5 months) | Atopic eczema: OR = 1.47 (1.10 to 1.97) |
| Fish (6 to 9 months vs. > 9 months) | Allergic rhinitis: OR = 0.63 (0.48 to 0.84) |
| Atopic sensitization: OR = 0.64 (0.52 to 0.79) | |
| Eggs (≤ 11 months vs. > 11 months) | All asthma: HR = 0.55 (0.38 to 0.81) |
| Atopic asthma: HR = 0.55 (0.34 to 0.91) | |
| Allergic rhinitis: OR = 0.72 (0.55 to 0.94) | |
| Atopic sensitization: OR = 0.71 (0.59 to 0.87) | |
| Exclusive breastfeeding (≤ 9.5 months vs. > 9.5 months) | All asthma: HR = 1.97 (1.28 to 3.02) |
| Nonatopic asthma: HR = 3.60 (1.67 to 7.76) |
HR = hazard ratio; OR = odds ratio.
*—Adjusted for confounding maternal, family, and demographic variables.
Information from Nwaru BI, Takkinen HM, Niemelä O, et al. Timing of infant feeding in relation to childhood asthma and allergic diseases. J Allergy Clin Immunol. 2013;131(1):84.
Should we believe this study?
Jill: This is a large cohort, with a good response rate and follow-up. The data collection is fairly robust, with repeated, timely assessments of complementary food introduction. Although a randomized controlled trial would be ideal, such a study would be difficult (if not impossible) to perform.
Mark: The study authors did a lot of comparisons, which introduces the likelihood of finding statistically significant differences by chance alone. The authors state that they accounted for this with “cautious interpretation of results.”
Bob: The biggest problem I have with this study (and many others in the allergy literature) is the use of a positive laboratory test result as an end point to indicate disease. In this study, 38% of the children tested positive for IgE. This suggests sensitization, but does not confirm a disease (i.e., allergy). In other words, the children had a positive IgE blood test result, but perhaps no clinical symptoms. This is precisely the reason the National Institute of Allergy and Infectious Diseases guidelines suggest an oral food challenge to confirm the presence of an allergy in children with a positive IgE blood test result.1 Case in point: A recent study demonstrated that only seven out of 79 children (9%) who tested positive for IgE to peanuts actually had an allergic reaction when given an oral food challenge.2
Jill: Reporting what proportion of sensitized children actually had symptoms would have made the results more relevant, statistically and clinically. The researchers did, however, control for some potential sources of bias. For example, the chance of recall bias was minimized with frequent nurse assessments of the timing of food introduction; they didn't just ask the parents to remember when they had introduced certain foods.
Mark: True, but reverse causation is also a consideration. Could the parents who noticed a tendency toward atopic disease have prolonged their breastfeeding or modified the timing of introduction of certain foods because they had prior knowledge about the risk of atopic sensitization? Other studies have demonstrated that this can affect results.3 And, some of the allergy vs. nonallergy groups differed by only two weeks of age. This does not make much physiologic sense.
Bob: Speaking of causation, we have to remember that association and causation are different. A cohort study like this can show associations. In this case, they do a decent job of establishing a temporal relationship. However, without randomization, it's really not possible to prove a causal relationship between the timing of introducing a specific food (or breastfeeding exclusivity or duration) and any of the outcomes.
Jill: One other concern is that this was part of a larger trial that included only infants with a specific human leukocyte antigen type. This is a pretty homogeneous population, and I wonder if these results are truly generalizable. There are many studies on the question of food introduction and atopy, and the results are not very consistent. Of course, part of the problem is that each study sets its own threshold for timing of complementary food introduction (three months, four months, six months). In this study, it is difficult to tell how they compared exposure timing. In some places they refer to tertiles, and in others quartiles.
What should the family physician do?
Jill: We should continue to advise the introduction of complementary food at six months of age while continuing to encourage breastfeeding, with slight modifications. When recommending exclusive breastfeeding in the first six months, we may want to focus less on how it may protect against atopic or allergic disorders, and more on the well-established benefits, such as preventing gastrointestinal diseases and enhancing immunity to infections in the infant, and weight loss and prolonged lactational amenorrhea in mothers.4 An infant's nutritional needs can be met with breastfeeding alone, and growth is not affected by delaying the introduction of complementary foods.
However, we should probably rethink our recommendations about introducing specific complementary foods and trying to identify ideal times for their introduction. These data support earlier introduction of specific allergenic foods in most low-risk infants.
Mark: Remember that some of these guidelines and recommendations exist for worldwide use. The recommendation to avoid complementary foods until six months of age, for example, also helps protect infants in impoverished countries where food and water are often contaminated or nutritionally inadequate. We have to make sure the results apply to a diverse patient population, and further investigate high-risk subgroups (e.g., children with familial predispositions to certain allergies).
Main Points
- Breastfeeding duration, rather than exclusivity, may be the most important factor in prevention of atopic diseases.
- Introducing fish, eggs, and certain cereals at intervals earlier than previously recommended may not increase the risk of asthma, allergies, and eczema by five years of age. Earlier introduction of these foods may help prevent allergic and atopic diseases, but these data are inconclusive.
EBM Points
- Reverse causation: In nonrandomized studies, participants may select their “intervention” behavior based on early symptoms or prior knowledge, which then may increase their risk of the outcome.
- Causation vs. association: A risk factor and outcome are associated if they occur together. Causation is more difficult to establish and requires randomization in most cases.
- Multiple comparisons: As the number of comparisons increases, it becomes more likely that the groups being compared will appear to differ in at least one attribute.
- Logistic regression attempts to control for confounders between the experimental groups or participants. However, it is at best inexact and cannot control for every potential confounder.

