Chronic daily headache is defined as the presence of a headache on 15 days or more per month for at least three months. The most common types of chronic daily headache are chronic migraines and chronic tension-type headaches. If a red flag for a secondary cause of headache is present, magnetic resonance imaging of the head should be performed. All patients should be asked about medication overuse, which can increase the frequency of headaches. Patients who overuse medications for abortive therapy for headache should be encouraged to stop the medications entirely and consider prophylactic treatment. Several prophylactic treatments for chronic daily headache can reduce headache frequency and severity, as well as improve overall quality of life. Nonpharmacologic treatments include relaxation techniques, cognitive behavior therapy, acupuncture, osteopathic manipulation, and cervical exercises. Pharmacologic therapies include amitriptyline, gabapentin, onabotulinumtoxinA, propranolol, tizanidine, topiramate, and valproate.
Chronic daily headache is defined as the presence of a headache on 15 days or more per month for at least three months.1 It is further divided into headaches of short or long duration (Table 1).2 Headaches of short duration are defined as lasting less than four hours, whereas headaches of long duration are defined as lasting more than four hours. This article follows a single illustrative case of a patient with chronic daily headache.
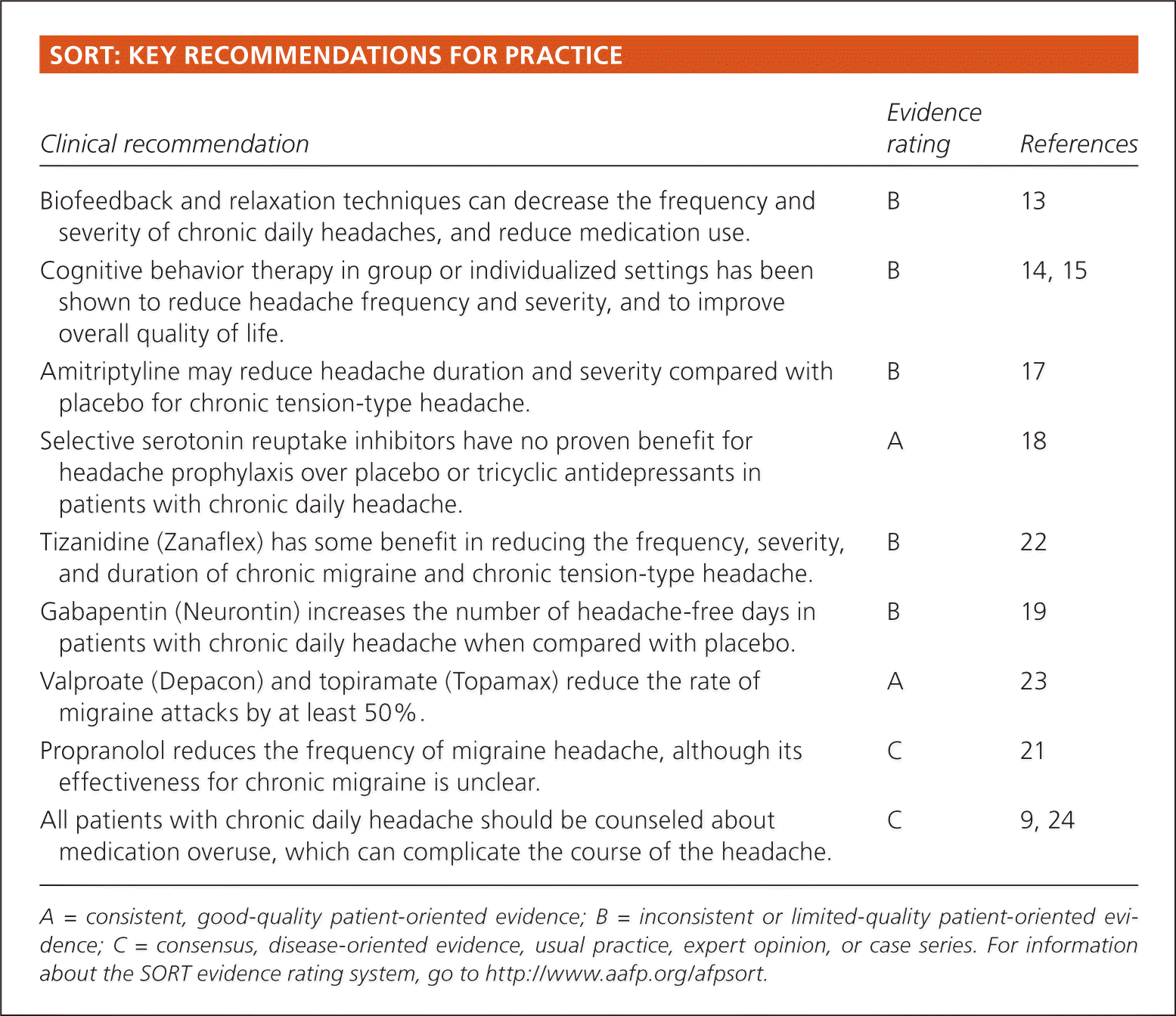
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Biofeedback and relaxation techniques can decrease the frequency and severity of chronic daily headaches, and reduce medication use. | B | 13 |
| Cognitive behavior therapy in group or individualized settings has been shown to reduce headache frequency and severity, and to improve overall quality of life. | B | 14, 15 |
| Amitriptyline may reduce headache duration and severity compared with placebo for chronic tension-type headache. | B | 17 |
| Selective serotonin reuptake inhibitors have no proven benefit for headache prophylaxis over placebo or tricyclic antidepressants in patients with chronic daily headache. | A | 18 |
| Tizanidine (Zanaflex) has some benefit in reducing the frequency, severity, and duration of chronic migraine and chronic tension-type headache. | B | 22 |
| Gabapentin (Neurontin) increases the number of headache-free days in patients with chronic daily headache when compared with placebo. | B | 19 |
| Valproate (Depacon) and topiramate (Topamax) reduce the rate of migraine attacks by at least 50%. | A | 23 |
| Propranolol reduces the frequency of migraine headache, although its effectiveness for chronic migraine is unclear. | C | 21 |
| All patients with chronic daily headache should be counseled about medication overuse, which can complicate the course of the headache. | C | 9, 24 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
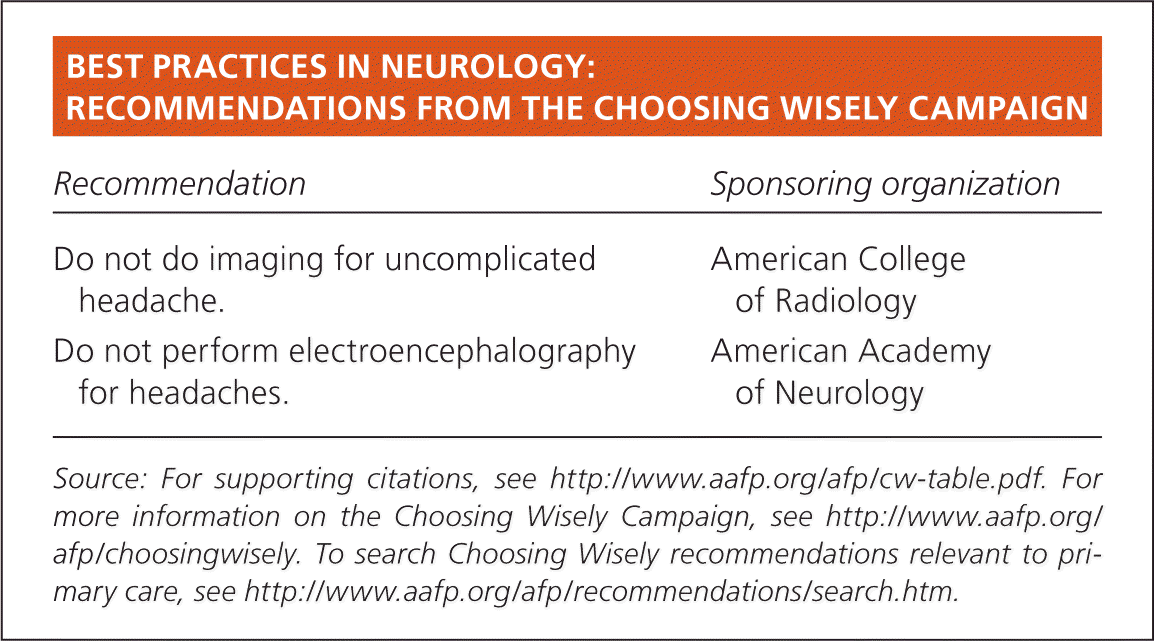
BEST PRACTICES IN NEUROLOGY: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN
| Recommendation | Sponsoring organization |
|---|---|
| Do not do imaging for uncomplicated headache. | American College of Radiology |
| Do not perform electroencephalography for headaches. | American Academy of Neurology |
Source: For supporting citations, see https://www.aafp.org/afp/cw-table.pdf. For more information on the Choosing Wisely Campaign, see https://www.aafp.org/afp/choosingwisely. To search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
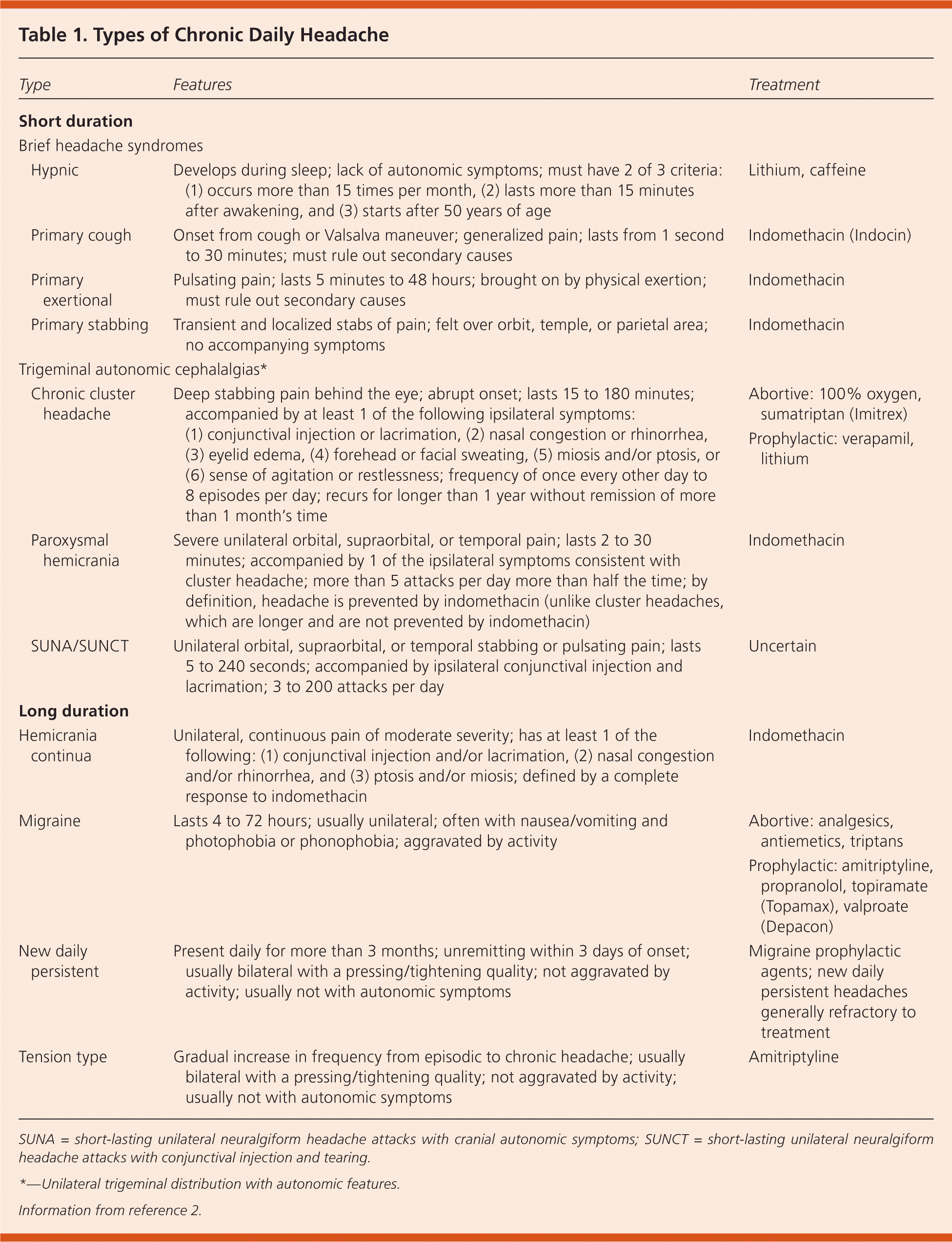
Table 1. Types of Chronic Daily Headache
| Type | Features | Treatment | |
|---|---|---|---|
| Short duration | |||
| Brief headache syndromes | |||
| Hypnic | Develops during sleep; lack of autonomic symptoms; must have 2 of 3 criteria: (1) occurs more than 15 times per month, (2) lasts more than 15 minutes after awakening, and (3) starts after 50 years of age | Lithium, caffeine | |
| Primary cough | Onset from cough or Valsalva maneuver; generalized pain; lasts from 1 second to 30 minutes; must rule out secondary causes | Indomethacin (Indocin) | |
| Primary exertional | Pulsating pain; lasts 5 minutes to 48 hours; brought on by physical exertion; must rule out secondary causes | Indomethacin | |
| Primary stabbing | Transient and localized stabs of pain; felt over orbit, temple, or parietal area; no accompanying symptoms | Indomethacin | |
| Trigeminal autonomic cephalalgias* | |||
| Chronic cluster headache | Deep stabbing pain behind the eye; abrupt onset; lasts 15 to 180 minutes; accompanied by at least 1 of the following ipsilateral symptoms: (1) conjunctival injection or lacrimation, (2) nasal congestion or rhinorrhea, (3) eyelid edema, (4) forehead or facial sweating, (5) miosis and/or ptosis, or (6) sense of agitation or restlessness; frequency of once every other day to 8 episodes per day; recurs for longer than 1 year without remission of more than 1 month's time | Abortive: 100% oxygen, sumatriptan (Imitrex) | |
| Prophylactic: verapamil, lithium | |||
| Paroxysmal hemicrania | Severe unilateral orbital, supraorbital, or temporal pain; lasts 2 to 30 minutes; accompanied by 1 of the ipsilateral symptoms consistent with cluster headache; more than 5 attacks per day more than half the time; by definition, headache is prevented by indomethacin (unlike cluster headaches, which are longer and are not prevented by indomethacin) | Indomethacin | |
| SUNA/SUNCT | Unilateral orbital, supraorbital, or temporal stabbing or pulsating pain; lasts 5 to 240 seconds; accompanied by ipsilateral conjunctival injection and lacrimation; 3 to 200 attacks per day | Uncertain | |
| Long duration | |||
| Hemicrania continua | Unilateral, continuous pain of moderate severity; has at least 1 of the following: (1) conjunctival injection and/or lacrimation, (2) nasal congestion and/or rhinorrhea, and (3) ptosis and/or miosis; defined by a complete response to indomethacin | Indomethacin | |
| Migraine | Lasts 4 to 72 hours; usually unilateral; often with nausea/vomiting and photophobia or phonophobia; aggravated by activity | Abortive: analgesics, antiemetics, triptans | |
| Prophylactic: amitriptyline, propranolol, topiramate (Topamax), valproate (Depacon) | |||
| New daily persistent | Present daily for more than 3 months; unremitting within 3 days of onset; usually bilateral with a pressing/tightening quality; not aggravated by activity; usually not with autonomic symptoms | Migraine prophylactic agents; new daily persistent headaches generally refractory to treatment | |
| Tension type | Gradual increase in frequency from episodic to chronic headache; usually bilateral with a pressing/tightening quality; not aggravated by activity; usually not with autonomic symptoms | Amitriptyline | |
SUNA = short-lasting unilateral neuralgiform headache attacks with cranial autonomic symptoms; SUNCT = short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing.
*—Unilateral trigeminal distribution with autonomic features.
Information from reference 2.
Case
A 30-year-old woman comes to your office seeking treatment for her headaches. She has had migraines since she was 14 years of age, but they have become more frequent over the past year. She now has a headache almost daily, making it difficult for her to concentrate at work. She was prompted to make this appointment after receiving a negative performance appraisal from her supervisor. The migraines have not changed in quality; they are typically right-sided and associated with blurry vision and nausea. Oral sumatriptan (Imitrex) used to effectively treat headaches that had already begun, but it no longer helps, even though she takes it almost daily. Her vital signs and appearance are unremarkable, and the results of her neurologic examination are normal.
Epidemiology
Headaches are common, affecting 50% of the general adult population at any given time, with a reported lifetime prevalence of 66% worldwide.1,3 Nearly one-half of those with acute headache have tension-type headaches, whereas 10% have migraines. Chronic daily headache is diagnosed in approximately 3% to 5% of patients presenting with acute headache.1,3 For patients with migraine, modifiable risk factors for progression to chronic migraine include obesity, medication overuse, stressful life events, snoring, caffeine overuse, and other causes of chronic pain.4
In the United States, chronic daily headache is 33% more common in whites and in women.5 The prevalence in women ranges from 5% to 9%, compared with 1% to 3% in men.5,6 In men and women, the prevalence of chronic daily headache is highest in those with lower total education levels.5,6 Overall, among persons who have chronic daily headache, 63% have used medication on 14 days or more of the month in an attempt to treat their headaches.6
Diagnosis
Patients who have chronic daily headache should provide a history and have a physical examination with a complete neurologic examination and medication review. Unless systemic symptoms are present, there is no role for laboratory testing. It is important to evaluate for red flags (Table 23,6 ) that may suggest a secondary cause of headache or a headache requiring more immediate evaluation. Table 3 lists some of the more common secondary causes of headache.3 It is important to keep in mind that the most pervasive secondary cause of chronic daily headache, medication overuse, often coexists with a primary headache syndrome. After other secondary causes have been ruled out, the clinical history helps determine what type of primary headache is present.
Table 2. Red Flags Suggestive of a Secondary Cause of Headache

| Red flag | Possible secondary etiologies |
|---|---|
| Headaches aggravated or relieved by assuming an upright or supine position | Intracranial hemorrhage |
| Headaches provoked by Valsalva maneuver | Arnold-Chiari malformation |
| History of sudden onset of headache | Subarachnoid hemorrhage |
| Onset of headache after 50 years of age | Brain neoplasm |
| Papilledema | Disorders with increased intracranial pressure (i.e., intracranial mass or bleed) |
| Presence of focal or lateralizing neurologic signs | Hemorrhagic stroke |
| Presence of systemic symptoms (i.e., weight loss, fevers, myalgias) | Giant cell arteritis, meningitis, encephalitis |
| Recent pregnancy | Postpartum preeclampsia |
Table 3. Secondary Causes of Headache

| Type | Examples |
|---|---|
| Infectious | Meningitis, sinusitis |
| Intracranial pressure disorders | Increased intracranial pressure from mass, decreased intracranial pressure from post–lumbar puncture headache |
| Medication related | Medication overuse headache, medication-induced adverse effects, intracranial hemorrhage secondary to anticoagulation |
| Metabolic | Hypoxia, obstructive sleep apnea |
| Neuralgias | Occipital or trigeminal neuralgia |
| Posttraumatic | Traumatic brain injury |
| Structural | Arnold-Chiari malformation; cervical spine, myofascial pain, or temporomandibular joint disorders |
| Vascular | Arterial aneurysm, cerebrovascular accident, giant cell arteritis, hypertensive urgency |
Adapted with permission from the American Academy of Neurology: Halker RB, Hastriter EV, Dodick DW. Chronic daily headache: an evidence-based and systematic approach to a challenging problem. Neurology. 2011;76(7 suppl 2):S38. Table 1 Causes of primary and secondary chronic daily headache on page S38. http://www.neurology.org/content/76/7_Supplement_2/S37.extract.
IMAGING
Imaging should be considered if red flags are present.7 The most useful test is magnetic resonance imaging (MRI), which is more sensitive than computed tomography for detecting many secondary causes of chronic daily headache. If there are no contraindications, MRI should be ordered with contrast media, particularly if there is concern for a mass. Computed tomography is more appropriate in the acute setting to rule out intracranial bleeding or mass effect. Primary headaches have no distinctive MRI findings.
SHORT-DURATION CHRONIC DAILY HEADACHE
Short-duration chronic daily headache includes trigeminal autonomic cephalalgias and brief headache syndromes (Table 1).2 Trigeminal autonomic cephalalgias have unilateral trigeminal distribution with autonomic features, and include chronic cluster headache, paroxysmal hemicrania, and short-lasting unilateral neuralgiform headache attacks with cranial autonomic symptoms or with conjunctival injection and tearing. Brief headache syndromes include hypnic, primary stabbing, primary cough, and primary exertional headaches. Trigeminal autonomic cephalalgias and brief headache syndromes are relatively rare and affect a small proportion of patients with chronic daily headache.8
LONG-DURATION CHRONIC DAILY HEADACHE
Most patients with long-duration chronic daily headaches have migraines or tension-type headaches. Other types of long-duration chronic daily headache include hemicrania continua and new daily persistent headache3 (Table 12 ).
Chronic migraines occur in patients with a history of migraines who have a rapid or gradual progression to chronic daily headache. The term “transformed migraine” has often been used to describe this headache, and patients commonly have a daily headache with flare-ups similar to their previous migraine.9 Overuse of abortive medication, including acetaminophen, nonsteroidal anti-inflammatory drugs, triptans, butalbital, caffeine, and narcotics, is found in two-thirds of patients, further complicating any treatment regimen.
Tension-type headaches are characterized by occipital or bilateral bandlike discomfort that builds slowly and may persist for several days. Unlike migraine, there is usually a lack of associated nausea or photophobia. It is important to note the time of progression from acute to chronic tension-type headaches; if the headache becomes constant within 72 hours, it should be classified as new daily persistent headache instead of the more slowly developing chronic tension-type headache. New daily persistent headache is generally more refractory to treatment than chronic tension-type headache. It is not uncommon for patients who progress to chronic daily headache to have symptoms characteristic of migraine and tension-type headaches, which can present difficulties for targeting a treatment regimen.7
Case Continued
After your patient expresses frustration that sumatriptan is no longer working, you explain that overusing the medication can make headaches more frequent. She is resistant to stopping sumatriptan therapy, but is willing to try a medication that prevents migraines. She is also surprised to hear about nonpharmacologic options that would allow her to avoid the adverse effects associated with medication.
Management
NONPHARMACOLOGIC THERAPIES
Several behavioral modifications are recommended for patients with chronic daily headache. These include cessation of caffeine and tobacco use, improved sleep hygiene, diet changes, and regular mealtimes. However, evidence supporting these modifications is lacking.3
One study examining regimens of low-load cervical exercises and osteopathic manipulation suggested some effectiveness for the treatment of “cervicogenic headache,”10 which, although not recognized by the International Headache Society, suggests that further study is needed to better understand whether these modalities can also be effective for International Headache Society–classified headache types. Acupuncture also has proven effective for reducing the frequency of headaches in persons with both migraine and tension-type headache, although no significant difference was detected between acupuncture and a sham procedure when looking at persons with migraine alone.11,12
There is a growing body of evidence to suggest that various psychotherapeutic regimens can be effective in decreasing disability for those with chronic daily headache, including Internet-based biofeedback and relaxation techniques that have been shown to decrease headache frequency and severity, and medication use.13 There is somewhat stronger evidence for the use of cognitive behavior therapy for chronic daily headache, both in group and individualized settings.14,15 Cognitive behavior therapy has been shown to reduce headache frequency and severity, and improve overall quality of life.14,15
Emerging evidence suggests that peripheral nerve stimulation in the occipital region can reduce pain, disability, and number of headache days in patients with chronic migraine for at least one year.16
PHARMACOLOGIC THERAPIES
Abortive drug therapies for acute headaches include acetaminophen, nonsteroidal anti-inflammatory drugs, tramadol (Ultram), and triptans. In the setting of chronic daily headache, concerns about headache from medication overuse should prompt the physician to consider headache prophylaxis to lessen the need for abortive therapy. An initial trial of discontinuing acute medications used for headaches may be warranted to help determine whether medication overuse has a role.9
Several prophylactic drug therapies have been studied for the treatment of chronic daily headache (Table 417–23 ). Amitriptyline, a tricyclic antidepressant, reduces headache duration and severity for chronic tension-type headache compared with placebo, and is thought also to be effective for other forms of chronic daily headache.17 Selective serotonin reuptake inhibitors, such as fluoxetine (Prozac), do not have proven benefit over placebo or tricyclic antidepressants for chronic daily headache.18
Table 4. Pharmacologic Therapies for Prophylaxis of Chronic Daily Headache

| Drug | Type | Study | Benefit |
|---|---|---|---|
| Amitriptyline | Tricyclic antidepressant | RCT; 391 patients17 | Reduces frequency of headaches by more than 50% in 46% of patients at 16 weeks, although not statistically different from placebo at 12 or 20 weeks |
| Fluoxetine (Prozac) | Selective serotonin reuptake inhibitor | Cochrane meta-analysis; 13 studies with 636 patients18 | No superiority to placebo for headache frequency or severity |
| Gabapentin (Neurontin) | Gamma-aminobutyric acid analogue | RCT; 133 patients19 | 9% absolute difference in headache-free days vs. placebo; average of 4-hour reduction in duration of headache per day |
| OnabotulinumtoxinA (Botox) | Injectable neurotoxin | Meta-analysis; 27 placebo-controlled trials with 5,313 patients20 | Reduces number of headaches per month by 2.3 in those with chronic migraine |
| Propranolol | Beta blocker | Cochrane meta-analysis; 58 studies with 5,072 patients21 | Reduces migraine frequency vs. placebo with standard mean difference of −0.4; study did not address population with chronic daily headache |
| Tizanidine (Zanaflex) | Alpha2-adrenergic agonist | RCT; 200 patients22 | 55% reduction in days with severe headache (21% with placebo); 35% reduction in severity (20% with placebo); 35% reduction in duration (19% with placebo) |
| Valproate (Depacon) and topiramate (Topamax) | Anticonvulsants | Cochrane meta-analysis; 23 studies with 902 patients23 | Odds ratio of 4.67 for valproate and 3.34 for topiramate to reduce frequency of headaches by more than 50% |
RCT = randomized controlled trial.
Other pharmacologic options include tizanidine (Zanaflex), certain anticonvulsants, propranolol, and onabotulinumtoxinA (Botox). There is evidence that tizanidine, an alpha2-adrenergic agonist, is effective for chronic migraine and chronic tension-type headache, reducing severity, frequency, and duration.22 One study showed that gabapentin (Neurontin), a gamma-aminobutyric acid analogue, increased the number of headache-free days compared with placebo in patients who had chronic daily headache, although the daily dosage was 2,400 mg.19 Valproate (Depacon) and topiramate (Topamax) are anticonvulsants that can reduce the frequency of chronic migraine by 50%.23 Propranolol, a beta blocker, also reduces the frequency of headache for persons with migraine, but its effectiveness for chronic migraine is unclear.21 OnabotulinumtoxinA is an injectable neurotoxin that has been shown to reduce headache frequency in those with chronic migraines, although evidence is lacking for chronic tension-type headache.20 Table 4 provides more details on the evidence for pharmacologic therapies in the treatment of chronic daily headache.17–23
Other Considerations
The most common complications of chronic daily headache, other than those related to untreated pain, are medication-induced adverse effects. It is important to work with patients to change the type, dosing, or timing of pharmacotherapy to maximize compliance and help prevent overuse of abortive therapies.
Education about headache from medication overuse is essential.3,9 Evidence suggests that educational interventions, whether face-to-face or in written form, can prevent medication overuse in patients with migraine.24 Although many experts recommend a complete withdrawal of acute medications in patients with headache from medication overuse, one randomized controlled trial suggests that patients can benefit from prophylactic treatment without complete withdrawal of abortive therapy.25
The indications for referral to a neurologist or headache specialist may include diagnostic uncertainty, unsuccessful outpatient therapy, or the desire to administer more specialized treatment, such as onabotulinumtoxinA. Patients with severe psychiatric illness should be evaluated by a psychiatrist. It may be necessary to hospitalize some patients (e.g., those with intractable migraine, those who are opioid dependent) to discontinue abortive medications in a monitored setting, and to treat the headache with intravenous medications, such as dihydroergotamine.3
Case Conclusion
After a thorough discussion of her options, your patient elects to try cognitive behavior therapy and topiramate for her chronic daily headache. She also agrees to reduce the amount of sumatriptan she is using, although she is reluctant to give up abortive therapy altogether. During a follow-up appointment two months later, she reports that her headaches have improved and now occur only about two to three times per week. Her current headaches are less intense than her previous chronic daily headaches. She feels her performance at work has improved because of better concentration and fewer missed days of work.
Data Sources: We searched the PubMed MeSH database and Cochrane database, including the terms headache syndromes, chronic migraine, and chronic tension-type headache. We also searched Essential Evidence Plus, American Family Physician content, and the New England Journal of Medicine's Clinical Practice review. Search dates: September and October 2011, and January 2014.

