Homelessness affects men, women, and children of all races and ethnicities. On any given night, more than 610,000 persons in the United States are homeless; a little more than one-third of these are families. Homeless persons are more likely to become ill, have greater hospitalization rates, and are more likely to die at a younger age than the general population. The average life span for a homeless person is between 42 and 52 years. Homeless children are much sicker and have more academic and behavioral problems. Insufficient personal income and the lack of affordable housing are the major reasons for homelessness. Complex, advanced medical problems and psychiatric illnesses, exacerbated by drug and alcohol abuse, in combination with the economic and social issues (such as the lack of housing and proper transportation) make this subset of the population a unique challenge for the health care system, local communities, and the government. An integrated, multidisciplinary health care team with an outreach focus, along with involvement of local and state agencies, seems best suited to address the components needed to ensure quality of care, to help make these patients self-sufficient, and to help them succeed. Family physicians are well suited to manage the needs of the homeless patient, provide continuity of care, and lead these multidisciplinary teams.
Homeless persons are individuals without permanent housing who may live on the streets; may stay in a shelter, mission, single room occupancy facility, abandoned building, or vehicle; or who are in any other unstable or nonpermanent situation. Persons may be considered homeless if circumstances force them to stay with a series of friends or extended family members, or if they have been released from prison or the hospital and do not have a stable housing situation to which they can return.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| For homeless patients, meeting standard blood pressure, cholesterol, and diabetes mellitus goals may require earlier initiation of drug therapy. Lifestyle modification usually does not work. | C | 26, 28–31 |
| All homeless patients should receive the influenza vaccine annually and be immunized against pneumococcus according to standard clinical guidelines. For homeless adults, hepatitis A and B vaccines should be provided and tetanus (tetanus and diphtheria toxoids; or tetanus, diphtheria, and acellular pertussis) vaccines updated if the patient's last immunization was more than 10 years ago. | C | 28 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease- oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Demographics
Homelessness affects men, women, and children of all races and ethnicities. In the United States, approximately 3 million persons, 1% of the population, are homeless in a given year. On any given night in 2013, more than 610,000 persons were homeless; approximately 36% were families and 35% were unsheltered.2 Most homeless persons' experiences are temporary, lasting a few days to several weeks.
Over the past 30 years, the increase in poverty and the growing shortage of affordable housing are the trends largely responsible for the increase in homelessness.3 In 2009, 14.3% of individuals and 10.5% of families had incomes below the poverty level, putting approximately 46.2 million Americans at risk of homelessness if they experience a single catastrophic financial or medical event.4 Economic and social factors linked to homelessness include unstable employment, low wages, declining public assistance, deinstitutionalization of persons with mental illness, being a veteran, lack of inexpensive housing, low education level, and lack of affordable health care. Any of these factors, compounded by alcohol and drug abuse, domestic violence, mental and physical illness, or abuse and neglect, can cause a person to become homeless.5,6
Risk Factors
In a homeless person, the association of one or more chronic illnesses with substance abuse or mental illness appears to increase the risk of early death. Compared with the general U.S. population, homeless persons are three to six times more likely to become ill, their hospitalization rates are four times higher, and they are three to four times more likely to die at a younger age.7–9 Disability is often the result of these medical and psychiatric conditions, is a barrier to employment, and perpetuates the cycle of homelessness. According to the Housing and Urban Development survey, approximately 37% of the estimated 1.6 million homeless persons living in shelters have a disability compared with 25% of those in poverty and 15.3% of the general population.10–13
Homelessness also has negative impacts on children. Infants born into homelessness have low birth weights and are nine times more likely to die within the first 12 months of life.14–16 Homeless children are sick four times more often than children who are not homeless and have an increased incidence of asthma, iron deficiency, lead poisoning, respiratory infections, ear infections, gastrointestinal problems, and emotional and behavioral problems (e.g., anxiety, depression, withdrawal, aggression, hostility). These children are also four times more likely to demonstrate delayed development, are six times more likely to have stunted growth, and have twice the expected rate of learning disabilities.17,18 In addition, they are more likely to experience hunger, abuse, neglect, and separation from family, and to have poor nutrition compared with the general population.19,20
Initial Approach
Identifying the homeless patient and those persons and families at risk is a priority.21–25 An outreach visit will most likely be the first contact with the homeless patient. During the initial clinic visit, the physician and clinic staff should focus on demonstrating genuine interest, empathy, and respect in a warm, nonthreatening, nonjudgmental environment. The goal is to address symptomatic problems first, which can be treated with simple guidance and will have a visible impact on the patient's life. This will help to establish confidence and mutual trust and encourage the patient to return to the physician's office. Once trust and rapport are established, visits can focus on identifying an emergency contact and discussing the patient's more challenging social, medical, and mental health problems, and end-of-life issues.
After completing the initial assessment, physicians should take into account the logistical complexities of developing an appropriate treatment plan for these patients. Making referrals, scheduling follow-up appointments, and monitoring laboratory tests and response to therapy are challenging because of the lack of dependable communication and transportation. A patient advocate or case manager can help in this area. Goal setting, short-term markers of success, and regular progress reports from clinical staff may assist with the biggest challenge of disease management.
Clinical and Medical Conditions
Homeless persons tend to have the same medical conditions as the general population. They differ from the general population, however, in that they experience long-term exposure to disease agents, overcrowding, unsanitary conditions, poor nutrition, sleep deprivation, violence, physical and emotional trauma, sexual abuse, and weather extremes. Limited education, mental illness, substance abuse, and distrust can affect their ability to respond appropriately to these adverse conditions and manage their medical problems. Based on these factors, homeless persons tend to present with advanced disease, and the approach to therapy is different depending on each person's situation.26–28
CARDIOVASCULAR DISEASE
Uncontrolled hypertension, coronary artery disease, congestive heart failure, and peripheral vascular disease are common in homeless persons. Poor diet contributes to nutrition-related disorders and the high prevalence of uncontrolled diabetes mellitus, hypercholesterolemia, and hypertension. Anger, excessive psychological stress, mental illness, poor coping mechanisms, and alcohol and drug abuse exacerbate the effect of the traditional risk factors and result in significant cardiovascular morbidity and mortality at a much earlier age. The average life span for a homeless person is between 42 and 52 years.7,29–31 To meet standard blood pressure, cholesterol, and diabetes goals, drug therapy should be initiated early, and the physician should work closely with a care manager and liaison to ensure a healthy diet, to reduce stress, and to improve the patient's compliance with the treatment plan. Lifestyle modification usually does not work.26,28–31
DUAL DIAGNOSIS: MENTAL ILLNESS AND SUBSTANCE ABUSE
Approximately 20% to 30% of homeless persons have a mental illness, whereas 30% to 50% have either substance abuse or dual disorders.32 Major depression, bipolar disorder, and schizophrenia are common. Risk factors for suicide include age younger than 30 years, Hispanic ethnicity, lower education level, and more days of homelessness. The two- or nine-item Patient Health Questionnaire is recommended by the Health Care for the Homeless Clinicians' Network for depression screening and the Simple Screening Instrument for Alcohol and Other Drug Abuse is recommended to screen for substance abuse.28 The foundation for treatment is to focus on finding stable housing in combination with access to therapy, supportive services, and, ultimately, employment.33
COGNITIVE DISORDERS AND TRAUMATIC BRAIN INJURY
Traumatic brain injury among homeless persons is estimated to be more than five times the rate in the general population.34 There is no cure for the original brain injury; however, a multidisciplinary approach involving family physicians, neuropsychiatric experts, and appropriate community and government resources provides the necessary evaluation, treatment, rehabilitation, and support. The Mini-Mental State Examination, Traumatic Brain Injury Questionnaire, and Repeatable Battery for the Assessment of Neuropsychological Status are useful in evaluating these patients.35 Cognitive rehabilitation is designed to maximize cognitive functioning and reduce functional impairment.36 In addition to performing the initial evaluation and confirming the diagnosis, family physicians can identify and treat specific conditions that commonly occur in these patients (i.e., anxiety, shortened attention span, dementia, depression, headaches, insomnia, and seizures).
INJURIES AND VIOLENCE
Domestic violence, rape, and physical assaults occur regularly in the homeless population and result in anxiety, posttraumatic stress disorder, and major depression.17 Fear of death is common and based on real threats. For women, sexually transmitted infections, unintended pregnancies, and posttraumatic stress are prevalent37 (Table 114–20,28,32,33,35,37–42 ). In children, stressful, traumatic and violent events lead to inhibition of physical, emotional, cognitive, social, and behavioral development. Homeless older persons are especially susceptible to violence and injury because of frailty, and physical and cognitive impairments.43,44 If abuse is suspected, the physician should evaluate and treat any injuries, develop a safety plan with the patient, and follow mandatory state reporting requirements. For suspected interpersonal violence, the Posttraumatic Diagnostic Scale Modified for Use with Extremely Low Income Women should be used.28 Trauma-informed care and trauma-specific interventions are designed to address the consequences of trauma and to promote healing.38
Table 1. Special Considerations in Health Care for Homeless Persons
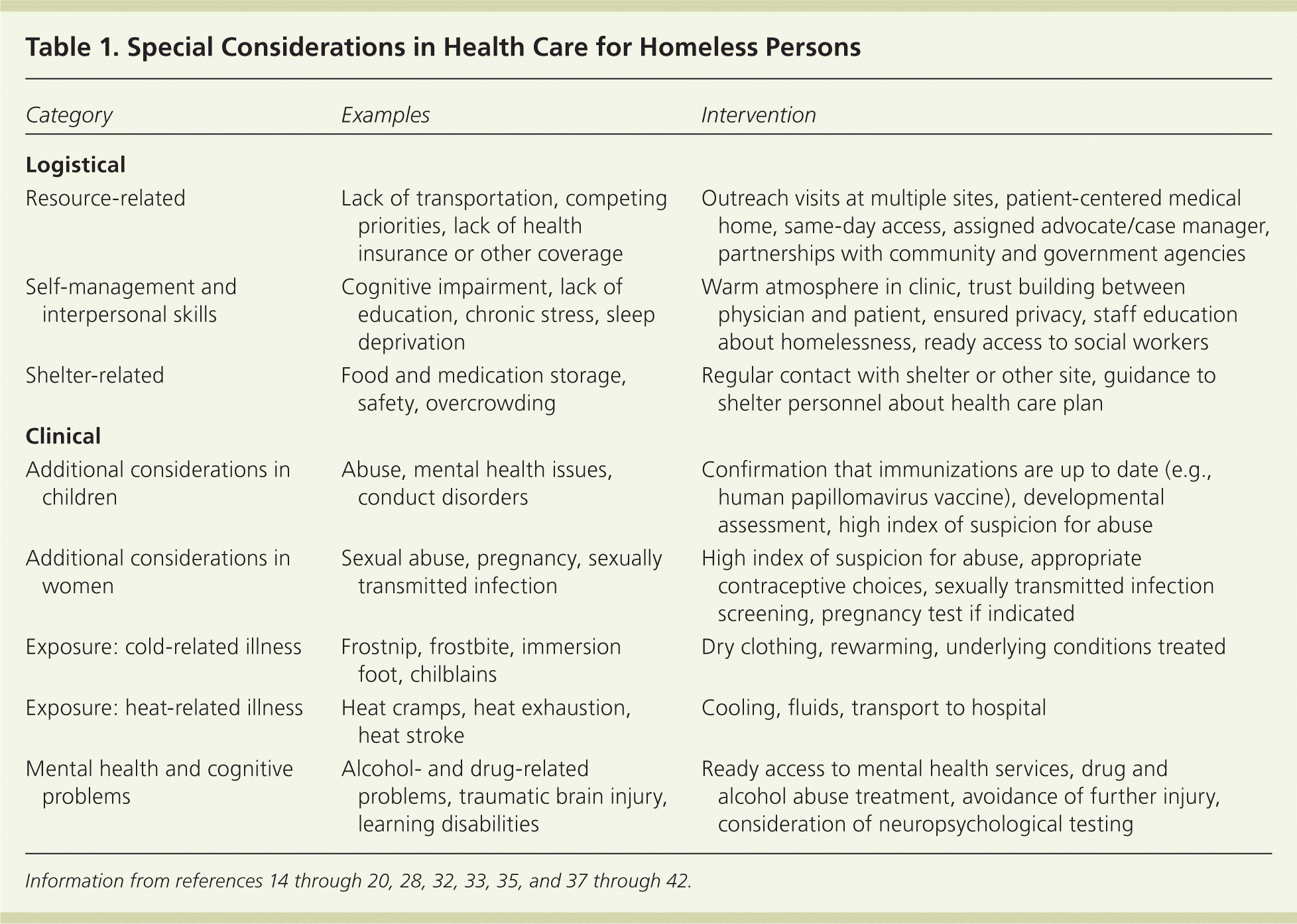
| Category | Examples | Intervention |
|---|---|---|
| Logistical | ||
| Resource-related | Lack of transportation, competing priorities, lack of health insurance or other coverage | Outreach visits at multiple sites, patient-centered medical home, same-day access, assigned advocate/case manager, partnerships with community and government agencies |
| Self-management and interpersonal skills | Cognitive impairment, lack of education, chronic stress, sleep deprivation | Warm atmosphere in clinic, trust building between physician and patient, ensured privacy, staff education about homelessness, ready access to social workers |
| Shelter-related | Food and medication storage, safety, overcrowding | Regular contact with shelter or other site, guidance to shelter personnel about health care plan |
| Clinical | ||
| Additional considerations in children | Abuse, mental health issues, conduct disorders | Confirmation that immunizations are up to date (e.g., human papillomavirus vaccine), developmental assessment, high index of suspicion for abuse |
| Additional considerations in women | Sexual abuse, pregnancy, sexually transmitted infection | High index of suspicion for abuse, appropriate contraceptive choices, sexually transmitted infection screening, pregnancy test if indicated |
| Exposure: cold-related illness | Frostnip, frostbite, immersion foot, chilblains | Dry clothing, rewarming, underlying conditions treated |
| Exposure: heat-related illness | Heat cramps, heat exhaustion, heat stroke | Cooling, fluids, transport to hospital |
| Mental health and cognitive problems | Alcohol- and drug-related problems, traumatic brain injury, learning disabilities | Ready access to mental health services, drug and alcohol abuse treatment, avoidance of further injury, consideration of neuropsychological testing |
Information from references 14 through 20, 28, 32, 33, 35, and 37 through 42.
PREVENTIVE HEALTH ISSUES, INFECTIOUS DISEASES, SEXUALLY TRANSMITTED INFECTIONS
Preventive health measures, periodic health examinations, and immunizations are often lacking in the homeless population. The guidelines for the general population also apply to these patients. Tetanus immunization (tetanus and diphtheria toxoids; or tetanus, diphtheria, and acellular pertussis) should be updated if the patient's last immunization was more than 10 years ago. Influenza vaccination should be provided annually, and all patients at risk of pneumonia should receive the pneumococcal vaccine. Physicians should test for bloodborne infections such as human immunodeficiency virus and hepatitis B and C.28 Alcoholism, human immunodeficiency virus coinfection, and length of shelter residence increase the risk of tuberculosis outbreaks. Directly observed therapy has markedly improved tuberculosis treatment effectiveness. While administering isoniazid and rifampin, it is important to monitor liver function because many of these patients have liver damage secondary to alcoholism, liver disease, and substance abuse39,45 (Table 224–31 ).
Table 2. Special Considerations for Medication Use in Homeless Persons
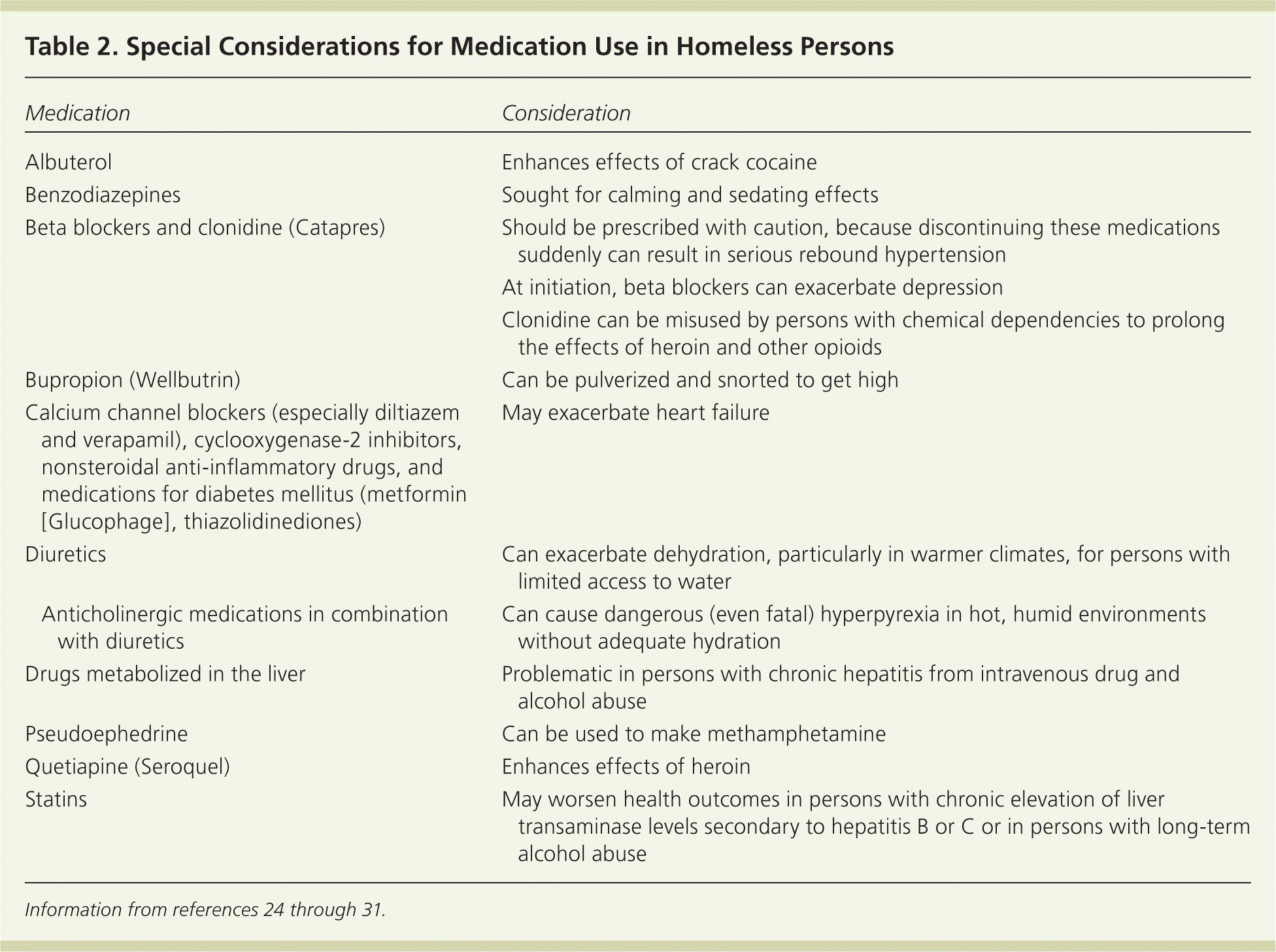
| Medication | Consideration | |
|---|---|---|
| Albuterol | Enhances effects of crack cocaine | |
| Benzodiazepines | Sought for calming and sedating effects | |
| Beta blockers and clonidine (Catapres) | Should be prescribed with caution, because discontinuing these medications suddenly can result in serious rebound hypertension | |
| At initiation, beta blockers can exacerbate depression | ||
| Clonidine can be misused by persons with chemical dependencies to prolong the effects of heroin and other opioids | ||
| Bupropion (Wellbutrin) | Can be pulverized and snorted to get high | |
| Calcium channel blockers (especially diltiazem and verapamil), cyclooxygenase-2 inhibitors, nonsteroidal anti-inflammatory drugs, and medications for diabetes mellitus (metformin [Glucophage], thiazolidinediones) | May exacerbate heart failure | |
| Diuretics | Can exacerbate dehydration, particularly in warmer climates, for persons with limited access to water | |
| Anticholinergic medications in combination with diuretics | Can cause dangerous (even fatal) hyperpyrexia in hot, humid environments without adequate hydration | |
| Drugs metabolized in the liver | Problematic in persons with chronic hepatitis from intravenous drug and alcohol abuse | |
| Pseudoephedrine | Can be used to make methamphetamine | |
| Quetiapine (Seroquel) | Enhances effects of heroin | |
| Statins | May worsen health outcomes in persons with chronic elevation of liver transaminase levels secondary to hepatitis B or C or in persons with long-term alcohol abuse | |
SKIN AND FOOT PROBLEMS
Lice, scabies, and secondary bacterial infections are endemic in homeless persons because of poor living conditions. Lice infestation has been associated with Bartonella quintana, the etiologic agent of trench fever (an influenza-like syndrome with relapsing fever), and blood culture–negative endocarditis in homeless persons.46 Poor foot hygiene, unsanitary living conditions, long periods of standing and walking, repetitive trauma from ill-fitting shoes, and macerated skin from wet socks and shoes predispose patients to abrasions, abscesses, corns, calluses, onychomycosis, tinea pedis, and immersion foot (an injury that develops after prolonged exposure to wet and cold conditions at temperatures above freezing). Prolonged standing leads to edema and venous stasis, which may lead to ulcerations and cellulitis requiring subsequent hospitalization for intravenous antibiotics. Copious irrigation, debridement, intramuscular antibiotics, and medicated compression wrapping (Unna boot) that can be left in place for up to a week are beneficial. Education regarding proper foot care, early detection of problems, proper fitting shoes, dry socks, sanitary living conditions, and appropriate follow-up are important preventive measures.
EXPOSURE-RELATED CONDITIONS
Cold- and heat-related injuries are common in homeless persons. In those who experience frostbite, immersion foot, or hypothermia, the risk of death from other causes is increased eightfold.40 Absolute temperature and duration of exposure to cold are the two factors that determine severity of injury and resultant tissue damage. Predisposing factors include use of alcohol, nicotine, and drugs; poor nutrition; dehydration; adrenal insufficiency; diabetes; hypothyroidism; peripheral vascular disease; and peripheral neuropathy.41 Frostnip is a mild, reversible form of cold-induced injury, which is associated with paresthesias that resolve after rewarming. Frostbite is a more severe injury that causes localized tissue loss. Salvaging damaged tissue, restoring function, and preventing complications are the major goals of therapy.47 Immersion foot (or trench foot) can be prevented by wearing dry socks.47 Heat cramps, heat exhaustion, and heat stroke occur during periods of extreme heat. Persons experiencing these conditions must be moved to a cool place and provided fluids. Hospital admission is required for severe cases. Death can occur with heat stroke.47
Model for Provision of Care
The best model of care involves an integrated, multidisciplinary approach by a team of health care personnel knowledgeable about the unique challenges faced by homeless persons, utilizing a patient-centered medical home model in association with outreach services at multiple sites with ready access to secondary/tertiary care, convalescent and respite care, community resources and local agencies for housing, employment, and legal assistance. The ability to care for medical and psychosocial needs in one place and the U.S. policy of “Housing First” are key components.6,28,42,48 This adaptation to standard clinical practice allows health care professionals to play an integral role in connecting with, treating, and educating patients and in promoting improved health care outcomes within this population. It also provides a practical basis for implementing the American Academy of Family Physicians' policies encouraging physician involvement for the medically underserved and homeless persons.49,50 Improving the health and well-being of homeless persons is a step toward employment, and hopefully, restoring these patients to living in their own homes. Family physicians are ideally suited to provide compassionate, comprehensive, and continuous care for these patients and to lead these multidisciplinary teams.
Table 3 provides resources on homelessness.
Table 3. Resources on Homelessness
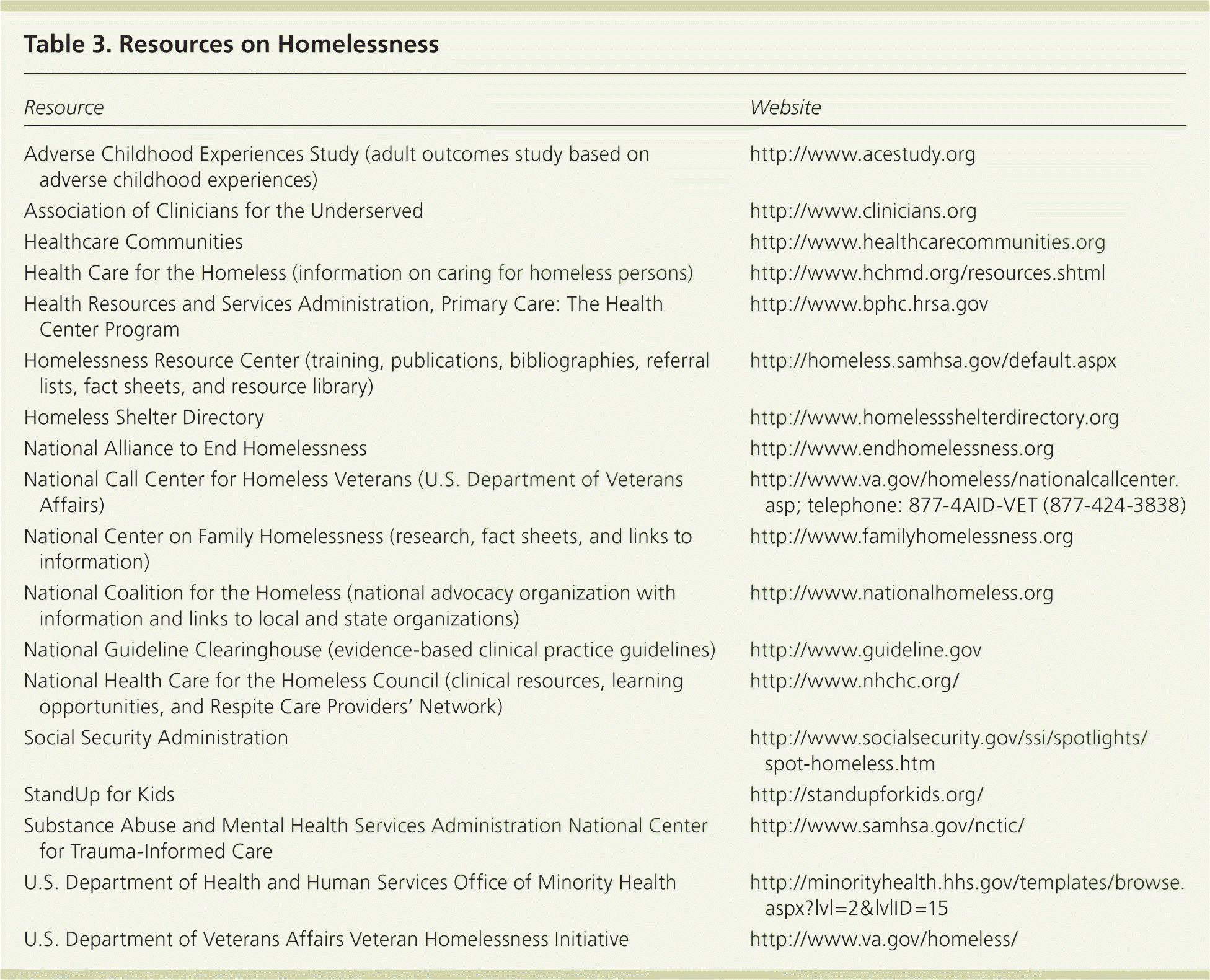
| Resource | Website |
|---|---|
| Adverse Childhood Experiences Study (adult outcomes study based on adverse childhood experiences) | http://www.acestudy.org |
| Association of Clinicians for the Underserved | http://www.clinicians.org |
| Healthcare Communities | http://www.healthcarecommunities.org |
| Health Care for the Homeless (information on caring for homeless persons) | http://www.hchmd.org/resources.shtml |
| Health Resources and Services Administration, Primary Care: The Health Center Program | http://www.bphc.hrsa.gov |
| Homelessness Resource Center (training, publications, bibliographies, referral lists, fact sheets, and resource library) | http://homeless.samhsa.gov/default.aspx |
| Homeless Shelter Directory | http://www.homelessshelterdirectory.org |
| National Alliance to End Homelessness | http://www.endhomelessness.org |
| National Call Center for Homeless Veterans (U.S. Department of Veterans Affairs) | http://www.va.gov/homeless/nationalcallcenter.asp; telephone: 877-4AID-VET (877-424-3838) |
| National Center on Family Homelessness (research, fact sheets, and links to information) | http://www.familyhomelessness.org |
| National Coalition for the Homeless (national advocacy organization with information and links to local and state organizations) | http://www.nationalhomeless.org |
| National Guideline Clearinghouse (evidence-based clinical practice guidelines) | http://www.guideline.gov |
| National Health Care for the Homeless Council (clinical resources, learning opportunities, and Respite Care Providers' Network) | http://www.nhchc.org/ |
| Social Security Administration | http://www.socialsecurity.gov/ssi/spotlights/spot-homeless.htm |
| StandUp for Kids | http://standupforkids.org/ |
| Substance Abuse and Mental Health Services Administration National Center for Trauma-Informed Care | http://www.samhsa.gov/nctic/ |
| U.S. Department of Health and Human Services Office of Minority Health | http://minorityhealth.hhs.gov/templates/browse.aspx?lvl=2&lvlID=15 |
| U.S. Department of Veterans Affairs Veteran Homelessness Initiative | http://www.va.gov/homeless/ |
Data Sources: An online search was conducted using the key terms homeless, homeless health, homeless women, homeless children, homeless elderly, and homeless health care. Initially, a broad-based overview of the topic was done on national websites such as National Coalition for the Homeless, National Alliance to End Homelessness, and National Health Care for the Homeless Council. After the background reading, the search was refined to identify major scholarly and professional resources on the topic using the following: UpToDate, National Guideline Clearinghouse, PubMed, the Cochrane database, the U.S. Preventive Services Task Force recommendation database, and Agency for Healthcare Research and Quality evidence reports. Search dates: June 2012 to January 27, 2014.

