Homelessness affects more than 580,000 Americans on any given night. Risk factors for homelessness include extreme poverty, substance use, and mental illness. People experiencing homelessness are likely to have multiple chronic medical or mental health conditions. Homelessness increases morbidity associated with cardiovascular, respiratory, and infectious diseases and all-cause mortality. A trauma-informed approach to the examination of people experiencing homelessness is imperative because previous exposure to physical or sexual trauma is common in this population, especially among women. Considerations for medical management include simplifying medication regimens, providing safe options for medication storage, and addressing environmental exposures. A multidisciplinary approach that includes pharmacists, case managers, and social workers improves chronic disease outcomes. Housing First initiatives decrease emergency department use and hospitalizations, and colocating primary care visits with shelters increases overall health care access.
Federal law defines people experiencing homelessness as those who lack a fixed, regular, and adequate nighttime residence designed for sleeping. This includes individuals and families facing the imminent loss of their housing with no subsequent housing identified and victims of domestic violence or sexual assault who are living in a dangerous or life-threatening situation.1 Chronic homelessness is defined as continuous homelessness for at least one year or at least four episodes of homelessness in the previous three years.2
SORT: KEY RECOMMENDATIONS FOR PRACTICE
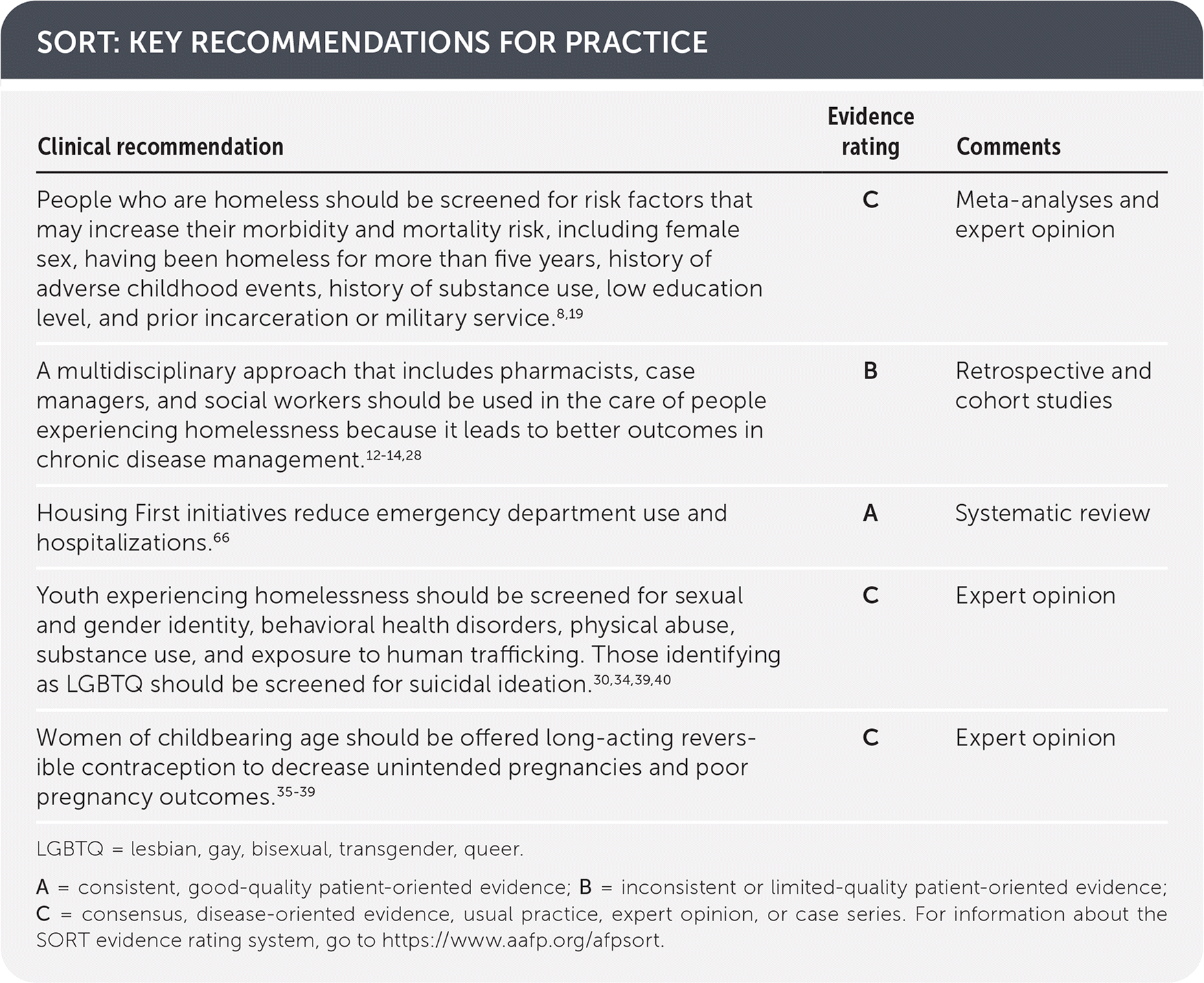
LGBTQ = lesbian, gay, bisexual, transgender, queer.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Demographics
Measuring the prevalence of homelessness and the demographic characteristics of the homeless population is difficult because they are ever changing. Most surveys rely on personal reports and may have a limited reach. Table 1 reviews approximate demographics of the homeless population.1–4 Table 2 lists risk factors for becoming homeless and for increased morbidity and mortality in the homeless population.5–7
TABLE 1. Demographics of People Experiencing Homelessness
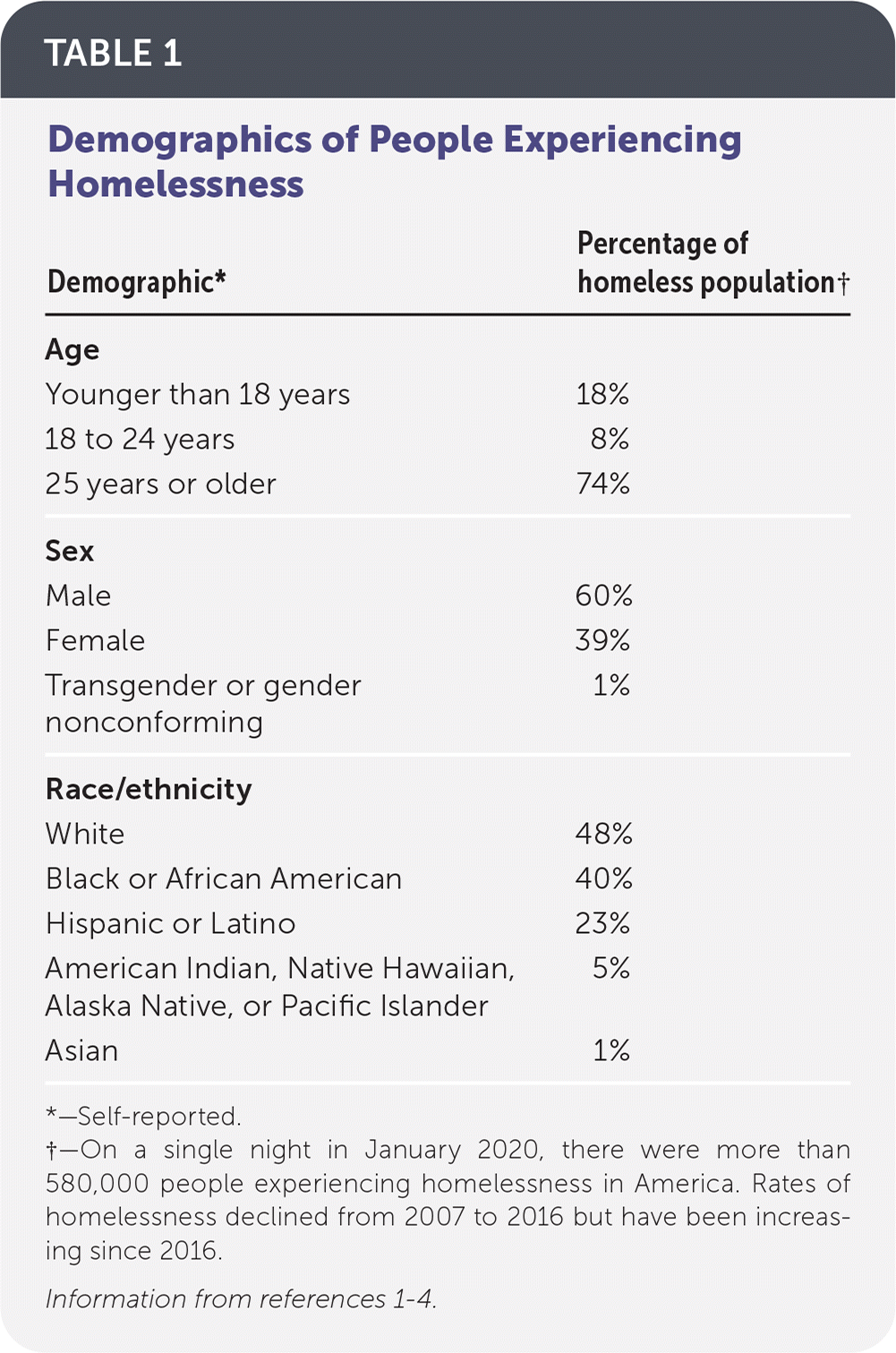
| Demographic* | Percentage of homeless population† |
|---|---|
| Age | |
| Younger than 18 years | 18% |
| 18 to 24 years | 8% |
| 25 years or older | 74% |
| Sex | |
| Male | 60% |
| Female | 39% |
| Transgender or gender | 1% |
| nonconforming | |
| Race/ethnicity | |
| White | 48% |
| Black or African American | 40% |
| Hispanic or Latino | 23% |
| American Indian, Native Hawaiian, Alaska Native, or Pacific Islander | 5% |
| Asian | 1% |
*—Self-reported.
†—On a single night in January 2020, there were more than 580,000 people experiencing homelessness in America. Rates of homelessness declined from 2007 to 2016 but have been increasing since 2016.
TABLE 2. Risk Factors for Homelessness and for Increased Morbidity and Mortality in the Homeless Population

| Risk factors for becoming homeless5 |
| Adverse childhood events |
| Criminal behavior/history of incarceration |
| Extreme poverty |
| History of being in foster care |
| History of military service |
| Low education level |
| Mental health disorders |
| Substance use |
| Unemployment |
| Risk factors for increased morbidity and mortality in people experiencing homelessness6,7 |
| Female sex |
| History of adverse childhood events |
| History of incarceration |
| History of military service |
| History of substance use |
| Homelessness lasting for more than five years |
| Low education level |
The increased risk of homelessness for those experiencing extreme poverty is exacerbated by a lack of affordable housing. On average, low-income American households use at least one-half of their income for housing, further limiting their resources and putting them at risk of homelessness. The supply of low-cost housing has continued to decline since 1980.8 In 2017, the hourly wage needed to afford the average two-bedroom rental home in the United States was nearly $14 higher than the federal minimum hourly wage of $7.25.8 Black and Hispanic communities are disproportionately affected by the scarcity of low-income housing because of the persisting effects of systemic housing discrimination.8
Screening for Homelessness
Housing instability is often grouped with other adverse social conditions associated with poor health, such as food insecurity and social isolation. These are collectively referred to as social risk factors.9 Social risk factors are associated with increased mortality, disease rates, and use of medical resources, and multiple risk factors often affect one individual or family.10
Screening for social risk factors in primary care is ideally paired with mechanisms for referral to social services or, at a minimum, incorporated into a care plan.11–13 Although multiple screening tools are available, outcomes data on their use are limited.14,15 Research on the use of screening tools for housing instability in the general population is also limited.16
In 2012, the Veterans Health Administration integrated a two-question screening tool for housing instability into electronic health records17,18:
- In the past two months, have you been living in stable housing that you own, rent, or stay in as part of a household? (Negative response indicates homelessness.)
- Are you worried or concerned that in the next two months you may not have stable housing that you own, rent, or stay in as part of a household? (Positive response indicates risk of homelessness.)
This screening, which is completed at all outpatient appointments, has resulted in earlier identification of homelessness and increased referrals for services.17 Once identified, people experiencing homelessness should be screened for risk factors that may increase their morbidity and mortality risk, including female sex, having been homeless for more than five years, history of adverse childhood events, history of substance use, low education level, and prior incarceration or military service.8,19
The Initial Clinic Visit
During the initial clinic visit with a person experiencing homelessness, physicians should dedicate time to identifying the patient’s main priorities. These patients may have multiple health conditions, likely with competing nonmedical priorities.6,20 Physicians and people experiencing homelessness tend to have different perceptions of the barriers to optimal disease management.21 Identifying these discrepancies can help build trust and establish shared priorities, a process that is crucial to the success of the visit and follow-up plans.3
Trauma-informed care is an essential component of establishing trust.21,22 People experiencing homelessness are more likely to have experienced or witnessed trauma, and it is important to prevent retraumatization.23 For example, women with a history of sexual trauma may have strong physical or psychological reactions to physical examinations.24
Trauma-informed care integrates an understanding of trauma and its pervasiveness into all policies, procedures, and practices while actively seeking to avoid retraumatization.21,22,25 A policy statement from the American Academy of Family Physicians recommends that trauma-informed care be universally adopted for all patient interactions.21 Patients should not be required to disclose prior trauma to receive trauma-informed care, and minimally invasive options for care should be available to address immediate concerns.22
Management Considerations
Medication management and storage are often a challenge for people experiencing homelessness because unstable housing limits security, privacy, and access to cool, dry, and refrigerated storage areas. Adverse medication effects, such as frequent urination or diarrhea when a toilet is not readily available, can significantly impact adherence.26 Although simplifying medication regimens is sometimes helpful, there is a delicate balance between maintaining optimal medical therapy and improving the patient’s ability to adhere to therapy.26,27 A multidisciplinary approach that includes pharmacists, case managers, and social workers should be used because it leads to better outcomes in chronic disease management.12–14,28
TABLE 3. Special Considerations in the Care of People Experiencing Homelessness
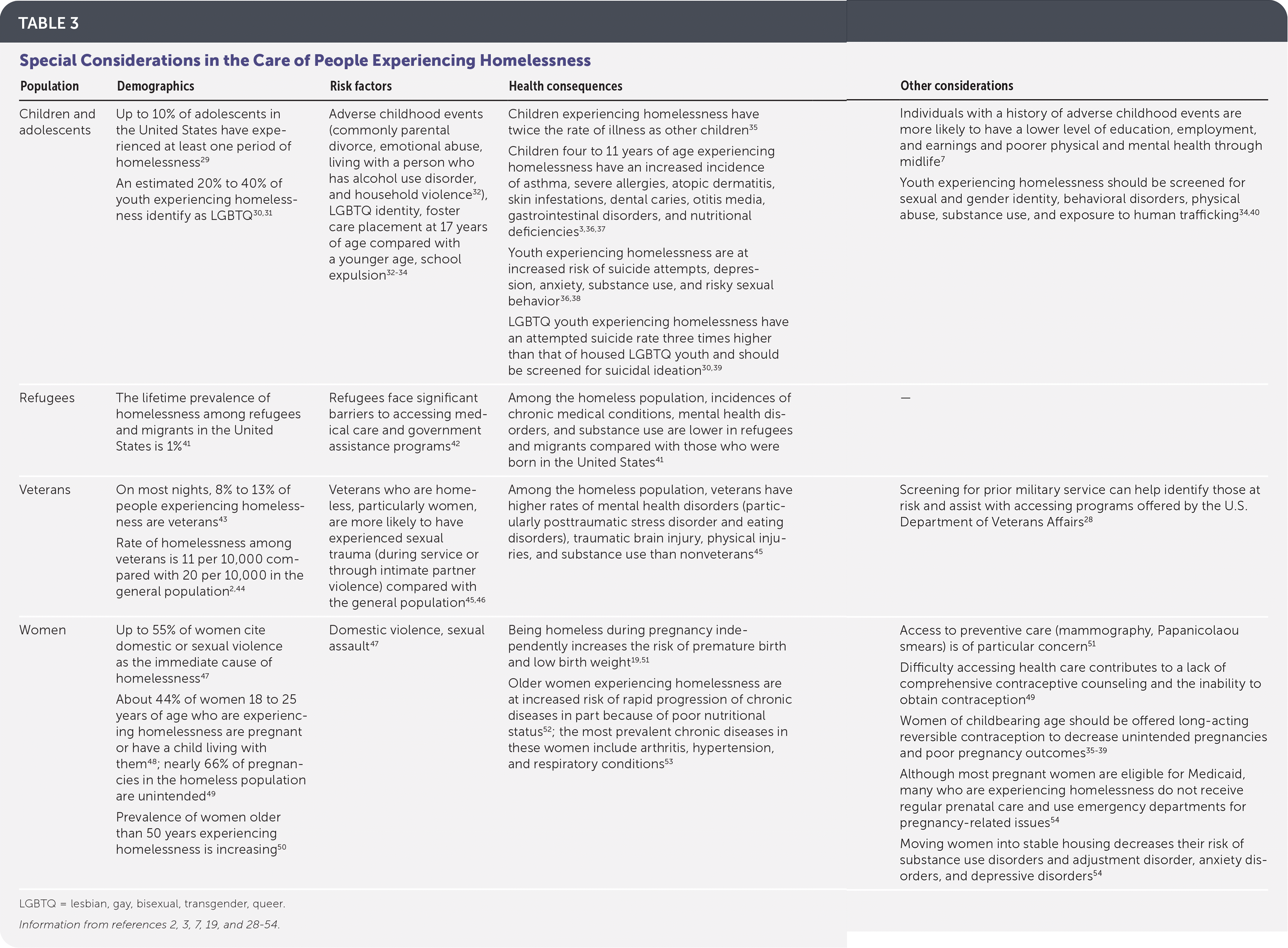
| Population | Demographics | Risk factors | Health consequences | Other considerations |
|---|---|---|---|---|
| Children and adolescents | Up to 10% of adolescents in the United States have experienced at least one period of homelessness29 An estimated 20% to 40% of youth experiencing homelessness identify as LGBTQ30,31 | Adverse childhood events (commonly parental divorce, emotional abuse, living with a person who has alcohol use disorder, and household violence32), LGBTQ identity, foster care placement at 17 years of age compared with a younger age, school expulsion32–34 | Children experiencing homelessness have twice the rate of illness as other children35 Children four to 11 years of age experiencing homelessness have an increased incidence of asthma, severe allergies, atopic dermatitis, skin infestations, dental caries, otitis media, gastrointestinal disorders, and nutritional deficiencies3,36,37 Youth experiencing homelessness are at increased risk of suicide attempts, depression, anxiety, substance use, and risky sexual behavior 36,38 LGBTQ youth experiencing homelessness have an attempted suicide rate three times higher than that of housed LGBTQ youth and should be screened for suicidal ideation30,39 | Individuals with a history of adverse childhood events are more likely to have a lower level of education, employment, and earnings and poorer physical and mental health through midlife 7 Youth experiencing homelessness should be screened for sexual and gender identity, behavioral disorders, physical abuse, substance use, and exposure to human trafficking34,40 |
| Refugees | The lifetime prevalence of homelessness among refugees and migrants in the United States is 1%41 | Refugees face significant barriers to accessing medical care and government assistance programs42 | Among the homeless population, incidences of chronic medical conditions, mental health disorders, and substance use are lower in refugees and migrants compared with those who were born in the United States41 | — |
| Veterans | On most nights, 8% to 13% of people experiencing homelessness are veterans43 Rate of homelessness among veterans is 11 per 10,000 compared with 20 per 10,000 in the general population2,44 | Veterans who are homeless, particularly women, are more likely to have experienced sexual trauma (during service or through intimate partner violence) compared with the general population45,46 | Among the homeless population, veterans have higher rates of mental health disorders (particularly posttraumatic stress disorder and eating disorders), traumatic brain injury, physical injuries, and substance use than nonveterans45 | Screening for prior military service can help identify those at risk and assist with accessing programs offered by the U.S. Department of Veterans Affairs28 |
| Women | Up to 55% of women cite domestic or sexual violence as the immediate cause of homelessness47 About 44% of women 18 to 25 years of age who are experiencing homelessness are pregnant or have a child living with them48; nearly 66% of pregnancies in the homeless population are unintended49 Prevalence of women older than 50 years experiencing homelessness is increasing50 | Domestic violence, sexual assault 47 | Being homeless during pregnancy independently increases the risk of premature birth and low birth weight 19,51 Older women experiencing homelessness are at increased risk of rapid progression of chronic diseases in part because of poor nutritional status52; the most prevalent chronic diseases in these women include arthritis, hypertension, and respiratory conditions53 | Access to preventive care (mammography, Papanicolaou smears) is of particular concern51 Difficulty accessing health care contributes to a lack of comprehensive contraceptive counseling and the inability to obtain contraception49 Women of childbearing age should be offered long-acting reversible contraception to decrease unintended pregnancies and poor pregnancy outcomes35–39 Although most pregnant women are eligible for Medicaid, many who are experiencing homelessness do not receive regular prenatal care and use emergency departments for pregnancy-related issues54 Moving women into stable housing decreases their risk of substance use disorders and adjustment disorder, anxiety disorders, and depressive disorders54 |
LGBTQ = lesbian, gay, bisexual, transgender, queer.
CARDIOVASCULAR DISEASE
Cardiovascular disease is a leading cause of death in people experiencing homelessness, likely because of poorly controlled comorbidities and higher rates of risk factors (substance use, smoking, chronic stress, mental illness treated with antipsychotic drugs).55 Making dietary changes and exercising regularly can be challenging for people experiencing homelessness. Continuity of care and involvement of a multidisciplinary team may improve follow-up and help optimize lifestyle factors.
The prevalence of tobacco use in people experiencing homelessness is nearly 70%, compared with 13% in the general population.56 Assisting patients with smoking cessation can have a large impact on cardiovascular risk.3,27 Medical respite units, such as those operated by the Health Care for the Homeless program, may be a valuable resource for patients recovering from interventional cardiac procedures.27
DIABETES MELLITUS
Homelessness presents many obstacles to the management of diabetes. Food insecurity may make it difficult to access healthy foods. It is often challenging for people experiencing homelessness to afford or appropriately store diabetes supplies and medications.20 It is also important for physicians to consider a patient’s ability to maintain a hygienic environment for performing finger sticks and injections. Medication regimens that entail fewer daily injections or do not require refrigeration can increase adherence to therapy. Providing refrigerated medication storage at the clinic can allow patients without reliable access to electricity to benefit from effective injectable medications. Physicians should provide clear instructions for the use of insulin therapies when food is not available.26
PULMONARY CONDITIONS
People experiencing homelessness are at increased risk of pulmonary disease exacerbations because of infections or allergens in tight living conditions, environmental exposures, and exposure to smoke from cigarettes and marijuana (personal or secondhand). Spirometry can be obtained if available but should not delay treatment. Physicians should ensure that immunizations are up to date.26
Although the incidence of tuberculosis (TB) has been declining in the general population, the estimated incidence in people experiencing homelessness continues to be nearly 50 times that of the general population. Use of interferon-gamma release assays; incentives for completing therapy; and a directly observed, 12-dose, weekly regimen of isoniazid and rifapentine (compared with daily rifampin) are useful strategies in the detection and treatment of TB.57 The patient’s liver function should be monitored while using isoniazid and rifapentine because of the higher prevalence of liver disease and cirrhosis among people experiencing homelessness.3 Partnering with shelters to provide TB tests can assist with identifying cases early and preventing spread.57
MENTAL HEALTH DISORDERS
The prevalence of mental health disorders is significantly higher in people experiencing homelessness than in the general population.58 Mental health disorders are closely linked to other chronic health conditions and can increase mortality rates by as much as 70% in people experiencing homelessness. Mental health conditions are associated with higher rates of criminal behavior and victimization.59
Screening tools such as the Patient Health Questionnaire and the Simple Screening Instrument for Alcohol and Other Drug Abuse can assist in identifying patients who would benefit from medical or nonmedical therapies.3 A multidisciplinary approach involving case managers improves psychiatric and substance use outcomes.27
INFECTIOUS DISEASE
Infectious diseases that often affect people experiencing homelessness include bloodborne, skin (bacterial and fungal), pulmonary, and gastrointestinal (including parasites) infections and infestations such as lice and scabies.3,57 Patients may be unaware that they have certain bloodborne infections early in the disease course, which can lead to transmission to others in the setting of intravenous drug use and needle sharing.57
Sexually transmitted infections are common in people experiencing homelessness and can be asymptomatic long enough for unintentional spread.59 For example, syphilis may go unnoticed because it presents as a painless lesion in the primary stages. A trauma-informed approach to examinations and testing for sexually transmitted infections is imperative.21
Offering vaccinations for infectious diseases such as hepatitis and human papillomavirus can help decrease transmission, complications, and severe illness.3,57 Poor hygiene and foot care due to weather exposures, unsanitary living conditions, prolonged walking, and poorly fitting shoes increase the risk of cellulitis and tinea infections. Education on proper hygiene should be emphasized, and provisions of clean socks, properly fitting shoes, and medicated foot powders are an important aspect of prevention.3
WEATHER-RELATED CONDITIONS
The nature of homelessness involves prolonged exposure to the elements, depending on the availability of shelter. People experiencing homelessness have a 13 times higher risk of death from hypothermia than the general population. Chronic conditions, such as kidney disease and heart failure, may be exacerbated by significant heat exposure. Working with local authorities and shelters to establish a notification system for extreme weather events can help prevent acute and severe cases of cold or heat exposure.60
INJURIES
Risk factors for acute injuries include decreased physical functioning and mobility, untreated seizure disorders, sleep deprivation, and exposure to violence.61,62 Traumatic brain injury is estimated to be five times more prevalent among people experiencing homelessness than in the general population.3 Screening for domestic violence and exposure to community violence can help identify those at risk of injury. Encouraging patients to use walk-in appointments for acute injuries can help decrease repeated radiation exposure from computed tomography and radiography in the emergency department that may not always be necessary.62
Long-term Outcomes and Initiatives
Homelessness independently increases morbidity associated with cardiovascular, respiratory, and infectious diseases and all-cause mortality compared with the lowest-income housed person.63–65 Over the past decade, emphasis has been placed on Housing First initiatives, which aim to expedite placement of people experiencing homelessness into permanent housing vs. Housing Ready programs, which first require individuals to be in mental health or substance use treatment programs.66 The American Academy of Family Physicians supports Housing First programs and encourages physicians to be involved in the health care of people experiencing homelessness.67 Individuals in Housing First programs have better quality of life and reduced hospitalizations and emergency department use.66 Further research is needed to establish whether there are additional health benefits compared with Housing Ready programs.
Colocating primary care, mental health, social support, pharmacy, and case management services is another effective strategy.68 Providing these services at shelters can shift care away from the emergency department and allow for more comprehensive care.51,54 Collaboration between pharmacists and physicians has been shown to improve outcomes in chronic disease management.69,70 Working with case managers can be useful for organizing the care of patients who see multiple specialists. Social workers can assist in providing resources for housing, rehabilitation, transportation, and therapy. Table 4 lists social support services for people experiencing homelessness.3 When a clinical model is used that offers a “one-stop-shop” primary care visit involving multidisciplinary teams, patient satisfaction and adherence to the care plan increase, and the burden of emergency department visits decreases.71
This article reviews previous articles on this topic by Maness and Khan3 and Montauk.26
Data Sources: A PubMed search in Clinical Queries used the key terms homeless, comprehensive health care, clinic visit, primary care, demographics, risk factors, and well visit. The search included meta-analyses, RCTs, clinical trials, and reviews. Also searched were the AHRQ Effective Healthcare Reports, the Cochrane database, U.S. Preventive Services Task Force guidelines, and Essential Evidence Plus. Search dates: June 1, 2022, and October 1, 2022.
Any opinions or assertions are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army at large.

