
Am Fam Physician. 2014;90(7):487-488
Author disclosure: No relevant financial affiliations.
A 27-year-old man on active military duty presented with severe sweating in both of his feet. He also had malodorous cracking skin and pain in his feet. The symptoms had been present for two years. Multiple home remedies such as frequent changing of his socks, new shoes, and the use of deodorants and drying powders did not improve his symptoms. He did not have excessive sweating in other areas of his body.
Physical examination revealed foul-smelling feet with multiple discrete punctate depressions on the plantar surface. The lesions were mostly distal in location (see accompanying figure). Physical examination findings were otherwise normal.
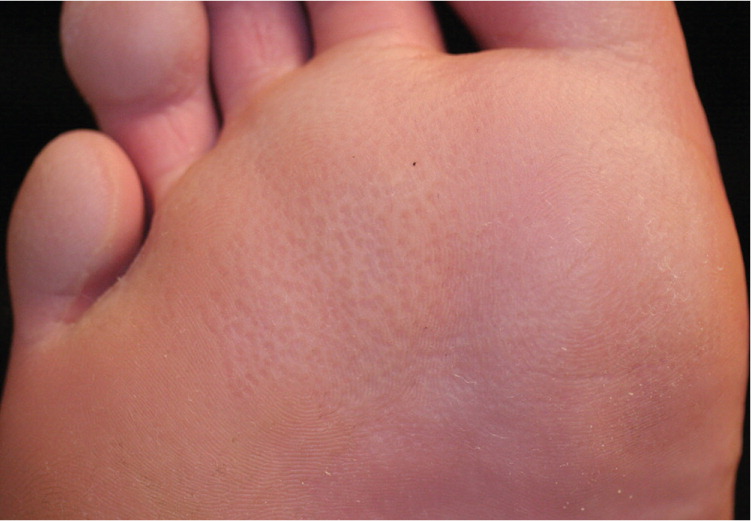
Question
Discussion
The answer is C: pitted keratolysis. Pitted keratolysis is caused by a bacterial infection (usually Corynebacterium), which is often misdiagnosed as a fungal infection.1 It typically presents as many circular or longitudinal “punched out” depressions in the skin of the weight-bearing surfaces of the soles, with associated severe malodor. The diagnosis is clinical, based on history findings and the presence of lesions. Pitted keratolysis is more common in persons younger than 35 years, and in those who wear occlusive footwear, are physically active, have a personal history of hyperhidrosis, or work or are active in a hot or humid environment. It is common in the active duty military population.1,2
Patients should begin with conservative treatment such as keeping the feet dry with frequent sock changes and drying powders. Twice-daily application of topical clindamycin, erythromycin, or mupirocin (Bactroban) is the most effective treatment. Oral clindamycin or erythromycin is also effective, but typically not needed with topical treatment. The lesions and odor usually resolve in three to four weeks.3
Dyshidrotic eczema is an idiopathic reaction that often presents as a hand dermatitis, but it can also affect the feet. It is common in patients with environmental allergies.4 Small, intensely pruritic blisters occur in the acute stage. The blisters last three to four weeks before spontaneously resolving. Chronic eczematous changes follow shortly afterward with erythema, peeling, cracking, scaling, and lichenification.1
Essential hyperhidrosis is excess sweating, usually on the palms, soles, and axillae. The sweating is beyond what is needed for thermoregulation and can cause significant embarrassment.5 Hyperhidrosis is most often idiopathic but can be secondary to hyperthyroidism, obesity, diabetes mellitus, and cardiovascular disorders. It can also be an adverse effect of some medications, most commonly tricyclic antidepressants.6
Plantar warts are caused by the human papillomavirus and typically occur at the point of maximal pressure on the plantar surface of the foot. Patients may alter their gait if a large callus forms, resulting in pain in other parts of the foot, leg, or back.1 Plantar warts can be distinguished from pitted keratolysis by the multiple small black petechiae within the lesion and the loss of dermatoglyphs.1
Tinea pedis is the most common dermatophyte infection. Shoes that promote warmth and sweating encourage fungal growth. The condition typically presents as toe web maceration, but may also present as a classic ringworm pattern or a moccasin-type distribution (i.e., primarily affecting the soles).1 Tinea pedis is more common in men and can be confirmed with potassium hydroxide scraping. It usually resolves with topical antifungal cream.7

| Condition | Characteristics |
|---|---|
| Dyshidrotic eczema | Vesicular dermatitis appearing most often on the hands, but can affect the feet; common in individuals with environmental allergies |
| Essential hyperhidrosis | Excess sweating usually on the palms, soles, and axillae; often idiopathic but may be secondary to a chronic medical condition (hyperthyroidism, obesity, diabetes mellitus) or medication use (tricyclic antidepressants) |
| Pitted keratolysis | Bacterial skin infection affecting the feet; most common in active, younger individuals in hot, humid environments; resolves in three to four weeks with topical antibiotic creams |
| Plantar warts | Caused by human papillomavirus; occur at the point of maximum pressure on the plantar surface of the foot; small black petechiae within the lesion and loss of dermatoglyphs |
| Tinea pedis | Toe web maceration is most common; may also present as the classic ringworm pattern or a moccasin-type distribution (i.e., primarily affecting the soles); confirmed with potassium hydroxide testing; typically resolves with antifungal cream |
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force Medical Department or the U.S. Air Force at large.
