Case Scenario
A 48-year-old Chinese immigrant presented to my office for a sick visit. At the time, I ordered hepatitis B screening because he had never received preventive care. The hepatitis B surface antigen came back positive, so I ordered follow-up tests to decide if treatment was needed. Luckily, his tests were reassuring, and he needs only monitoring for now. With similar patients in the past, I have had difficulty with poor follow-up after I tell them that they do not need immediate treatment. How should I approach the situation with this patient to encourage long-term monitoring and prevent future morbidity?
Commentary
In cases such as this, patients are often told, “You don't need treatment now,” but they only hear, “You are fine.” Subsequent failure to follow up may result from a combination of issues related to health literacy, educational attainment, linguistic barriers, and cultural differences.
Numbering 14.7 million in the 2010 census, Asian Americans are the fastest growing racial group in the United States.1 Most Asian Americans are immigrants; as of 2011, there were 11.6 million foreign-born persons from Asia in the United States.2 For nonimmigrant patients with chronic conditions, it is often enough to simply advise follow-up examinations and testing within a specified time frame. However, for patients from immigrant families, physicians should not assume the same health literacy as American-born patients.3 Also, despite the common perception that all Asians are well-educated, many Asian immigrants have low educational attainment and poor medical knowledge; for example, 30% of Vietnamese Americans 25 years or older have completed less than a high school education (compared with 11% in non-Hispanic whites).4 Consequently, greater effort must be taken to educate patients and families about the long-term implications of chronic conditions and the potential for patients to change outcomes through close clinical follow-up.
A high percentage of Asian Americans have limited English proficiency, with 77% speaking a language other than English at home.4 Even when patients and family members appear to have good command of conversational English, their linguistic skills may not be adequate for clinical discussions. When interpreters are used, physicians must remember to speak in short phrases, pausing for interpretation, and to avoid the use of jargon, idioms, and colloquialisms that are difficult to translate.
Culturally, Asian families may adhere to a collectivistic approach.5 Major health care decisions are often made as a family, and the adult children of immigrant patients can be helpful allies in ensuring mutual understanding and promoting adherence to care plans.
Physicians should ask explicitly about use of supplements and herbals, because patients often do not think to mention this during medication review.6 Asian ethnic newspapers may include more nutritional supplement advertisements than actual health articles,7 and patients may believe that the use of such products can supplant the need for medical care and follow-up testing.
Finally, the previous health care experiences of immigrants from low- and middle-income countries are different from what physicians are accustomed to seeing in the United States.8 These patients typically seek physicians only when they feel symptoms, and perhaps only when symptoms are severe. Even when patients are aware of chronic conditions, they may self-manage through nonallopathic approaches rather than through formal medical care. Therefore, as in this scenario, physicians should emphasize screening and prevention during sick visits in addition to well visits, because many Asian American patients will not schedule health maintenance visits. Table 1lists some preventive care considerations relevant to Asian Americans.9-20 Many items on the list can be accomplished with a simple blood draw and can be addressed without adding too much time to the office visit.
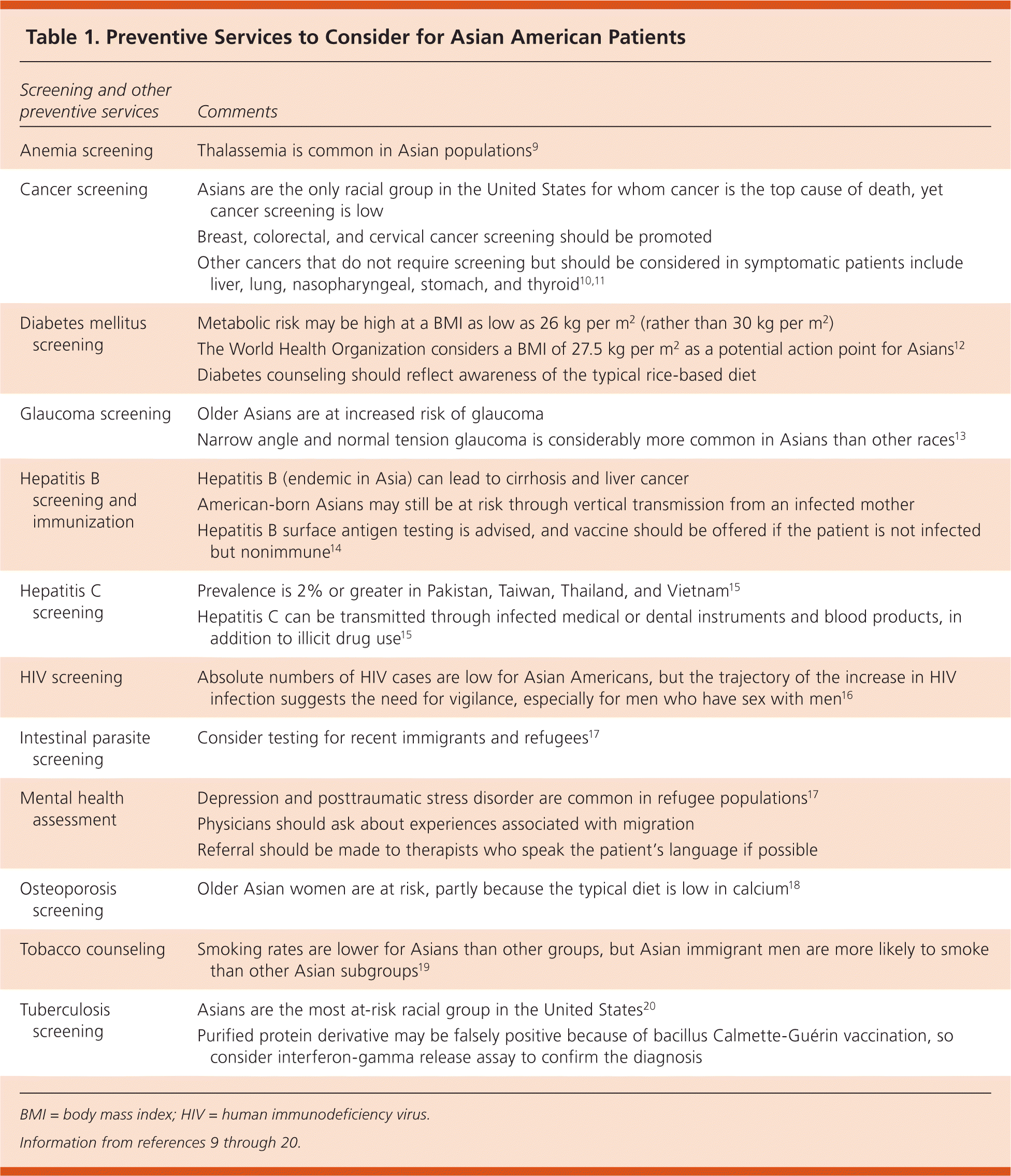
Table 1. Preventive Services to Consider for Asian American Patients
| Screening and other preventive services | Comments |
|---|---|
| Anemia screening | Thalassemia is common in Asian populations9 |
| Cancer screening | Asians are the only racial group in the United States for whom cancer is the top cause of death, yet cancer screening is low |
| Breast, colorectal, and cervical cancer screening should be promoted | |
| Other cancers that do not require screening but should be considered in symptomatic patients include liver, lung, nasopharyngeal, stomach, and thyroid10,11 | |
| Diabetes mellitus screening | Metabolic risk may be high at a BMI as low as 26 kg per m2 (rather than 30 kg per m2) |
| The World Health Organization considers a BMI of 27.5 kg per m2 as a potential action point for Asians12 | |
| Diabetes counseling should reflect awareness of the typical rice-based diet | |
| Glaucoma screening | Older Asians are at increased risk of glaucoma |
| Narrow angle and normal tension glaucoma is considerably more common in Asians than other races13 | |
| Hepatitis B screening and immunization | Hepatitis B (endemic in Asia) can lead to cirrhosis and liver cancer |
| American-born Asians may still be at risk through vertical transmission from an infected mother | |
| Hepatitis B surface antigen testing is advised, and vaccine should be offered if the patient is not infected but nonimmune14 | |
| Hepatitis C screening | Prevalence is 2% or greater in Pakistan, Taiwan, Thailand, and Vietnam15 |
| Hepatitis C can be transmitted through infected medical or dental instruments and blood products, in addition to illicit drug use15 | |
| HIV screening | Absolute numbers of HIV cases are low for Asian Americans, but the trajectory of the increase in HIV infection suggests the need for vigilance, especially for men who have sex with men16 |
| Intestinal parasite screening | Consider testing for recent immigrants and refugees17 |
| Mental health assessment | Depression and posttraumatic stress disorder are common in refugee populations17 |
| Physicians should ask about experiences associated with migration | |
| Referral should be made to therapists who speak the patient's language if possible | |
| Osteoporosis screening | Older Asian women are at risk, partly because the typical diet is low in calcium18 |
| Tobacco counseling | Smoking rates are lower for Asians than other groups, but Asian immigrant men are more likely to smoke than other Asian subgroups19 |
| Tuberculosis screening | Asians are the most at-risk racial group in the United States20 |
| Purified protein derivative may be falsely positive because of bacillus Calmette-Guérin vaccination, so consider interferon-gamma release assay to confirm the diagnosis |
BMI = body mass index; HIV = human immunodeficiency virus.
By using nonpreventive visits for preventive care, and by proactively addressing the health literacy, linguistic needs, and cultural nuances relevant to Asian American patients, primary care physicians can take full advantage of every opportunity to promote the care of a population that has often been underserved.

