Schizophrenia is the most common psychotic disease, with a global prevalence of less than 1%. It affects all ethnicities and is slightly more common in men. Patients with schizophrenia commonly experience debilitating social and occupational impairments, but some are able to function well with proper treatment. Symptom onset is generally between late adolescence and the mid-30s. There are two categories of symptoms: positive and negative. Hallucinations, delusions, and disorganized speech are examples of positive symptoms, whereas decreased emotional expression and lack of motivation are negative symptoms. Antipsychotic medications can treat some symptoms of schizophrenia but are associated with multiple adverse effects, including extrapyramidal symptoms and metabolic changes. Patients receiving antipsychotic medications, especially second-generation (or atypical) antipsychotics, should be monitored regularly for metabolic changes and cardiovascular risk factors. Persons with schizophrenia who undergo psychosocial therapy in addition to medical therapy have better outcomes. Patients diagnosed with schizophrenia have a higher overall mortality rate than the general public, partly because of the increased suicide risk associated with schizophrenia.
Schizophrenia is a pervasive, chronic mental disorder with a global prevalence of 0.3% to 0.7%.1 Although there is no significant difference between sexes, a slight predominance is noted in men.1,2 Schizophrenia affects persons in all ethnicities. However, a recent study confirmed that in the United States, blacks are diagnosed with schizophrenia at a disproportionately higher rate compared with non-Hispanic whites.3 This finding could point to a racial or ethnic bias in the diagnosis of schizophrenia in black persons who present with psychosis.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Patients who have been diagnosed with psychosis and/or schizophrenia should be urgently referred for psychiatric evaluation. | C | 8 |
| Antipsychotic drugs should be initiated as soon as possible after schizophrenia is diagnosed. | A | 1, 8, 10, 11, 13–15, 21, 25 |
| All patients receiving second-generation antipsychotic medications should be monitored at least annually for metabolic changes and cardiovascular risk factors. | C | 10, 28–30 |
| Patients with schizophrenia should be offered psychosocial therapies, including cognitive behavior therapy, family interventions, and social skills training, in addition to medical treatment. | B | 8–10, 13 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN PSYCHIATRY: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not prescribe antipsychotic medications to patients for any indication without appropriate initial evaluation and appropriate ongoing monitoring. | American Psychiatric Association |
| Do not routinely prescribe two or more antipsychotic medications concurrently. | American Psychiatric Association |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Schizophrenia is the most common psychotic disease.4 Therefore, family physicians should have an overall knowledge of the disease, including the initial presentation, treatment and its challenges, and how to address comorbidities. Whenever possible, family physicians should educate patients and their families about medication reactions and the importance of compliance with treatment. Referral to a psychiatrist is appropriate for patients presenting with psychosis.
Etiology and Risk Factors
Genetics have an important role in the etiology of schizophrenia, even though most patients diagnosed with the disease have no family history of psychosis. The genetic variation responsible for the disease has not been identified. Relatives of persons with schizophrenia are also at risk of schizoaffective disorder, schizotypal personality disorder, bipolar disorder, depression, and autism spectrum disorder.1,5
Environmental factors may have a role.1 Possible environmental factors include being born and raised in an urban area, cannabis use, infection with Toxoplasma gondii,2,6,7 obstetric complications, central nervous system infection in early childhood, and advanced paternal age (older than 55 years).1
Clinical Presentation
The symptoms of schizophrenia usually begin between late adolescence and the mid-30s. Cases involving children as young as five years have been reported, but these are rare. In men, the symptoms tend to present between 18 and 25 years of age. In women, the onset of symptoms has two peaks, the first between 25 years of age and the mid-30s, and the second after 40 years of age.1
Patients may have symptoms during a prodromal phase before they become psychotic. These symptoms include social withdrawal, loss of interest in work or school, deterioration of hygiene, angry outbursts, and behavior that is out of character.1 This phase may be mistaken for depression or other mood disorders. The patient will eventually exhibit active-phase symptoms of the disorder.1
Diagnosis
Criteria for schizophrenia include signs and symptoms of at least six months' duration, including at least one month of active-phase positive and negative symptoms (Table 1).1 Delusions, hallucinations, disorganized speech, and disorganized behavior are examples of positive symptoms. Negative symptoms include a decrease in the range and intensity of expressed emotions (i.e., affective flattening) and a diminished initiation of goal-directed activities (i.e., avolition).
Table 1. Diagnostic Criteria for Schizophrenia

| A. Two (or more) of the following, each present for a significant portion of time during a 1-month period (or less if successfully treated). At least one of these must be (1), (2), or (3): | |
| 1. Delusions | |
| 2. Hallucinations | |
| 3. Disorganized speech (e.g., frequent derailment or incoherence) | |
| 4. Grossly disorganized or catatonic behavior | |
| 5. Negative symptoms (i.e., diminished emotional expression or avolition) | |
| B. For a significant portion of the time since the onset of the disturbance, level of functioning in one or more major areas, such as work, interpersonal relations, or self-care, is markedly below the level achieved prior to the onset (or when the onset is in childhood or adolescence, there is failure to achieve expected level of interpersonal, academic, or occupational functioning) | |
| C. Continuous signs of the disturbance persist for at least 6 months. This 6-month period must include at least 1 month of symptoms (or less if successfully treated) that meet Criterion A (i.e., active-phase symptoms) and may include periods of prodromal or residual symptoms. During these prodromal or residual periods, the signs of the disturbance may be manifested by only negative symptoms or by two or more symptoms listed in Criterion A present in an attenuated form (e.g., odd beliefs, unusual perceptual experiences) | |
| D. Schizoaffective disorder and depressive or bipolar disorder with psychotic features have been ruled out because either: (1) no major depressive or manic episodes have occurred concurrently with the active-phase symptoms, or (2) if mood episodes have occurred during active-phase symptoms, they have been present for a minority of the total duration of the active and residual periods of the illness | |
| E. The disturbance is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a medication) or another medical condition | |
| F. If there is a history of autism spectrum disorder or a communication disorder of childhood onset, the additional diagnosis of schizophrenia is made only if prominent delusions or hallucinations, in addition to the other required symptoms of schizophrenia, are also present for at least 1 month (or less if successfully treated) | |
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Association; 2013:99.
DIFFERENTIAL DIAGNOSIS
Other organic and psychiatric diagnoses can present with symptoms of psychosis (Table 2).1 Initially, patients should be evaluated for any intrinsic cause of psychosis (e.g., delirium, mood disorder with psychosis, Cushing syndrome, drug use [illicit and prescribed]). Ideally, patients should be observed in a controlled setting for an extended time. This allows for differentiation between psychiatric disorders; however, this is not always feasible. In most situations, physicians must rely on a history provided by family members.1 The physical examination will also help determine organic causes of psychosis.
Table 2. Differential Diagnosis of Schizophrenia

| Diagnosis | Distinguishing features | Laboratory/imaging findings |
|---|---|---|
| Psychiatric conditions | ||
| Brief psychotic disorder | Delusions, hallucinations, and disorganized speech or behavior lasting for at least one day but less than one month | NA |
| Major depressive or bipolar disorder with psychotic or catatonic features | Psychotic symptoms occur exclusively during periods of mood disturbance | NA |
| Posttraumatic stress disorder | Traumatic inciting event; symptoms relate to reliving or reacting to the event | NA |
| Obsessive-compulsive disorder and body dysmorphic disorder | Prominent obsessions, compulsions, and preoccupations with appearance or body odor, hoarding, or body-focused repetitive behaviors | NA |
| Schizotypal personality disorder | Subthreshold symptoms that are associated with persistent personality features | NA |
| Autism spectrum disorder or communication disorders | Deficits in social interaction with repetitive and restricted behaviors and other cognitive and communication deficits | NA |
| Schizoaffective disorder | Mood episode concurrent with active-phase symptoms; mood symptoms present for a substantial portion of the disturbance; delusions present for two weeks without prominent mood symptoms | NA |
| Schizophreniform disorder | Duration of symptoms is at least one month but less than six months | NA |
| Delusional disorder | Nonbizarre delusions, absence of hallucinations, disorganized speech or behavior, negative symptoms | NA |
| Medical conditions | ||
| Substance abuse | Abnormal vital signs, needle marks, poor nutrition | Elevated blood alcohol level, positive results on urine drug screen |
| Thyroid disorder | Coarse hair and skin, exophthalmos, goiter, pretibial myxedema, tachycardia/bradycardia, tremor | Abnormal thyroid-stimulating hormone level, anemia, hyponatremia |
| Delirium caused by infection | Altered consciousness, fever, hyporeflexia/hyperreflexia, hypotension, infection source | Abnormal leukocyte count, positive results on human immunodeficiency virus or rapid plasma reagin test |
| Dementia | Cognitive/memory deficits, abnormal results on Mini-Mental State Examination | NA |
| Vitamin B12 deficiency | Ataxia, atrophic glossitis, memory impairment, muscle weakness | Elevated iron and indirect bilirubin levels, low vitamin B12 levels, macrocytic anemia |
| Systemic lupus erythematosus | Alopecia, discoid rash, fever, malar rash, oral ulcers, phlebitis, pleural/pericardial rub | Anemia, elevated antinuclear antibody titers, pleural effusion detected on chest radiography, proteinuria |
| Cushing syndrome | Abdominal striae, buffalo hump, hirsutism, moon face, proximal muscle weakness | Elevated 24-hour urine cortisol level |
| Temporal lobe epilepsy | Postictal state, abnormal neurologic findings | Abnormal electroencephalography findings |
| Brain tumor | Focal neurologic deficits | Lesions detected on computed tomography or magnetic resonance imaging of the brain |
| Wilson disease | Ataxia, dysarthria, hepatomegaly, hyperreflexia, jaundice, Kayser-Fleischer rings in the cornea | Basal ganglia lesions detected on magnetic resonance imaging, Coombs-negative hemolytic anemia, elevated liver enzyme levels |
| Porphyria | Proximal muscle weakness, tachycardia | Elevated urine porphobilinogen level, hyponatremia |
note: Diagnoses are listed from most to least prevalent.
NA = not applicable.
Information from reference 1.
Treatment
Patients diagnosed with psychosis, schizophrenia, or both should be urgently referred for psychiatric evaluation.8 Not all patients with acute psychosis require hospitalization, but it should be considered for those who may pose a danger to themselves or others.4 The most effective treatment for schizophrenia is a multidisciplinary approach including medication, psychological treatment, and social support.5,9–11 The goal of treatment is remission, which is defined as a period of six months with no symptoms or mild symptoms that do not interfere with a person's behaviors.12
ANTIPSYCHOTICS
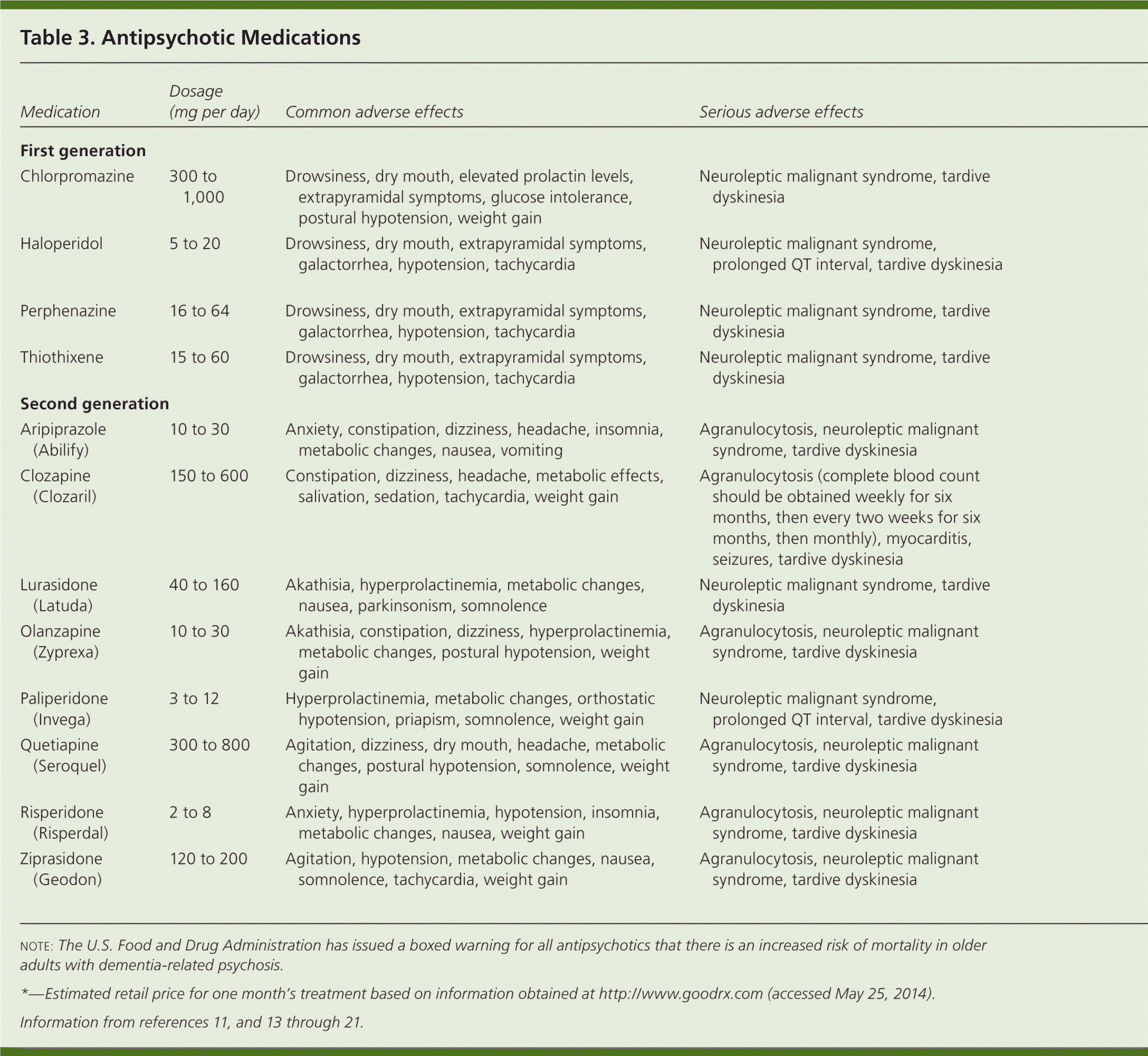
Antipsychotic agents are the first-line treatment for patients with schizophrenia. There are two general types of antipsychotic drugs: first-generation (typical) and second-generation (atypical) agents. Table 3 lists commonly used antipsychotic drugs, their adverse effects, typical dosages, and price.11,13–21 Multiple guidelines recommend starting antipsychotic medications as soon as possible after psychotic symptoms are recognized and/or the patient is diagnosed with schizophrenia.8,10,11,13,21,22 The National Institute for Health and Care Excellence suggests urgent referral to mental health services when a person presents with psychotic symptoms, and recommends that primary care physicians initiate antipsychotic medications only in consultation with a psychiatrist (Table 4).8 Initial medication choice should be individualized, taking into account financial considerations, adverse effect profiles, dosing regimens, and patient preferences.
Table 3. Antipsychotic Medications
| Medication | Dosage (mg per day) | Common adverse effects | Serious adverse effects | Comments | Monthly cost* |
|---|---|---|---|---|---|
| First generation | |||||
| Chlorpromazine | 300 to 1,000 | Drowsiness, dry mouth, elevated prolactin levels, extrapyramidal symptoms, glucose intolerance, postural hypotension, weight gain | Neuroleptic malignant syndrome, tardive dyskinesia | First drug used to treat psychosis | $235 to $590 |
| Haloperidol | 5 to 20 | Drowsiness, dry mouth, extrapyramidal symptoms, galactorrhea, hypotension, tachycardia | Neuroleptic malignant syndrome, prolonged QT interval, tardive dyskinesia | More effective for treating positive symptoms,13 but has a high risk of extrapyramidal symptoms14 | $5 to $30 |
| Perphenazine | 16 to 64 | Drowsiness, dry mouth, extrapyramidal symptoms, galactorrhea, hypotension, tachycardia | Neuroleptic malignant syndrome, tardive dyskinesia | — | $55 to $215 |
| Thiothixene | 15 to 60 | Drowsiness, dry mouth, extrapyramidal symptoms, galactorrhea, hypotension, tachycardia | Neuroleptic malignant syndrome, tardive dyskinesia | — | $35 to $45 |
| Second generation | |||||
| Aripiprazole (Abilify) | 10 to 30 | Anxiety, constipation, dizziness, headache, insomnia, metabolic changes, nausea, vomiting | Agranulocytosis, neuroleptic malignant syndrome, tardive dyskinesia | Smaller effect on lipids compared with other second-generation antipsychotics15 | ($825 to $1,165 brand) |
| Clozapine (Clozaril) | 150 to 600 | Constipation, dizziness, headache, metabolic effects, salivation, sedation, tachycardia, weight gain | Agranulocytosis (complete blood count should be obtained weekly for six months, then every two weeks for six months, then monthly), myocarditis, seizures, tardive dyskinesia | Reserved for severe, treatment-refractory schizophrenia11 | $80 to $200 ($510 to $2,010 brand) |
| Lurasidone (Latuda) | 40 to 160 | Akathisia, hyperprolactinemia, metabolic changes, nausea, parkinsonism, somnolence | Neuroleptic malignant syndrome, tardive dyskinesia | Higher incidence of adverse effects with higher dosages16 | ($745 to $1,490 brand) |
| Olanzapine (Zyprexa) | 10 to 30 | Akathisia, constipation, dizziness, hyperprolactinemia, metabolic changes, postural hypotension, weight gain | Agranulocytosis, neuroleptic malignant syndrome, tardive dyskinesia | More weight gain compared with older second-generation antipsychotics, but a lower discontinuation rate17,18 | $15 to $45 ($590 to $1,760 brand) |
| Paliperidone (Invega) | 3 to 12 | Hyperprolactinemia, metabolic changes, orthostatic hypotension, priapism, somnolence, weight gain | Neuroleptic malignant syndrome, prolonged QT interval, tardive dyskinesia | Active metabolite of risperidone | ($775 to $1,550 brand) |
| Quetiapine (Seroquel) | 300 to 800 | Agitation, dizziness, dry mouth, headache, metabolic changes, postural hypotension, somnolence, weight gain | Agranulocytosis, neuroleptic malignant syndrome, tardive dyskinesia | High discontinuation rate compared with other second-generation antipsychotics19 | $25 to $45 ($530 to $1,235 brand) |
| Risperidone (Risperdal) | 2 to 8 | Anxiety, hyperprolactinemia, hypotension, insomnia, metabolic changes, nausea, weight gain | Agranulocytosis, neuroleptic malignant syndrome, tardive dyskinesia | Higher incidence of extrapyramidal effects, increased prolactin levels18,20 | $10 to $20 ($400 to $1,255 brand) |
| Ziprasidone (Geodon) | 120 to 200 | Agitation, hypotension, metabolic changes, nausea, somnolence, tachycardia, weight gain | Agranulocytosis, neuroleptic malignant syndrome, tardive dyskinesia | Least amount of weight gain compared with other second-generation antipsychotics21 | $135 to $170 ($830 to $1,060 brand) |
note: The U.S. Food and Drug Administration has issued a boxed warning for all antipsychotics that there is an increased risk of mortality in older adults with dementia-related psychosis.
*—Estimated retail price for one month's treatment based on information obtained at http://www.goodrx.com (accessed May 25, 2014).
Table 4. National Institute for Health and Care Excellence Guidelines for Management of Schizophrenia

| All persons presenting with psychotic symptoms should be urgently referred to mental health services |
| Antipsychotic medication for a first presentation of sustained psychotic symptoms should not be initiated in the primary care setting unless it is done in consultation with a psychiatrist |
| Patients should be offered an antipsychotic medication when they are initially diagnosed with schizophrenia |
| The risks and benefits of the medication should be discussed with the patient |
| Potential adverse effects should be considered when deciding on a medication |
| A combination of antipsychotics should not be prescribed |
| A loading dose of antipsychotics should not be prescribed |
| Oral antipsychotics should be offered to patients with acute exacerbations or recurrences of psychotic symptoms |
| Patients with schizophrenia should be informed of the high risk of relapse if medical therapy is discontinued within one to two years |
| Physical examinations and cardiovascular risk assessment should be performed at least annually in patients with schizophrenia, and results should be shared with the psychiatrist |
| Cognitive behavior therapy should be offered to all persons with schizophrenia |
| Patients whose symptoms have responded to treatment and remain stable should be given the option of returning to their primary care physician for continued management |
| Physicians should consider re-referral to mental health services if there is poor treatment response, nonadherence to treatment, intolerable adverse effects of medications, or comorbid substance use, or if the patient is a threat to him- or herself or others |
Information from reference 8.
Antipsychotic medications are more effective than placebo in reducing overall symptoms of schizophrenia and preventing relapse.13–15 Patients with schizophrenia who are receiving antipsychotic drugs report a better quality of life, but have a higher incidence of weight gain, sedation, and movement disorders.15 As such, all patients who report symptom relief while receiving medication should be offered maintenance therapy with antipsychotics.11 A patient's response to treatment during the first two to four weeks is highly predictive of long-term response, although it may take several months to achieve maximal effect.17 Patients should be given an adequate trial of therapy (at least four weeks at a therapeutic dose) before discontinuing the drug or transitioning to a different medication.22
Studies have shown that there is no difference in effectiveness between first- and second-generation antipsychotics.23,24 Quality of life is also similar at one year between groups of patients treated with each drug class.23 The main difference between these medications is their adverse effect profiles; first-generation antipsychotics most commonly cause extrapyramidal symptoms, whereas second-generation agents most commonly cause weight gain and metabolic changes.22,25–27 Adverse reactions and previous response to antipsychotic medications should be taken into account when deciding which class of medication to initiate.
ADVERSE EFFECTS AND MONITORING
Extrapyramidal symptoms such as pseudoparkinsonism, akathisia (a sensation of inner restlessness and inability to be still), and dystonia are associated with first-generation antipsychotics. Patients receiving these medications should be routinely monitored for adverse effects and maintained on the lowest effective dose that controls their symptoms. Medications such as propranolol, lorazepam (Ativan), amantadine, benztropine, and diphenhydramine (Benadryl) are used to treat extrapyramidal symptoms.25 Tardive dyskinesia involving facial muscles generally occurs after the patient has been taking antipsychotic medications for a prolonged time. Symptoms include puffing of the cheeks, protrusion of the tongue, chewing motions, and pursing of the lips. The condition is typically irreversible, but symptoms may lessen after the medication is discontinued. Laboratory monitoring is not necessary for patients receiving first-generation antipsychotics. Patients receiving the second-generation antipsychotic clozapine (Clozaril) are at high risk of agranulocytosis, and the package insert recommends a complete blood count weekly for six months, then every two weeks for an additional six months, then monthly. Clozapine is reserved for patients with severe refractory symptoms because of its increased risk of adverse effects; it should be prescribed only by a psychiatrist.11
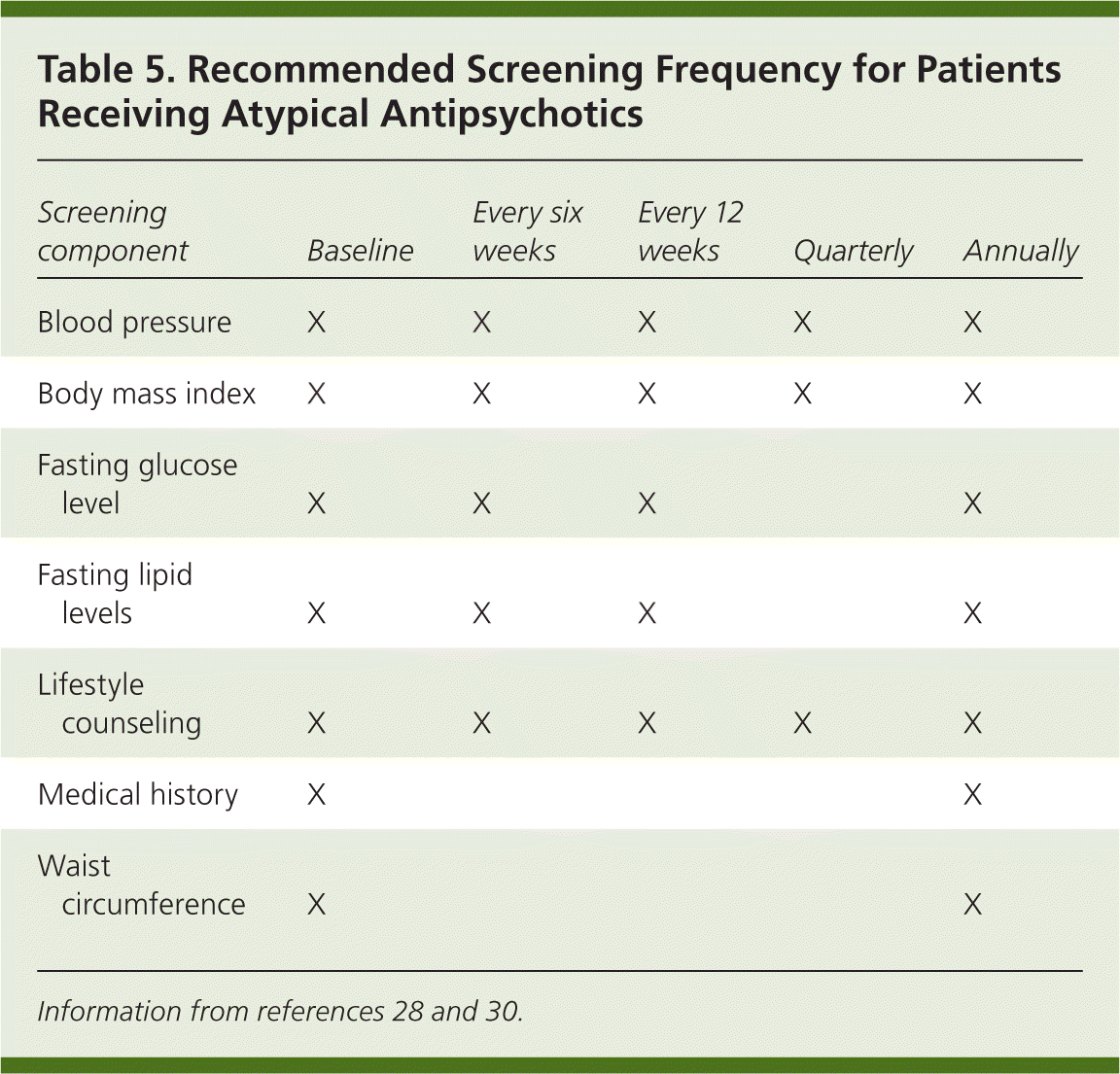
The most worrisome adverse effects associated with second-generation antipsychotics are metabolic changes, such as weight gain, insulin resistance, hyperglycemia, and lipid abnormalities.15,25,27,28 All second-generation antipsychotics confer varying degrees of risk for metabolic changes,28 and these effects are not dose-dependent.29 Weight gain is usually rapid in the first few weeks of treatment, then plateaus; however, this can take a year or more to occur.27 Therefore, patients should be examined frequently after initiating treatment with second-generation antipsychotics, and at least annually if they have normal baseline values. Patients with cardiovascular risk factors require more frequent monitoring.28,30 Table 5 outlines the recommended frequency of monitoring for patients receiving second-generation antipsychotics.28,30 Primary care physicians should regularly assess body mass index, fasting glucose levels, and lipid profiles, and work toward minimizing these and other cardiovascular risk factors.8,30,31
Table 5. Recommended Screening Frequency for Patients Receiving Atypical Antipsychotics
ADJUNCTIVE TREATMENTS
In addition to medication, patients with schizophrenia should be offered adjunctive therapies such as cognitive behavior therapy, family interventions, and social skills training.8–10,13 Cognitive behavior therapy is the most commonly used adjunctive therapy, but a Cochrane review found no clear evidence that it is superior to other talking therapies, although it may be helpful in dealing with emotions and distressing feelings.32 A Chinese study found that psychosocial treatment combined with medication improved treatment adherence, insight, and quality of life, and decreased hospital admissions.9 Patients receiving combined treatment were less likely to discontinue their medication or to relapse (absolute risk reduction = 14% and 8%; number needed to treat = 7 and 12, respectively).
There is a higher incidence of anxiety disorders, panic symptoms, posttraumatic stress disorder, and obsessive compulsive disorder in patients with schizophrenia compared with the general public.33 Medications such as selective serotonin reuptake inhibitors and anxiolytics can be helpful in treating comorbid mood disorders in these patients, but do not treat the symptoms of schizophrenia.34
Clinical Course and Prognosis
Patients with schizophrenia have a varied clinical course that may include remission, exacerbations, or a more persistent chronic illness. Among patients who remain ill despite therapy, some have a stable clinical course, whereas others experience worsening symptoms and functioning. Factors that predict the clinical course and prognosis of these patients are not understood, and there is no reliable way to predict outcomes. Approximately 20% of patients can be expected to have a positive outcome.1
Suicide is a concern when treating patients with schizophrenia. The risk of suicide is 13 times greater in persons diagnosed with schizophrenia compared with the general public, with a lifetime risk of about 5%.1,4,35 Patients with auditory hallucinations, delusions, substance abuse, or a history of suicide attempts are at higher risk. Adequate treatment of schizophrenia and its comorbidities, along with diligent screening for risk factors, reduces the likelihood of suicide.35 The overall mortality rate for patients with schizophrenia is two to three times higher than that of the general public.1,36 Most deaths are related to an increased rate of cardiovascular and respiratory diseases, stroke, cancer, and thromboembolic events.36
In the past, schizophrenia was viewed as a disease with a poor prognosis. Currently, the disease course and response to treatment are marked by heterogeneity; differences in treatment response, disease course, and prognosis are to be expected.5,12 Despite adequate treatment, one-third of patients will remain symptomatic. Although most patients need some form of support, most are able to live independently and actively participate in their lives.5
Data Sources: We were provided a search from Essential Evidence Plus using the search term schizophrenia. We searched the National Institute for Health and Care Excellence, U.S. Preventive Services Task Force, and Agency for Healthcare Research and Quality. A PubMed search was completed using the search subjects schizophrenia, schizophrenia diagnosis, schizophrenia treatment, and schizophrenia prognosis. Search dates: March and September 2012, and August 2014.
The authors thank Monica Kalra, DO; Robert Suter, DO; Khadija Kabani, DO; Brenda Wilson; and Sharon West for their assistance with the preparation of the manuscript.