Benign prostatic hyperplasia (BPH) is a common condition that increases in prevalence with age. A history should include onset, duration, and severity of lower urinary tract symptoms and medication use to rule out other causes of symptoms. Physical examination includes a digital rectal examination and assessment for bladder distention or neurologic impairment. Recommended tests include serum prostate-specific antigen measurement and urinalysis to help identify infection, genitourinary cancer, or calculi as an alternative cause of lower urinary tract symptoms. BPH severity is assessed using validated, self-administered symptom questionnaires such as the American Urological Association Symptom Index or International Prostate Symptom Score. Mild or nonbothersome symptoms do not require treatment. Bothersome symptoms are managed with lifestyle modifications, medications, and surgery. Alpha blockers are first-line medications for BPH. Surgical referral is indicated if BPH-related complications develop, medical therapy fails, or the patient chooses it. Dietary supplements, such as saw palmetto, pygeum, cernilton, and beta sitosterols, and acupuncture are not recommended for the management of BPH.
The prevalence of benign prostatic hyperplasia (BPH) increases with age.1 BPH can present as lower urinary tract symptoms such as incomplete emptying, frequency, intermittency, urgency, weak stream, straining, or nocturia. The physician must determine if the symptoms are secondary to BPH or other causes and provide appropriate treatment. This article provides evidence-based answers to common questions about the diagnosis and management of BPH.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should obtain a history and perform a physical examination, including digital rectal examination and assessment for bladder distention and neurologic impairment, to rule out causes of lower urinary tract symptoms independent of BPH. | C | 2, 3 |
| Recommended tests for men with symptoms of BPH include serum prostate-specific antigen and urinalysis. | C | 2, 3, 11 |
| Alpha blockers are effective first-line treatments for patients with bothersome, moderate to severe BPH symptoms. | A | 2, 15, 19 |
| The addition of a 5-alpha reductase inhibitor is effective in men with bothersome, moderate to severe BPH symptoms and a documented enlarged prostate when alpha-blocker monotherapy is not effective. | A | 2, 9, 23, 26, 27 |
| Complementary and alternative treatments (e.g., saw palmetto) are not recommended for the management of BPH. | B | 2, 29–33 |
BPH = benign prostatic hyperplasia.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN UROLOGY: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not order creatinine or upper-tract imaging for patients with benign prostatic hyperplasia. | American Urological Association |
source: For more information on the Choosing Wisely Campaign, see https://www.aafp.org/afp/choosingwisely. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
What Should Be Included in the History and Physical Examination in Men with Symptoms Suggesting BPH?
Onset, duration, and severity of lower urinary tract symptoms, along with additional history to rule out other causes of symptoms, should be determined. Physical examination should include a digital rectal examination and assessment for bladder distention or neurologic impairment.
EVIDENCE SUMMARY
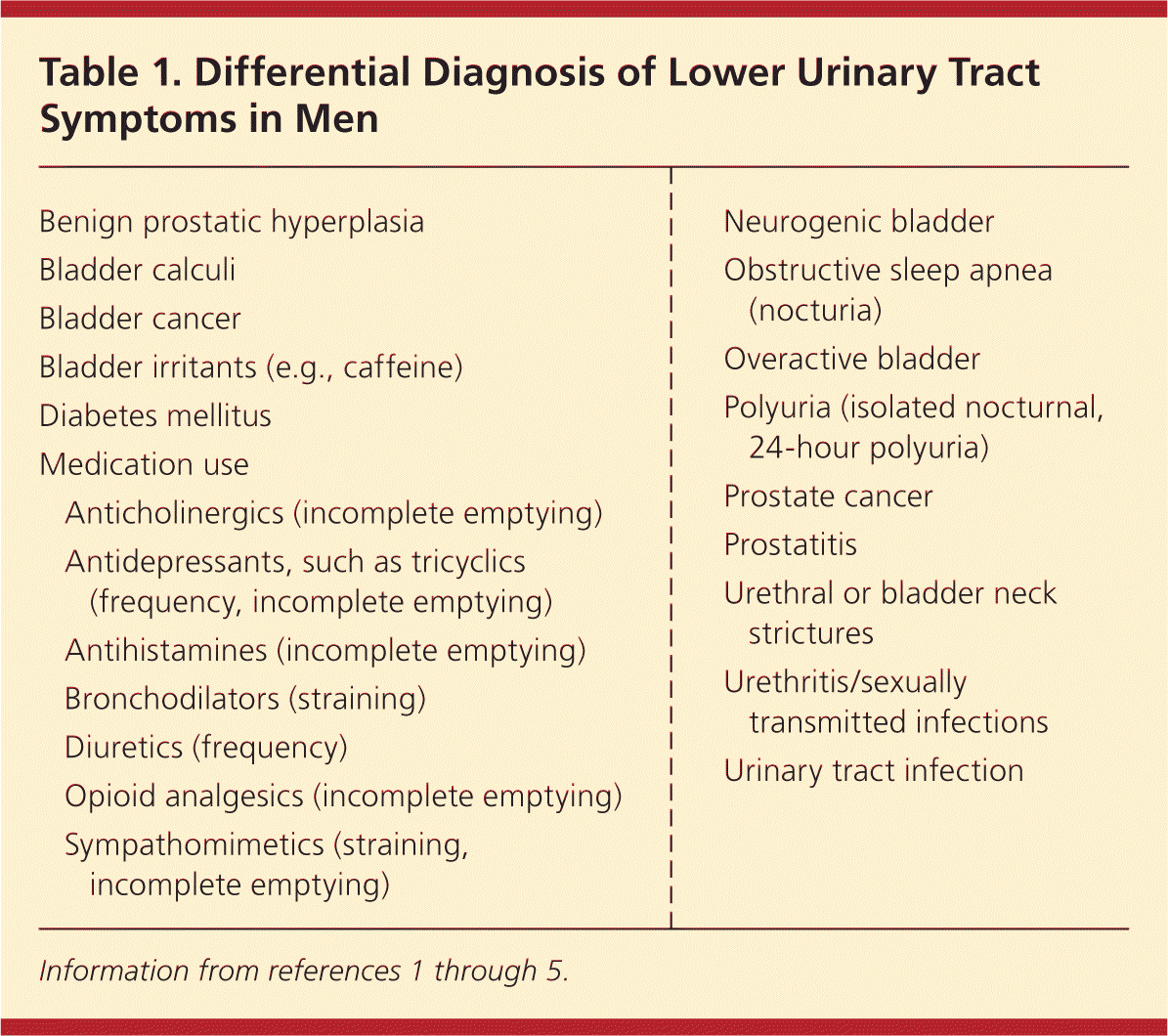
The initial history and physical examination focus on excluding etiologies of lower urinary tract infections other than BPH (Table 1).1–5 In addition to onset and duration of symptoms, any history of fever, dysuria, gross hematuria, pain suggestive of stones, or previous urethral instrumentation should be obtained. Identification of medication use is helpful because medications account for 10% of lower urinary tract symptoms in men.4 Other key information includes history of diabetes mellitus, tobacco use, intake of bladder irritants (e.g., caffeine), sexual dysfunction, or conditions resulting in neurologic impairment (e.g., neurogenic bladder), and a personal or family history of prostate or bladder cancer.2,5 Assessing overall health can guide eligibility for future medical and surgical interventions.2
Table 1. Differential Diagnosis of Lower Urinary Tract Symptoms in Men
| Benign prostatic hyperplasia | |
| Bladder calculi | |
| Bladder cancer | |
| Bladder irritants (e.g., caffeine) | |
| Diabetes mellitus | |
| Medication use | |
| Anticholinergics (incomplete emptying) | |
| Antidepressants, such as tricyclics (frequency, incomplete emptying) | |
| Antihistamines (incomplete emptying) | |
| Bronchodilators (straining) | |
| Diuretics (frequency) | |
| Opioid analgesics (incomplete emptying) | |
| Sympathomimetics (straining, incomplete emptying) | |
| Neurogenic bladder | |
| Obstructive sleep apnea (nocturia) | |
| Overactive bladder | |
| Polyuria (isolated nocturnal, 24-hour polyuria) | |
| Prostate cancer | |
| Prostatitis | |
| Urethral or bladder neck strictures | |
| Urethritis/sexually transmitted infections | |
| Urinary tract infection | |
The physical examination should include a digital rectal examination assessing prostate size, nodularity, and asymmetry, which may raise suspicion for malignancy.2 A digital rectal examination is recommended by the American Urological Association (AUA) despite limitations such as interexaminer variability, low sensitivity (59%), and low positive predictive value (28%) for detecting prostate cancer.2,6,7 The physician should assess for bladder distention, motor and sensory deficits of the lower extremities and perineum, and decreased anal sphincter tone to identify neurogenic bladder as a cause of lower urinary tract symptoms independent of BPH.3
How Is BPH Severity Quantified?
BPH severity is quantified using a validated, self-administered symptom questionnaire such as the AUA Symptom Index (AUA-SI) or International Prostate Symptom Score (I-PSS).
EVIDENCE SUMMARY
Assessing BPH severity is important because it guides management decisions. The AUA-SI (Figure 1) has been validated as a clinical tool and may be used throughout management.8 BPH severity is quantified as mild (AUA-SI score of 0 to 7), moderate (8 to 19), and severe (20 to 35). A three- or four-point improvement in AUA-SI score is clinically significant.2,9 The I-PSS is identical to the AUA-SI but asks one more question regarding impact of symptoms on quality of life, which can help guide management.10
Figure 1. American Urological Association Symptom Index
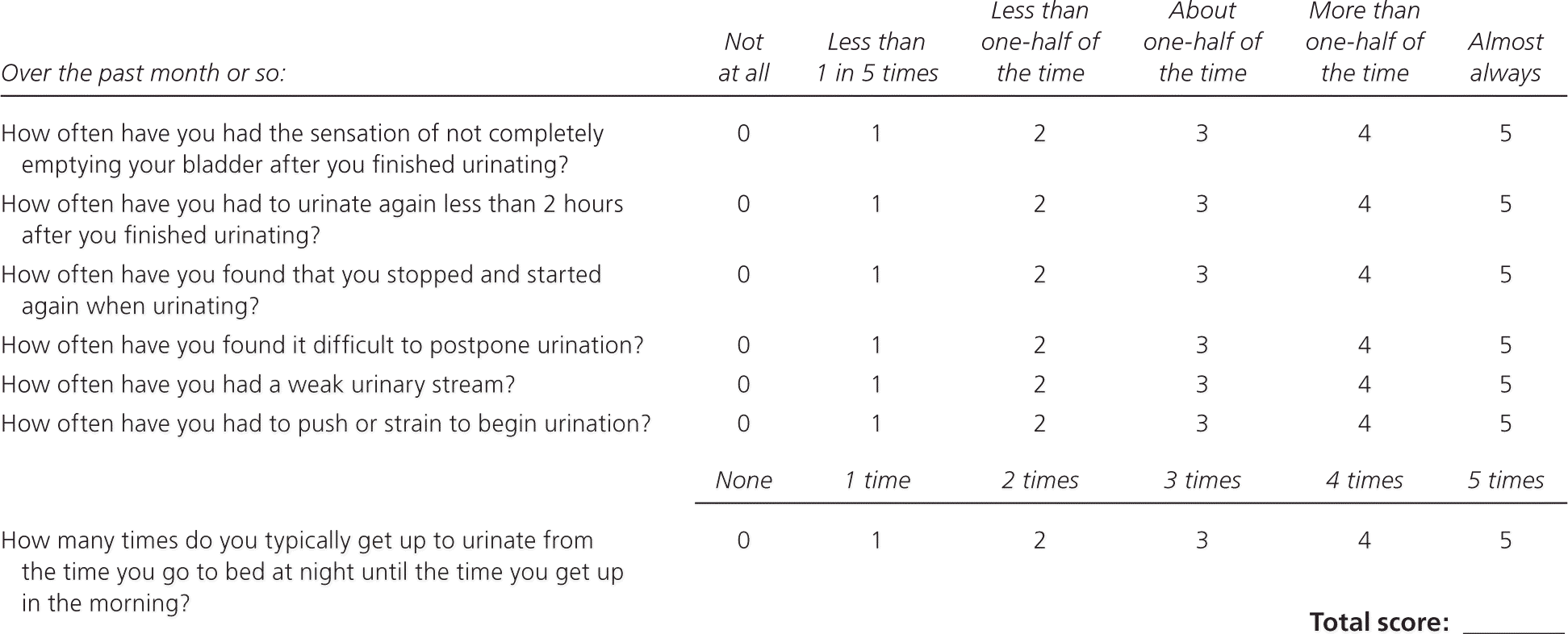
American Urological Association Symptom Index to assess severity of benign prostatic hyperplasia (BPH). A score of 0 to 7 indicates mild BPH, 8 to 19 moderate BPH, and 20 to 35 severe BPH.
Adapted with permission from Barry MJ, Fowler FJ Jr, O'Leary MP, et al.; The Measurement Committee of the American Urological Association. The American Urological Association symptom index for benign prostatic hyperplasia. J Urol. 1992;148(5):1555.
What Tests Are Recommended in Men with Symptoms Suggesting BPH?
Recommended tests are serum prostate-specific antigen (PSA) measurement and urinalysis. Optional tests include postvoid residual urine measurement if history and physical examination findings suggest urinary retention, and use of a frequency volume chart if nocturia is the predominant symptom. Pressure flow studies, ultrasonography of the prostate or upper urinary tract, endoscopy of the lower urinary tract, and serum creatinine measurement are not recommended.
EVIDENCE SUMMARY
The purpose of laboratory or radiologic testing is to identify alternative causes of symptoms (Table 1).1–5 A urinalysis is recommended in all men with lower urinary tract symptoms.2,3,11 Additional workup and treatment should be pursued if hematuria, proteinuria, or evidence of urinary tract infection is found. The AUA recommends a serum PSA measurement in men with lower urinary tract symptoms and a life expectancy greater than 10 years.2 BPH is not an established risk factor for prostate cancer; the risk of prostate cancer is lower in men with lower urinary tract symptoms and an elevated PSA level than in those without symptoms.12 The decision to order a PSA measurement should be individualized after discussing with the patient the risks of false-positive and false-negative results, as well as the possible need for biopsy.2,12
Postvoid residual urine measurement using a bladder scanner (normal residual urine is less than 100 mL) should be performed if history and physical examination suggest urinary retention.2,3,13 If significant nocturia is the main symptom, consider using a frequency volume chart that documents date/time, fluid intake, and urine voided (eFigure A) or a sleep study to find alternative causes, such as isolated nocturnal polyuria (more than 33% of urine output at night), 24-hour polyuria (3 L or more of urinary output in 24 hours), or sleep apnea.2,3
eFigure A. Frequency Volume Chart

Frequency volume charts are useful if nocturia (≥ 2 voids per night) is the main symptom. This chart can identify isolated nocturnal polyuria (≥ 33% of urine output occurring at night) or 24-hour polyuria (≥ 3 L of urinary output in 24 hours).
Information from McVary KT, Roehrborn CG, Avins AL, et al. Update on AUA guideline on the management of benign prostatic hyperplasia. J Urol. 2011;185(5):1793–1803, and Abrams P, Chapple C, Khoury S, Roehrborn C, de la Rosette J; International Scientific Committee. Evaluation and treatment of lower urinary tract symptoms in older men. J Urol. 2009;181(4):1779–1787.
Pressure flow studies, ultrasonography of the prostate or upper urinary tract, and endoscopy of the lower urinary tract are not recommended in the routine evaluation of lower urinary tract symptoms.2,3 Serum creatinine measurement is not indicated because the incidence of baseline renal insufficiency in men with BPH is similar to that in the general population.2,9
How Should BPH Severity Guide Management?
Mild symptoms (AUA-SI score of 0 to 7) as well as nonbothersome moderate (8 to 19) to severe (20 to 35) symptoms require no treatment. Individuals bothered by moderate to severe lower urinary tract symptoms can be treated with lifestyle modifications, medications, and surgery.
EVIDENCE SUMMARY
Most men with BPH and symptoms that do not impact quality of life are unlikely to experience future complications.2,9,14 As a result, men presenting with mild symptoms or nonbothersome moderate to severe symptoms do not require further treatment.2,14 In the Medical Therapy of Prostatic Symptoms Study, the placebo arm (n = 737) demonstrated BPH progression (i.e., four-point increase in AUA-SI score, acute urinary retention, renal insufficiency, recurrent urinary tract infection, or urinary incontinence) at a rate of 4.5 events per 100 person-years.9
Men presenting with bothersome, moderate to severe BPH symptoms may be treated with lifestyle modifications, medications, or surgery (Table 2).2,3,5,14–22 Regardless of symptom severity score, complicated lower urinary tract symptoms (suspicious digital rectal examination findings, hematuria, abnormal PSA findings, recurrent infection, distended bladder, or neurologic disease) should prompt a referral to urology before treatment is initiated.2
Table 2. Treatment Options for Bothersome, Moderate to Severe Benign Prostatic Hyperplasia

| Lifestyle modifications |
| Losing weight |
| Decreasing evening fluid intake |
| Avoiding excess alcohol, caffeine, or highly seasoned foods |
| Limiting medications known to cause lower urinary tract symptoms |
| Medications |
| Alpha blockers |
| 5-alpha reductase inhibitors |
| Anticholinergic agents |
| Surgery |
| Photoselective vaporization of the prostate |
| Transurethral incision of the prostate |
| Transurethral laser prostatectomy (holmium:yttrium-aluminum-garnet [YAG] laser ablation, enucleation, or resection of the prostate) |
| Transurethral microwave thermotherapy |
| Transurethral needle ablation of the prostate |
| Transurethral resection of the prostate |
| Transurethral vaporization of the prostate |
Which Medical Therapies Are Effective in the Management of BPH?
Alpha blockers are effective for bothersome, moderate to severe BPH and are recommended in men not undergoing planned cataract surgery. The combination of alpha blockers and 5-alpha reductase inhibitors is effective for long-term management of BPH and demonstrated large prostates. Anticholinergic agents can benefit selected patients with predominantly irritative lower urinary tract symptoms and a normal postvoid residual urine measurement.
EVIDENCE SUMMARY
Alpha Blockers. Alpha blockers antagonize alpha1-receptors in the prostatic urethra and bladder neck, resulting in smooth muscle relaxation and improvement of lower urinary tract symptoms, typically within two to four weeks after initiation.2 The AUA recommends the alpha blockers alfuzosin (Uroxatral), doxazosin (Cardura), tamsulosin (Flomax), and terazosin as first-line treatments for men with BPH and bothersome, moderate to severe symptoms.2 A meta-analysis of 21 studies (n = 6,333) comparing these four alpha blockers with placebo demonstrated 30% to 45% improvement in symptom scores over one month to one year; the alpha blockers were equally effective.15 Silodosin (Rapaflo) is another alpha blocker with demonstrated effectiveness in BPH management.19 The evidence for phenoxybenzamine (Dibenzyline) and prazosin (Mini-press) is insufficient, and these medications are not recommended.2
Adverse effect profiles vary among selective and non-selective alpha blockers (Table 3).2,3,15,19,20,23,24 The AUA recommends avoidance of all alpha blockers in men with planned cataract surgery because of the risk of intraoperative floppy iris syndrome.2,20 It is unclear if the dose, duration of therapy, or stopping the alpha blocker lowers this risk.
Table 3. Medical Therapies for Benign Prostatic Hyperplasia
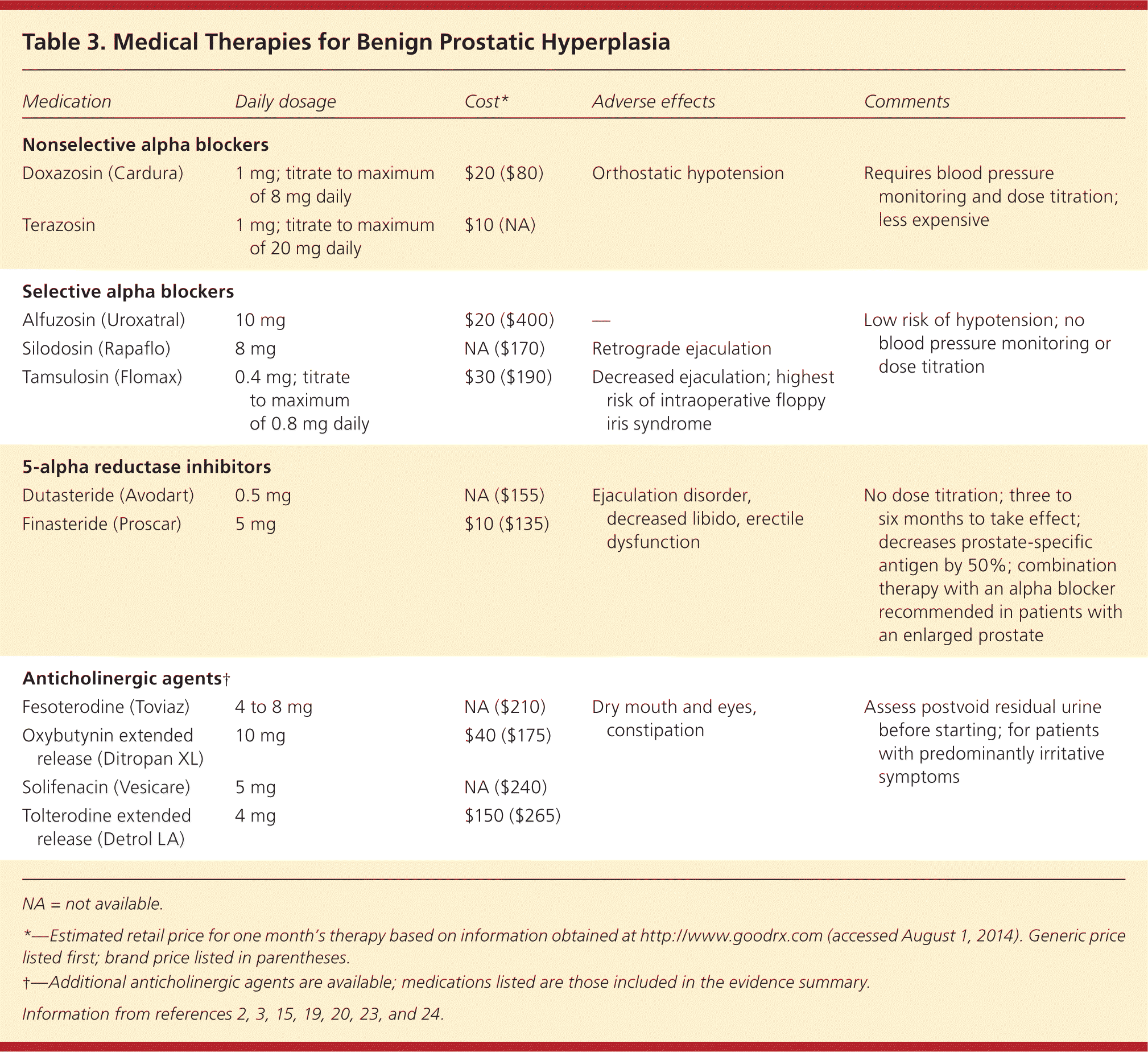
| Medication | Daily dosage | Cost* | Adverse effects | Comments |
|---|---|---|---|---|
| Nonselective alpha blockers | ||||
| Doxazosin (Cardura) | 1 mg; titrate to maximum of 8 mg daily | $20 ($80) | Orthostatic hypotension | Requires blood pressure monitoring and dose titration; less expensive |
| Terazosin | 1 mg; titrate to maximum of 20 mg daily | $10 (NA) | ||
| Selective alpha blockers | ||||
| Alfuzosin (Uroxatral) | 10 mg | $20 ($400) | — | Low risk of hypotension; no blood pressure monitoring or dose titration |
| Silodosin (Rapaflo) | 8 mg | NA ($170) | Retrograde ejaculation | |
| Tamsulosin (Flomax) | 0.4 mg; titrate to maximum of 0.8 mg daily | $30 ($190) | Decreased ejaculation; highest risk of intraoperative floppy iris syndrome | |
| 5-alpha reductase inhibitors | ||||
| Dutasteride (Avodart) | 0.5 mg | NA ($155) | Ejaculation disorder, decreased libido, erectile dysfunction | No dose titration; three to six months to take effect; decreases prostate-specific antigen by 50%; combination therapy with an alpha blocker recommended in patients with an enlarged prostate |
| Finasteride (Proscar) | 5 mg | $10 ($135) | ||
| Anticholinergic agents† | ||||
| Fesoterodine (Toviaz) | 4 to 8 mg | NA ($210) | Dry mouth and eyes, constipation | Assess postvoid residual urine before starting; for patients with predominantly irritative symptoms |
| Oxybutynin extended release (Ditropan XL) | 10 mg | $40 ($175) | ||
| Solifenacin (Vesicare) | 5 mg | NA ($240) | ||
| Tolterodine extended release (Detrol LA) | 4 mg | $150 ($265) | ||
NA = not available.
*—Estimated retail price for one month's therapy based on information obtained at http://www.goodrx.com (accessed August 1, 2014). Generic price listed first; brand price listed in parentheses.
†—Additional anticholinergic agents are available; medications listed are those included in the evidence summary.
5-Alpha Reductase Inhibitors. Dutasteride (Avodart) and finasteride (Proscar) block the conversion of testosterone to dihydrotestosterone, resulting in a gradual decrease in prostatic volume. The AUA recommends combination therapy with a 5-alpha reductase inhibitor and alpha blocker when alpha-blocker monotherapy is not effective and the patient has an enlarged prostate based on digital rectal examination findings, volume measurement, or serum PSA level as proxy for volume measurement (1.5 ng per mL [1.5 mcg per L] or more).2 Dutasteride and finasteride are equally effective and decrease the risk of BPH progression (urinary retention or prostate surgery).2,9,23,25–27 The use of 5-alpha reductase inhibitors decreases prostate size and decreases serum PSA levels by 50%, although it takes at least three to six months.2,23,25,28 These changes must be considered when assessing for prostate cancer.
Anticholinergic Agents. Anticholinergic agents block the effects of acetylcholine on muscarinic receptors in the bladder, resulting in decreased bladder contractions. Anticholinergic agents, such as tolterodine (Detrol), can benefit selected patients with predominantly irritative lower urinary tract symptoms (frequency, urgency) and a normal postvoid residual urine measurement.2 There is an increased risk of urinary retention with a post-void residual urine measurement greater than 250 mL.2 A meta-analysis of seven randomized controlled trials (RCTs; n = 3,629) comparing combination anticholinergic and alpha-blocker therapy with alpha-blocker mono-therapy demonstrated greater reduction of I-PSS scores in the combination group. There was one additional episode of acute urinary retention for every 101 men treated in the combination group.24
Which Patients Should Be Referred for Surgery?
Patients with BPH and bothersome, moderate to severe lower urinary tract symptoms should be referred for surgical consultation if BPH-related complications develop, medical therapy fails, or the patient chooses it.
EVIDENCE SUMMARY
The AUA recommends surgery if medical therapy fails or the patient develops BPH-related complications, such as bladder calculi, bladder decompensation (decreased detrusor contractions), hematuria (gross and microscopic), recurrent urinary tract infections, renal insufficiency, and urinary retention.2,14 Patients should be informed that surgery is an option for initial treatment; however, the benefits and risks compared with no treatment and medical therapy should also be reviewed.
Transurethral resection of the prostate (TURP) is the standard against which other surgical procedures are compared. Because of cost, morbidity, and the need for hospitalization, less invasive procedures have been developed. There are limited high-quality studies comparing these interventions. eTable A summarizes the surgical options. A TURP procedure is recommended for healthy men with low surgical risk who require surgery, whereas men who cannot tolerate general anesthesia should consider non-TURP surgical intervention.2
eTable A. Surgical Therapies for the Treatment of Benign Prostatic Hyperplasia
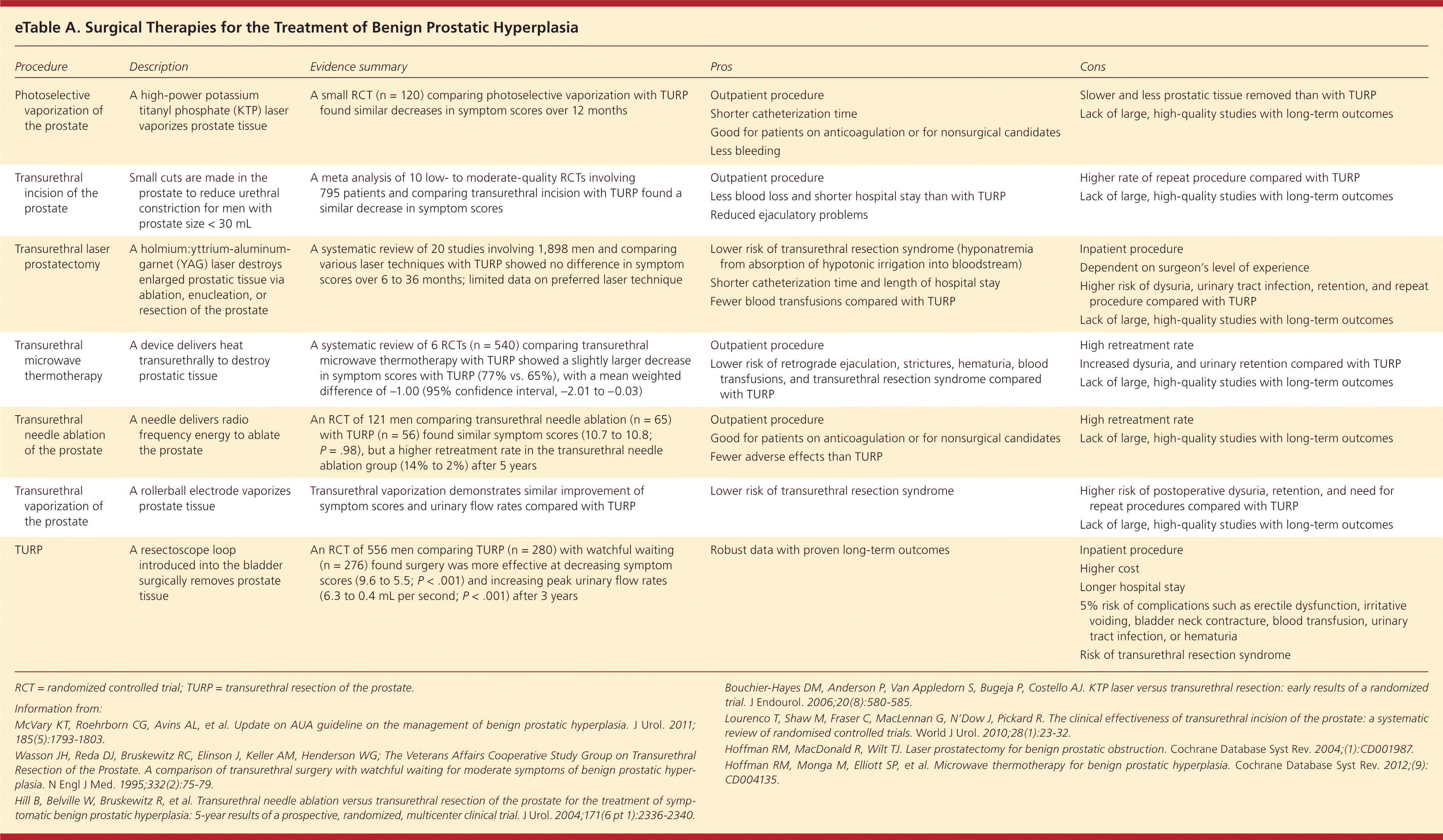
| Procedure | Description | Evidence summary | Pros | Cons |
|---|---|---|---|---|
| Photoselective vaporization of the prostate | A high-power potassium titanyl phosphate (KTP) laser vaporizes prostate tissue | A small RCT (n = 120) comparing photoselective vaporization with TURP found similar decreases in symptom scores over 12 months |
|
|
| Transurethral incision of the prostate | Small cuts are made in the prostate to reduce urethral constriction for men with prostate size < 30 mL | A meta analysis of 10 low- to moderate-quality RCTs involving 795 patients and comparing transurethral incision with TURP found a similar decrease in symptom scores |
|
|
| Transurethral laser prostatectomy | A holmium:yttrium-aluminum-garnet (YAG) laser destroys enlarged prostatic tissue via ablation, enucleation, or resection of the prostate | A systematic review of 20 studies involving 1,898 men and comparing various laser techniques with TURP showed no difference in symptom scores over 6 to 36 months; limited data on preferred laser technique |
|
|
| Transurethral microwave thermotherapy | A device delivers heat transurethrally to destroy prostatic tissue | A systematic review of 6 RCTs (n = 540) comparing transurethral microwave thermotherapy with TURP showed a slightly larger decrease in symptom scores with TURP (77% vs. 65%), with a mean weighted difference of −1.00 (95% confidence interval, −2.01 to −0.03) |
|
|
| Transurethral needle ablation of the prostate | A needle delivers radio frequency energy to ablate the prostate | An RCT of 121 men comparing transurethral needle ablation (n = 65) with TURP (n = 56) found similar symptom scores (10.7 to 10.8; P = .98), but a higher retreatment rate in the transurethral needle ablation group (14% to 2%) after 5 years |
|
|
| Transurethral vaporization of the prostate | A rollerball electrode vaporizes prostate tissue | Transurethral vaporization demonstrates similar improvement of symptom scores and urinary flow rates compared with TURP |
|
|
| TURP | A resectoscope loop introduced into the bladder surgically removes prostate tissue | An RCT of 556 men comparing TURP (n = 280) with watchful waiting (n = 276) found surgery was more effective at decreasing symptom scores (9.6 to 5.5; P < .001) and increasing peak urinary flow rates (6.3 to 0.4 mL per second; P < .001) after 3 years |
|
|
RCT = randomized controlled trial; TURP = transurethral resection of the prostate.
Information from: McVary KT, Roehrborn CG, Avins AL, et al. Update on AUA guideline on the management of benign prostatic hyperplasia. J Urol . 2011; 185(5):1793–1803.
Wasson JH, Reda DJ, Bruskewitz RC, Elinson J, Keller AM, Henderson WG; The Veterans Affairs Cooperative Study Group on Transurethral Resection of the Prostate. A comparison of transurethral surgery with watchful waiting for moderate symptoms of benign prostatic hyperplasia. N Engl J Med . 1995;332(2):75–79.
Hill B, Belville W, Bruskewitz R, et al. Transurethral needle ablation versus transurethral resection of the prostate for the treatment of symptomatic benign prostatic hyperplasia: 5-year results of a prospective, randomized, multicenter clinical trial. J Urol . 2004;171(6 pt 1):2336–2340.
Bouchier-Hayes DM, Anderson P, Van Appledorn S, Bugeja P, Costello AJ. KTP laser versus transurethral resection: early results of a randomized trial.J Endourol . 2006;20(8):580–585.
Lourenco T, Shaw M, Fraser C, MacLennan G, N'Dow J, Pickard R. The clinical effectiveness of transurethral incision of the prostate: a systematic review of randomised controlled trials. World J Urol . 2010;28(1):23–32.
Hoffman RM, MacDonald R, Wilt TJ. Laser prostatectomy for benign prostatic obstruction. Cochrane Database Syst Rev . 2004;(1):CD001987.
Hoffman RM, Monga M, Elliott SP, et al. Microwave thermotherapy for benign prostatic hyperplasia. Cochrane Database Syst Rev . 2012;(9): CD004135.
Is There a Role for Complementary and Alternative Therapies in BPH Management?
Dietary supplements (i.e., saw palmetto, pygeum, cernilton, or beta sitosterols) and acupuncture are not recommended for the treatment of BPH.
EVIDENCE SUMMARY
A 2012 systematic review of 32 RCTs involving 5,666 men treated for four to 72 weeks demonstrated that saw palmetto did not reduce nocturia, peak urine flow, prostate size, or AUA-SI scores compared with placebo in men with BPH.29
Systematic reviews of pygeum, cernilton, and herbs containing beta sitosterols found that trials were limited by short duration, small sample size, and varied doses and preparations. There is no current evidence to support their use.2,30–32
A small single-blinded RCT of acupuncture for BPH found no difference in I-PSS scores after three months among the following treatment groups: observation, acupuncture of the kidney-bladder distinct meridian, or sham acupuncture.33
Data Sources: We searched Ovid Medline and Essential Evidence Plus using the key term prostatic hyperplasia. The search included meta-analyses, systematic reviews, core clinical journals, and evidence-based medicine topic reviews. Search dates: December 2013, January and October 2014.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force, the Department of Defense, or Kaiser Permanente.

