Down syndrome is the most common chromosomal abnormality, occurring in one in 691 live births in the United States each year. Prenatally, the sequential contingent test for aneuploidy screening is highly sensitive for Down syndrome and has a low false-positive rate. The diagnosis should be confirmed with fluorescent in situ hybridization followed by chromosomal karyotyping at birth. Children with Down syndrome have varied degrees of intellectual disability and more health complications than other children. However, advancements in recent decades have led to improved life expectancy, satisfaction, and quality of life. Newborns with Down syndrome require echocardiography and cardiology evaluation. Children should have annual screenings for vision and hearing, and laboratory studies for subclinical thyroid disease and blood disorders. Clinicians should provide unbiased and comprehensive culturally sensitive information regarding available services for children with Down syndrome. There is good evidence that comprehensive early intervention programs (e.g., speech, visual, physical, and occupational therapy; child psychology) enhance development. It is important to enroll children with Down syndrome in state-specific resources as early as possible. Given the advances in medical care and early intervention programs, regular health supervision by family physicians can allow children with Down syndrome to lead healthy and productive lives.
Down syndrome is the most common chromosomal abnormality. Almost 10,000 children are born with Down syndrome in the United States each year (one in 691 live births; prevalence of 10.3 per 10,000).1–4 Birth rates are highest among mothers of advanced maternal age (one in 400 at 35 years of age, one in 105 at 40 years of age, one in 12 at 45 years of age); however, 80% of all children with Down syndrome are born to mothers younger than 35 years.4 The underlying karyotype is 95% nonfamilial trisomy 21 (47 total chromosomes), 3% to 4% unbalanced translocation, and 1% to 2% genetic mosaicism (Table 1).3,5 The five-year survival rate is greater than 90%,6 and current life expectancy exceeds 60 years.3,7,8 Most children can participate fully in integrated public school education programs and community activities.
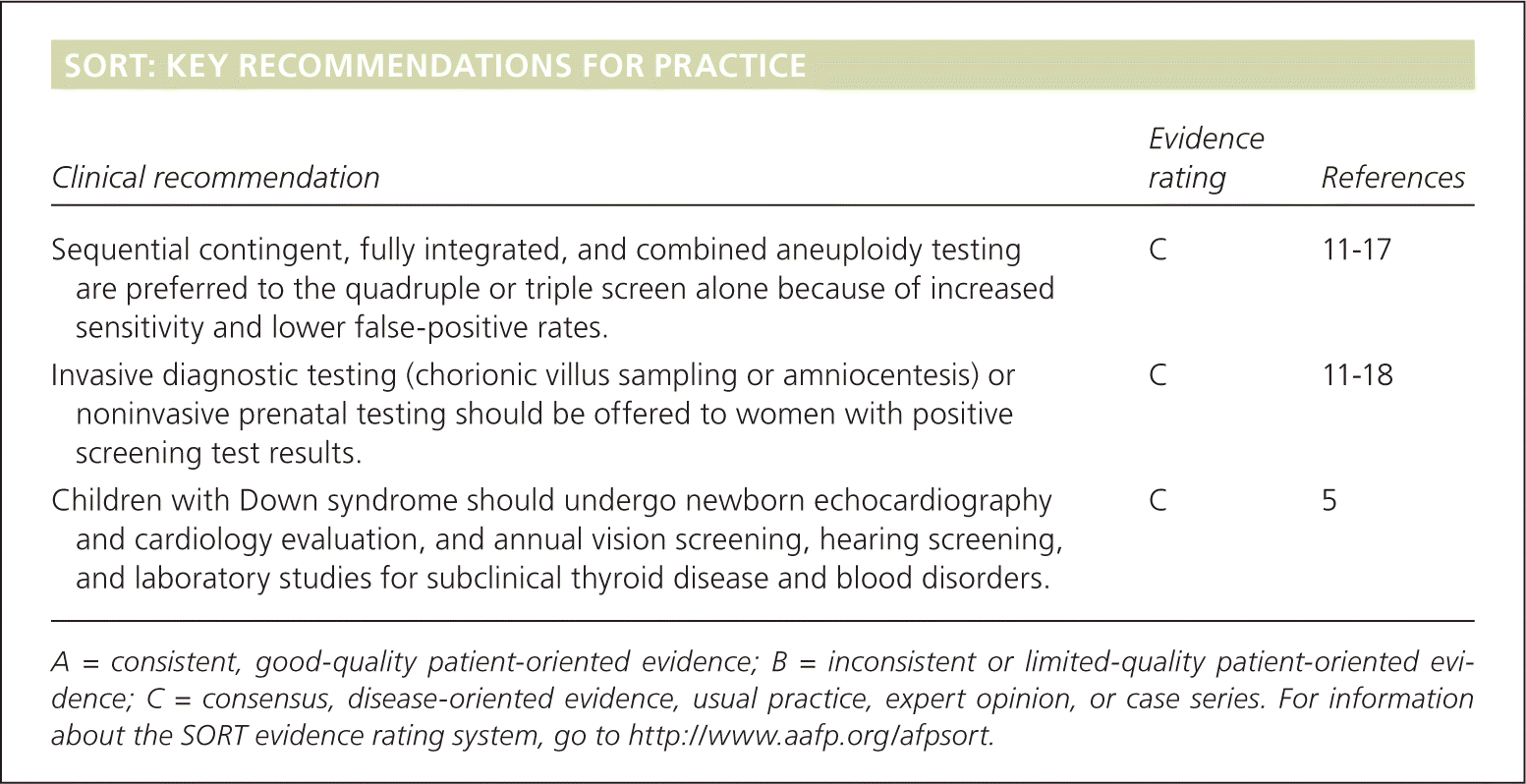
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Sequential contingent, fully integrated, and combined aneuploidy testing are preferred to the quadruple or triple screen alone because of increased sensitivity and lower false-positive rates. | C | 11–17 |
| Invasive diagnostic testing (chorionic villus sampling or amniocentesis) or noninvasive prenatal testing should be offered to women with positive screening test results. | C | 11–18 |
| Children with Down syndrome should undergo newborn echocardiography and cardiology evaluation, and annual vision screening, hearing screening, and laboratory studies for subclinical thyroid disease and blood disorders. | C | 5 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN GENETICS – RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not offer noninvasive prenatal testing to low-risk patients or make irreversible decisions based on the results of this screening test. | Society for Maternal-Fetal Medicine |
source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Table 1. Glossary of Genetic and Prenatal Screening Terminology

| Term | Definition |
|---|---|
| Balanced translocation | Rearrangement of genetic material equally between chromosomes |
| Cell-free fetal DNA | Fetal DNA freely circulating in maternal blood; measured as part of aneuploidy screening for high-risk women |
| Combined test | First trimester measurement of hormones (beta subunit of human chorionic gonadotropin and pregnancy-associated plasma protein A) plus nuchal translucency |
| Fully integrated test | Combined test in first trimester plus quadruple screen in second trimester; screening report produced after both complete |
| Genetic mosaicism | Presence of more than one population of cells with different genotypes in a single individual |
| Nuchal translucency | Fluid-filled nuchal space (posterior neck) best visualized on ultrasonography between 11 and 14 weeks of gestation |
| Sequential contingent test | After initial screening report in first trimester, women at high risk are offered invasive diagnostic testing; women at moderate risk are offered further second trimester testing; and women at low risk have no further testing |
| Unbalanced translocation | Inheritance of a chromosome with extra or missing genetic material from a parent with a balanced translocation |
Intellectual disability and developmental delays vary widely in children with Down syndrome. Significant gains have occurred in recent decades in satisfaction and quality of life for children and adults with Down syndrome. However, relative to other children, additional health complications increase the risk of hospitalization and can create a significant emotional and financial impact on families.9,10 Family physicians can play an integral role in parental support, diagnosis, initial management, treatment of common medical problems, and health maintenance for children with Down syndrome.
Prenatal Testing
Aneuploidy screening and both noninvasive and invasive diagnostic testing should be discussed at the first prenatal visit.11 Prenatal testing options include laboratory testing, imaging (nuchal translucency or ultrasonography), invasive diagnostic testing (chorionic villus sampling or amniocentesis), and noninvasive prenatal testing using cell-free fetal DNA.12
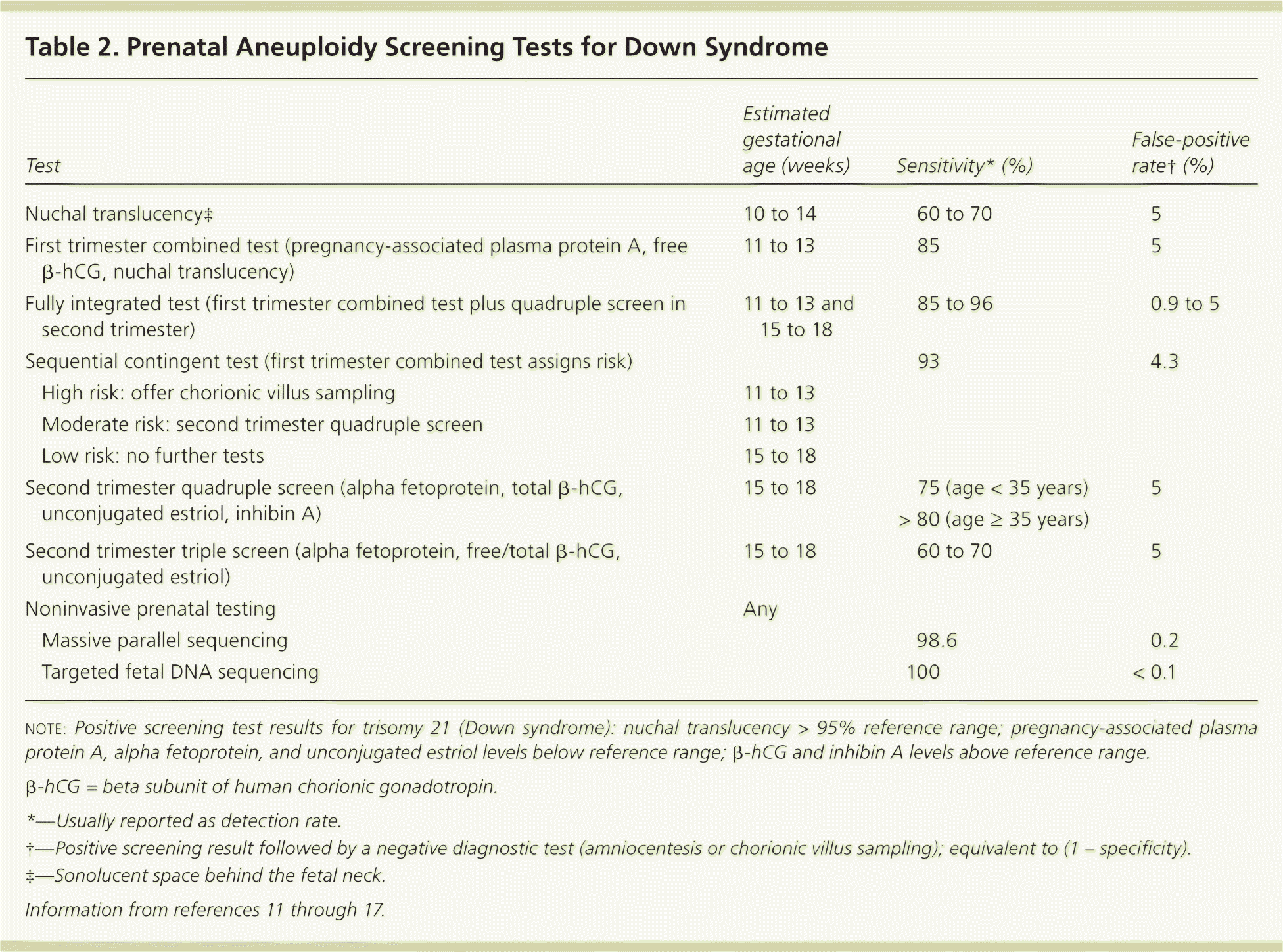
Prenatal screening is time sensitive and should be offered within the recommended prenatal window.11 The most sensitive options are sequential contingent, fully integrated, and first trimester combined aneuploidy testing (Table 2).11–17 These tests are preferred to quadruple or triple screening tests alone.11–17
Table 2. Prenatal Aneuploidy Screening Tests for Down Syndrome
| Test | Estimated gestational age (weeks) | Sensitivity* (%) | False-positive rate†(%) | |
|---|---|---|---|---|
| Nuchal translucency‡ | 10 to 14 | 60 to 70 | 5 | |
| First trimester combined test (pregnancy-associated plasma protein A, free β-hCG, nuchal translucency) | 11 to 13 | 85 | 5 | |
| Fully integrated test (first trimester combined test plus quadruple screen in second trimester) | 11 to 13 and 15 to 18 | 85 to 96 | 0.9 to 5 | |
| Sequential contingent test (first trimester combined test assigns risk) | 93 | 4.3 | ||
| High risk: offer chorionic villus sampling | 11 to 13 | |||
| Moderate risk: second trimester quadruple screen | 11 to 13 | |||
| Low risk: no further tests | 15 to 18 | |||
| Second trimester quadruple screen (alpha fetoprotein, total β-hCG, unconjugated estriol, inhibin A) | 15 to 18 | 75 (age < 35 years) > 80 (age ≥ 35 years) | 5 | |
| Second trimester triple screen (alpha fetoprotein, free/total β-hCG, unconjugated estriol) | 15 to 18 | 60 to 70 | 5 | |
| Noninvasive prenatal testing | Any | |||
| Massive parallel sequencing | 98.6 | 0.2 | ||
| Targeted fetal DNA sequencing | 100 | < 0.1 | ||
note: Positive screening test results for trisomy 21 (Down syndrome): nuchal translucency > 95% reference range; pregnancy-associated plasma protein A, alpha fetoprotein, and unconjugated estriol levels below reference range; β-hCG and inhibin A levels above reference range.
β-hCG = beta subunit of human chorionic gonadotropin.
*—Usually reported as detection rate.
†—Positive screening result followed by a negative diagnostic test (amniocentesis or chorionic villus sampling); equivalent to (1 – specificity).
‡—Sonolucent space behind the fetal neck.
Initial positive screening test results can be followed with invasive diagnostic testing or noninvasive prenatal testing.11–18 The American College of Obstetricians and Gynecologists' Committee on Genetics states that noninvasive prenatal testing or invasive diagnostic testing alone can also be offered to women at increased risk (e.g., age older than 35 years, positive screening test, ultrasonographic findings suggesting aneuploidy, previous child with or family history of chromosomal abnormality).16,18 Noninvasive prenatal testing has a reported sensitivity and specificity of 99% to 100%, and unlike invasive diagnostic testing, it does not increase the risk of spontaneous abortion.12,16,17 Women with an abnormal screening test result, women at higher risk, and women who are considering invasive diagnostic testing should be referred to a genetic counselor or maternal-fetal medicine specialist.16,19 Parental decisions to decline screening tests after being fully informed of the options, including risks and benefits, should be respected.
Initial Management
Any prenatal diagnosis or phenotypic features suggesting Down syndrome (Table 33,5 ) should be confirmed in the newborn using fluorescent in situ hybridization followed by a complete genetic karyotype analysis. The specific karyotype can help guide future pregnancy planning.3,5
Table 3. Common Physical Characteristics in Newborns with Down Syndrome

| Head/neck |
| Arched palate |
| Brachycephaly (flattened head, usually posterior aspect) |
| Brushfield spots (hypopigmented iris spots) |
| Ear abnormalities (low-set/folded) |
| Epicanthal folds |
| Excessive skin on nape of neck |
| Flat facial profile |
| Macroglossia |
| Short neck and microcephaly |
| Small nose |
| Upward slant to the eyes |
| Hands |
| Clinodactyly (curved fifth finger) |
| Short, broad hands |
| Short fifth finger |
| Single palmar crease |
| Feet |
| Widened gap between first and second toes (sandal gap) |
| Global |
| Hyperflexibility |
| Muscular hypotonia |
All newborns with Down syndrome should undergo screening for cardiac, feeding, vision, hearing, thyroid, and hematologic abnormalities as soon as possible.3,5 Because up to 50% of newborns with Down syndrome have a congenital cardiac defect that is often undetectable on prenatal ultrasonography,3,5,20 an echocardiogram, reviewed by a pediatric cardiologist, is essential. Marked hypotonia or other feeding difficulties should prompt a radiographic swallowing assessment.5 Red reflex testing should be performed to check for congenital cataracts.5 A standard objective hearing screening using brainstem auditory evoked response or otoacoustic emission is recommended.3,5 Screening for subclinical thyroid disease using thyroid-stimulating hormone (TSH) and free thyroxine levels should be performed.1,3,5 A complete blood count (CBC) should be performed because of the increased risk of transient myeloproliferative disorder, leukemoid reaction, and polycythemia.3,5,21–23
Parents who are not anticipating a child with Down syndrome most likely will have heightened concerns and emotional turmoil as the diagnosis is confirmed. It is important to congratulate the new parents on the birth of their child, explain the rationale for each recommended test, and clarify what the specific results mean. Allowing parents time to process information and develop questions is important. Clinicians should provide parents with unbiased, comprehensive, and culturally sensitive information about Down syndrome and available services.5,24 To facilitate this discussion, the National Down Syndrome Society website (http://www.ndss.org) provides information on preferred language, emphasizing that a child with Down syndrome is a child first, and explains that the word retarded is derogatory and outdated.25
Common Medical Problems
Children with Down syndrome are generally shorter and heavier than their peers.5 Standard World Health Organization growth charts should be used for monitoring, because the original Down syndrome–specific growth charts are not reflective of the current population.26,27
IQ remains the main descriptor for intellectual disability in Down syndrome. It is quantified as mild (IQ of 50 to 69), moderate (IQ of 35 to 49), and occasionally severe (IQ of 20 to 34).5,28 All areas of developmental progress should be documented and evaluated relative to the child's peers but, more importantly, relative to the child's own progress, because milestone achievement varies in all children. Any regression requires further evaluation.5
Additional medical problems that can present in children with Down syndrome are listed in Table 4.5,20–23,29–42
Table 4. Common Medical Problems in Persons with Down Syndrome

| Condition | % | |
|---|---|---|
| Obstructive sleep apnea5 | 50 to 79 | |
| Hearing loss29 | 75 | |
| Otitis media30 | 50 to 70 | |
| Vision and eye disease/cataracts31–35 | 60/15 | |
| Congenital heart defects20,36 | 50 | |
| Hypodontia and delayed dental eruption37 | 23 | |
| Thyroid disease1,38 | 4 to 18 | |
| Neurologic dysfunction/seizures5 | 1 to 13 | |
| Gastrointestinal atresias36 | 12 | |
| Autism39,40 | 7 | |
| Hip dislocation5 | 6 | |
| Celiac disease41 | 5 | |
| Hematologic problems21–23 | ||
| Polycythemia | 18 to 64 | |
| Iron deficiency anemia | 10 | |
| Transient myeloproliferative disorder | 10 | |
| Leukemia | 1 | |
| Atlantoaxial instability5 | 1 to 2 | |
| Hirschsprung disease42 | < 1 | |
Information from references 5, 20 through 23, and 29 through 42.
Health Maintenance
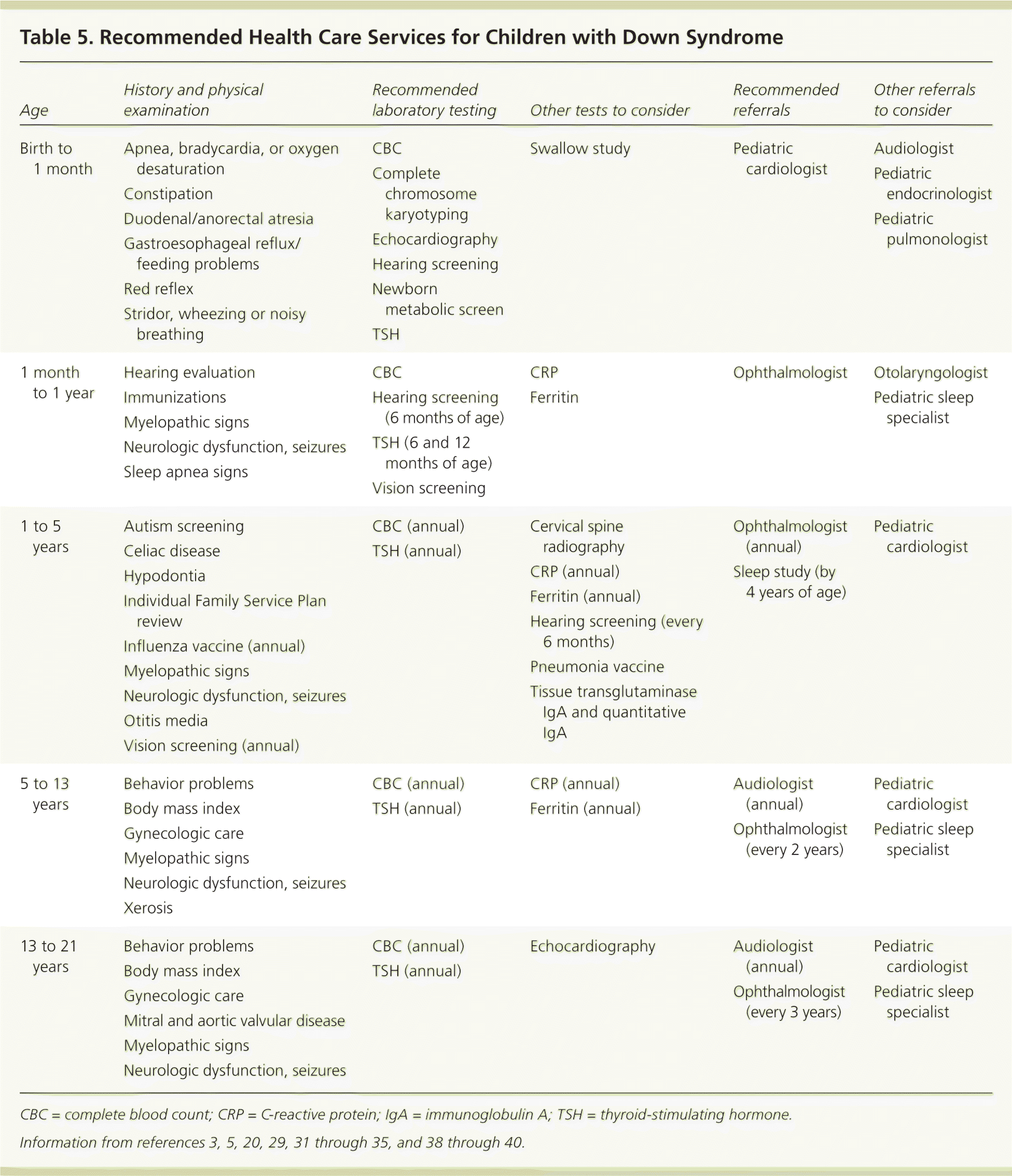
The 2011 American Academy of Pediatrics' report “Health Supervision for Children With Down Syndrome” is a comprehensive guide to preventive screening and health maintenance5 (Table 53,5,20,29,31–35,38–40 ).
BIRTH TO ONE MONTH
In addition to the physical examination, laboratory tests, and imaging studies, clinicians should evaluate for oxygen desaturation in a car safety seat, constipation, gastroesophageal reflux, and breathing difficulties. Anticipatory guidance during this time period focuses on an increased susceptibility to respiratory infections and emphasizes the importance of feeding and nutrition.5
It is important to identify and enroll newborns in state-specific early intervention programs as soon as possible to improve short- and long-term outcomes.5,43–46 Typical components of a comprehensive program include physical and occupational therapy, speech and vision therapy, and child psychology. Goals of early intervention programs include establishing care in a patient-centered medical home, reviewing eligibility for parental financial and psychological support programs, and creating an Individual Family Service Plan.5 This plan should be reviewed at least every six months, because it guides all components until the child is three years of age and reflects the child's needs.5,43
ONE MONTH TO ONE YEAR
Growth and global development should be monitored carefully in the first year of life, because failure-to-thrive may suggest underlying feeding or medical problems.5 By six months of age, infants should have a repeat hearing screening and a comprehensive evaluation by a pediatric ophthalmologist.3,5,31–34 A TSH level measurement should be repeated at six and 12 months of age and then annually thereafter regardless of the initial free thyroxine and TSH results.1,5,38 Symptoms of obstructive sleep apnea require referral to a pediatric sleep specialist.5
Anticipatory guidance should focus on ensuring the infant is healthy and thriving, evaluating and establishing emotional family support, providing clear explanation and guidance for health issues, and periodically reviewing the Individual Family Service Plan progress.43 Discussions with parents should include guardianship decisions and long-term financial plans (e.g., special needs trusts).5
Table 5. Recommended Health Care Services for Children with Down Syndrome
| Age | History and physical examination | Recommended laboratory testing | Other tests to consider | Recommended referrals | Other referrals to consider |
|---|---|---|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
CBC = complete blood count; CRP = C-reactive protein; IgA = immunoglobulin A; TSH = thyroid-stimulating hormone.
Information from references 3, 5, 20, 29, 31through35, and 38 through 40.
ONE TO FIVE YEARS
Hearing screening should be performed every six months until approximately four years of age, with otolaryngology referral if results are abnormal.29 Annual visits with a pediatric ophthalmologist are recommended, because there is a 50% chance of refractive errors leading to amblyopia by five years of age.31–35 Because of the potential for atlantoaxial instability, parents should be counseled about signs and symptoms of spinal cord impingement (e.g., gait disturbance, change in bowel or bladder function, weakness). Although screening is not necessary in asymptomatic children, cervical spine radiography in the neutral position is the image of choice in symptomatic children older than three years. Referral to pediatric neurosurgery is needed if abnormalities are noted.5
All children with Down syndrome should undergo polysomnography to be evaluated for obstructive sleep apnea by four years of age. Because of the increased prevalence of celiac disease, a review of dietary symptoms should be completed at each visit, and laboratory testing with immunoglobulin A tissue transglutaminase and quantitative immunoglobulin A should be considered when symptoms suggest celiac disease.5
Anticipatory guidance should focus on the transition around three years of age from an early intervention program Individual Family Service Plan to a school-focused Individualized Education Program.5 Screening for autism spectrum disorder with validated tools should be performed between 18 and 24 months of age because of the increased prevalence in children with Down syndrome.39,40 However, screening may not be able to be accomplished effectively during this period in a child with Down syndrome, and may need to be postponed until three to five years of age if developmental delays are present.
FIVE TO 13 YEARS
Visits during childhood should focus on healthy diet and growth, with attention to chronic conditions. Hearing screening, TSH level measurement, and CBC should be continued annually.5,29 Ophthalmology visits can occur every other year.5,31–34 Significant xerosis may be an early sign of hypothyroidism.5
Anticipatory guidance should focus on family support, the child's Individualized Education Program, and socialization. Clinicians should be alert for signs of cervical spine injury, obesity, and behavior problems, such as attention-deficit/hyperactivity disorder.5,39
13 TO 21 YEARS
TSH level measurement, CBC, and audiology evaluation should be performed annually, and ophthalmology examination should be performed every three years during adolescence.31–34 Patients with Down syndrome are at risk of acquired mitral or aortic valvular disease, and echocardiography should be performed for any concerning symptoms.5,20
Discussions with parents should include financial planning, transition to more independent living, vocational training, and community employment options. Female adolescents with Down syndrome should have appropriate gynecologic care, and sexuality should be discussed with all adolescents.5
Parental Resources
To provide effective care for children with Down syndrome, family physicians should be aware of resources available for parents (see accompanying patient handout). These include clinics specializing in Down syndrome care, local chapters affiliated with the National Down Syndrome Society, and local support groups. With advances in medical care and early intervention programs, regular health supervision by family physicians can allow children with Down syndrome to lead healthy and productive lives.
Data Sources: A PubMed search was completed in Clinical Queries using the key term Down syndrome. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cumulative Index to Nursing and Allied Health Literature, the Agency for Healthcare Research and Quality evidence reports, Essential Evidence Plus, the Cochrane Database of Systematic Reviews, and the National Guideline Clearinghouse. Search dates: June 24, 2013; August 22, 2013; and September 12, 2014.
In loving memory of our daughter, Sophie Analie (3/7/11–2/21/12): a beautiful gift, tied with an extra chromosome.
The authors thank Alison Rollins for assistance with the literature search, and Mark Stephens, MD, and Meredith Towbin, MA, for editorial assistance.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force Medical Service or the U.S. Air Force at large.

