Nausea and vomiting are mediated primarily by three neurotransmitter pathways: visceral stimulation releases dopamine and serotonin; vestibular and central nervous system activation release histamine and acetylcholine; and chemoreceptor trigger zone activation releases dopamine and serotonin. Clinicians can improve the effectiveness and cost-effectiveness of treatments by targeting the appropriate pathways. Antihistamines and anticholinergics are most effective in patients with vestibular-mediated nausea secondary to vertigo. Serotonin antagonists block serotonin in the intestines and chemoreceptor trigger zone, and are most effective for treating gastroenteritis. Dopamine antagonists block dopamine in the intestines and chemoreceptor trigger zone; indications for these agents are similar to those for serotonin antagonists. For treatment of mild pregnancy-induced nausea, pyridoxine with or without doxylamine is recommended, and ginger may also be effective. In patients with migraine headache–associated nausea, metoclopramide improves response to oral anti-migraine agents. Ondansetron reduces nausea and vomiting in children with acute gastroenteritis and in women with hyperemesis gravidarum.
Nausea and vomiting are common complications of multiple conditions, procedures, and therapies, and adversely affect quality of life in millions of patients each year. Pregnancy-induced nausea alone accounts for an estimated 8.5 million lost working days and costs nearly $2 billion annually.1 Acute gastroenteritis causes 1.5 million visits to primary care clinicians annually and accounts for 10% of all hospital admissions in the United States.2 The causes and evaluation of nausea and vomiting have been reviewed in American Family Physician,3 and treatment is ideally directed at the underlying cause. By understanding the neurotransmitters involved in different types of nausea, clinicians can improve the effectiveness and cost-effectiveness of symptomatic treatments (Table 1).
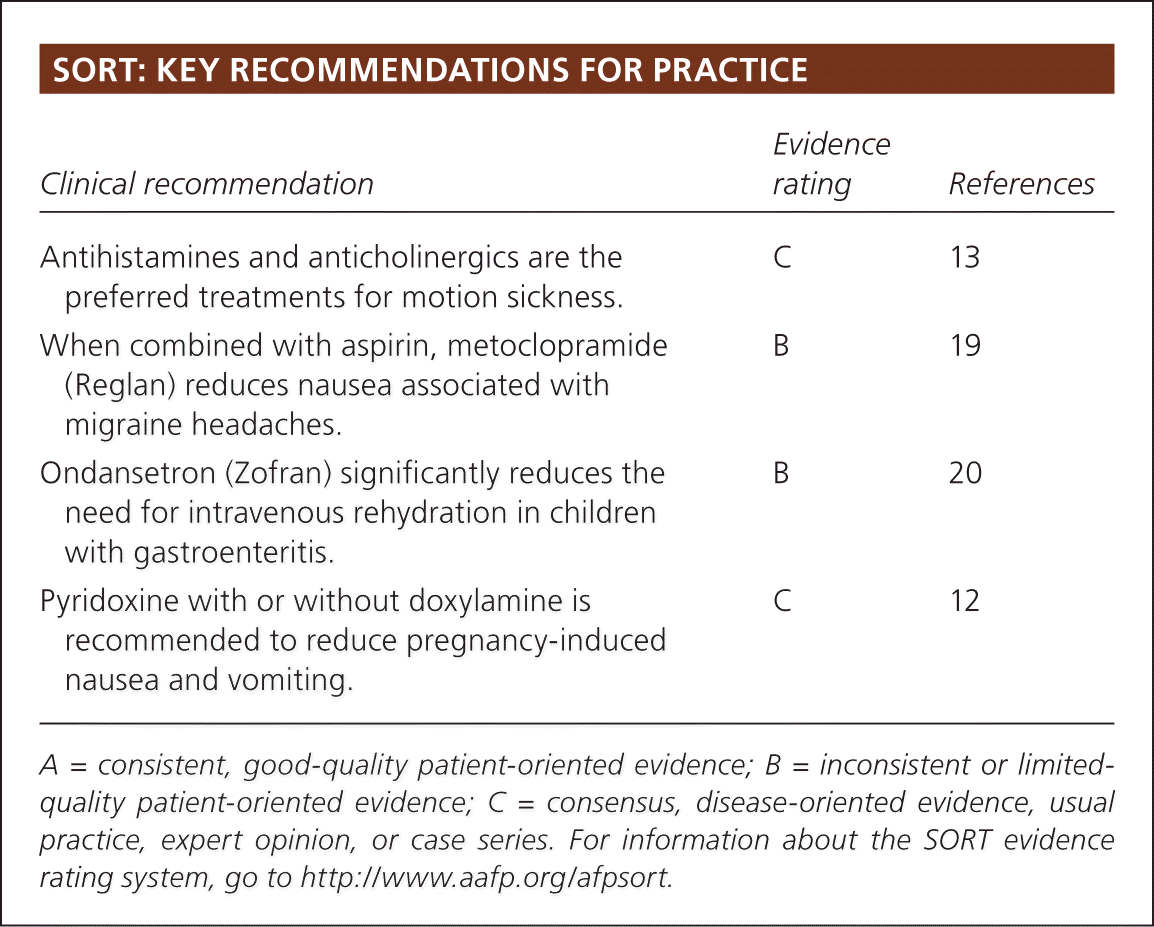
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Antihistamines and anticholinergics are the preferred treatments for motion sickness. | C | 13 |
| When combined with aspirin, metoclopramide (Reglan) reduces nausea associated with migraine headaches. | B | 19 |
| Ondansetron (Zofran) significantly reduces the need for intravenous rehydration in children with gastroenteritis. | B | 20 |
| Pyridoxine with or without doxylamine is recommended to reduce pregnancy-induced nausea and vomiting. | C | 12 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN GASTROENTEROLOGY – RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not use topical lorazepam (Ativan), diphenhydramine (Benadryl), or haloperidol (Haldol) (“ABH”) gel for nausea. | American Academy of Hospice and Palliative Medicine |
source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Table 1. Selection of Antiemetics by Clinical Situation

| Clinical situation | Associated neurotransmitters | Recommended antiemetic |
|---|---|---|
| Vestibular nausea/motion sickness | Histamine, acetylcholine | Meclizine (Antivert), scopolamine |
| Migraine-associated nausea | Dopamine | Metoclopramide (Reglan), prochlorperazine, promethazine |
| Gastroenteritis | Dopamine, serotonin | Promethazine, serotonin antagonists |
| Pregnancy-induced nausea | Unknown | Mild: ginger, pyridoxine with or without doxylamine |
| Hyperemesis: corticosteroids,* ondansetron (Zofran) |
*—Avoid use before 10 weeks' gestation because of the increased risk of oral clefts.
Three primary pathophysiologic pathways stimulate the physiologic vomiting center in the medulla that mediates nausea and vomiting (Figure 1). This center can be stimulated by vestibular fibers, afferent visceral fibers, and input from the chemoreceptor trigger zone in the base of the fourth ventricle. The neurotransmitters histamine, acetylcholine, serotonin, and dopamine are often implicated in these pathways and are the targets of most therapies.
Figure 1. Treatment of Nausea and Vomiting
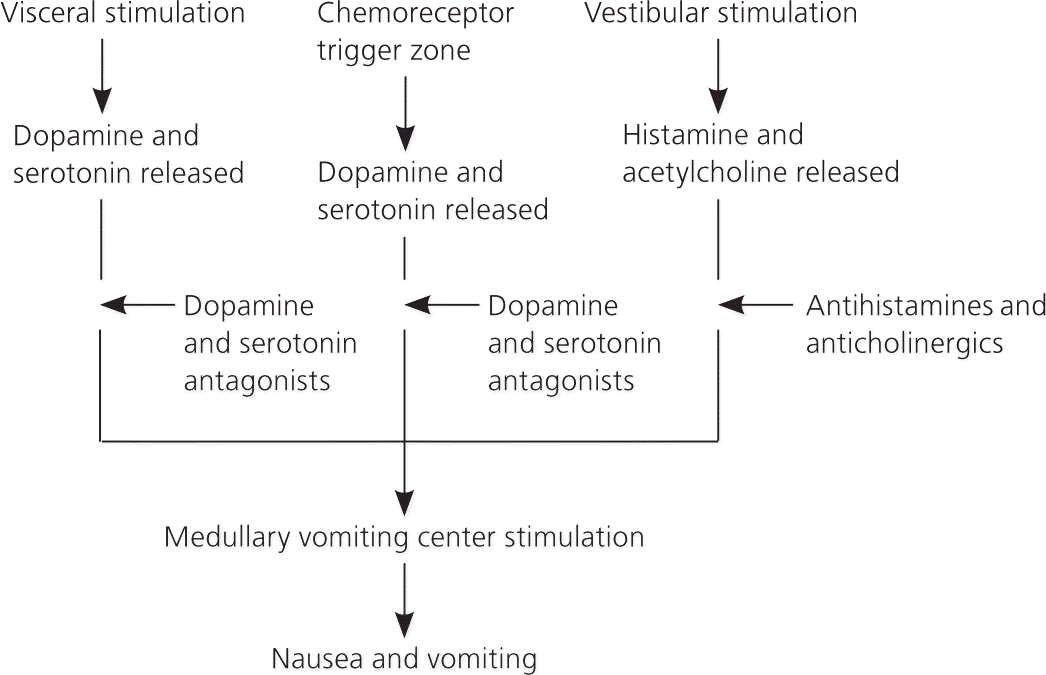
Neurotransmitters involved in nausea and vomiting, and the medications used to mitigate their effects.
Medication Classes
ANTIHISTAMINES AND ANTICHOLINERGICS
Antihistamines and anticholinergics limit stimulation of the vomiting center through inhibition of the histamine H1 receptor and acetylcholine, respectively. Antihistamines such as meclizine (Antivert) and scopolamine are particularly beneficial in vestibular-mediated nausea. Common adverse effects for both classes include sedation, constipation, dry mouth, and urinary retention.4 Antihistamines and anticholinergics are inexpensive, with most options costing less than $1 per dose5 (Table 2).
Table 2. Common Antiemetics Used in the Ambulatory Setting
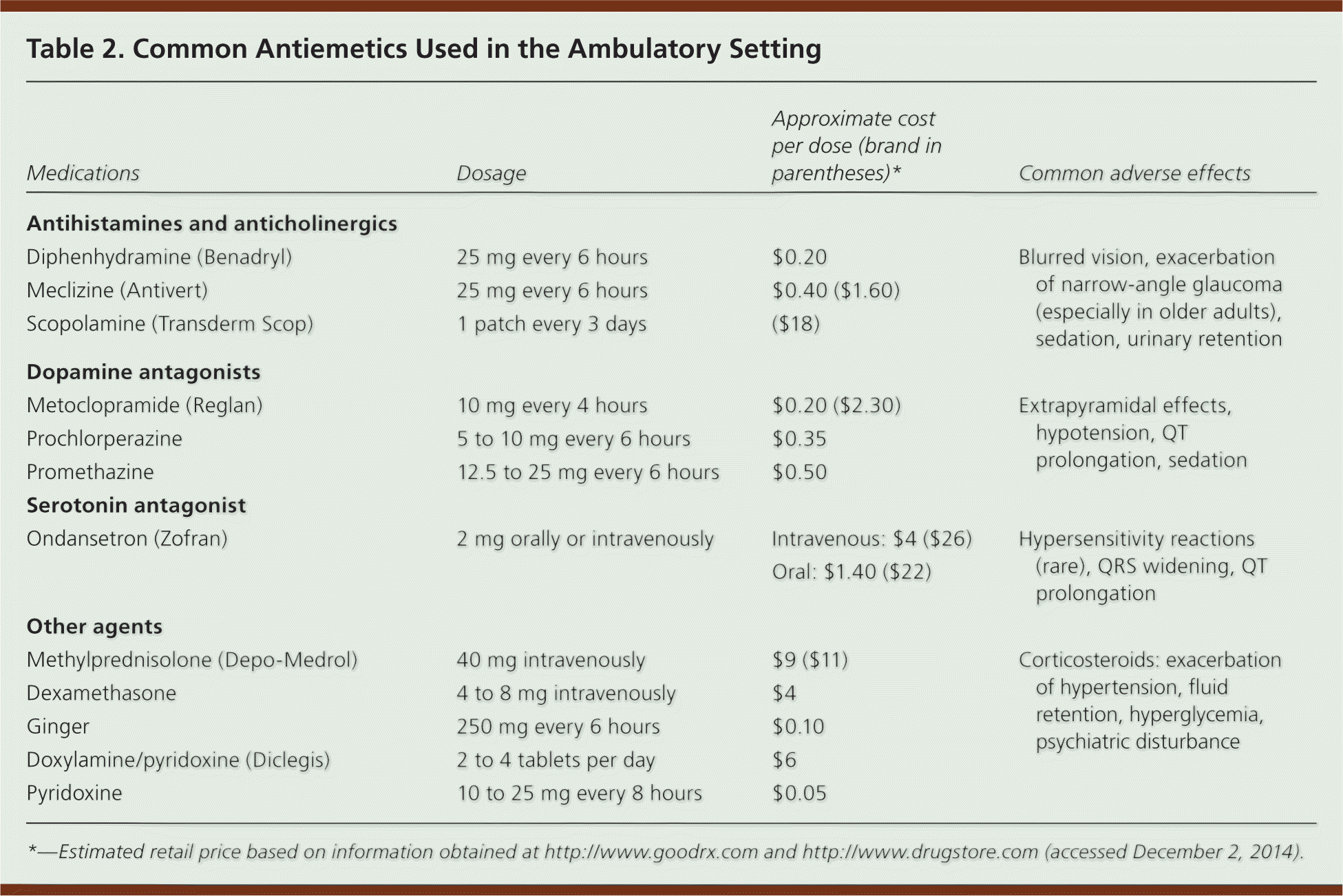
| Medications | Dosage | Approximate cost per dose (brand in parentheses)* | Common adverse effects |
|---|---|---|---|
| Antihistamines and anticholinergics | |||
| Diphenhydramine (Benadryl) | 25 mg every 6 hours | $0.20 | Blurred vision, exacerbation of narrow-angle glaucoma (especially in older adults), sedation, urinary retention |
| Meclizine (Antivert) | 25 mg every 6 hours | $0.40 ($1.60) | |
| Scopolamine (Transderm Scop) | 1 patch every 3 days | ($18) | |
| Dopamine antagonists | |||
| Metoclopramide (Reglan) | 10 mg every 4 hours | $0.20 ($2.30) | Extrapyramidal effects, hypotension, QT prolongation, sedation |
| Prochlorperazine | 5 to 10 mg every 6 hours | $0.35 | |
| Promethazine | 12.5 to 25 mg every 6 hours | $0.50 | |
| Serotonin antagonist | |||
| Ondansetron (Zofran) | 2 mg orally or intravenously | Intravenous: $4 ($26) | Hypersensitivity reactions (rare), QRS widening, QT prolongation |
| Oral: $1.40 ($22) | |||
| Other agents | |||
| Methylprednisolone (Depo-Medrol) | 40 mg intravenously | $9 ($11) | Corticosteroids: exacerbation of hypertension, fluid retention, hyperglycemia, psychiatric disturbance |
| Dexamethasone | 4 to 8 mg intravenously | $4 | |
| Ginger | 250 mg every 6 hours | $0.10 | |
| Doxylamine/pyridoxine (Diclegis) | 2 to 4 tablets per day | $6 | |
| Pyridoxine | 10 to 25 mg every 8 hours | $0.05 | |
*—Estimated retail price based on information obtained at http://www.goodrx.com and http://www.drugstore.com (accessed December 2, 2014).
DOPAMINE ANTAGONISTS
Dopamine antagonists include metoclopramide (Reglan), promethazine, and prochlorperazine. They block dopamine stimulation in the chemoreceptor trigger zone, thereby limiting emetic input to the medullary vomiting center. Dopamine antagonists are inexpensive, but have strong antihistamine effects and can cause significant sedation.
Metoclopramide can cause extrapyramidal effects, including irreversible tardive dyskinesia, although this is rare (incidence of less than 1%).6 Because this risk may be greater in frail older adults, independent of diagnoses, the American Geriatrics Society strongly recommends avoiding the use of metoclopramide for nausea in this population.7 Metoclopramide should not be used in patients receiving antipsychotics or other dopamine antagonists.
SELECTIVE SEROTONIN ANTAGONISTS
Selective serotonin antagonists inhibit serotonin at the 5-HT3 receptor in the small bowel, vagus nerve, and chemoreceptor trigger zone. They are generally effective and have largely replaced dopamine antagonists in most clinical situations. Adverse effects are uncommon but can include headache, diarrhea, and fatigue; these occur independent of dose and route of administration. All selective serotonin antagonists can cause asymptomatic, self-limited QT prolongation and QRS widening.8,9 In patients with underlying QT prolongation or who are taking concomitant medications that have the potential to prolong the QT interval, clinicians should use the lowest dose or consider alternatives.
COMPLEMENTARY AND ALTERNATIVE THERAPIES
Ginger has been used in traditional Indian and Chinese medicine as an antiemetic. Although its mechanism of action is not completely understood, ginger is thought to antagonize the 5-HT3 and cholinergic receptors, and may have direct activity on the gastrointestinal tract. Although ginger can cause reflux and heartburn, and may potentiate bleeding because of its anticoagulant effects, dosages of up to 2 g per day in divided doses of 250 mg are considered safe, even in pregnant women.10,11
Pyridoxine (vitamin B6), with or without doxylamine, has been recommended for treating nausea and vomiting in pregnancy. Typical dosages of 10 to 25 mg every eight hours cause minimal adverse effects12; however, there is little evidence to support the use of pyridoxine for the treatment of nausea and vomiting from other causes.
Clinical Situations
VESTIBULAR NAUSEA/MOTION SICKNESS
Unlike other forms of nausea, which tend to be mediated by dopamine and serotonin, vestibular system–induced nausea is mediated primarily by histamine and acetylcholine. Consequently, the American Gastroenterological Association recommends the use of antihistamines and anticholinergics for nausea secondary to vertigo and motion sickness.13 Antihistamines are the most common agents used in the treatment of vestibular-mediated motion sickness.14 However, the use of antihistamines is limited by their sedative effects. Transdermal scopolamine (Transderm Scop) is preferred over antihistamines for prevention of motion sickness in persons desiring wakefulness during travel.15 It can be used for up to 72 hours per dose, with the onset occurring six to eight hours after application to the mastoid.16 Ginger also relieves nausea associated with motion sickness, and is most effective if the patient believes it will work.15
MIGRAINE-ASSOCIATED NAUSEA
Migraine headaches are commonly associated with gastrointestinal symptoms. Approximately 60% of patients with migraines develop nausea and vomiting during an acute attack.17 Nausea and vomiting associated with migraines are caused by a central process, with dopamine being a primary mediator; thus, dopamine antagonists such as metoclopramide, prochlorperazine, and chlorpromazine are logical choices for treatment. Although triptans may abort the central process contributing to nausea, they have lower oral bioavailability during an acute attack because of altered gastric motility.18 Metoclopramide increases gastric motility and response to oral anti-migraine medications. A Cochrane review found that in patients with acute migraine, a combination of metoclopramide and aspirin improved nausea and vomiting with fewer adverse events compared with sumatriptan (Imitrex).19
GASTROENTERITIS
Oral rehydration solution is strongly recommended as first-line treatment of acute gastroenteritis with mild to moderate dehydration.2 When administration is limited by multiple episodes of vomiting, antiemetics may be useful. Because nausea in gastroenteritis is a result of visceral stimulation mediated primarily by serotonin, 5-HT3 antagonists are an effective treatment.13 A Cochrane review of several randomized, placebo-controlled trials concluded that a single oral dose of ondansetron (Zofran) controls vomiting and reduces hospitalizations and the need for intravenous fluid administration in children and adolescents.20 Ondansetron may increase episodes of diarrhea in this population. Although ondansetron costs more than promethazine, the reduced need for intravenous fluids makes it a cost-effective option.21
PREGNANCY-INDUCED NAUSEA
Nausea and vomiting occur in more than one-half of pregnancies.10,12 Although the pathogenesis of nausea and vomiting in pregnancy is not completely understood, it is thought to be multifactorial, with hormonal changes having a key role.12,22 Several antiemetic drug classes have been used for treatment, but there is limited evidence on fetal outcomes.
The American College of Obstetricians and Gynecologists recommends the use of pyridoxine with or without doxylamine as first-line pharmacotherapy for nausea and vomiting in pregnant women.12 A delayed-release formulation of 10 mg of doxylamine and 10 mg of pyridoxine (Diclegis) is available in the United States. In more severe cases in which dehydration or hyperemesis gravidarum occurs, intravenous rehydration may be necessary, and may be used in combination with antiemetics. Ondansetron has comparable effectiveness to older antiemetics, such as promethazine, and causes less sedation.23 Corticosteroids may be used in severe, persistent cases, but are not recommended before 10 weeks' gestation because of the increased risk of oral clefts.12
Complementary and alternative medicine is often used by pregnant women who wish to avoid pharmacologic therapies. Two recent meta-analyses found that, compared with placebo, ginger improves nausea and vomiting if taken for at least four days.10,24
Data Sources: Essential Evidence Plus, PubMed, the Cochrane database, and the National Guideline Clearinghouse were searched using the key terms nausea and vomiting, migraine headaches, motion sickness, gastroenteritis, ondansetron, and metoclopramide. The search included randomized controlled trials, clinical trials, and reviews. Search date: August 2014.

