A seven-year-old girl presented with a history of pain in her lower abdomen and buttocks. Her mother noticed blisters developing on the child's buttock. The child had no history of nausea, vomiting, diarrhea, fever, or chills. She had no history of trauma or new contacts, and was not taking any medications.
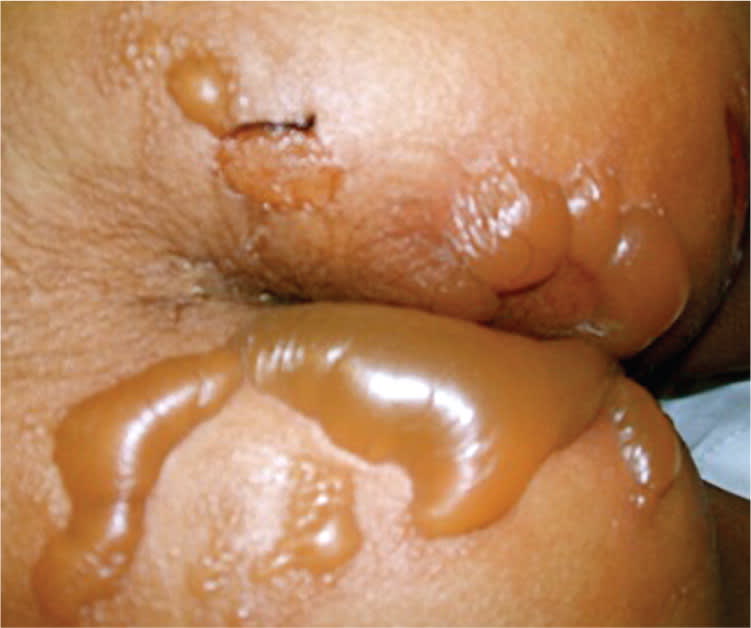
On examination, she was afebrile, and her pulse was 115 beats per minute. Her skin examination revealed multiple bullous lesions in the perirectal area involving the gluteal cleft and both buttocks (Figure 1). The bullae were 3 to 4 cm in diameter without surrounding erythema. There were no lesions elsewhere on her body. Her workup included a complete blood count, with a total white blood cell count of 12,000 per mm3 (12 × 109 per L) and an atypical lymphocyte count of 4.0%. A C-reactive protein measurement was normal at less than 0.5 mg per L (4.76 nmol per L).
Figure 1.
Question
Based on the patient's history, physical examination, and laboratory findings, which one of the following is the most likely diagnosis?
A. Allergic contact dermatitis.
B. Bullous impetigo.
C. Bullous pemphigus.
D. Dermatitis herpetiformis.
E. Linear immunoglobulin A (IgA) dermatosis.
Discussion
The answer is B: bullous impetigo. Impetigo is a highly contagious, superficial skin infection that most commonly affects children two to five years of age. The two types of impetigo are bullous and nonbullous. The diagnosis is clinical, and culture is rarely used for confirmation. Bullous impetigo begins with small vesicles on the face, trunk, buttocks, perineum, or extremities, with no surrounding erythema.1 The vesicles enlarge rapidly into flaccid, transparent bullae that are 1 to 5 cm in diameter. Nonbullous impetigo presents as thick adherent crusty lesions with a characteristic golden appearance. It usually affects the face and extremities.
Complications of impetigo may include lymphadenitis, cellulitis, sepsis, or nephritis. The topical antibiotics mupirocin (Bactroban), retapamulin (Altabax), and fusidic acid are as effective as oral antibiotics when disease is limited.2 Oral antibiotics are considered when disease is extensive or to help decrease transmission in a community outbreak.3
Allergic contact dermatitis presents as localized pruritic dermatitis 12 to 24 hours after exposure to a contact allergen. The configuration and location of the dermatitis are often clues to the offending allergen.4 Epicutaneous patch testing may be necessary to identify specific exposure antigens. Topical therapy with a midpotency corticosteroid ointment is recommended.
Bullous pemphigus is a blistering disease caused by autoantibodies that interfere with adhesion of keratinocytes. Pemphigus vulgaris leads to blisters and erosions of mucous membranes and skin. The diagnosis of pemphigus requires the biopsy of a skin lesion. Systemic steroids are the mainstay of therapy.
Dermatitis herpetiformis is an autoimmune blistering disorder associated with gluten sensitive enteropathy. It is highly pruritic, and the vesicles are often excoriated to erosions by the time of physical examination. Onset is often between 20 and 40 years of age, but may occur at any age. Patients typically experience prompt relief of lesions within one to two days of treatment with dapsone or sulfapyridine.
Linear IgA dermatosis is an autoimmune skin disease. It is usually idiopathic but can be caused by infections, medication use (e.g., vancomycin), or malignancy. It usually presents before five years of age with the abrupt onset of tense bullae on an inflamed, erythematous base. It is accompanied by pruritus and a burning sensation. The diagnosis can be confirmed by direct immunofluorescence, which displays linear IgA deposits along the epidermal basement membrane. Treatment may include dapsone, sulfapyridine, or steroids.
Summary Table
| Condition | Characteristics |
|---|---|
| Allergic contact dermatitis | Localized pruritic dermatitis; in configuration and location of exposure to contact allergen |
| Bullous impetigo | Crusty golden lesions on face and extremities; enlarging flaccid transparent bullae; most common in children 2 to 5 years of age |
| Bullous pemphigus | Autoimmune disease; blisters and erosions of mucous membranes and skin |
| Dermatitis herpetiformis | Autoimmune disease; associated with gluten sensitive enteropathy; extremely pruritic vesicles with symmetric distribution on extensor surfaces; onset often occurs between 20 and 40 years of age |
| Linear immunoglobulin A dermatosis | Autoimmune disease; abrupt onset of tense bullae on an inflamed, erythematous base; associated with pruritus and burning sensation; usually presents before 5 years of age |

