More than 30% of U.S. adults report having experienced low back pain within the preceding three months. Although most low back pain is nonspecific and self-limiting, a subset of patients develop chronic low back pain, defined as persistent symptoms for longer than three months. Low back pain is categorized as nonspecific low back pain without radiculopathy, low back pain with radicular symptoms, or secondary low back pain with a spinal cause. Imaging should be reserved for patients with red flags for cauda equina syndrome, recent trauma, risk of infection, or when warranted before treatment (e.g., surgical, interventional). Prompt recognition of cauda equina syndrome is critical. Patient education should be combined with evidence-guided pharmacologic therapy. Goals of therapy include reducing the severity of pain symptoms, pain interference, and disability, as well as maximizing activity. Validated tools such as the Oswestry Disability Index can help assess symptom severity and functional change in patients with chronic low back pain. Epidural steroid injections do not improve pain or disability in patients with spinal stenosis. Spinal manipulation therapy produces small benefits for up to six months. Because long-term data are lacking for spinal surgery, patient education about realistic outcome expectations is essential.
More than 30% of U.S. adults report experiencing low back pain in the preceding three months. Significant functional and financial sequelae arise from this poorly understood pain syndrome.1 The National Institute of Neurological Disorders and Stroke defines chronic low back pain as lumbar pain present for more than three months. Interprofessional, multimodal care coordinated by a primary care physician is often required for optimal control of chronic low back pain.2–6 Figure 1 provides a suggested approach to the evaluation and management of chronic low back pain.
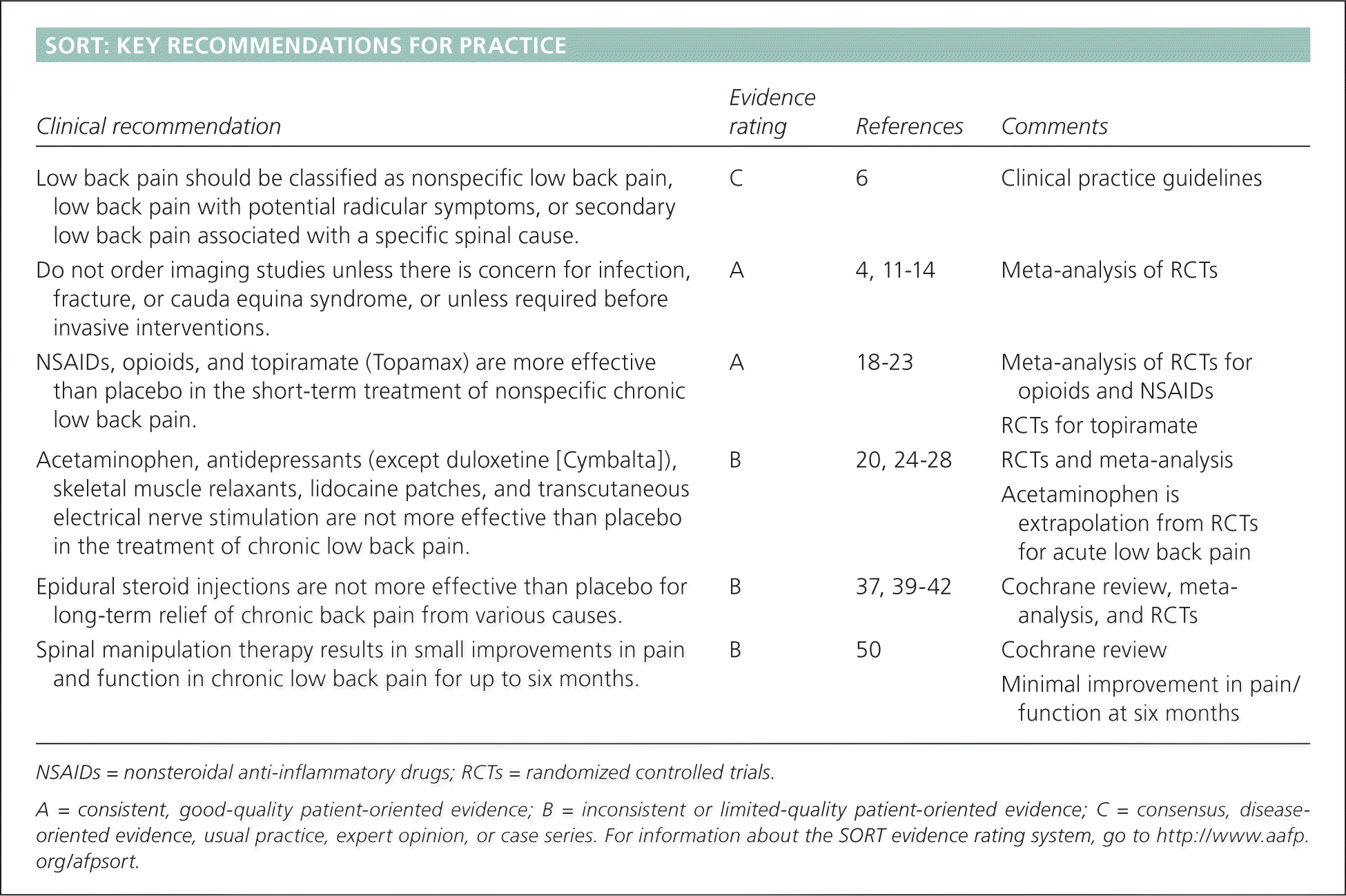
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Low back pain should be classified as nonspecific low back pain, low back pain with potential radicular symptoms, or secondary low back pain associated with a specific spinal cause. | C | 6 | Clinical practice guidelines |
| Do not order imaging studies unless there is concern for infection, fracture, or cauda equina syndrome, or unless required before invasive interventions. | A | 4, 11–14 | Meta-analysis of RCTs |
| NSAIDs, opioids, and topiramate (Topamax) are more effective than placebo in the short-term treatment of nonspecific chronic low back pain. | A | 18–23 | Meta-analysis of RCTs for opioids and NSAIDs RCTs for topiramate |
| Acetaminophen, antidepressants (except duloxetine [Cymbalta]), skeletal muscle relaxants, lidocaine patches, and transcutaneous electrical nerve stimulation are not more effective than placebo in the treatment of chronic low back pain. | B | 20, 24–28 | RCTs and meta-analysis Acetaminophen is extrapolation from RCTs for acute low back pain |
| Epidural steroid injections are not more effective than placebo for long-term relief of chronic back pain from various causes. | B | 37, 39–42 | Cochrane review, meta-analysis, and RCTs |
| Spinal manipulation therapy results in small improvements in pain and function in chronic low back pain for up to six months. | B | 50 | Cochrane review Minimal improvement in pain/ function at six months |
NSAIDs = nonsteroidal anti-inflammatory drugs; RCTs = randomized controlled trials.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN MUSCULOSKELETAL CARE: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not order an electromyogram for low back pain unless there is leg pain or sciatica. | American Academy of Physical Medicine and Rehabilitation |
| Do not order an imaging study for back pain without performing a thorough physical examination. | American Academy of Physical Medicine and Rehabilitation |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Figure 1. Suggested Approach to the Patient with Chronic Low Back Pain
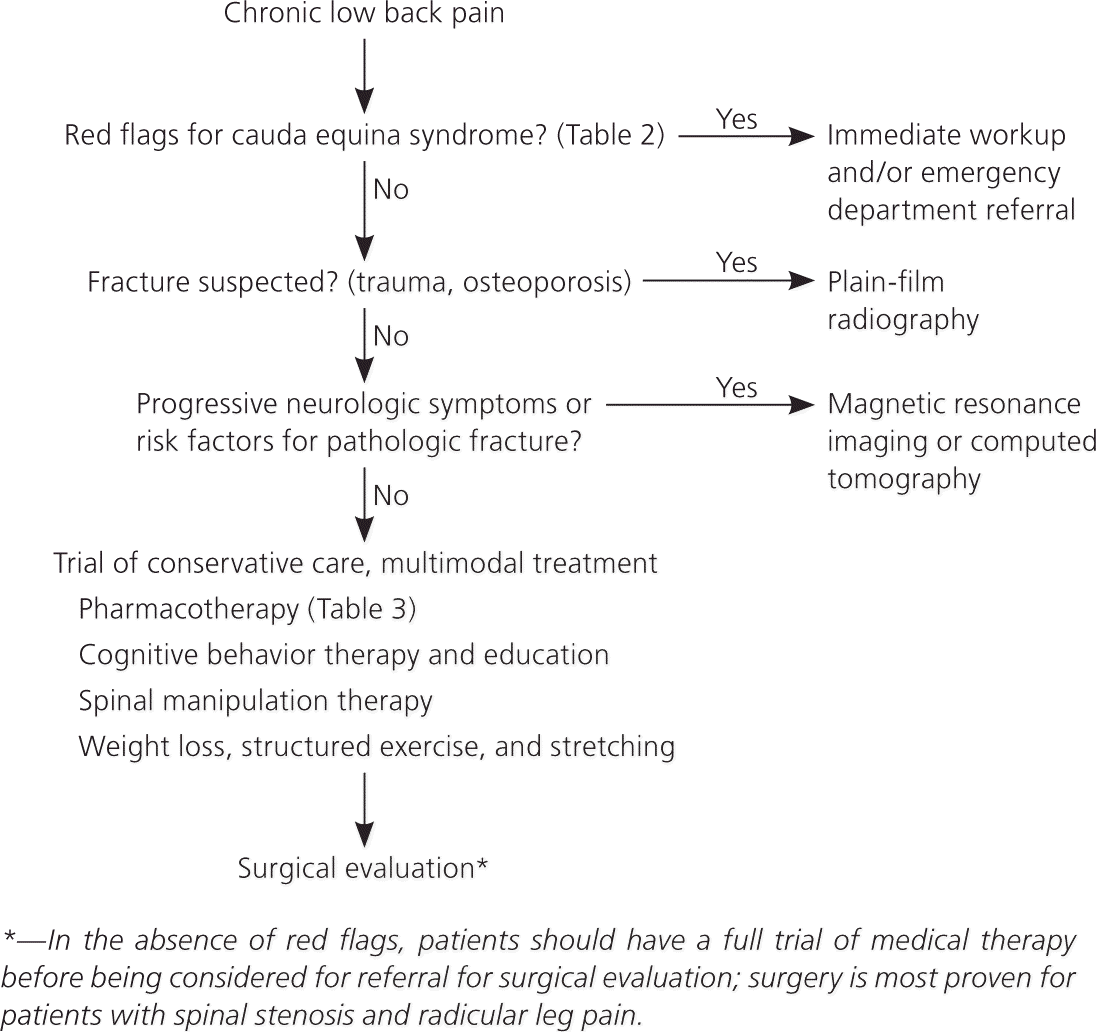
A suggested approach to the patient with chronic low back pain.
Evaluation
Depending on the chronicity of the pain symptoms, numerous diagnoses should be considered during evaluation (Table 1). A history and targeted physical examination will often narrow the list of potential diagnoses.7 Acute low back pain from musculoskeletal sprain or strain rarely necessitates extensive workup or imaging. Guidelines from the American College of Physicians and the American Pain Society recommend initial categorization of low back pain into nonspecific low back pain, low back pain with potential radicular symptoms, or secondary low back pain associated with a specific spinal cause (i.e., neoplasm or infectious process).6 These practice guidelines outline an approach to the initial presentation of symptoms, rather than the ongoing management of chronic low back pain. There are few data to support provocative or palliative discography before selecting treatments.5
Table 1. Selected Differential Diagnosis for Chronic Low Back Pain

| Abdominal aortic aneurysm |
| Ankylosing spondylitis |
| Epidural abscess |
| Fracture of the pars interarticularis |
| Metastatic malignancy |
| Osteoarthritis of the hip |
| Osteoporosis |
| Piriformis syndrome |
| Radiculitis |
| Sacroiliac joint dysfunction |
| Traumatic fracture |
| Trochanteric bursitis |
| Varicella zoster virus |
What Are the Red Flags for Epidural Spinal Cord Compression/Cauda Equina Syndrome?
It is critical to promptly identify and refer patients with evidence of severe central canal stenosis resulting in epidural spinal cord compression or, below the L1 vertebral level, cauda equina syndrome, which may result in irreversible neurologic dysfunction.8 The cauda equina, Latin for horse's tail, consists of a complex group of spinal nerves and associated roots spanning from the L2 to the S5 vertebral levels.9 Significant impingement or compression typically results from neoplastic invasion or severe broad-based disk bulge or herniation. Common red flags for cauda equina syndrome are provided in Table 2 and include acute presentation or worsening of radiating pain, sensorimotor disturbances, gait abnormalities resulting from impaired foot dorsiflexion, and urinary and/or bowel dysfunction.10 Epidural spinal cord compression and cauda equina syndrome should be considered medical emergencies.
Table 2. Red Flag Signs and Symptoms for Cauda Equina Syndrome or Serious Underlying Cause of Back Pain

| Abnormal gait with lack of heel to toe ambulation |
| Absence of perineal reflex |
| Acute presentation of bilateral sciatica |
| Acute urinary retention |
| Drop foot or inability to dorsiflex the foot |
| Intravenous drug abuse |
| Progressive neuromotor or sensory loss |
| Recent diagnosis of malignancy |
| Recent infection |
| Recumbent worsening of pain |
| Saddle block anesthesia |
| Urinary and/or bowel incontinence |
When Should Imaging Be Considered?
In the absence of red flags, plain-film radiography, magnetic resonance imaging (MRI), or computed tomography (CT) is not warranted in the acute presentation of low back pain and does not modify patient outcomes.4,11 Unless a high suspicion for infection, fracture, or cauda equina exists, clinicians should not order imaging for acute low back pain. Numerous high-quality randomized studies have compared immediate vs. delayed imaging with no appreciable differences in disease course.4,12 Additionally, no difference in outcomes for patients with low back pain was identified when comparing the less expensive plain-film lumbar radiography with more expensive imaging modalities such as MRI or CT.13,14
The American College of Physicians/American Pain Society joint guidelines discourage routine imaging for nonspecific low back pain.6 Consideration of imaging should be guided by the history and physical examination. Plain-film radiography of the lumbar spine is warranted in patients at risk of ventral vertebral fracture due to recent trauma or osteoporosis. CT or MRI should be considered for patients with significant risk factors for underlying serious conditions or progressive neurologic changes (Table 2).
Which Patients with Acute Low Back Pain Develop Chronic Low Back Pain?
Few objective measures accurately predict progression from acute to nonspecific chronic low back pain or resulting disability. Imaging results, physical examination findings, and type of injury do not correlate with chronicity or severity of symptoms.12 Several large case-control studies have identified nonpathology-dependent variables that are associated with back pain persistence and greater severity of symptoms.15,16 These variables include workers' compensation claim status, litigation status, comorbid mental health diagnosis, injury sustained at work vs. at home, and socioeconomic factors.17 These “yellow flags” suggest that biopsychosocial factors significantly contribute to symptoms and underline the importance of a multiprofessional approach to treatment.
Which Medications Are Effective?
Pharmacologic therapy for chronic low back pain may be categorized into nonopioid analgesics (e.g., nonsteroidal anti-inflammatory drugs, acetaminophen), opioids, skeletal muscle relaxants, and adjuvant analgesics (e.g., anti-depressants, anticonvulsants).18–20
In general, long-term controlled studies of medications for chronic low back pain are lacking. Specifically, topiramate (Topamax), select opioids, and nonsteroidal anti-inflammatory drugs appear more effective than placebo in the short-term treatment of chronic nonspecific low back pain.18–23 Acetaminophen, antidepressants (excluding duloxetine [Cymbalta]), skeletal muscle relaxants, and lidocaine patches are not more effective than placebo for chronic low back pain.20,24–28 Classes of medications with corresponding levels of supporting evidence are provided in Table 3.21–26,28–30 Combining drug classes or combining pharmacologic with nonpharmacologic interventions, although of uncertain benefit, is often necessary to alleviate symptoms and improve disability.
Table 3. Pharmacologic Treatment Options for Chronic Low Back Pain
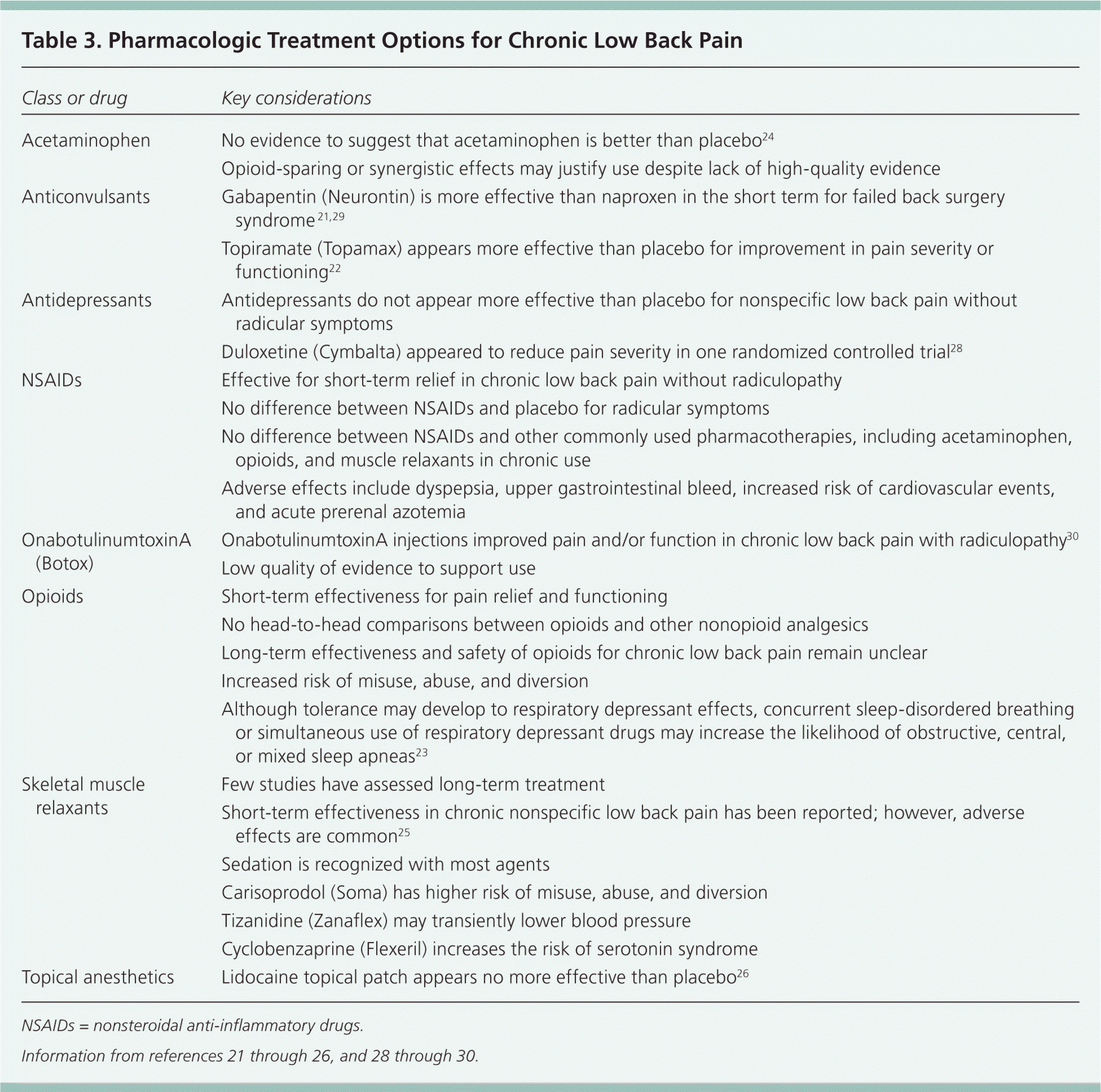
| Class or drug | Key considerations |
|---|---|
| Acetaminophen | No evidence to suggest that acetaminophen is better than placebo24 |
| Opioid-sparing or synergistic effects may justify use despite lack of high-quality evidence | |
| Anticonvulsants | Gabapentin (Neurontin) is more effective than naproxen in the short term for failed back surgery syndrome 21,29 |
| Topiramate (Topamax) appears more effective than placebo for improvement in pain severity or functioning22 | |
| Antidepressants | Antidepressants do not appear more effective than placebo for nonspecific low back pain without radicular symptoms |
| Duloxetine (Cymbalta) appeared to reduce pain severity in one randomized controlled trial28 | |
| NSAIDs | Effective for short-term relief in chronic low back pain without radiculopathy |
| No difference between NSAIDs and placebo for radicular symptoms | |
| No difference between NSAIDs and other commonly used pharmacotherapies, including acetaminophen, opioids, and muscle relaxants in chronic use | |
| Adverse effects include dyspepsia, upper gastrointestinal bleed, increased risk of cardiovascular events, and acute prerenal azotemia | |
| OnabotulinumtoxinA (Botox) | OnabotulinumtoxinA injections improved pain and/or function in chronic low back pain with radiculopathy30 |
| Low quality of evidence to support use | |
| Opioids | Short-term effectiveness for pain relief and functioning |
| No head-to-head comparisons between opioids and other nonopioid analgesics | |
| Long-term effectiveness and safety of opioids for chronic low back pain remain unclear | |
| Increased risk of misuse, abuse, and diversion | |
| Although tolerance may develop to respiratory depressant effects, concurrent sleep-disordered breathing or simultaneous use of respiratory depressant drugs may increase the likelihood of obstructive, central, or mixed sleep apneas23 | |
| Skeletal muscle relaxants | Few studies have assessed long-term treatment |
| Short-term effectiveness in chronic nonspecific low back pain has been reported; however, adverse effects are common25 | |
| Sedation is recognized with most agents | |
| Carisoprodol (Soma) has higher risk of misuse, abuse, and diversion | |
| Tizanidine (Zanaflex) may transiently lower blood pressure | |
| Cyclobenzaprine (Flexeril) increases the risk of serotonin syndrome | |
| Topical anesthetics | Lidocaine topical patch appears no more effective than placebo26 |
NSAIDs = nonsteroidal anti-inflammatory drugs.
Information from references 21 through 26, and 28 through 30.
What Is the Role of Opioid Analgesics in the Treatment of Chronic Low Back Pain?
A recent systematic review identified 15 randomized controlled trials of varying quality and duration assessing the impact of opioid analgesic therapy on pain severity and functional outcomes in chronic low back pain.23 Seven trials compared tramadol or tramadol/acetaminophen vs. placebo or celecoxib (Celebrex). Additional studies included in the systematic review assessed buprenorphine, hydromorphone (Dilaudid), morphine, oxycodone, oxymorphone, and tapentadol (Nucynta). Overall, opioids demonstrated only short-term reduction in severity scores and improvement of functional outcomes of questionable clinical significance. However, several clinical chronic pain guidelines not specifically addressing low back pain support the judicious use of chronic opioid therapy for severe pain that is refractory to other modalities if the benefits outweigh the risks.31,32
Should Patients Be Referred for Formal Education Programs or Behavior Treatment?
Well-designed studies have assessed the impact of formal patient education programs on pain severity, symptom catastrophizing, functionality, and disability in patients with chronic low back pain. Numerous educational modalities have demonstrated short-term improvement in symptoms and other outcomes, although it is uncertain how long these effects persist. When available, formal education should be offered to all patients with chronic low back pain. Cognitive behavior therapy and acceptance and coping therapy represent an essential component of multidisciplinary management of chronic low back pain.33 Other nonpharmacologic therapies (e.g., exercise programs, relaxation therapy, guided imagery), although lacking high-quality supporting evidence, should be considered as part of the rehabilitative plan.34 A meta-analysis of 41 randomized controlled trials suggests that multidisciplinary biopsychosocial rehabilitation has small, yet meaningful, effects on symptom severity, disability, and work outcomes in patients with chronic low back pain compared with standard care.35
Which Monitoring Strategy Should Be Used for Ongoing Patient Assessment?
Numerous validated tools can help clinicians assess symptom severity and functional change in patients with chronic low back pain. Perhaps the most widely used tool is the Oswestry Disability Index, which consists of 12 assessment items covering 10 domains including pain intensity, personal care, lifting, walking, sitting, standing, sleeping, sex life, social life, and traveling.36 The index is available at http://www.aadep.org/documents/resources/Appendix_D__The_Oswestry_Disability_477E0AE6E8258.pdf. The scoring directions allow the clinician to assess the level of associated disability or pain interference. Clinician preference and ease of administration should guide tool selection. Consistency in assessment method is paramount. Patients should be periodically assessed for new signs or symptoms of serious underlying pathology.
Which Interventions Should Be Considered for Patients with Chronic Low Back Pain?
A 2008 Cochrane review included two studies that compared the effectiveness of facet or epidural steroid injection (ESI) vs. placebo for pain relief and disability in low back pain.37 Neither study found a significant difference between the injection and placebo groups in general improvement, pain relief, or disability. In contrast, a 2009 review on nonsurgical interventional therapies for low back pain found some evidence of short-term benefit from ESI.2 More recently, two separate, high-quality trials randomized patients with documented spinal stenosis and moderate to severe radicular symptoms to receive ESI plus lidocaine vs. transforaminal epidural lidocaine alone.38,39 The ESI plus lidocaine group fared no better than the control group in symptom severity or disability index score, even when controlled for specific injection technique and approach. A 2013 meta-analysis of 29 studies found no differences in outcomes between ESI and control groups at six months after controlling for baseline pain scores.40 Before the use of fluoroscopy-guided ESI, a series of injections were performed to account for the variability in drug placement. A 2008 literature review examined the rationale for administering repeat ESIs in radicular low back pain, and concluded that there is no evidence to support repeated ESI.41
Currently, there are no moderate- or high-quality studies to support the routine use of spinal cord stimulator placement for nonspecific chronic low back pain. However, it may improve pain scores and disability measures in a subset of patients with failed back surgery syndrome.42
Which Patients Should Be Considered for Surgical Evaluation?
Although approximately 1 million spinal surgeries are performed annually in the United States,43 high-quality, long-term data are lacking or equivocal for many of the procedures performed. The Spine Patient Outcomes Research Trial, a randomized cohort study, compared the effect of surgical intervention with that of nonsurgical medical management for spinal stenosis, lumbar disk herniation, and spondylolisthesis.44–47 Patients with lumbar disk herniation who received open discectomy or microdiscectomy did not differ statistically from the nonsurgical control group. Similarly, treatment outcomes for patients who underwent laminectomy with or without fusion for degenerative spondylolisthesis were similar to outcomes in the nonsurgical control group on intent-to-treat analysis. In contrast, patients with evidence of spinal stenosis and radicular leg pain who were assigned to decompressive laminectomy showed sustained improvement in bodily pain, physical function, and Oswestry Disability Index scores up to four years postsurgery.47 However, it is difficult to interpret these findings given the high frequency of crossover and variability in symptom severity. Minimally invasive spinal surgery appears to be a promising treatment modality, although rigorous studies have not been completed to date.48,49 Patient education on realistic expectations of outcomes from a surgical referral for chronic low back pain is essential.
How Does Spinal Manipulation Therapy Compare with Other Interventions?
A 2011 Cochrane review compared spinal manipulation therapy vs. other standard forms of therapy, such as exercise, medical treatment, or physical therapy.50 Only nine of 26 reviewed studies were determined to have a low risk of bias. Of these, eight compared spinal manipulation therapy with all other therapies and found that spinal manipulation therapy resulted in a small but statistically significant improvement in patients' pain level at one and six months. The clinical significance of this difference was very small. In addition, three of these studies also included a 12-month follow-up showing that spinal manipulation therapy was not more effective in reducing pain at 12 months. For functional status, there was statistically significant but clinically small improvement at one month, but no statistically significant improvement at six or 12 months.
Is TENS an Effective Treatment for Chronic Low Back Pain?
Transcutaneous electrical nerve stimulation (TENS) therapy uses electrical current, delivered via electrodes placed on intact skin, to stimulate peripheral nerves. According to the gate-control theory, this stimulation activates inhibitory interneurons in the spinal cord, thereby interfering with the propagation of pain signals.51 A Cochrane review on the subject included four high-quality randomized controlled trials and concluded that TENS was not more effective than placebo for low back pain.27 Three studies addressed whether the use of TENS decreased the intensity of chronic low back pain, and found conflicting evidence of benefit. Two of the studies showed no statistically significant or clinically important improvements at their end points of two weeks and four weeks.52,53 In the same Cochrane review, two studies addressed whether TENS improves functional status in patients with chronic low back pain using validated scales of disability. Both studies failed to demonstrate improvement in functional status.54,55
Data Sources: EBSCO Host and PubMed searches were completed using the key term low back pain alone and in combination with assessment, diagnosis, clinical practice guidelines, injections, management, prognosis, systematic review, treatment, and surgery. Additionally, we searched the Cochrane, National Institute of Neurological Disorders and Stroke, National Institutes of Health Pain Consortium, and the National Guideline Clearinghouse databases using the key term chronic low back pain. Search dates: November 21, 2014, and February 13, 2015.

