Hypertension is one of the most common conditions encountered in primary care. Nonpharmacologic strategies have been shown to help lower blood pressure. Lifestyle modifications are recommended for all patients with hypertension. The American Heart Association/American College of Cardiology lifestyle management guideline recommends a diet emphasizing vegetables, fruits, and whole grains; limiting sodium intake to less than 2,400 mg per day; and exercising three or four times per week for an average of 40 minutes per session. Other nonpharmacologic strategies include weight loss, tobacco cessation, decreased alcohol consumption, biofeedback, and self-measured blood pressure monitoring. For patients with obstructive sleep apnea, the use of continuous positive airway pressure has been shown to improve blood pressure. Dietary supplements such as garlic, cocoa, vitamin C, coenzyme Q10, omega-3 fatty acids, and magnesium have been suggested for lowering blood pressure, but evidence is lacking.
Hypertension is one of the most preventable contributors to disease and death.1–3 Based on data from 2007 to 2010, 33% of U.S. adults 20 years and older—an estimated 78 million—have hypertension, which is defined as blood pressure greater than 140/90 mm Hg.4 The prevalence is nearly equal between men and women. Worldwide, hypertension is most prevalent among black adults (44%).4 It is the most common condition treated in primary care and can lead to myocardial infarction, stroke, renal failure, and death if not detected early and treated appropriately.4
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendations | Evidence rating | References |
|---|---|---|
| A diet that emphasizes vegetables, fruits, and whole grains is recommended to lower blood pressure. | A | 6, 7 |
| Limiting sodium intake to 2,400 mg per day is recommended to lower blood pressure. Additional benefit occurs with a limit of 1,500 mg per day. | B | 6 |
| To lower blood pressure, patients should engage in moderate to vigorous aerobic physical activity three or four times per week for an average of 40 minutes per session. | A | 6, 14 |
| Clinicians should ask all adults about tobacco use and provide tobacco cessation interventions for those who use tobacco products. | A | 17, 18, 21 |
| To lower blood pressure, alcohol consumption should be limited to no more than two drinks per day for most men and one drink per day for women. | C | 2, 22 |
| Self-measured blood pressure monitoring, with or without additional support (e.g., education, counseling, telemedicine, home visits, Web-based logging), lowers blood pressure compared with usual care, although the benefits beyond 12 months are not clear. | A | 25 |
| Patients with hypertension and obstructive sleep apnea should use continuous positive airway pressure to lower blood pressure. | C | 30 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
A reduction in systolic blood pressure of 5 mm Hg has been associated in observational studies with mortality reductions of 14% from stroke, 9% from heart disease, and 7% from all causes.5 In 2014, the eighth report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 8) addressed guidelines to offer clinicians an analysis of what is and what is not known about blood pressure treatment thresholds, goals, and drug treatment strategies based on evidence from randomized controlled trials.1
JNC 8 did not directly address lifestyle treatments such as healthy diet, weight control, and regular exercise.1 However, a subgroup of the JNC 8 committee later published the American Heart Association/American College of Cardiology (AHA/ACC) lifestyle management guideline,6 which will be outlined in this article. In addition, other nonpharmacologic strategies such as weight loss, tobacco cessation, meditation, acupuncture, biofeedback, self-measured blood pressure monitoring, dietary supplements (e.g., garlic, cocoa, vitamin C, coenzyme Q10, omega-3 fatty acids, magnesium), and the use of continuous positive airway pressure for patients with obstructive sleep apnea (OSA) will be discussed.
Diet
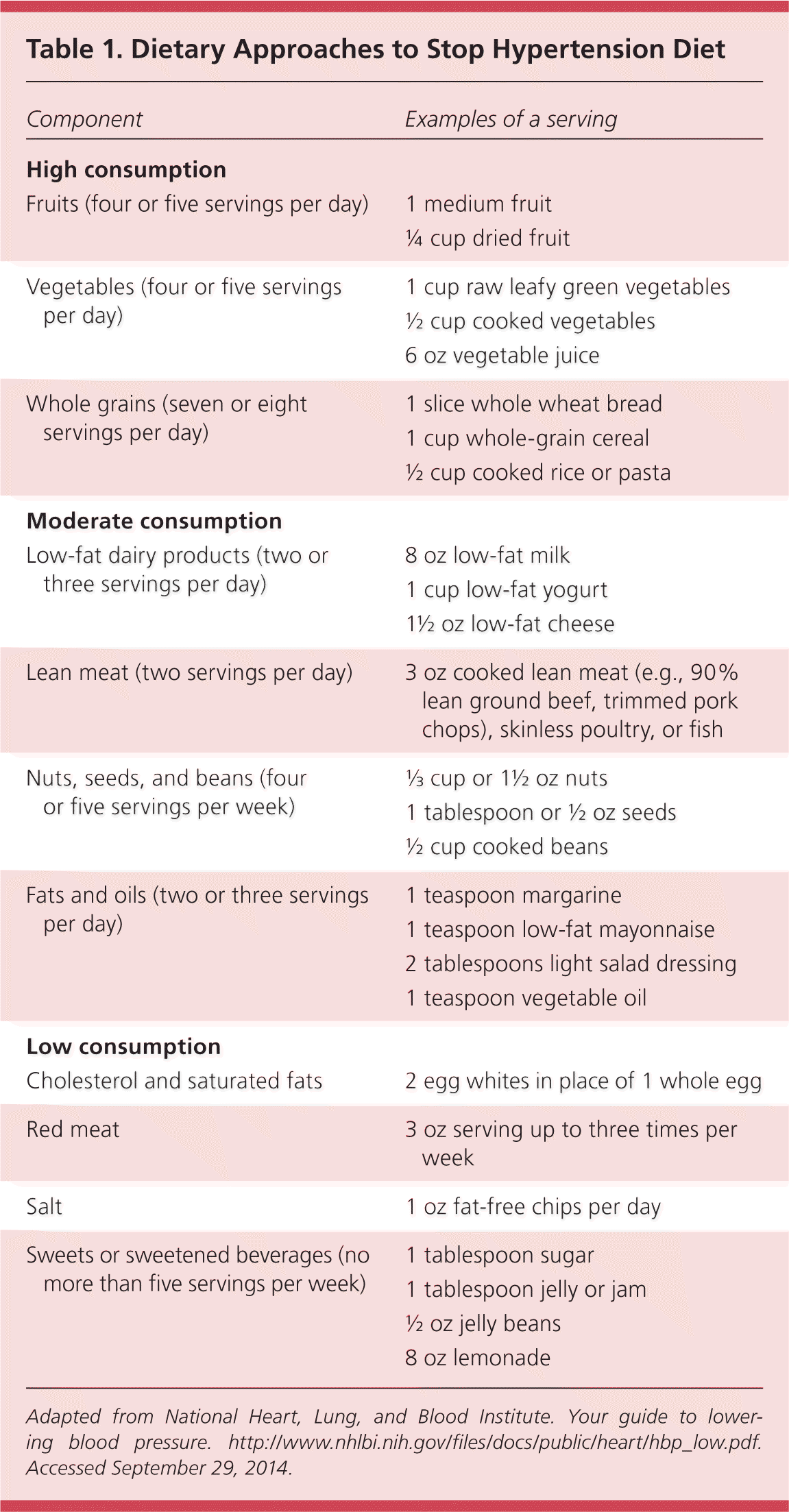
A diet with a high intake of vegetables, fruits, and whole grains is recommended.6,7 Other recommendations include consuming low-fat dairy products, poultry, fish, legumes, non-tropical vegetable oils, and nuts; and limiting intake of sweets, sugar-sweetened beverages, and red meat. This dietary pattern should be adapted to appropriate calorie requirements, personal and cultural food preferences, and nutritional therapy for other medical conditions, including diabetes mellitus. One way to achieve this is by following plans such as the Dietary Approaches to Stop Hypertension (DASH) diet (Table 18 ), the U.S. Department of Agriculture (USDA) Food Patterns, or the AHA diet.
Table 1. Dietary Approaches to Stop Hypertension Diet
| Component | Examples of a serving |
|---|---|
| High consumption | |
| Fruits (four or five servings per day) | 1 medium fruit |
| ¼ cup dried fruit | |
| Vegetables (four or five servings per day) | 1 cup raw leafy green vegetables |
| ½ cup cooked vegetables | |
| 6 oz vegetable juice | |
| Whole grains (seven or eight servings per day) | 1 slice whole wheat bread |
| 1 cup whole-grain cereal | |
| ½ cup cooked rice or pasta | |
| Moderate consumption | |
| Low-fat dairy products (two or three servings per day) | 8 oz low-fat milk |
| 1 cup low-fat yogurt | |
| 1½ oz low-fat cheese | |
| Lean meat (two servings per day) | 3 oz cooked lean meat (e.g., 90% lean ground beef, trimmed pork chops), skinless poultry, or fish |
| Nuts, seeds, and beans (four or five servings per week) | ⅓ cup or 1½ oz nuts |
| 1 tablespoon or ½ oz seeds | |
| ½ cup cooked beans | |
| Fats and oils (two or three servings per day) | 1 teaspoon margarine |
| 1 teaspoon low-fat mayonnaise | |
| 2 tablespoons light salad dressing | |
| 1 teaspoon vegetable oil | |
| Low consumption | |
| Cholesterol and saturated fats | 2 egg whites in place of 1 whole egg |
| Red meat | 3 oz serving up to three times per week |
| Salt | 1 oz fat-free chips per day |
| Sweets or sweetened beverages (no more than five servings per week) | 1 tablespoon sugar |
| 1 tablespoon jelly or jam | |
| ½ oz jelly beans | |
| 8 oz lemonade |
Adapted from National Heart, Lung, and Blood Institute. Your guide to lowering blood pressure. http://www.nhlbi.nih.gov/files/docs/public/heart/hbp_low.pdf. Accessed September 29, 2014.
Compared with a typical American diet of the 1990s, the DASH diet lowers systolic blood pressure by 5 to 6 mm Hg and diastolic blood pressure by 3 mm Hg.9–11 The USDA Food Patterns offer lacto-ovo vegetarian and vegan adaptations. The DASH diet is based on the AHA diet and emphasizes consuming less red meat, sweets, and sugar-sweetened beverages. More information about these diets is available at http://fnic.nal.usda.gov/diet-and-disease/heart-health.
Sodium Intake
There is strong and consistent evidence that reducing sodium intake reduces blood pressure. Adults who would benefit from lowering blood pressure should be advised to limit their sodium intake to no more than 2,400 mg per day (about 1 teaspoon of table salt).6 Further reduction of sodium intake to 1,500 mg per day is desirable because it is associated with an even greater reduction in blood pressure. The average blood pressure reduction in patients consuming a sodium-restricted diet of 2,400 mg per day is 2/1 mm Hg, or 7/3 mm Hg for those restricting sodium to 1,500 mg per day.12,13 Reducing baseline sodium intake by at least 1,000 mg per day will lower blood pressure even if the desired daily sodium intake is not yet achieved. Food prepared in restaurants, canned foods, and prepackaged foods (dry or frozen) tend to contain more sodium than home-cooked meals or frozen vegetables.
Physical Activity and Weight Loss
Adults should engage in moderate to vigorous aerobic physical activity three or four times per week for an average of 40 minutes per session to lower blood pressure.6,14 Most health benefits occur with at least 150 minutes per week of moderate-intensity physical activity, such as brisk walking (Table 2).14 Some physical activity is better than none, and more activity results in greater benefits.15 Health benefits of exercise include reduced rates of all-cause mortality, coronary heart disease, hypertension, stroke, type 2 diabetes, metabolic syndrome, colon cancer, breast cancer, and depression.15
Table 2. Examples of Aerobic Exercise

| Aerobic exercise class |
| Bicycling |
| Dancing |
| Gardening or yard work (e.g., raking, pushing a lawn mower) |
| Golfing without using a cart |
| Jogging |
| Moderate-intensity swimming |
| Tennis |
| Walking briskly |
Information from reference 14.
The U.S. Preventive Services Task Force recommends offering or referring overweight and obese adults who have additional cardiovascular risk factors to intensive behavioral counseling interventions to promote a healthy diet and physical activity.16 One way to encourage patients to exercise is to write exercise prescriptions, especially for activities they enjoy.
Weight loss is another important lifestyle modification for reducing blood pressure. Weight loss of approximately 10 kg (22 lb) may reduce systolic blood pressure by 5 to 20 mm Hg.2
Smoking Cessation
Cigarette smoking is the leading preventable cause of death in the United States17 and significantly increases the risk of cardiovascular disease.18 Smoking causes an immediate increase in sympathetic nervous activity, which in turn increases myocardial oxygen demand through increased blood pressure, heart rate, and myocardial contractility.19 A meta-analysis of 20 prospective cohort studies found that quitting smoking after a heart attack or cardiac surgery decreases a patient's risk of death by more than 33% over five years.20 Primary care physicians can use the five A's framework (ask, advise, assess, assist, arrange) to incorporate smoking cessation counseling into their daily practices (Table 3).21
Table 3. Five A's Model for Treating Tobacco Use and Dependence

| Component | Description |
|---|---|
| Ask about tobacco use | Identify and document tobacco use status for every patient at every visit. |
| Advise patient to quit | In a clear, strong, and personalized manner, urge every patient who uses tobacco to quit. |
| Assess willingness to attempt to quit | Is the patient willing to attempt to quit at this time? |
| Assist in quitting | For patients who are willing to attempt to quit, offer medication and provide or refer for counseling or additional treatment. |
| For patients who are unwilling to attempt to quit, provide interventions designed to increase future attempts to quit. | |
| Arrange follow-up | For patients who are willing to attempt to quit, arrange follow-up beginning within the first week after the quit date. |
| For patients who are unwilling to attempt to quit, address tobacco dependence and willingness to quit at next visit. |
Adapted from Fiore MC, Jaén CR, Baker TB, et al.; U.S. Department of Health and Human Services. Treating tobacco use and dependence: 2008 update. http://www.ahrq.gov/professionals/clinicians-providers/guidelines-recommendations/tobacco/clinicians/update/treating_tobacco_use08.pdf. Accessed June 12, 2014.
Alcohol Consumption
Moderate alcohol consumption has been shown to lower blood pressure.2 However, excessive alcohol consumption can raise blood pressure, and persons who do not drink alcohol should not be encouraged to start for the purposes of lowering blood pressure. For potentially beneficial health effects, alcohol consumption should be limited to two drinks per day (about 1 oz or 30 mL of ethanol) for most men and one drink per day for women and lighter-weight men.2,22
Dietary Supplements
Garlic is commonly used as a dietary supplement to lower blood pressure. Data from two randomized controlled trials comparing the use of garlic vs. placebo in patients with hypertension showed that garlic may have some blood pressure–lowering effect.23 However, compared with dietary changes, reduced sodium intake, and physical activity, there is insufficient evidence to support the use of garlic in reducing morbidity or mortality associated with cardiovascular events.
Cocoa has a small but statistically significant blood pressure–lowering effect (average of 2 to 3 mm Hg) in adults with hypertension, but there is no evidence that it improves patient-oriented outcomes in the long term.24
Although vitamin C, coenzyme Q10, omega-3 fatty acids, and magnesium have been used for lowering blood pressure, there is no evidence to support their use in the management of hypertension.
Relaxation Techniques
The mechanism by which relaxation techniques lower blood pressure is unclear. One theory suggests that they may help lower the stress and physiologic arousal produced by the autonomic nervous system, thereby reducing blood pressure. Evidence shows that transcendental meditation may modestly lower blood pressure.15 However, no specific method has been proven beneficial. Because of mixed results in trials and numerous limitations, the AHA does not recommend yoga or acupuncture to lower blood pressure.15 Biofeedback techniques have been proven effective and may be considered in clinical practice to lower blood pressure.15
Self-Measured Blood Pressure Monitoring
A review of 52 trials by the Agency for Healthcare Research and Quality showed that self-measured blood pressure monitoring—with or without additional support such as education, counseling, telemedicine, home visits, or Web-based logging—lowers blood pressure compared with usual care, but effects and long-term benefits beyond 12 months remain uncertain.25 Self-monitoring of blood pressure resulted in a mean reduction in systolic blood pressure of 3.9 mm Hg at six months, and self-monitoring of blood pressure with additional support resulted in a reduction in systolic blood pressure of 2.1 to 8.3 mm Hg, which remained significant at 12 months. Future studies are needed to determine the long-term benefits of self-measured blood pressure monitoring.
Obstructive Sleep Apnea
OSA occurs when the upper airway is repeatedly obstructed during sleep, causing arousals and intermittent hypoxemia. Recent data have shown that it may contribute to poorly controlled high blood pressure.26 International guidelines now recognize OSA as one of the most common risk factors for resistant hypertension.7 The link between OSA and hypertension is likely related to increased sympathetic activity (due to intermittent hypoxia),27 endothelial dysfunction and systemic inflammation,28 and abnormal autonomic function.29
A recent meta-analysis of randomized controlled trials showed that the use of continuous positive airway pressure lowered 24-hour blood pressure levels in persons with resistant hypertension and OSA.30
Data Sources: Essential Evidence Plus, PubMed, the Cochrane Database of Systematic Reviews, U.S. Preventive Services Task Force, and UpToDate were searched using the key terms hypertension and non-pharmacologic with other key terms diet, salt reduction, exercise, weight loss, smoking, obstructive sleep apnea, meditation, alcohol use, and supplements. The search included meta-analyses, randomized controlled trials, clinical trials, guidelines, and reviews. Search dates: May 1, 2014, to June 21, 2014.

