Most of the nearly 4 million births in the United States annually are normal spontaneous vaginal deliveries. In the first stage of labor, normal birth outcomes can be improved by encouraging the patient to walk and stay in upright positions, waiting until at least 6 cm dilation to diagnose active stage arrest, providing continuous labor support, using intermittent auscultation in low-risk deliveries, and following the Centers for Disease Control and Prevention guidelines for group B streptococcus prophylaxis. Most women with a low transverse uterine incision are candidates for a trial of labor after cesarean delivery and should be counseled accordingly. Pain management during labor includes complementary modalities and systemic opioids, epidural anesthesia, and pudendal block. Outcomes in the second stage of labor can be improved by using warm perineal compresses, allowing women more time to push before intervening, and offering labor support. Delayed pushing increases the length of the second stage of labor and does not affect the rate of spontaneous vaginal delivery. A tight nuchal cord can be clamped twice and cut before delivery of the shoulders, or the baby may be delivered using a somersault maneuver in which the cord is left nuchal and the distance from the cord to placenta minimized by pushing the head toward the maternal thigh. After delivery, skin-to-skin contact with the mother is recommended. Beyond 35 weeks' gestation, there is no benefit to bulb suctioning the nose and mouth. Postpartum maternal and neonatal outcomes can be improved through delayed cord clamping, active management to prevent postpartum hemorrhage, careful examination for external anal sphincter injuries, and use of absorbable synthetic suture for second-degree perineal laceration repair. Practices that will not improve outcomes and may result in negative outcomes include discontinuation of epidurals late in labor and routine episiotomy.
Out of the nearly 4 million births in the United States in 2013, approximately 3 million were vaginal deliveries.1 Accurate pregnancy dating is essential for anticipating complications and preparing for delivery. A woman's estimated due date is 40 weeks from the first day of her last menstrual period. If ultrasonography is performed, the due date calculated by the first ultrasound will either confirm or change the due date based on the last menstrual period (Table 1).2 If reproductive technology was used to achieve pregnancy, dating should be based on the timing of embryo transfer.2
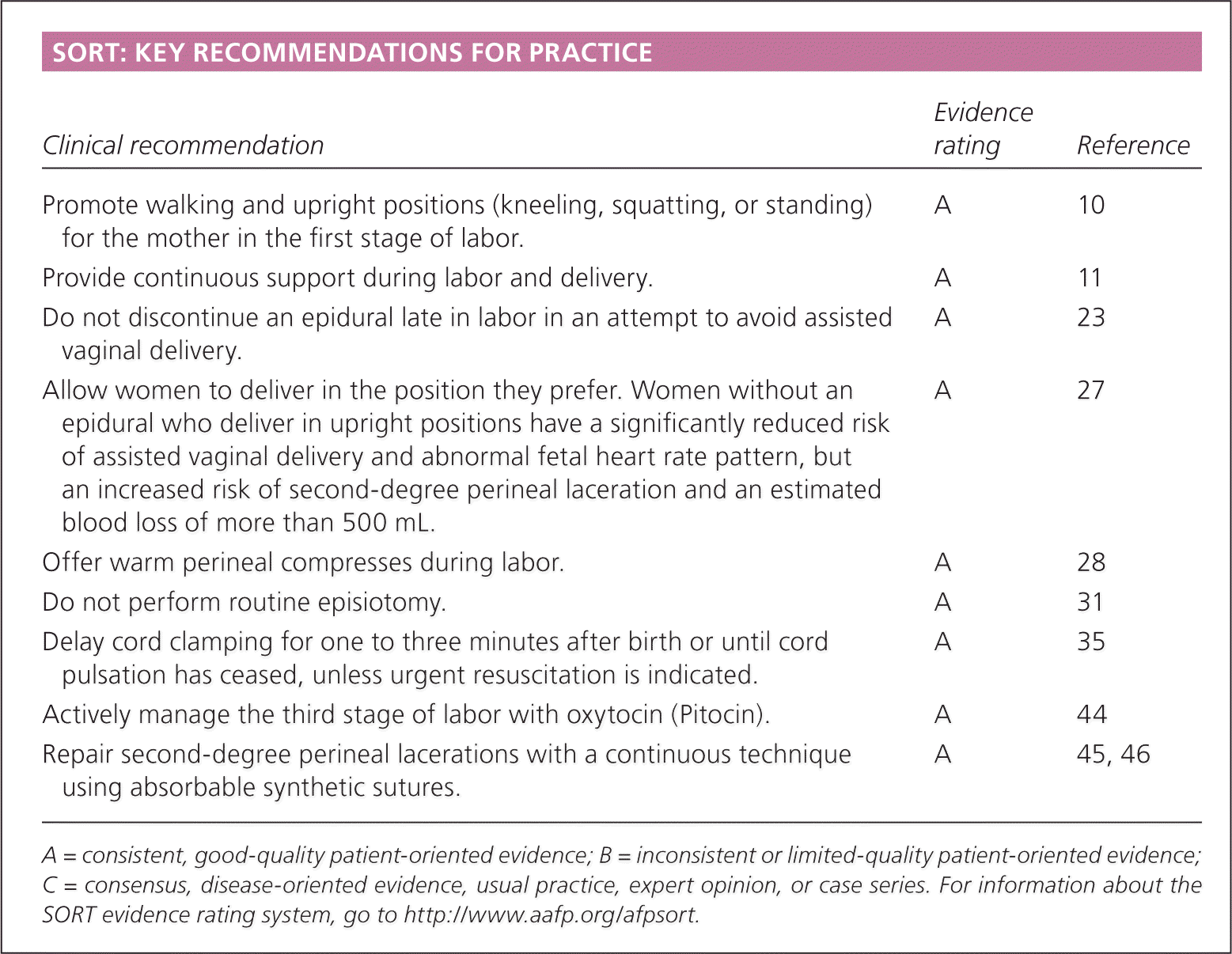
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Reference |
|---|---|---|
| Promote walking and upright positions (kneeling, squatting, or standing) for the mother in the first stage of labor. | A | 10 |
| Provide continuous support during labor and delivery. | A | 11 |
| Do not discontinue an epidural late in labor in an attempt to avoid assisted vaginal delivery. | A | 23 |
| Allow women to deliver in the position they prefer. Women without an epidural who deliver in upright positions have a significantly reduced risk of assisted vaginal delivery and abnormal fetal heart rate pattern, but an increased risk of second-degree perineal laceration and an estimated blood loss of more than 500 mL. | A | 27 |
| Offer warm perineal compresses during labor. | A | 28 |
| Do not perform routine episiotomy. | A | 31 |
| Delay cord clamping for one to three minutes after birth or until cord pulsation has ceased, unless urgent resuscitation is indicated. | A | 35 |
| Actively manage the third stage of labor with oxytocin (Pitocin). | A | 44 |
| Repair second-degree perineal lacerations with a continuous technique using absorbable synthetic sutures. | A | 45, 46 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN MATERNITY CARE: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Don't automatically initiate continuous electronic fetal heart rate monitoring during labor for women without risk factors; consider intermittent auscultation first. | American Academy of Nursing |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Table 1. When to Change Due Date Based on Ultrasound Findings

| Gestational age (weeks) | Difference in estimated due date (days)* |
|---|---|
| ≤ 8 6/7 | 5 |
| 9 0/7 to 15 6/7 | 7 |
| 16 0/7 to 21 6/7 | 10 |
| 22 0/7 to 27 6/7 | 14 |
| ≥ 28 | 21 |
*—If the estimated due date calculated using ultrasonography differs from the estimated due date calculated using the last menstrual period by this many days, the due date can be changed.
Adapted with permission from Committee opinion no 611: method for estimating due date. Obstet Gynecol. 2014;124(4):864.
When describing how a pregnancy is dated, “by last menstrual period” means ultrasonography has not been performed, “by X-week ultrasonography” means that the due date is based on ultrasound findings only, and “by last menstrual period consistent with X-week ultrasound findings” means ultrasonography confirmed the estimated due date calculated using the last menstrual period.
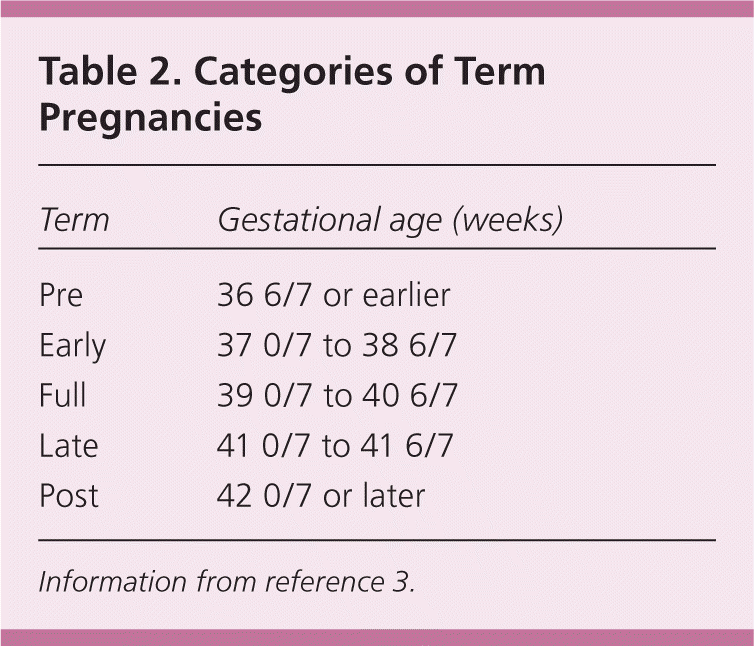
Table 2 defines the classifications of terms of pregnancies.3 Maternity care clinicians can learn more from the American Academy of Family Physicians (AAFP) Advanced Life Support in Obstetrics (ALSO) course (https://www.aafp.org/also). Emergency medical technicians, medical students, and others with limited maternity care experience may benefit from the AAFP Basic Life Support in Obstetrics course (https://www.aafp.org/blso), which offers a module on normal labor and delivery. The Global ALSO manual (https://www.aafp.org/globalalso) provides additional training for normal delivery in low-resource settings.
Table 2. Categories of Term Pregnancies
| Term | Gestational age (weeks) |
|---|---|
| Pre | 36 6/7 or earlier |
| Early | 37 0/7 to 38 6/7 |
| Full | 39 0/7 to 40 6/7 |
| Late | 41 0/7 to 41 6/7 |
| Post | 42 0/7 or later |
Information from reference 3.
Onset of Labor
Labor begins when regular uterine contractions cause progressive cervical effacement and dilation. The risk of infection increases after rupture of membranes, which may occur before or during labor. Induction is recommended for a term pregnancy if the membranes rupture before labor begins.4 Intrapartum antibiotic prophylaxis is indicated if the patient is positive for group B streptococcus at the 35- to 37-week screening or within five weeks of screening if performed earlier in pregnancy, or if the patient has group B streptococcus bacteriuria in the current pregnancy or had a previous infant with group B streptococcus sepsis.5 If the group B streptococcus status is unknown at the time of labor, the patient should receive prophylaxis if she is less than 37 weeks' gestation, the membranes have been ruptured for 18 hours or more, she has a low-grade fever of at least 100.4°F (38°C), or an intrapartum nucleic acid amplification test result is positive.5
The First Stage of Labor
The first stage of labor begins with regular uterine contractions and ends with complete cervical dilation (10 cm). Reanalysis of data from the National Collaborative Perinatal Project (including 39,491 deliveries between 1959 and 1966) and new data from the Consortium on Safe Labor (including 98,359 deliveries between 2002 and 2008) have led to reevaluation of the normal labor curve. Latent labor lasting many hours is normal and is not an indication for cesarean delivery.6–8 Active labor with more rapid dilation may not occur until 6 cm is achieved. Cesarean delivery for failure to progress in active labor is indicated only if the woman is 6 cm or more dilated with ruptured membranes, and she has no cervical change for at least four hours of adequate contractions (more than 200 Montevideo units per intrauterine pressure catheter) or inadequate contractions for at least six hours.8 If possible, the membranes should be ruptured before diagnosing failure to progress. Labor can be significantly longer in obese women.9 Walking, an upright position, and continuous labor support in the first stage of labor increase the likelihood of spontaneous vaginal delivery and decrease the use of regional anesthesia.10,11
Most women who have had a prior cesarean delivery with a low transverse uterine incision are candidates for labor after cesarean delivery (LAC) and should be counseled accordingly.12 A recent AAFP guideline concludes that planned labor and vaginal delivery are an appropriate option for most women with a previous cesarean delivery.13 Women who may want more children should be encouraged to try LAC because the risk of pregnancy complications increases with increasing number of cesarean deliveries.12 The risk of uterine rupture with cesarean delivery is less than 1%, and the risk of the infant dying or having permanent brain injury is approximately one in 2,000 (the same as for vaginal delivery in primiparous women).14 Based on the clinical scenario, women with two prior cesarean deliveries may also try LAC.12 Contraindications to vaginal delivery are outlined in Table 3.
Table 3. Contraindications to Vaginal Delivery

| Active herpes simplex lesions or prodromal (warning) symptoms |
| Certain malpresentations (e.g., nonfrank breech, transverse, face with mentum posterior) [corrected] |
| Complete placenta previa |
| Previous vertical uterine incision or transfundal uterine surgery |
| The mother does not wish to have vaginal birth after cesarean delivery |
In low-risk deliveries, intermittent auscultation by handheld Doppler ultrasonography has advantages over continuous electronic fetal monitoring. Although continuous electronic fetal monitoring is associated with a decrease in the rare outcome of neonatal seizures, it is associated with an increase in cesarean and assisted vaginal deliveries with no other improvement in neonatal outcomes.15 When electronic fetal monitoring is employed, the National Institute of Child Health and Human Development definitions and categories should be used (Table 4).16
Table 4. Tracing Categories for Electronic Fetal Monitoring

| Category | Description | |
|---|---|---|
| 1 | Normal baseline (110 to 160 beats per minute), moderate variability and no variable or late decelerations (accelerations may or may not be present) | |
| 2 | Anything that is not a category 1 or 3 tracing | |
| 3 | Absent variability in the presence of recurrent variable decelerations, recurrent late decelerations or bradycardia | |
| or | ||
| Sinusoidal pattern | ||
Information from reference 16.
Pain management includes nonpharmacologic and pharmacologic methods.17 Nonpharmacologic approaches include acupuncture and acupressure18; other complementary and alternative therapies, including audioanalgesia, aromatherapy, hypnosis, massage, and relaxation techniques19; sterile water injections17; continuous labor support11; and immersion in water.20 Pharmacologic analgesia includes systemic opioids, nitrous oxide, epidural anesthesia, and pudendal block.17,21 Although epidurals provide better pain relief than systemic opioids, they are associated with a significantly longer second stage of labor; an increased rate of oxytocin (Pitocin) augmentation; assisted vaginal delivery; and an increased risk of maternal hypotension, urinary retention, and fever.22 Cesarean delivery for abnormal fetal heart tracings is more common in women with epidurals, but there is no significant difference in overall cesarean delivery rates compared with women who do not have epidurals.22 Discontinuing an epidural late in labor does not increase the likelihood of vaginal delivery and increases inadequate pain relief.23
The Second Stage of Labor
The second stage begins with complete cervical dilation and ends with delivery. The fetal head comes below the pubic symphysis and then extends. Pushing can begin once the cervix is fully dilated. Although delayed pushing or “laboring down” shortens the duration of pushing, it increases the length of the second stage and does not affect the rate of spontaneous vaginal delivery.24 Arrest of the second stage of labor is defined as no descent or rotation after two hours of pushing for a multiparous woman without an epidural, three hours of pushing for a multiparous woman with an epidural or a nulliparous woman without an epidural, and four hours of pushing for a nulliparous woman with an epidural.8 A prolonged second stage in nulliparous women is associated with chorioamnionitis and neonatal sepsis in the newborn.25
If the fetus is in the occipitotransverse or occipitoposterior position in the second stage, manual rotation to the occipitoanterior position decreases the likelihood of operative vaginal and cesarean delivery.26 Fetal position can be determined by identifying the sagittal suture with four suture lines by the anterior (larger) fontanelle and three by the posterior fontanelle. The position of the ears can also be helpful in determining fetal position when a large amount of caput is present and the sutures are difficult to palpate. Bedside ultrasonography is helpful when position is unclear by examination findings.
Women may push in any position that they prefer. Potential positions include on the back, side, or hands and knees; standing; or squatting. Women without epidurals who deliver in upright positions (kneeling, squatting, or standing) have a significantly reduced risk of assisted vaginal delivery and abnormal fetal heart rate pattern, but an increased risk of second-degree perineal laceration and an estimated blood loss of more than 500 mL.27 Flexing the hips and legs increases the pelvic inlet diameter, allowing more room for delivery.
Second stage warm perineal compresses have been associated with a reduction in third- and fourth-degree perineal lacerations.28 Studies have not shown benefit to keeping hands on vs. hands off the fetal head and maternal perineum during delivery.29 Although not well studied, shorter pushes as the head is crowning are encouraged by many clinicians in an attempt to decrease perineal lacerations. Also, delivering between contractions may decrease perineal lacerations.30 Routine episiotomy should not be performed. Episiotomy is associated with more severe perineal trauma, increased need for suturing, and more healing complications.31
Once the infant's head is delivered, the clinician can check for a nuchal cord. The cord may be wrapped around the neck one or more times. If the nuchal cord is loose, it can be gently pulled over the head if possible or left in place if it does not interfere with delivery. A tight nuchal cord can be clamped twice and cut before delivery of the shoulders, although this may be associated with increased neonatal complications, including hypovolemia, anemia, shock, hypoxic-ischemic encephalopathy, cerebral palsy, and death according to case reports. The tight nuchal cord itself may contribute to some of these outcomes, however.32 Another option for a tight nuchal cord is the somersault maneuver (carefully delivering the anterior and posterior shoulder, and then delivering the body by somersault while the head is kept next to the maternal thigh). After delivery, the cord can be removed from the neck.32 A video of the somersault maneuver is available at https://www.youtube.com/watch?v=WaJ6sZ4nfnQ. More research on the safety and effectiveness of this maneuver is needed.
After delivery of the head, gentle downward traction should be applied with one gloved hand on each side of the fetal head to facilitate delivery of the shoulders. After the anterior shoulder delivers, the clinician pulls up gently, and the rest of the body should deliver easily. The vigorous newborn should be placed directly in contact with the mother's skin and covered with a blanket. Skin-to-skin contact is associated with decreased time to the first feeding, improved breastfeeding initiation and continuation, higher blood glucose level, decreased crying, and decreased hypothermia.33 After delivery, quick drying of the newborn helps prevent hypothermia and stimulates crying and breathing. Beyond 35 weeks' gestation, there is no benefit to bulb suctioning the nose and mouth; earlier gestational ages have not been studied.34
Delayed cord clamping, defined as waiting to clamp the umbilical cord for one to three minutes after birth or until cord pulsation has ceased, is associated with benefits in term infants, including higher birth weight, higher hemoglobin concentration, improved iron stores at six months, and improved respiratory transition.35 Benefits are even greater with preterm infants.36 However, delayed cord clamping is associated with an increase in jaundice requiring phototherapy.35 Delayed cord clamping is indicated with all deliveries unless urgent resuscitation is needed. It is not necessary to keep the newborn below the level of the placenta before cutting the cord.37 The cord should be clamped twice, leaving 2 to 4 cm of cord between the newborn and the closest clamp, and then the cord is cut between the clamps.
The Third Stage of Labor
The third stage begins after delivery of the newborn and ends with the delivery of the placenta. The average length of the third stage of labor is eight to nine minutes.38
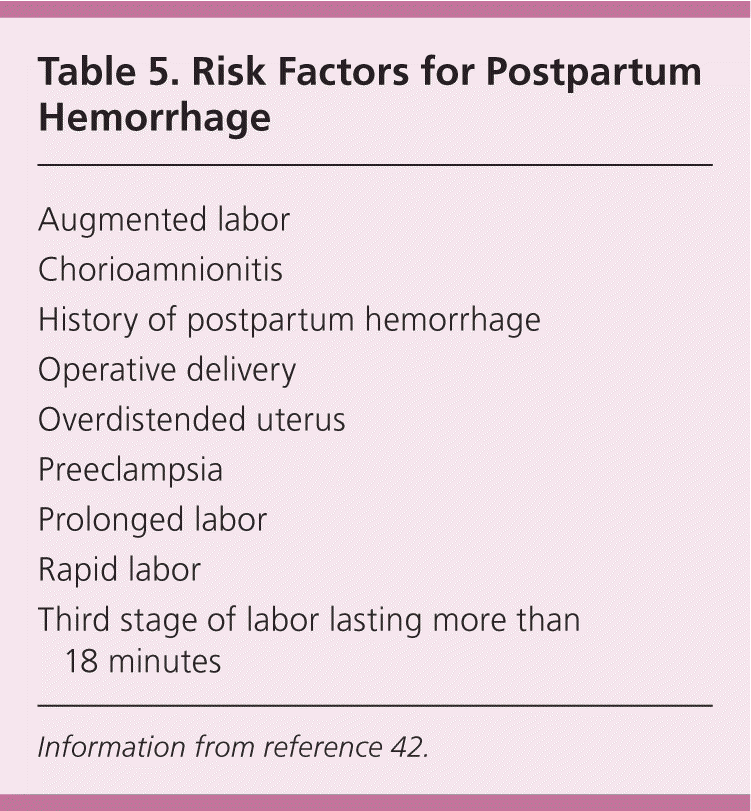
The greatest risk in the third stage is postpartum hemorrhage, which was recently redefined as 1,000 mL or more of blood loss or signs and symptoms of hypovolemia.39 The median blood loss with vaginal delivery is 574 mL.40 Blood loss is often underestimated by as much as 30%, and underestimation increases with increasing blood loss.41 The risk of hemorrhage increases after 18 minutes and is six times greater after 30 minutes.38 Postpartum hemorrhage is most commonly caused by atony (70% of cases).42 Other causes include vaginal or cervical lacerations, uterine inversion, retained products of conception, and coagulopathy.42 Table 5 lists risk factors for postpartum hemorrhage.42
Table 5. Risk Factors for Postpartum Hemorrhage
| Augmented labor |
| Chorioamnionitis |
| History of postpartum hemorrhage |
| Operative delivery |
| Overdistended uterus |
| Preeclampsia |
| Prolonged labor |
| Rapid labor |
| Third stage of labor lasting more than 18 minutes |
Information from reference 42.
Active management of the third stage of labor (AMTSL), which is recommended by the World Health Organization,43 is associated with a reduction in the risk of hemorrhage, both greater than 500 mL and greater than 1,000 mL, maternal hemoglobin level of less than 9 g per dL (90 g per L) after delivery, need for maternal blood transfusion, and need for more uterotonics in labor or in the first 24 hours after delivery.44 However, AMTSL is also associated with an increase in postpartum maternal diastolic blood pressure, emesis, and use of analgesia and a decrease in neonatal birth weight.44 Although AMTSL has traditionally consisted of oxytocin (10 IU intramuscularly or 20 IU per L intravenously at 250 mL per hour) and early cord clamping, the most important component now appears to be the administration of oxytocin.43,44 Early cord clamping is no longer a component because it does not decrease postpartum hemorrhage and may be associated with neonatal harm.35,44 Delayed cord clamping may avoid interfering with early transplacental transfusion and avoid the increase in maternal blood pressure and decrease in fetal weight associated with traditional AMTSL.44 More research is needed regarding the effects of individual components of AMTSL.44
Cervical, vaginal, and perineal lacerations should be repaired if there is bleeding. Second-degree laceration repairs are best performed in a continuous manner with absorbable synthetic suture. Compared with interrupted sutures, continuous repair of second-degree perineal lacerations is associated with less analgesia use, less short-term pain, and less need for suture removal.45 Compared with catgut (chromic) sutures, synthetic sutures (polyglactin 910 [Vicryl], polyglycolic acid [Dexon]) are associated with less pain, less analgesia use, and less need for resuturing. However, synthetic sutures are associated with increased need for unabsorbed suture removal.46
There are no quality randomized controlled trials assessing repair vs. nonrepair of second-degree perineal lacerations.47 External anal sphincter injuries are often unrecognized, which can lead to fecal incontinence.48 Knowledge of perineal anatomy and careful visual and digital examination can increase external anal sphincter injury detection.48
Data Sources: A PubMed search was completed in Clinical Queries using key terms including labor and obstetric, delivery and obstetric, labor stage and first, labor stage and second, labor stage and third, doulas, anesthesia and epidural, and postpartum hemorrhage. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. We also searched the Cochrane database, Essential Evidence Plus, the National Guideline Clearinghouse database, and the U.S. Preventive Services Task Force. Search dates: September 4, 2014, and April 23, 2015.
This article is one in a series on “Advanced Life Support in Obstetrics (ALSO),” initially established by Mark Deutchman, MD, Denver, Colo. The coordinator of this series is Larry Leeman, MD, MPH, ALSO Managing Editor, Albuquerque, N.M.

