Family physicians are often a source of information and advice on early childhood concerns regarding sleep, thumb-sucking/pacifier use, picky eating, school readiness, and oral health. Evidence indicates that family variables are important in the genesis of sleep difficulties, and that traditional behavioral methods are not as effective as previously thought. Attention to family psychosocial well-being, especially maternal functioning, is important in addressing childhood sleep difficulties. Thumb-sucking and pacifier use may be associated with negative consequences if they persist, and referral is recommended after four years of age if appropriate behavioral interventions are ineffective. Picky eating is heavily influenced by environmental factors, and food neophobia is a normal stage of development. The main approaches to childhood eating problems include social modeling of normal eating behaviors, repeated exposures to new foods, and positive mealtime experiences. School readiness focuses on supporting the psychosocial variables that are associated with school success. Reading with the child enhances literacy skills. Quality early childhood education programs are also effective in enhancing school success. Delaying school entry is not beneficial and may be detrimental. School readiness includes the schools' role in supporting the learning needs of all children regardless of their abilities and skills. Oral health is increasingly recognized as an important contributor to overall health. Oral health should be incorporated into well-child visits beginning at the eruption of the first tooth.
Early childhood concerns often represent individual variations of normal development. A number of factors, including family dynamics, cultural expectations, and family resources, determine whether these issues are seen as problematic. Normal variations may sometimes deviate into abnormalities that can affect future health if not addressed. Providing families with the available evidence regarding these issues is often helpful to patients and the entire family unit.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Parental education about sleep and sleep schedules, bedtime routines, and acquisition of self-soothing skills are effective in improving sleep problems and nighttime awakenings in children. | C | 18 |
| Children older than four years who suck their thumbs despite appropriate behavioral interventions should be referred to a pediatric dentist. | C | 36 |
| Delaying school enrollment by one or more years is not beneficial and may be associated with increased rates of behavioral problems. | C | 44, 47 |
| In children five years and younger, fluoride varnish should be applied periodically to primary teeth as soon as they erupt. Application once per year has comparable effectiveness to application every six months. | B | 49, 50 |
| Starting at six months of age, oral fluoride supplementation is recommended in communities with insufficient fluoride in the water supply (less than 0.6 ppm). | B | 49, 50 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Sleep Issues
During infancy, sleep awakenings are normal as infants transition from short sleep cycles with multiple awakenings to a normal sleep pattern in which most sleep occurs at night. Approximately two-thirds of children progress steadily to a normal sleep pattern with infrequent disruptive night awakenings.1 One study found that by six months of age most infants (58%) were waking up in the middle of the night twice a week or less.2 However, in the first three years of life, 10% to 30% of healthy children have sleep patterns that unacceptably disrupt caretaker and family functioning.3–5 These patterns include bedtime struggles, prolonged sleep onset latency, sleep interruptions, and shortened sleep durations.
Difficult temperament, illness, and developmental problems (e.g., autism spectrum disorders) in a child are strongly associated with reported sleep problems.6–8 Sleep problems have also been associated with family discord, low socioeconomic status, ethnicity, and maternal sensitivity and mental health problems, although the reason is unclear.9–13 International surveys point to cultural and environmental factors as additional influences on childhood sleep patterns.14–16
The National Sleep Foundation recommends the following daily sleep durations for healthy children: 14 to 17 hours for newborns, 12 to 15 hours for infants, 11 to 14 hours for toddlers, and 10 to 13 hours for preschoolers.17
Parental education about sleep and sleep schedules, bedtime routines, and acquisition of self-soothing skills are effective in improving sleep problems and nighttime awakenings in children.18 To reduce bedtime problems and nighttime awakenings, thereby improving caretaker well-being and the child's daytime functioning, the American Academy of Sleep Medicine recommends that caretakers implement behavioral interventions for children through four years of age.18 These interventions include unmodified extinction (caretaker leaves the child to “cry it out” in his or her crib), modified or graduated extinction (caretaker gradually withdraws from the child's room), and initiation of bedtime schedules and routines. There is insufficient evidence to support one intervention, or a combination, over others.18
A meta-analysis concluded that behavioral interventions in the first six months of life do not decrease crying, prevent behavioral or sleep problems in infants, or reduce maternal depression. In addition, unintended outcomes of behavioral interventions in this age group may include increased infant crying, increased maternal anxiety, and premature termination of breastfeeding.19 Additionally, the feasibility and acceptability of these behavioral interventions to parents have not been rigorously assessed.20
Although sleep problems among young children can be stressful for families, family physicians can educate concerned parents and reassure them that some sleep issues are a normal part of development. However, physicians should also identify any concerns for abuse; explore underlying conditions, including postpartum depression; and provide sources of additional support to families experiencing excessive stress. Table 1 summarizes sleep interventions for infants.18
Table 1. Sleep Interventions for Infants
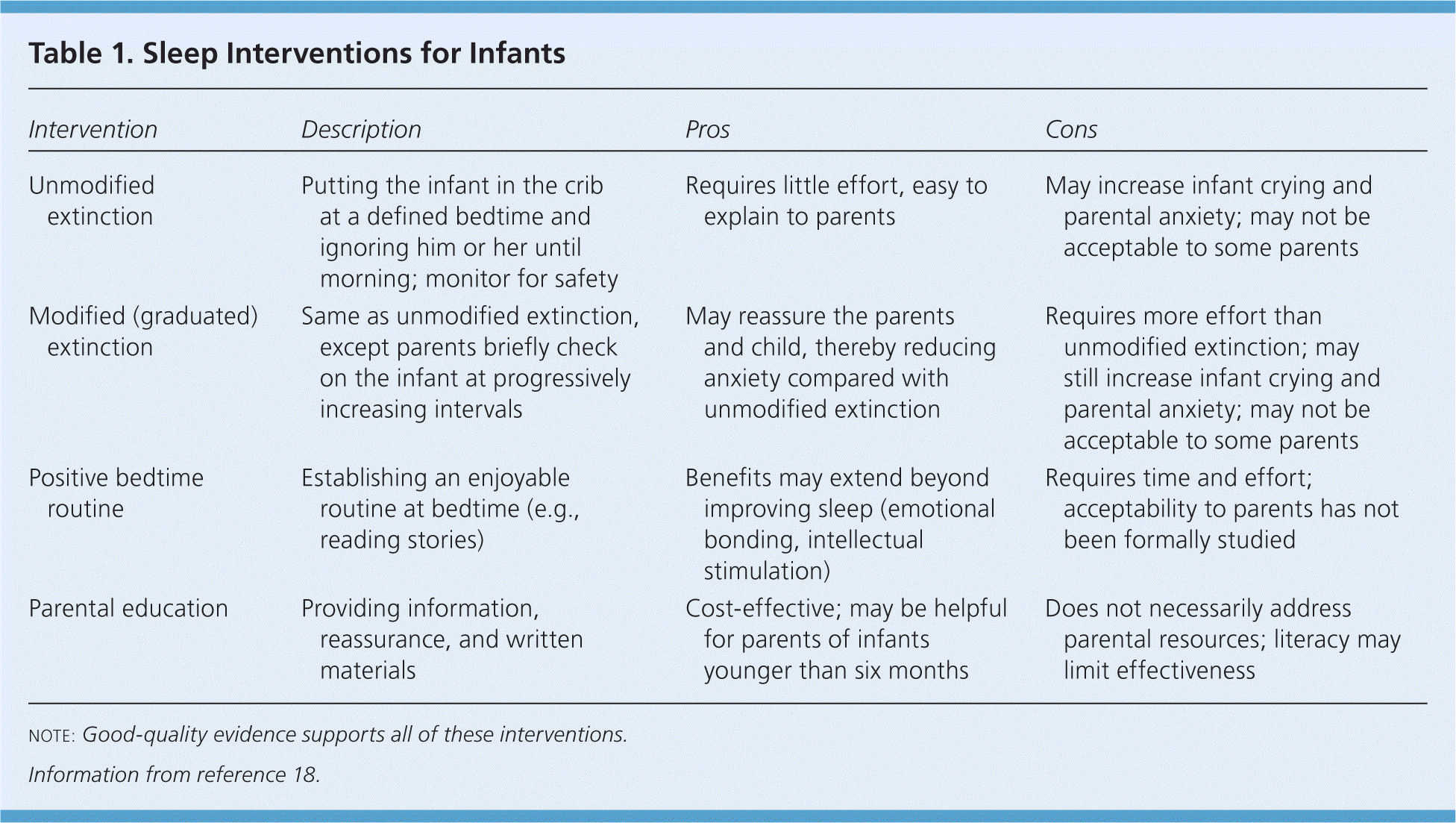
| Intervention | Description | Pros | Cons |
|---|---|---|---|
| Unmodified extinction | Putting the infant in the crib at a defined bedtime and ignoring him or her until morning; monitor for safety | Requires little effort, easy to explain to parents | May increase infant crying and parental anxiety; may not be acceptable to some parents |
| Modified (graduated) extinction | Same as unmodified extinction, except parents briefly check on the infant at progressively increasing intervals | May reassure the parents and child, thereby reducing anxiety compared with unmodified extinction | Requires more effort than unmodified extinction; may still increase infant crying and parental anxiety; may not be acceptable to some parents |
| Positive bedtime routine | Establishing an enjoyable routine at bedtime (e.g., reading stories) | Benefits may extend beyond improving sleep (emotional bonding, intellectual stimulation) | Requires time and effort; acceptability to parents has not been formally studied |
| Parental education | Providing information, reassurance, and written materials | Cost-effective; may be helpful for parents of infants younger than six months | Does not necessarily address parental resources; literacy may limit effectiveness |
note: Good-quality evidence supports all of these interventions.
Information from reference 18.
Thumb-Sucking and Pacifier Use
Nonnutritive sucking habits such as thumb- and finger-sucking and pacifier use are prevalent among children in all parts of the world and in all socioeconomic classes.21–24 In most cases, the habits cease spontaneously between two and four years of age. However, persistence of these oral habits can lead to negative consequences, such as koilonychia (deformity of the nail), paronychia, and dental malocclusion.25–27 Behavioral interventions for these habits include aversive conditioning by applying a bad-tasting substance (e.g., Thum Liquid), or positive reinforcement when the child avoids the habit.28,29
Pacifier use is associated with a reduced incidence of sudden infant death syndrome in infants younger than six months,30 although the cause-effect relationship is unclear. However, pacifier use may also be associated with recurrent otitis media and increases in wheezing, cough, and diarrhea.31 American Academy of Pediatrics guidelines acknowledge that reducing or eliminating pacifier use after six months of age may reduce otitis media.32 Pacifier use is also a stronger risk factor for dental malocclusion than is thumb- or finger-sucking among older children.33–35
Referral to a pediatric dentist should be considered if nonnutritive sucking habits persist beyond about four years of age despite appropriate behavioral interventions. The use of preventive orthodontics for thumb-sucking may be a cost-effective way of preventing malocclusion in these children.36
Picky Eating
Parents often describe their toddlers and preschoolers as picky eaters. The reluctance to eat or try new foods (food neophobia) is a normal developmental stage that the child usually outgrows. However, there are picky or fussy eaters who restrict their intake to only a few food items, regardless of whether they are new or familiar.37
Picky eaters tend to consume more sweetened foods and foods with high carbohydrate content.38 Children with sensory defensiveness such as those with autism spectrum disorders are more likely to be picky eaters. Picky or fussy eating is heavily influenced by environmental factors (e.g., parent behaviors, such as offering limited food choices).
The main approaches to picky eating include social modeling of normal eating behaviors, repeated exposures to new foods, and positive mealtime experiences.39 There is a strong correlation between parent and child nutritional behaviors.40 Parental efforts to control the child's intake of food using pressure to eat a certain food or quantity of food, restriction of certain foods, or promise of a reward have negative effects on food acceptance and are discouraged.41 In the Satters' Division of Responsibility Model, the parents' role is to provide mealtime structure, positive social modeling, and a variety of healthy foods, whereas the child decides how much and which foods to eat (Table 2).42,43
Table 2. Satters' Division of Responsibility Model: Mealtime Roles for Parents and Children

| Parents |
| Provide mealtime structure: time and place |
| Create a positive environment: pleasant interaction |
| Allow the child to feed himself or herself |
| Provide a variety of healthy foods |
| Children |
| Eat if he or she wants to |
| Choose what to eat out of the offered foods |
| Stop eating when full |
School Readiness
The concept of school readiness has been informed by the knowledge of early brain development and includes psychosocial constructs that influence academic and school success. Schools are required to support the educational needs of all children regardless of their skills or abilities.
Family psychosocial risk factors and the child's social and emotional development are more predictive of school success than academic milestones.44 The family environment plays a critical role in providing positive early childhood experiences. The family physician can screen for psychosocial risk factors, such as family turmoil or abuse, and provide referral to support services. Additionally, surveillance of the child's physical, emotional, and behavioral health and development (e.g., ability to follow instructions and pay attention), and early interventions may be beneficial.
Reading to children starting at an early age has been shown to enhance language development and literacy skills.45 Similarly, enrollment in quality preschool programs has been shown to improve school outcomes.46 Delaying school enrollment by one or more years to allow children to mature or to attain more skills is not beneficial and may be associated with increased rates of behavioral problems.44,47
Oral Health
Oral health is increasingly recognized as a significant contributor to overall health. The family physician is an important advocate for oral health and can incorporate oral health into well-child visits.
The American Academy of Pediatrics and the American Academy of Pediatric Dentistry recommend the integration of oral health prevention into health care maintenance at the time of first tooth eruption. Parents should limit their children's juice intake to 4 to 6 oz per day given in a cup at mealtimes, not give carbonated beverages to children, not put children to bed with a bottle containing anything but water, and brush children's teeth twice daily with fluoridated toothpaste.48
No more than a rice-sized amount of toothpaste should be used for infants and children younger than three years, and no more than a pea-sized amount should be used for children up to six years of age.48 In addition, the periodic application of fluoride varnish is recommended at first tooth eruption in children five years and younger; application once per year has comparable effectiveness to application every six months.49,50 Oral fluoride supplementation starting at six months of age is recommended if the community water supply is fluoride deficient (less than 0.6 ppm). Referral to a dentist to establish a dental home is recommended toward the end of the first year of life.49,50 Table 3 summarizes U.S. Preventive Services Task Force recommendations for oral health screening in young children.50
Table 3. U.S. Preventive Services Task Force Recommendations for Oral Health in Children Five Years and Younger

| Oral fluoride supplementation is recommended for children starting at six months of age who live in communities with less than 0.6 ppm of fluoride in the water supply. |
| Fluoride varnish is recommended starting at the eruption of the first primary tooth through five years of age. Application once per year has comparable effectiveness to application every six months. |
| There is insufficient evidence to support routine oral screening examination by primary care clinicians. |
Information from reference 50.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms thumb-sucking, malocclusion, pacifier use, infant sleep problems, picky eating, school readiness, and pediatric oral health. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cochrane database and the National Guideline Clearinghouse. Search dates: November 1, 2014, to February 12, 2015.
NOTE: This review updates a previous article on early childhood issues by Drs. Tseng and Biagioli.

