Sexual dysfunction in women is a common and often distressing problem that has a negative impact on quality of life and medication compliance. The problem is often multifactorial, necessitating a multidisciplinary evaluation and treatment approach that addresses biological, psychological, sociocultural, and relational factors. Criteria for sexual interest/arousal disorder require the presence of at least three specific symptoms lasting for at least six months. Lifelong anorgasmia may suggest the patient is unfamiliar or uncomfortable with self-stimulation or sexual communication with her partner. Delayed or less intense orgasms may be a natural process of aging due to decreased genital blood flow and dulled genital sensations. Genito-pelvic pain/penetration disorder includes fear or anxiety, marked tightening or tensing of the abdominal and pelvic muscles, or actual pain associated with attempts toward vaginal penetration that is persistent or recurrent for at least six months. Treatment depends on the etiology. Estrogen is effective for the treatment of dyspareunia associated with genitourinary syndrome of menopause. Testosterone, with and without concomitant use of estrogen, is associated with improvements in sexual functioning in naturally and surgically menopausal women, although data on long-term risks and benefits are lacking. Bupropion has been shown to improve the adverse sexual effects associated with antidepressant use; however, data are limited. Psychotherapy or sex therapy is useful for management of the psychological, relational, and sociocultural factors impacting a woman's sexual function. Clinicians can address many of these issues in addition to providing education and validating women's sexual health concerns.
Female sexual dysfunction is a general term comprising several sexual health concerns that can be distressing for patients, including female sexual interest/arousal disorder, female orgasmic disorder, and genito-pelvic pain/penetration disorder. These sexual health concerns are not considered dysfunctions unless they cause distress. About 12% of women in the United States report distressing sexual health concerns, although as many as 40% report sexual concerns overall.1
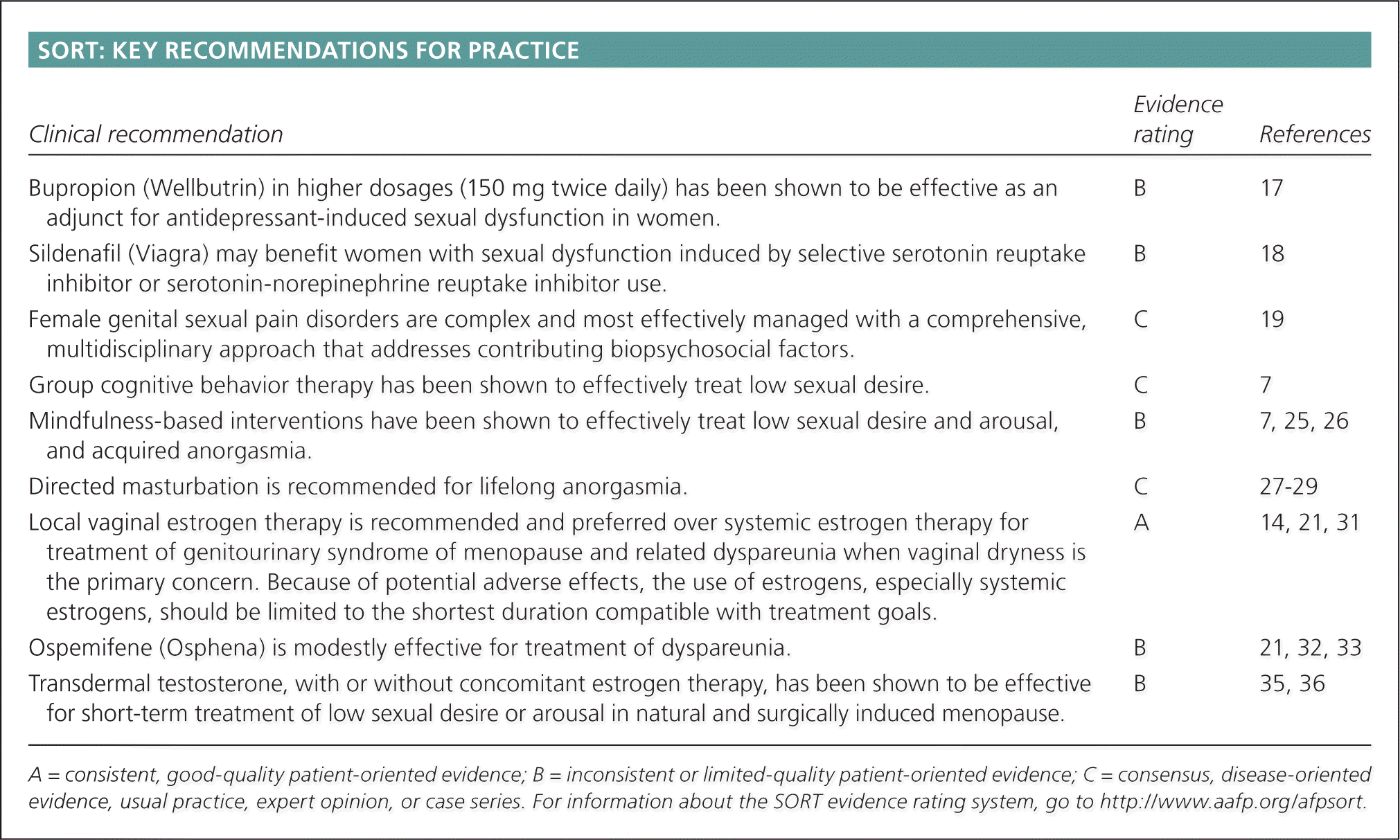
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Bupropion (Wellbutrin) in higher dosages (150 mg twice daily) has been shown to be effective as an adjunct for antidepressant-induced sexual dysfunction in women. | B | 17 |
| Sildenafil (Viagra) may benefit women with sexual dysfunction induced by selective serotonin reuptake inhibitor or serotonin-norepinephrine reuptake inhibitor use. | B | 18 |
| Female genital sexual pain disorders are complex and most effectively managed with a comprehensive, multidisciplinary approach that addresses contributing biopsychosocial factors. | C | 19 |
| Group cognitive behavior therapy has been shown to effectively treat low sexual desire. | C | 7 |
| Mindfulness-based interventions have been shown to effectively treat low sexual desire and arousal, and acquired anorgasmia. | B | 7, 25, 26 |
| Directed masturbation is recommended for lifelong anorgasmia. | A [ | 27–29 |
| Local vaginal estrogen therapy is recommended and preferred over systemic estrogen therapy for treatment of genitourinary syndrome of menopause and related dyspareunia when vaginal dryness is the primary concern. Because of potential adverse effects, the use of estrogens, especially systemic estrogens, should be limited to the shortest duration compatible with treatment goals. | A | 14, 21, 31 |
| Ospemifene (Osphena) is modestly effective for treatment of dyspareunia. | B | 21, 32, 33 |
| Transdermal testosterone, with or without concomitant estrogen therapy, has been shown to be effective for short-term treatment of low sexual desire or arousal in natural and surgically induced menopause. | B | 35, 36 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Etiology and Pathophysiology
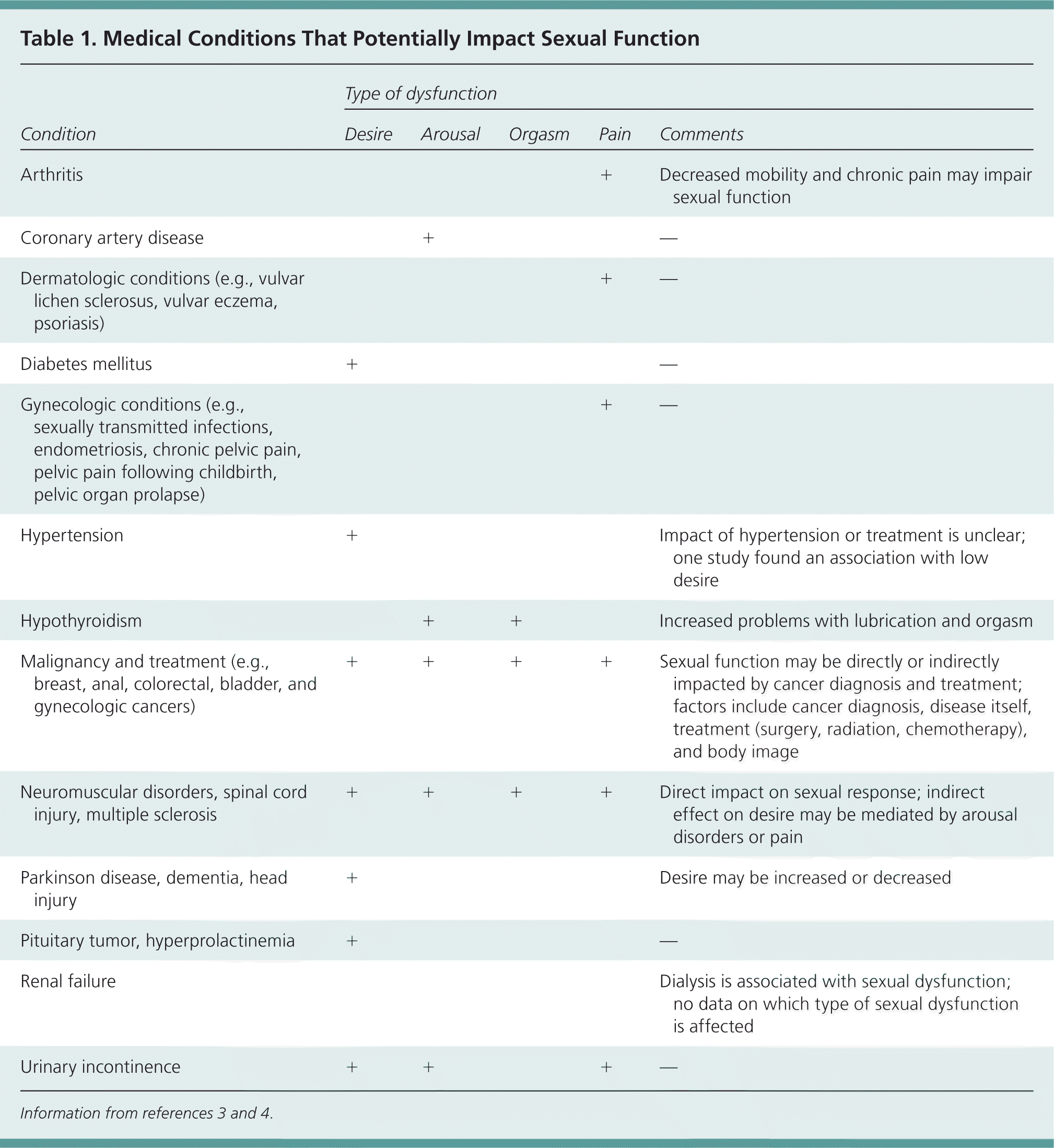
The etiology of female sexual dysfunction is multifactorial, encompassing biological, psychological, relational, and sociocultural factors.2 Biological factors may impact sexual function in a variety of ways. Some chronic illnesses, such as vascular disease, diabetes mellitus, neurologic disease, and malignancy, can directly or indirectly impact sexual function (Table 1).3,4 Aging itself is associated with decreased sexual responsiveness, sexual activity, and libido.4,5
Table 1. Medical Conditions That Potentially Impact Sexual Function
| Condition | Type of dysfunction | ||||
|---|---|---|---|---|---|
| Desire | Arousal | Orgasm | Pain | Comments | |
| Arthritis | + | Decreased mobility and chronic pain may impair sexual function | |||
| Coronary artery disease | + | — | |||
| Dermatologic conditions (e.g., vulvar lichen sclerosus, vulvar eczema, psoriasis) | + | — | |||
| Diabetes mellitus | + | — | |||
| Gynecologic conditions (e.g., sexually transmitted infections, endometriosis, chronic pelvic pain, pelvic pain following childbirth, pelvic organ prolapse) | + | — | |||
| Hypertension | + | Impact of hypertension or treatment is unclear; one study found an association with low desire | |||
| Hypothyroidism | + | + | Increased problems with lubrication and orgasm | ||
| Malignancy and treatment (e.g., breast, anal, colorectal, bladder, and gynecologic cancers) | + | + | + | + | Sexual function may be directly or indirectly impacted by cancer diagnosis and treatment; factors include cancer diagnosis, disease itself, treatment (surgery, radiation, chemotherapy), and body image |
| Neuromuscular disorders, spinal cord injury, multiple sclerosis | + | + | + | + | Direct impact on sexual response; indirect effect on desire may be mediated by arousal disorders or pain |
| Parkinson disease, dementia, head injury | + | Desire may be increased or decreased | |||
| Pituitary tumor, hyperprolactinemia | + | — | |||
| Renal failure | Dialysis is associated with sexual dysfunction; no data on which type of sexual dysfunction is affected | ||||
| Urinary incontinence | + | + | + | — | |
Hormonal changes occurring in midlife may impact a woman's sexual function. Menopause is marked by a decline in ovarian hormone levels, which occurs gradually in natural menopause but may be sudden if menopause occurs because of surgery, radiation, or chemotherapy. Decreased vaginal lubrication and dyspareunia are associated with low estradiol levels; however, the association between low sexual desire and lower estradiol levels has been inconsistent. Testosterone levels do not correlate with female sexual function or overall well-being, possibly because of the difficulty in accurately measuring free and total testosterone levels at the lower end of the female range.4 Although androgens are positively associated with improvements in all aspects of sexual functioning (e.g., subjective arousal, vaginal blood flow, sexual desire, orgasm), there is no lower level of testosterone that predicts sexual dysfunction, and androgen levels are not used to define an androgen deficiency syndrome in women.
Serotonin-enhancing medications have an inhibitory effect on sexual function. Sexual dysfunction induced by selective serotonin reuptake inhibitor use is common, with an incidence between 30% and 70%, and may include difficulty with sexual desire, arousal, and orgasm.4 Further, many other commonly prescribed medications may adversely affect sexual functioning, including antiestrogens, such as tamoxifen and aromatase inhibitors, and oral estrogens, including combined hormonal contraception (Table 2).6 [corrected]
Table 2. Medications Associated with Female Sexual Dysfunction

| Type of dysfunction | ||||
|---|---|---|---|---|
| Medication | Desire disorder | Arousal disorders | Orgasm disorders | |
| Amphetamines and related anorectic medications | + | |||
| Anticholinergics | + | |||
| Antihistamines | + | |||
| Cardiovascular and antihypertensive medications | ||||
| Antilipids | + | |||
| Beta blockers | + | |||
| Clonidine | + | + | ||
| Digoxin | + | + | ||
| Methyldopa | + | |||
| Spironolactone | + | |||
| Hormonal preparations | ||||
| Antiandrogens | + | + | + | |
| Danazol | + | |||
| Gonadotropin-releasing hormone agonists | + | |||
| Gonadotropin-releasing hormone analogues | + | + | ||
| Hormonal contraceptives | + | |||
| Tamoxifen | + | + | ||
| Ultra-low-potency contraceptives | + | + | ||
| Narcotics | + | |||
| Psychotropics | ||||
| Antipsychotics | + | + | ||
| Barbiturates | + | + | + | |
| Benzodiazepines | + | + | ||
| Lithium | + | + | + | |
| Monoamine oxidase inhibitors | ||||
| Selective serotonin reuptake inhibitors | + | + | + | |
| Trazodone | + | |||
| Tricyclic antidepressants | + | + | + | |
| Venlafaxine | + | |||
| Other | ||||
| Aromatase inhibitors | + | + | ||
| Chemotherapeutic agents | + | + | ||
| Histamine H2 blockers and promotility agents | + | |||
| Indomethacin | + | |||
| Ketoconazole | + | |||
| Phenytoin (Dilantin) | + | |||
Adapted with permission from Buster JE. Managing female sexual dysfunction. Fertil Steril. 2013;100(4)905-915.
The most common psychological factors impacting female sexual function are depression, anxiety, distraction, negative body image, sexual abuse, and emotional neglect. Common contextual or sociocultural factors that cause or maintain sexual dysfunction include relationship discord, partner sexual dysfunction (e.g., erectile dysfunction), life stage stressors (e.g., transition into retirement, children leaving home), and cultural or religious messages that inhibit sexuality.7
Evaluation
Assessment of female sexual dysfunction is best approached using a biopsychosocial model (eFigure A), and should include a sexual history and physical examination. Laboratory testing is usually not needed to identify causes of sexual dysfunction.8 Table 3 includes important questions to ask patients during a sexual functioning assessment.8
eFigure A.
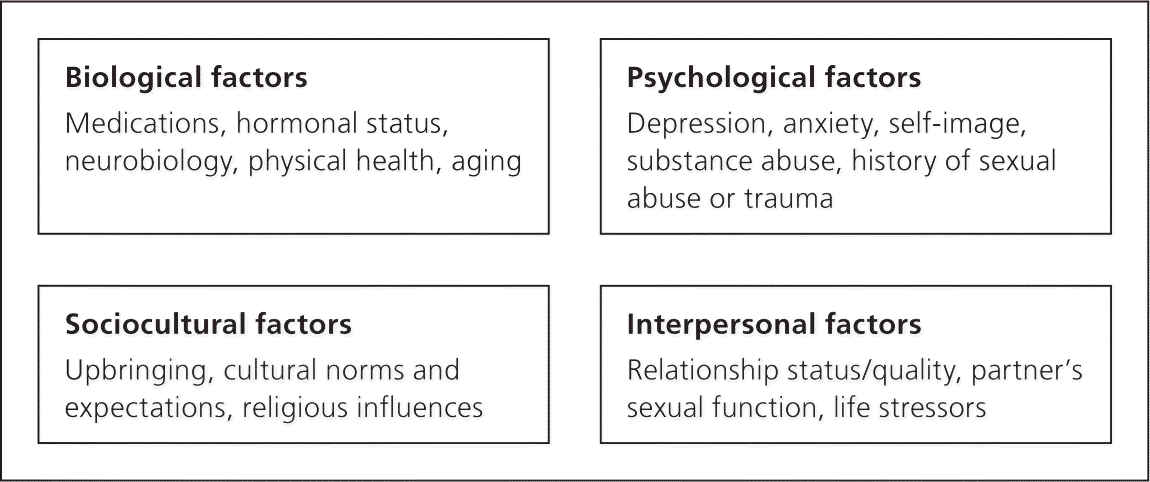
Biopsychosocial model of female sexual dysfunction. Various factors from different realms can promote or hinder normal sexual function.
Information from:
Bitzer J, Giraldi A, Pfaus J. Sexual desire and hypoactive sexual desire disorder in women. Introduction and overview. Standard operating procedure (SOP Part 1). J Sex Med. 2013;10(1):36–49.
Fugl-Meyer KS, Bohm-Starke N, Damsted Petersen C, Fugl-Meyer A, Parish S, Giraldi A. Standard operating procedures for female genital sexual pain. J Sex Med. 2013;101(1):83–93. Latif EZ, Diamond MP. Arriving at the diagnosis of female sexual dysfunction. Fertil Steril. 2013;100(4):898–904.
Table 3. Questions to Facilitate the Assessment of Female Sexual Functioning

| Question | Interpretation of “Yes” answers* | |
|---|---|---|
| Are you currently sexually active (with men, women, or both)? | Continue to the next question (if “No,” also continue to the next question) | |
| Do you have any sexual health concerns? | Continue to the next question | |
| Specifically, any distress related to: | ||
| Your level of sexual desire/interest? | Assess for sexual interest/arousal disorder | |
| Your ability to become or stay sexually aroused (“turned on,” vaginal lubrication, blood flow/warmth/tingly feelings in genitals)? | Assess for sexual interest/arousal disorder | |
| Your ability to experience or reach the desired intensity of an orgasm? | Assess for orgasmic disorder | |
| Are you experiencing any genital pain? | Assess for genito-pelvic pain/penetration disorder, genitourinary syndrome of menopause, and pelvic floor muscle dysfunction | |
| Vaginal dryness or burning? | Assess for genitourinary syndrome of menopause | |
| Pain with sexual activity (insertional or deeper pain)? | Assess for genitourinary syndrome of menopause and pelvic floor muscle dysfunction | |
*—Starting with the second question, if the answer is “No,” the assessment can end.
Information from reference 8.
FEMALE SEXUAL INTEREST/AROUSAL DISORDER
The Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5), combines hypoactive sexual desire disorder and female sexual arousal disorder into a single disorder: female sexual interest/arousal disorder.9 Whereas sexual desire is the motivation to have sex, sexual arousal refers to the physiologic processes of arousal, including vaginal lubrication and genital warmth related to blood flow. Women commonly report experiencing these as part of the same process.10 The DSM-5 criteria for female sexual interest/arousal disorder are presented in Table 4.9
Table 4. DSM-5 Criteria for Female Sexual Interest/Arousal Disorder

| A. Lack of, or significantly reduced, sexual interest/arousal, as manifested by at least three of the following: | |
| 1. Absent/reduced interest in sexual activity. | |
| 2. Absent/reduced sexual/erotic thoughts or fantasies. | |
| 3. No/reduced initiation of sexual activity, and typically unreceptive to a partner's attempts to initiate. | |
| 4. Absent/reduced sexual excitement/pleasure during sexual activity in almost all or all (approximately 75%–100%) sexual encounters (in identified situational contexts or, if generalized, in all contexts). | |
| 5. Absent/reduced sexual interest/arousal in response to any internal or external sexual/erotic cues (e.g., written, verbal, visual). | |
| 6. Absent/reduced genital or nongenital sensations during sexual activity in almost all or all (approximately 75%–100%) sexual encounters (in identified situational contexts or, if generalized, in all contexts). | |
| B. The symptoms in Criterion A have persisted for a minimum duration of approximately 6 months. | |
| C. The symptoms in Criterion A cause clinically significant distress in the individual. | |
| D. The sexual dysfunction is not better explained by a nonsexual mental disorder or as a consequence of severe relationship distress (e.g., partner violence) or other significant stressors and is not attributable to the effects of a substance/medication or another medical condition. | |
| Specify whether: | |
| Lifelong: The disturbance has been present since the individual became sexually active. | |
| Acquired: The disturbance began after a period of relatively normal sexual function. | |
| Specify whether: | |
| Generalized: Not limited to certain types of stimulation, situations, or partners. | |
| Situational: Only occurs with certain types of stimulation, situations, or partners. | |
| Specify current severity | |
| Mild: Evidence of mild distress over the symptoms in Criterion A. | |
| Moderate: Evidence of moderate distress over the symptoms in Criterion A. | |
| Severe: Evidence of severe or extreme distress over the symptoms in Criterion A. | |
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Arlington, Va.: American Psychiatric Association; 2013:433.
It is important to determine whether the patient's problem with desire or arousal is a dysfunction or a normal variation of sexual response. The following examples are not considered sexual dysfunction: a patient reports little or no spontaneous desire but continues to experience responsive desire; a patient maintains spontaneous or responsive desire but reports a desire discrepancy between herself and her partner; a patient has reduced physiologic sexual arousal (e.g., decreased vaginal lubrication or genital blood flow) related to menopausal transition.
FEMALE ORGASMIC DISORDER
DSM-5 criteria for female orgasmic disorder include a marked delay in orgasm, infrequency or absence of orgasm, or less intense orgasm for at least six months in 75% to 100% of sexual interactions.9 Establishing the presence of orgasm is important, because many women may not know whether they have experienced orgasm.11 The next step is determining whether these problems are causing distress. About one-half of women who do not consistently reach orgasm during sexual activity do not report distress.1 If distress exists, the assessment follows the biopsychosocial model with the addition of several key questions that will assist in treatment planning: Is this a change in previous orgasmic functioning? Does this difficulty occur during self-stimulation, partnered sexual activity, or both? Does this difficulty occur across different sexual activities (e.g., oral, manual, vaginal penetration) and with different sex partners?
Orgasmic difficulties may be lifelong (present since sexual debut) or acquired (starting after a period of no dysfunction). Lifelong anorgasmia may suggest the patient is unfamiliar or uncomfortable with self-stimulation or sexual communication with her partner, or lacks adequate sex education.12 Delayed or less intense orgasms may be related to decreased genital blood flow and dulled genital sensations occurring naturally with aging. These examples are not considered sexual dysfunction.
The clinician should determine whether orgasmic difficulties occur only with certain types of stimulation, situations, or partners. If the patient reports difficulty during partnered sexual activity but not with self-stimulation, it may be the result of inadequate sexual stimulation.11 Biological factors requiring assessment and treatment include medical conditions and use of medications that impact sexual functioning11 (Tables 13,4 and 26 ).
GENITO-PELVIC PAIN/PENETRATION DISORDER
In the DSM-5, vaginismus and dyspareunia are combined in genito-pelvic pain/penetration disorder. This disorder of sexual pain is defined as fear or anxiety, marked tightening or tensing of the abdominal and pelvic muscles, or actual pain with vaginal penetration that is persistent or recurrent for at least six months. This may be lifelong or acquired after a period of no dysfunction.9 The clinician should determine if the pain occurs with initial vaginal penetration, deeper penetration, or both.
Treatment
Although female sexual dysfunction often requires multidisciplinary treatment, even the initial visit can be beneficial. Table 5 summarizes the PLISSIT (permission, limited information, specific suggestions, intensive therapy) model for addressing sexual health with patients.13
Table 5. PLISSIT Model for Addressing Sexual Health with Women

| Steps | Examples of what to say to patients |
|---|---|
| Permission: Give patient permission to speak about her sexual health and to do what she is already doing sexually (or may want to do). | “This is important. Thank you for sharing. Many postmenopausal women report a decrease in sexual desire.” |
| Limited information: Provide basic accurate sex education (e.g., female sexual response cycle, impact of aging on sexual function, anatomy). | “Sexual desire changes with age. After menopause you may experience more responsive desire than spontaneous desire.” |
| Specific suggestions: Provide simple suggestions to increase sexual function (e.g., lubricant use, vibrator use, ways to increase emotional intimacy). | “Your responsive sexual desire may benefit from being more planful with sexual activity. Talk with your partner about how to be more intentional sexually.” |
| Intensive therapy: Validate the patient's concerns and refer her to a subspecialist (see eTable A for resources). | “Your sexual health is important. I'd like to refer you to someone with expertise in sexual health.” |
Information from reference 13.
The unique predisposing, precipitating, and maintaining factors for a woman's sexual dysfunction will determine the treatment plan.7,14 Biological factors, such as medication use, are best treated by the clinician.15 Strategies for managing antidepressant-induced dysfunction include reducing the dose if possible, switching to an antidepressant with fewer sexual adverse effects (vs. proactively initiating an antidepressant with fewer sexual adverse effects), or adding bupropion (Wellbutrin) as an adjunct.16 A Cochrane review supports the addition of bupropion in higher dosages (150 mg twice daily) for treatment of antidepressant-induced sexual dysfunction in women, but additional study is needed.17 In one small study, the addition of sildenafil (Viagra) reduced sexual dysfunction induced by selective serotonin reuptake inhibitors or serotoninnorepinephrine reuptake inhibitors.18
Female genital sexual pain disorders are complex and most effectively managed with a comprehensive, multidisciplinary approach that addresses contributing biopsychosocial factors.19 Sexual pain with deeper vaginal penetration suggests the possibility of a musculoskeletal component. This pain may be described as a deeper pelvic pain associated with penetrative sexual activity, pain that radiates to the low back or inner thigh, or pain that persists for some time after vaginal penetration.20 Pelvic floor dysfunction is optimally treated by a physical therapist trained in treating this condition. Consistent painless sexual activity and sexual stimulation with the therapeutic use of a vibrator may also help maintain vaginal health.21 If a patient reports painful sexual activity, it is important to advise her to stop engaging in this activity because it can increase situational anxiety, resulting in tensing of the pelvic floor muscles and increasing pain. Psychotherapy or sex therapy is useful for women who have relational or sociocultural factors contributing to their pain, and for those who experience anxiety in conjunction with their pain.22,23 Psychological, interpersonal, and sociocultural factors are most appropriately treated by a mental health subspecialist. Sexual pain during initial vaginal penetration may suggest inadequate sexual arousal before penetration, genitourinary syndrome of menopause (formerly termed vulvovaginal atrophy),24 or provoked vestibulodynia.
Group cognitive behavior therapy may be effective for low sexual desire.8 Mindfulness-based interventions have been shown to effectively treat several types of female sexual dysfunction, including low sexual desire and arousal, and acquired anorgasmia.7,25,26 Directed masturbation training is the treatment of choice for lifelong anorgasmia.27–29 eTable A includes resources for referral and further information on sexual health.
eTable A. Resources for More Information on Female Sexual Health and Referral

| Resources for clinicians | |
| American Association of Sexuality Educators, Counselors, and Therapists | |
| http://www.aamft.org | |
| International Society for the Study of Women's Sexual Health | |
| http://www.isswsh.org | |
| Society for Sex Therapy and Research | |
| http://www.sstarnet.org | |
| Couples therapy | |
| American Association for Marriage and Family Therapy | |
| http://www.aamft.org | |
| Pelvic physical therapy | |
| American Physical Therapy Association | |
| http://www.moveforwardpt.com/symptomsconditionsdetail.aspx?cid=4c28867f-b11f-4148-a21c-f8b6c5ac7002#.VP0NO_mjOm4 | |
| International Pelvic Pain Society | |
| http://www.pelvicpain.org | |
Special Considerations
MENOPAUSE
Sexual health concerns are common in natural or surgically induced menopause, particularly sexual pain related to genitourinary syndrome of menopause. A Cochrane review showed that hormone therapy (estrogen alone or in combination with a progestogen) was associated with a small to moderate improvement in sexual function, especially pain, in symptomatic or early menopausal women.30 Estrogen treatment is highly effective for genitourinary syndrome of menopause and related dyspareunia; local vaginal estrogen is preferred if vaginal dryness is the primary concern.14,21,31 Ospemifene (Osphena) is a selective estrogen receptor modulator that has been shown to improve the vaginal maturation index, vaginal pH, and symptoms of vaginal dryness.21,32,33 The U.S. Food and Drug Administration (FDA) has approved it for treatment of moderate to severe dyspareunia. The route of administration of estrogen can impact sexual function. Oral estrogens increase sex hormone–binding globulin, which reduces available free testosterone and may thereby adversely impact sexual function, whereas transdermal estrogens have no such effect.6
Women with genitourinary syndrome of menopause and sexual pain may have dysfunctional pelvic floor muscles, which may become tense or tight as a result of ongoing vaginal dryness and discomfort or pain with sexual activity.34 Pelvic floor physical therapy may benefit these women.34
Randomized controlled trials involving naturally or surgically menopausal women with low sexual desire or arousal have shown improvements in sexual function with transdermal testosterone therapy (with or without concomitant estrogen therapy).35–39 However, overall, data on the benefit of testosterone therapy are limited and inconsistent.35,40,41 The Endocrine Society suggests considering a three- to six-month trial of testosterone therapy for postmenopausal women with low sexual desire associated with distress. However, because of the lack of long-term data on safety and effectiveness, it does not recommend routine testosterone treatment for women with low androgen levels related to hypopituitarism, bilateral oophorectomy, or adrenal insufficiency.41 Testosterone therapy is not FDA-approved for use in women, and using testosterone formulations made for men is discouraged. If therapy is initiated, clinical evaluation and laboratory monitoring of testosterone levels are suggested to evaluate for overuse and signs of hyperandrogenism (e.g., acne, hair growth).41
SEXUAL DISTRESS WITHOUT DYSFUNCTION
If a patient reports distress but does not meet criteria for sexual dysfunction, intervention is still needed. Women who report low desire or arousal, difficulty with orgasm, or inadequate sexual stimulation may benefit from normalization, sexual health education, and referral to a sex therapist.42
The female sexual response cycle (eFigure B) is an important educational tool that clinicians can use when counseling women with sexual concerns. Women enter this cycle of sexual response with spontaneous sexual drive (i.e., the internal desire for sexual activity) or more commonly from a nonsexual state. A woman in a nonsexual state may engage in a sexual encounter for a number of nonsexual reasons (e.g., to please her partner, to feel emotionally connected, out of a sense of duty). Once sexual activity (with adequate stimulation) begins, the woman may experience sexual arousal, which may lead to responsive sexual desire and motivation for future sexual responsiveness.42 This model delineates spontaneous and responsive desire, normalizes the sexual experience of arousal preceding desire, and stresses emotional intimacy as a major motivator for sexual responsiveness.
eFigure B
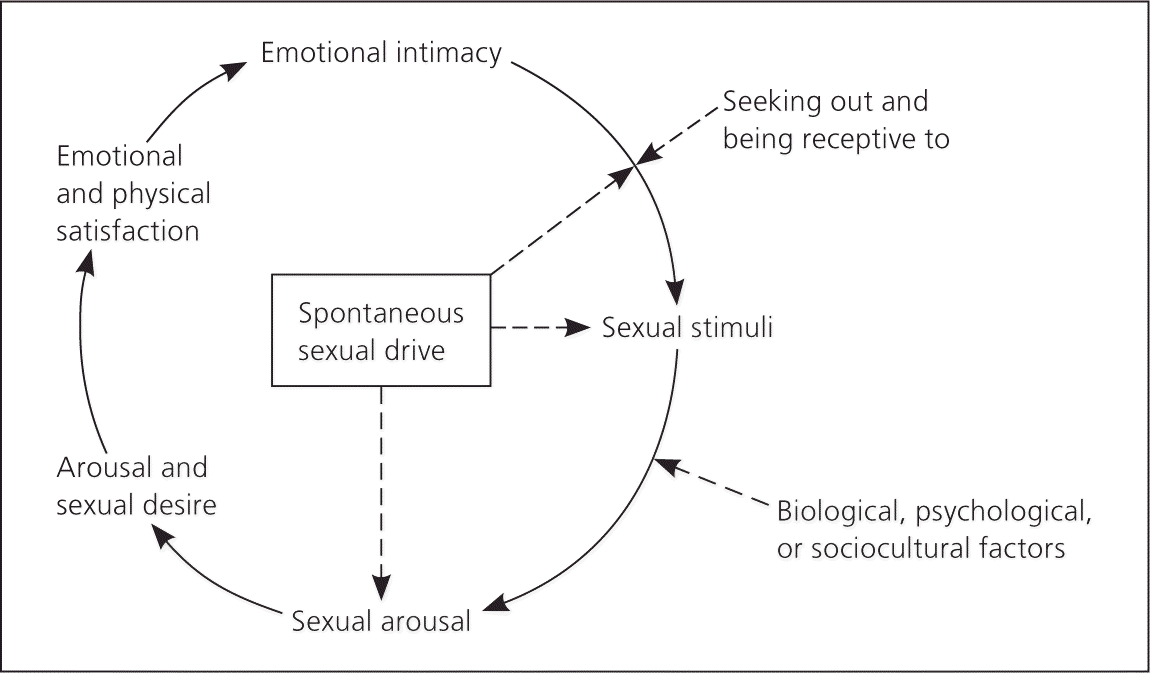
Female sexual response cycle. Interrelated factors work together to promote sexual response.
Adapted with permission from Basson R. Human sex-response cycles. J Sex Marital Ther. 2001;27(1):34.
Data Sources: A comprehensive English-language search of several databases from 2004 to August 7, 2014, was conducted and included MEDLINE In-Process & Other Non-Indexed Citations, MEDLINE, EMBASE, PsycINFO, Cochrane Database of Systematic Reviews, Cochrane Central Register of Controlled Trials, U.S. Preventive Services Task Force recommendations, National Guideline Clearinghouse, Agency for Healthcare Research and Quality evidence reports, the Institute for Clinical Systems Improvement guidelines, and Essential Evidence. Keywords included dyspareunia, libido, orgasm, orgasmic, orgasms, sexual arousal, sexual desire, and sexual dysfunction. Search dates: August to October 2014.
The authors thank Kristi Simmons, Mayo Clinic Research and Academic Support Services, for her assistance in formatting and proofreading the manuscript.

