The preparticipation physical evaluation is a commonly requested medical visit for amateur and professional athletes of all ages. The overarching goal is to maximize the health of athletes and their safe participation in sports. Although studies have not found that the preparticipation physical evaluation prevents morbidity and mortality associated with sports, it may detect conditions that predispose the athlete to injury or illness and can provide strategies to prevent injuries. Clearance depends on the outcome of the evaluation and the type of sport (and sometimes position or event) in which the athlete participates. All persons undergoing a preparticipation physical evaluation should be questioned about exertional symptoms, presence of a heart murmur, symptoms of Marfan syndrome, and family history of premature serious cardiac conditions or sudden death. The physical examination should focus on the cardiovascular and musculoskeletal systems. U.S. medical and athletic organizations discourage screening electrocardiography and blood and urine testing in asymptomatic patients. Further evaluation should be considered for persons with heart or lung disease, bleeding disorders, musculoskeletal problems, history of concussion, or other neurologic disorders.
Approximately 30 million athletes younger than 18 years and another 3 million athletes with special needs receive medical clearance to participate in sports every year.1 The purpose of the preparticipation physical evaluation (PPE) is to maximize the health of athletes and their safe participation in sports. The most comprehensive guideline on the PPE is the 4th edition of the American Academy of Pediatrics' PPE recommendations, which contains consensus recommendations and has been endorsed by multiple stakeholder medical societies.2 Although studies have not found that the PPE prevents morbidity and mortality associated with sports participation,2 it may detect conditions that predispose the athlete to injury or illness and can provide strategies to prevent injuries.3
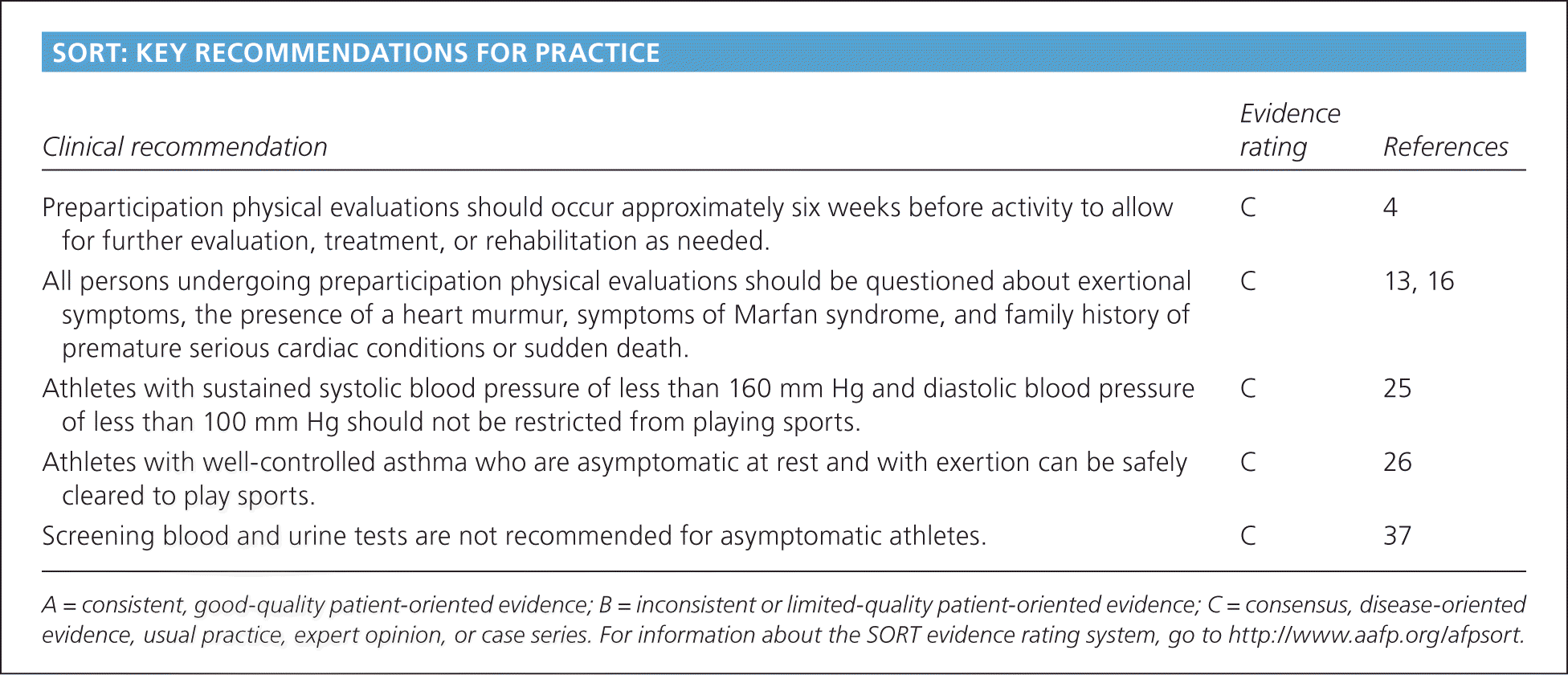
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Preparticipation physical evaluations should occur approximately six weeks before activity to allow for further evaluation, treatment, or rehabilitation as needed. | C | 4 |
| All persons undergoing preparticipation physical evaluations should be questioned about exertional symptoms, the presence of a heart murmur, symptoms of Marfan syndrome, and family history of premature serious cardiac conditions or sudden death. | C | 13, 16 |
| Athletes with sustained systolic blood pressure of less than 160 mm Hg and diastolic blood pressure of less than 100 mm Hg should not be restricted from playing sports. | C | 25 |
| Athletes with well-controlled asthma who are asymptomatic at rest and with exertion can be safely cleared to play sports. | C | 26 |
| Screening blood and urine tests are not recommended for asymptomatic athletes. | C | 37 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN PREVENTIVE MEDICINE: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not order annual electrocardiography or any other cardiac screening for asymptomatic, low-risk patients. | American Academy of Family Physicians and American College of Physicians |
| Do not screen adolescents for scoliosis. | American Academy of Family Physicians |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Ideally, the athlete's personal physician should provide the PPE in a medical home where patients are comfortable discussing sensitive information and where past medical records are available. Alternate models include mass participation screenings and PPEs conducted by a team physician at a student health, outpatient, or athletic facility. Mass screenings are not ideal, given the unavailability of parents and previous medical records, and decreased continuity of care. Supervision of mass screenings by a designated primary care physician can improve this process by ensuring that all results are reviewed and by coordinating follow-up when necessary. PPEs should occur approximately six weeks before activity to allow for further evaluation, treatment, or rehabilitation as needed.4 Consensus guidelines recommend yearly PPEs2; however, the optimal interval is uncertain, and local regulatory agencies may require more or less frequent PPEs for athletic participation.5
General Principles
The examining physician should determine clearance for participation in coordination with specialists or team physicians. Clearance depends on the outcome of the evaluation and the type of sport (and sometimes position or event) in which the athlete wishes to participate. Most healthy athletes will receive unrestricted clearance to play any sport. An athlete may be provisionally cleared pending successful completion of a specified treatment, test, or rehabilitation program.
For athletes restricted from certain sports, guidance should be provided based on the general category of the sport. Sports may be classified as collision, contact, or noncontact activities or classified based on physical intensity (Figure 1).6 The risk of injury depends on the following variables: speed, force of impact, height, and unpredictability of both the actions of the sport and conditions. Even persons with serious medical illness may be able to participate in nonstrenuous or noncontact activities. Rarely, athletes may be disqualified completely from participation (Table 1).7 A 2012 study found that 5.5% of adolescents were deemed ineligible for sports.8 eFigures A through D outline a standardized approach to components of the PPE, including a supplemental history form that can be used for athletes who have special needs.
Figure 1. Classification of Sports by Physical Intensity
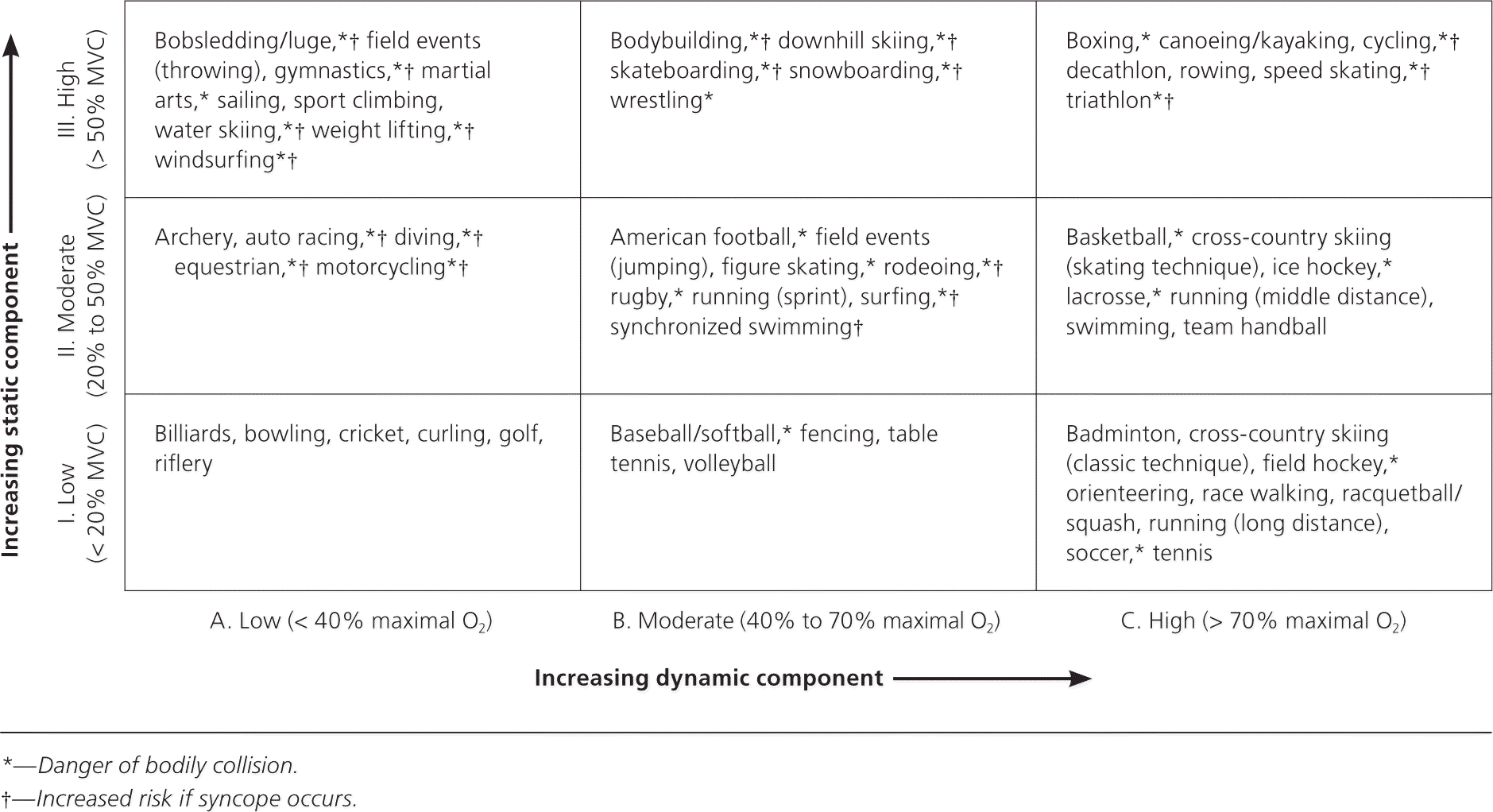
Classification of sports by physical intensity. (MVC = maximal voluntary contraction.)
Adapted with permission from Mitchell JH, Haskell W, Snell P, Van Camp SP. Task Force 8: classification of sports. J Am Coll Cardiol. 2005;45(8):1366.
Table 1. Contraindications for Sports Participation

| Active myocarditis or pericarditis |
| Acute enlargement of spleen or liver |
| Eating disorder in which athlete is not compliant with therapy and follow-up, or when there is evidence of diminished performance or potential injury because of the eating disorder |
| History of recent concussion and symptoms of postconcussion syndrome (no contact or collision sports) |
| Hypertrophic cardiomyopathy |
| Long QT syndrome |
| Poorly controlled convulsive disorder (no archery, riflery, swimming, weight lifting or powerlifting, strength training, or sports involving heights) |
| Recurrent episodes of burning upper-extremity pain or weakness, or episodes of transient quadriplegia until stability of cervical spine can be assured (no contact or collision sports) |
| Severe hypertension until controlled by therapy (static resistance activities, such as weight lifting, are particularly contraindicated) |
| Sickle cell disease (no high-exertion, contact, or collision sports) |
| Suspected coronary artery disease until fully evaluated (patients with impaired resting left ventricular systolic function less than 50%, exercise-induced ventricular dysrhythmias, or exercise-induced ischemia on exercise stress testing are at greatest risk of sudden death) |
Adapted with permission from Kurowski K, Chandran S. The preparticipation athletic evaluation. Am Fam Physician. 2000;61(9):2688.
History
A thorough history is critical to identify athletes with underlying medical conditions that may interfere with participation in sports. The history alone may uncover 88% of medical conditions and 67% of musculoskeletal problems during the PPE.9 Particular attention should be given to the personal and family cardiac histories (Table 2).10 Ideally, a parent or guardian should be present at the PPE to provide historical details for athletes younger than 18 years.
Table 2. American Heart Association Recommendations on Screening for Cardiovascular Abnormalities in Competitive Athletes

| Personal history |
| Elevated blood pressure |
| Excessive dyspnea or fatigue associated with exercise |
| Exertional chest pain or discomfort |
| Prior recognition of a heart murmur |
| Unexplained syncope or near-syncope |
| Family history |
| Disability from heart disease in a close relative younger than 50 years |
| Premature death (sudden and unexpected, or otherwise) before 50 years of age due to heart disease |
| Specific knowledge of certain cardiac conditions in family members: hypertrophic or dilated cardiomyopathy, long QT syndrome, Marfan syndrome, or arrhythmias |
| Physical examination |
| Brachial artery blood pressure (sitting position) |
| Femoral pulses to exclude aortic coarctation |
| Heart murmur* |
| Physical stigmata of Marfan syndrome |
*—Auscultation should be performed in the supine and standing positions (or with the Valsalva maneuver) to identify murmurs of dynamic left ventricular outflow tract obstruction.
Adapted with permission from Maron BJ, Thompson PD, Ackerman MJ, et al. Recommendations and considerations related to preparticipation screening for cardiovascular abnormalities in competitive athletes: 2007 update: a scientific statement from the American Heart Association Council on Nutrition, Physical Activity, and Metabolism. Circulation. 2007;115(12):1646.
All persons undergoing a PPE should be questioned using the American Heart Association's (AHA's) recommended inquiries about exertional symptoms, the presence of a heart murmur, symptoms of Marfan syndrome, and a family history of premature serious cardiac conditions or sudden death.10 Other inquiries about potentially life-threatening or disqualifying illnesses include a history or symptoms compatible with spinal and brachial plexus injuries, concussion, hematologic disorders, loss of paired organs, asthma or exercise-induced bronchospasm, neurologic disorders, heat illness, and musculoskeletal injuries.
Physical Examination
At minimum, the physical examination should include assessment of vital signs, vision, hearing, and the cardiovascular and musculoskeletal systems. The most common abnormal PPE findings are elevated blood pressure and vision problems.11 Genital examination is not recommended in females but may be indicated in males with symptoms or a history of genitourinary problems. Although a brief standardized orthopedic screening is adequate in asymptomatic athletes (see https://www.aafp.org/afp/2000/0501/p2696.html), a more focused physical examination is necessary in persons with a history of musculoskeletal injury.11
Special Considerations
CARDIOVASCULAR DISEASE
The 36th Bethesda guidelines, a consensus statement published by the American College of Cardiology (ACC) and the AHA, include recommendations about eligibility based on the physical strenuousness of the sport for competitive athletes who have previously diagnosed cardiac conditions.12 For example, the guidelines permit persons with known hypertrophic cardiomyopathy to participate in low-intensity activities, but recommend exclusion from most strenuous activities.12
Screening asymptomatic athletes for previously undetected heart conditions, such as hypertrophic cardiomyopathy or arrhythmogenic right ventricular dysplasia, is recommended by the ACC/AHA guidelines, but the optimal protocol and overall effectiveness are controversial.13–15 As currently used, the PPE has not been successful in decreasing rates of sudden cardiac death during sports in young athletes.16,17 Screening electrocardiography (ECG) and echocardiography may increase sensitivity for detection of undiagnosed cardiac disease,18 but accurate interpretation can be challenging and may result in false-positive findings when performed by clinicians who are less experienced in distinguishing athletic heart adaptations from cardiomyopathy.19 The ACC/AHA guidelines do not recommend ECG in asymptomatic patients during physical examination, but do support local programs in which ECG can be applied with high-quality cardiology resources.10,20 In contrast, the International Olympic Committee21 and the European Society of Cardiology recommend routine screening ECG,13 and this practice is becoming more common in professional sports22 and in the community setting.
Recently, the Seattle criteria were proposed to help physicians interpret screening ECG in athletes with the goals of identifying abnormalities that likely represent serious cardiac pathology and reducing false-positive interpretations.23 Although these criteria have improved the specificity of ECG and may be useful to physicians who are asked to interpret screening ECG in athletes, they have not been prospectively evaluated for decreasing morbidity.24
Because exercise is therapeutic for persons with hypertension, athletes with sustained systolic blood pressure of less than 160 mm Hg and diastolic blood pressure of less than 100 mm Hg should not be restricted from sports.25 Athletes with higher blood pressures benefit from further evaluation and initiation of treatment before unrestricted clearance is provided.
ORTHOPEDIC AND MUSCULOSKELETAL INJURIES
Patients with known orthopedic injuries should undergo a thorough joint-specific examination. Strict return-to-play timelines (e.g., two weeks after an ankle sprain) are counterproductive; injuries should be treated and cleared on a functional basis. Generally, if the athlete has no disabling pain, full range of motion, and full strength in the affected area, and is able to pass functional tests in a supervised sports setting, clearance can be provided after a PPE, barring other contraindications.
ASTHMA AND EXERCISE-INDUCED BRONCHOSPASM
Patients with a history of asthma should be risk stratified based on their history. Standard classification of asthma as mild intermittent, mild persistent, moderate, or severe can help guide decisions. An understanding of asthma triggers is also essential, especially for exercise-induced bronchospasm. Athletes with well-controlled asthma who are asymptomatic at rest and with exertion can be safely cleared after a PPE.26 Pulmonary function testing should be considered for patients with a historical diagnosis of exercise-induced bronchospasm to exclude undiagnosed asthma. Athletes who are actively wheezing or recovering from an asthma exacerbation should be restricted from participation until symptoms have stabilized. Physicians may require athletes to have a rescue inhaler immediately available as a condition for athletic participation.
EPILEPSY
Persons with well-controlled seizures can participate in sports.27 Exceptions include sports in which a seizure could be fatal, such as skydiving, hang gliding, and scuba diving.
CONCUSSION
In athletes with a history of concussion, physicians should determine the number of concussions they have had; their duration, frequency, and recovery time; and risk factors.28 A complete neurologic examination should be performed. Athletes with signs and symptoms of concussion or postconcussion syndrome should not be cleared for participation until all symptoms have resolved.29 Neuroimaging is generally not needed. Formal balance testing, such as the Balance Error Scoring System and neuropsychologic testing, can help inform decisions about when to return to play.30 Disqualification for athletes with a history of frequent or severe concussions is controversial.31
HEMATOLOGIC DISORDERS
Consensus guidelines from the National Hemophilia Foundation advise that athletes with bleeding disorders such as hemophilia be restricted from contact or collision sports.32 Athletes with von Willebrand disease also may be restricted, depending on the subtype.33 Although persons with sickle cell disease are functionally limited to low-intensity activities, those with sickle cell trait may participate in all activities.34 Athletes with sickle cell trait may experience exertional sickling in conjunction with other risk factors such as elevation, dehydration, or illness. In 2010, the National Collegiate Athletic Association (NCAA) mandated that the sickle cell trait status of all incoming athletes must be established by the time of the PPE; however, athletes are allowed to decline screening.5 Sickle cell trait is associated with 2% of deaths in NCAA football players.35
EATING DISORDERS, PSYCHIATRIC DISORDERS, AND DRUG ABUSE
Athletes in weight-sensitive sports (e.g., boxing, wrestling) and aesthetic sports (e.g., diving, figure skating, dance) are at risk of eating disorders and general disordered eating.36 In females, disordered eating and excessive exercise may lead to low body mass index, menstrual irregularity, and low bone mineral density (i.e., the female athlete triad). These patients should be engaged in a multidisciplinary treatment program with further risk stratification before return to sport.36 Athletes with untreated mental illness should receive treatment and be stabilized before resuming athletic participation. Athletes with identified drug abuse should also receive treatment before returning to sport.
Laboratory and Imaging Studies
Laboratory and imaging studies should be used as an extension of the history and physical examination when additional information is needed to evaluate a concern. Screening blood and urine tests are not recommended for asymptomatic athletes.37 Athletes with previously treated or chronic conditions may require further testing.11,38
Data Sources: We searched the Cochrane database, Medline, and Essential Evidence Plus with the key words PPE, preparticipation physical exam, preseason physical, and sports clearance. The search was not limited by study type. Search dates: April 24, 2014, through April 25, 2015.

